The goal of this article is to enhance the surgical precision and accuracy of surgeons performing upper and lower eyelid blepharoplasty. The most common blepharoplasty complications are described and how to avoid them is discussed in detail. Complications range from mild to severe and for each, preoperative measures to prevent, perioperative measures to avoid, and postoperative measures to minimize complications are detailed. After reading this article the surgeon should have a greater understanding of blepharoplasty complications and how to best manage and avoid them.
Key points
- •
Always err on the conservative side, as it is far easier to remove more tissue than to replace deficient tissue.
- •
Be patient during the healing process; time heals many imperfections and avoid early interventions.
- •
Proper preoperative counseling of patients is essential to maximize patient satisfaction with surgery.
- •
Preoperative and prior patient photographs are necessary to review before surgery and also help to document improvement.
- •
Upper eyelid markings are crucial to achieving optimal results and many complications can be avoided with proper markings.
Introduction
The earliest attempts at removing excess skin, puffiness, and wrinkling of the eyelid skin was during the tenth and eleventh centuries by Arabic surgeons. Today, blepharoplasty has become the second most common cosmetic procedure performed in the United States. It is one of the least invasive cosmetic surgeries available and, when performed correctly, is very safe and yields excellent results. It is one of the most effective ways to rejuvenate the periocular area. However, devastating complications, ranging from permanent vision loss to cosmetic deformity can occur following blepharoplasty. Most complications result from unrecognized changes in anatomy, errors in measurements, or overzealous removal of tissue ( Table 1 ). This article outlines the most common blepharoplasty complications that occur, and offers preventive measures to avoid such complications.
| Complication | Causes | Avoidance | Correction |
|---|---|---|---|
| Residual upper lid skin | Underestimation of dermatochalasis | Learn and use proper pinch technique | Revision with skin excision |
| Eyelid ptosis | Unrecognized preoperatively, trauma to levator aponeurosis during blepharoplasty | Measure MRD preoperatively | Surgical correction of ptosis |
| Superior sulcus deformity | Overaggressive removal of fat during blepharoplasty | Evaluate superior sulcus preoperatively; judicious fat excision, medial only | Augment superior sulcus with fillers (autologous, hyaluronic acid) |
| Eyelid crease asymmetry | Uneven marking of eyelid crease | Measure eyelid crease with caliper at various points across lid | Crease revision with fixation to levator aponeurosis |
| Eyelid retraction/ectropion | Overly aggressive skin removal, scarring of the middle lamella | Conservative skin excision; minimize cautery | Middle lamellar release with posterior lamellar grafting |
| Canthal webbing | Extending incision too close to lid margin medially or laterally | Proper marking preoperatively | Z-plasty, canthoplasty, skin grafting |
| Brow ptosis | Unrecognized preoperatively; overaggressive skin removal from upper eyelid accentuates brow ptosis | Evaluate eyebrow position with patient in the relaxed state preoperatively | Correct eyebrow ptosis |
| Lagophthalmos | Overly aggressive skin removal from upper or lower eyelids | Conservative removal of skin | Full-thickness skin grafting; midface lifting, posterior/middle lamellar grafting |
| Globe perforation | Misdirection of needle during injection of local anesthetic | Never direct needle at globe | Emergent referral to ophthalmologist for complete eye examination |
| Hemorrhage (preseptal, retrobulbar) | Excessive venous or arterial hemorrhage | Stop anticoagulation; ensure surgical field is dry; avoid valsalva | Emergent canthotomy/cantholysis (retrobulbar); conservative measures (preseptal hematoma) |
| Infection (preseptal, orbital) | Bacterial, fungal | Prep with betadine; instruct patient to keep area clean and dry; antibiotic ointment | Preseptal: Trial of broad-spectrum oral antibiotics Orbital: Admit to hospital for intravenous antibiotics; ophthalmology consult |
| Diplopia | Traumatic injury to extraocular muscles; injection of local anesthetic into extraocular muscles; suture incorporation of muscle | Avoid deep injection | Referral to strabismus specialist |
| Lacrimal gland injury | Inadvertent resection of the lacrimal gland | Recognize appearance of lacrimal gland prolapse | Supportive measures with artificial tears, ointments |
| Horizontal eyelid phimosis | Lateral canthal dehiscence | Ensure lower crux of canthus is reapproximated to superior crux | Canthus-sparing canthopexy/canthoplasty |
| Corneal abrasion | Exposed cornea during surgery; accidental trauma during surgery | Corneal protectors with ointment | Referral to ophthalmologist |
| Fire | Spontaneous combustion of flammable material, spark, and oxygen | Avoid use of cautery, moisten field during cautery use, turn off supplemental oxygen | Supportive measures |
| Wound dehiscence | Poorly tied sutures, patient noncompliance (rubbing, exertion) | Proper suture technique | Debride wound and resuture |
| Suture granuloma | Foreign body reaction to suture | Use smallest sutures possible | Observation, trial of steroid cream, excision |
| The dissatisfied patient | Unrealistic expectations, unexpected bruising or postoperative healing, personality difference | Full disclosure of risks of surgery, realistic expectations of surgery | Reassurance, empathy frequent office visits |
Introduction
The earliest attempts at removing excess skin, puffiness, and wrinkling of the eyelid skin was during the tenth and eleventh centuries by Arabic surgeons. Today, blepharoplasty has become the second most common cosmetic procedure performed in the United States. It is one of the least invasive cosmetic surgeries available and, when performed correctly, is very safe and yields excellent results. It is one of the most effective ways to rejuvenate the periocular area. However, devastating complications, ranging from permanent vision loss to cosmetic deformity can occur following blepharoplasty. Most complications result from unrecognized changes in anatomy, errors in measurements, or overzealous removal of tissue ( Table 1 ). This article outlines the most common blepharoplasty complications that occur, and offers preventive measures to avoid such complications.
| Complication | Causes | Avoidance | Correction |
|---|---|---|---|
| Residual upper lid skin | Underestimation of dermatochalasis | Learn and use proper pinch technique | Revision with skin excision |
| Eyelid ptosis | Unrecognized preoperatively, trauma to levator aponeurosis during blepharoplasty | Measure MRD preoperatively | Surgical correction of ptosis |
| Superior sulcus deformity | Overaggressive removal of fat during blepharoplasty | Evaluate superior sulcus preoperatively; judicious fat excision, medial only | Augment superior sulcus with fillers (autologous, hyaluronic acid) |
| Eyelid crease asymmetry | Uneven marking of eyelid crease | Measure eyelid crease with caliper at various points across lid | Crease revision with fixation to levator aponeurosis |
| Eyelid retraction/ectropion | Overly aggressive skin removal, scarring of the middle lamella | Conservative skin excision; minimize cautery | Middle lamellar release with posterior lamellar grafting |
| Canthal webbing | Extending incision too close to lid margin medially or laterally | Proper marking preoperatively | Z-plasty, canthoplasty, skin grafting |
| Brow ptosis | Unrecognized preoperatively; overaggressive skin removal from upper eyelid accentuates brow ptosis | Evaluate eyebrow position with patient in the relaxed state preoperatively | Correct eyebrow ptosis |
| Lagophthalmos | Overly aggressive skin removal from upper or lower eyelids | Conservative removal of skin | Full-thickness skin grafting; midface lifting, posterior/middle lamellar grafting |
| Globe perforation | Misdirection of needle during injection of local anesthetic | Never direct needle at globe | Emergent referral to ophthalmologist for complete eye examination |
| Hemorrhage (preseptal, retrobulbar) | Excessive venous or arterial hemorrhage | Stop anticoagulation; ensure surgical field is dry; avoid valsalva | Emergent canthotomy/cantholysis (retrobulbar); conservative measures (preseptal hematoma) |
| Infection (preseptal, orbital) | Bacterial, fungal | Prep with betadine; instruct patient to keep area clean and dry; antibiotic ointment | Preseptal: Trial of broad-spectrum oral antibiotics Orbital: Admit to hospital for intravenous antibiotics; ophthalmology consult |
| Diplopia | Traumatic injury to extraocular muscles; injection of local anesthetic into extraocular muscles; suture incorporation of muscle | Avoid deep injection | Referral to strabismus specialist |
| Lacrimal gland injury | Inadvertent resection of the lacrimal gland | Recognize appearance of lacrimal gland prolapse | Supportive measures with artificial tears, ointments |
| Horizontal eyelid phimosis | Lateral canthal dehiscence | Ensure lower crux of canthus is reapproximated to superior crux | Canthus-sparing canthopexy/canthoplasty |
| Corneal abrasion | Exposed cornea during surgery; accidental trauma during surgery | Corneal protectors with ointment | Referral to ophthalmologist |
| Fire | Spontaneous combustion of flammable material, spark, and oxygen | Avoid use of cautery, moisten field during cautery use, turn off supplemental oxygen | Supportive measures |
| Wound dehiscence | Poorly tied sutures, patient noncompliance (rubbing, exertion) | Proper suture technique | Debride wound and resuture |
| Suture granuloma | Foreign body reaction to suture | Use smallest sutures possible | Observation, trial of steroid cream, excision |
| The dissatisfied patient | Unrealistic expectations, unexpected bruising or postoperative healing, personality difference | Full disclosure of risks of surgery, realistic expectations of surgery | Reassurance, empathy frequent office visits |
Inadvertent errors in assessment
Residual Skin Excess
A conservative approach to blepharoplasty is essential, as the consequences of overaggressive tissue removal are more difficult to correct than the consequences of residual skin excess. Patients should be counseled preoperatively that approximately 5% to 10% of patients will need additional residual skin removed following blepharoplasty and that removing more skin later does not limit the final cosmetic result. Residual dermatochalasis usually results from an underestimation of how much dermatochalasis is present and is noted most commonly on the lateral eyelid.
In any patient desiring further removal of eyelid skin, evaluation for eyebrow ptosis should be performed. If concurrent eyebrow ptosis is present, removal of more skin will only exaggerate the eyebrow ptosis. For these patients, the eyebrow ptosis should be addressed before revising the blepharoplasty. If eyebrow ptosis is not present, the surgeon must ensure adequate skin remains for the eyelid to properly close after revision. Historically, this has been 20 mm measured in the center of the eyelid, from the lash line to the base of the brow. If the patient has cosmetically altered the brows with tattoos, the natural brow height should be used.
Patients may request more skin to be removed when there is questionable residual skin present. Explanation of the importance of proper lid function and avoidance of lagophthalmos informs the patient of additional risk and usually dissuades the patient from seeking further revision. Revision should be considered only after healing is complete, usually 3 to 6 months after the initial surgery.
Eyelid Ptosis
If unrecognized, uncorrected eyelid ptosis limits the cosmetic result of a blepharoplasty. Ptosis is defined medically as a margin-to-reflex distance-1 of 2.5 mm or less. However, many patients recognize even more subtle differences between the eyelid heights, and even as little as 0.5 mm will be intolerable to some patients. Therefore, the margin-to-reflex distance must be measured preoperatively with the patient in the relaxed state to document asymmetry. Preoperative discussion with the patient regarding preexisting ptosis is essential to avoid postoperative disappointment.
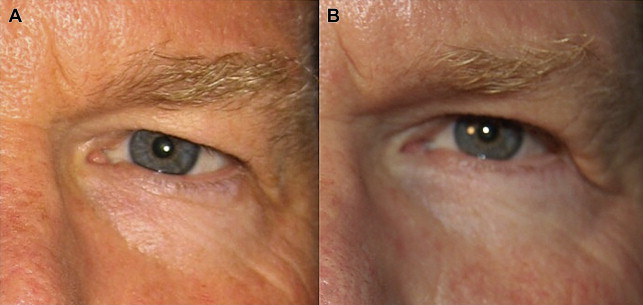
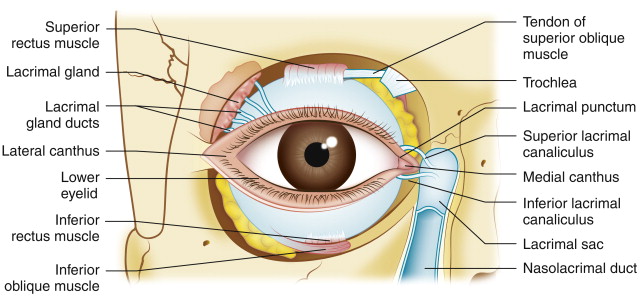
In the early postoperative period, eyelid ptosis following blepharoplasty is not uncommon. It can be the result of postoperative edema and should not be worrisome; however, if ptosis persists after resolution of postoperative edema, it is possible the levator muscle/aponeurosis was traumatized or disinserted during blepharoplasty ( Fig. 1 ). If the levator function is decreased following surgery, damage to the muscle should be expected and likely the patient will require levator advancement to correct the ptosis. Sound knowledge of the eyelid anatomy is essential to avoid inadvertent damage to surrounding structures. The levator muscle is located directly beneath the preaponeurotic fat pad; therefore, dissection beyond the fat pads should be limited to avoid levator injury ( Fig. 2 ).
Superior Sulcus Contour Deformity/Hollowing
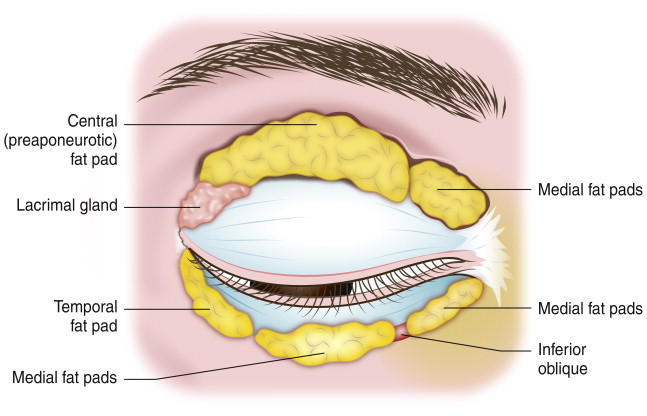
Trends in upper and lower blepharoplasty rejuvenation techniques have shifted from fat resection to fat conservation. A youthful upper eyelid is full, especially in the lateral aspect. With time, the central fat pad atrophies, while the medial fat pad become more prominent; this can cause a tear drop–shaped deformity in an otherwise hollowed eyelid ( Fig. 3 ). Overaggressive resection of fat during upper eyelid blepharoplasty can result in a hollowed superior sulcus that is particularly aging. The volume of the upper eyelid is in part made up of the medial and central fat pads, as well as the eyebrow fat pad. The composition of these fat pads is different. The medial fat pad is lighter in color due to variations in carotenoid composition and possibly from enrichment of orbital stem cells. Targeted removal or repositioning of the medial upper eyelid fat may be necessary if a patient has a tear drop nasal fat accumulation. Preoperative examination should include observation of the medial and lateral eyelid contour to evaluate the prominence of the medial and central fat pads.
Asymmetric Eyelid Crease
Although there are studies both for and against symmetry equaling beauty in a face, almost all faces have some asymmetry. Patients seeking cosmetic or functional blepharoplasty, however, expect relative symmetry postoperatively. After blepharoplasty, some patients will notice asymmetry between their eyes that was present preoperatively, but never recognized. For this reason, it is essential to have high-quality preoperative photographs documenting asymmetry.
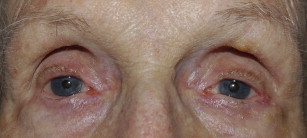
However, errors in preoperative assessment and markings, in some cases, may lead to avoidable asymmetry postoperatively ( Fig. 4 ). Complete preoperative examination of eyelids for ptosis, globe prominence, and thyroid eye disease is necessary to avoid suboptimal results.
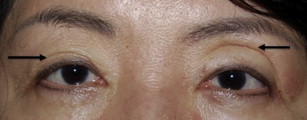
Marking of the skin is the most critical portion of the upper eyelid blepharoplasty surgery. Although there are standard guidelines, the markings are for the most part artistic and decided on by the surgeon. Some variations in markings exist that will yield slight differences in results, but in general the better outcome is in the eye of the beholder ( Fig. 5 ). Usually, respecting the patient’s natural eyelid crease is desired, unless the patient wishes an altered lid crease. If no obvious crease is visible or if the crease is heightened due to levator dehiscence, marking the eyelid crease 7 to 8 mm above the lash line in Caucasian men and 8 to 10 mm above the lash line in Caucasian women yields are good guidelines. Guidelines in Asian men are a crease set between 5 to 6 mm and Asian women at 6 to 7 mm.
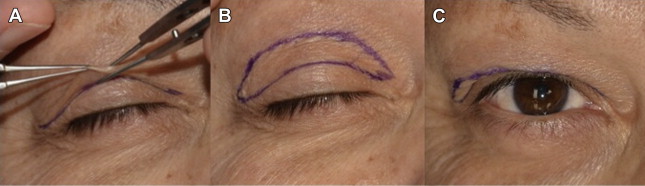
The crease extends in a fairly mild arc from lateral to medial canthus. Beyond the puncta, the marking should angle superiorly to avoid medial canthal webbing postoperatively. Laterally, beyond the lateral canthus, the marking should also angle superiorly to address any hooding. Then, 2 nontoothed forceps should be used to pinch the excess skin while avoiding lagophthalmos. This should be performed centrally, medially, and laterally to mark the redundant skin. These points should then be connected in a smooth arc. The patient is then asked to open his or her eyelids and the upper and lower markings should blend together (see Fig. 5 C).
Initially, asymmetry between the eyelids is common and the patient can be reassured. However, once the healing is complete, if significant asymmetry exists, revision may be considered. In general, it is easier to raise a crease rather than lowering one. A higher crease may be created by making a new incision above the previous mark and fixating the orbicularis at the new height to the levator aponeurosis. Lowering the crease is more difficult, and requires making a lower incision at the new lower level with advancement of the preaponeurotic fat or placing free fat pearls to prevent readhesion at the higher level. Although good results can be obtained, these results are often not as desirable as appropriate initial marking.
Eyelid Retraction/Ectropion
One of the most troublesome complications following lower eyelid blepharoplasty is eyelid retraction and cicatricial ectropion, as they are not only cosmetically deforming, but can cause agonizing symptoms of foreign body sensation and decreased vision ( Fig. 6 A). Eyelid retraction often results from scarring of the middle lamella during lower eyelid blepharoplasty. Eyelid ectropion is typically caused by aggressive removal of skin during lower eyelid blepharoplasty and unrecognized lower eyelid laxity. To avoid this, judicious skin removal should be performed during lower eyelid blepharoplasty only if significant redundancy of the skin exists. In general, at most only a few millimeters of skin should be removed. Many patients only require lower eyelid fat recontouring rather than skin excision. It is important to explain to patients preoperatively that lower eyelid blepharoplasty addresses the contour of the lower eyelid rather than removal of skin. The crepelike quality and deep rhytids of the skin will not change with blepharoplasty. Often a skin treatment, such as a chemical peel or laser resurfacing, is needed to address this.
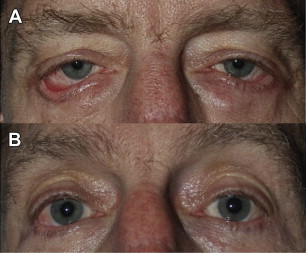
Correction of eyelid retraction can be performed with autologous tissue, such as hard palate, dermis fat, or acellular dermis, to build up the posterior with complete release of the middle lamella (see Fig. 6 B). Skin grafting is considered the last option and will likely be necessary only in severe cases. Although reconstructive efforts result in restored lid position, often the function and cosmetic result is not as ideal as if the retraction and ectropion did not occur.
Canthal Webbing
An unsightly complication following blepharoplasty is webbing of the tissue at the medial or lateral canthus. Medially, this often results from the incision nearing the lid margin too closely or if the incision is extended to far medially or inappropriately angled inferiorly. Laterally, this results when the upper and lower incisions join to create an inferior angle or if too much skin is removed. This is more likely to occur in Asian patients, or any patient with a lower-set eyelid crease and patients with brow ptosis. Proper marking is essential to avoid this complication.
Brow Ptosis
Accurate preoperative assessment of the facial and eyelid anatomy is essential to achieving a sound cosmetic result. Identification of the eyebrow ptosis preoperatively is essential. Regardless of the amount of skin to be removed during blepharoplasty, at least 20 mm of skin should remain on the upper eyelid to allow for proper eyelid closure following surgery. If brow ptosis is unrecognized and the amount of remaining skin is not measured, excessive skin can be removed, leading to lagophthalmos and further exaggeration of the eyebrow ptosis ( Fig. 7 ). This is a difficult problem to fix and may require skin grafting to ameliorate the problem. In cosmetic patients, this may not be an acceptable option, so supportive measures with aggressive lubrication should be initiated.