Fig. 1.1
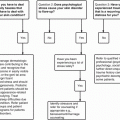
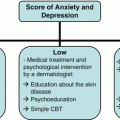
Role of Stress in neuroimmunological response
Psychoineuroimmulongy
Psychoneuroimmunology, a relatively new field which relates to the study of complex and synchronous activation and interactions of behavioral, neural, endocrine, and immune systems leading to a successful defense response to an internal or external challenge including psychosocial stress. This intriguing phenomenon explains that immune system is rather one part of a multisystem response of a body challenged by an internal or external threat or psychological stress. This multisystem interplay that initiates and orchestrate a defense response helps us understand the complexities and intricacies of stress and adaptation of a body to it and how imbalance caused by severe or continual stress in can be detrimental to physical and mental wellbeing (Fig. 1.2).
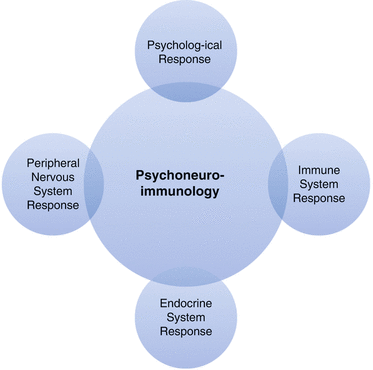

Fig. 1.2
A simple representation of psychoneuroimmunological response to a stressor
The intricate multidimensional workflow of central and peripheral nervous systems, endocrine and immune system when gets overwhelmed or gets disturbed by high level of stress it results in expression of a disease process, including skin diseases. These three systems while respond to stress on their own they also interact with each other to orchestrate a stress response. The interaction of these three systems prepare body and mind to adapt to the stess induced changes by utilizing a series of neuropetides, neurotransmitters, and neurohormones. While stress affects a person at different levels, stress can impact each and every cell and organ in a body. Skin being the most outer, biggest and most innervated organ can show the burden of stress in most obvious way. Stress plays amajor role in the pathogenesis and expression of many skin diseases and dermatological diseases can appear de novo or relapse in response to psychological stress. Skin and brain both share an embryological origin from the single layer of germinal cells; the ectoderm. A specialized population of multi-potent cells known as neural crest cells emerge from the junction of neural and surface ectoderm; these cells can develop in different types of cells like epidermis, sympathetic nervous system, peripheral sensory neurons, and melanocytes [2] under the influence of neurotrophins such as nerve growth factor and other chemical signals that attract or dispel certain cells, ensuring growth and expansion of the sensory peripheral nerve cells, ganglion, and interconnection between the neuronal system within different organs and in skin in the right direction [3, 4].
The complex relationship between stress and skin disease can not be fully explained unless we understands the mecahnisms by which the body responds to stress at macro and micro levels.
Nervous System Response to Stress
Central nervous system (CNS) modulates the immune response to stress via three distinct mecahnisms; activation of hypothalamic-pituitary-adrenal axis (HPA axis) and autonomic nervous system (ANS) and modulation of microglia on local level. This two prong activation of ANS as well as HPA axis ensures a prompt yet sustained respose to a particular stress stimuli as long as it is needed. Both of these systems work in-synch to each other in a bidirectional way to maintain the equilibirium in the stess response and to rheostat the intensity and duration of immune response [5]. Initiation of both of these pathways also leads to production of biologically active molecules that in turn can interact with immune cells directly and cn further modulate the stress immune respose [5].
ANS activation starts the releases of norepinephrine from the adrenal cortex. Most of the organs are innervated with noradrenergic postganglioning nerver fibers and lymphoid argans are no exception. Primary and secondary lymphoid organs like spleen, thymus, bone marrow, mucosal lymph glands and lymph nodes are activated through release of norepinephrine via peptidergic nerve fibers. The sympathetic innervations generally follow a similar pattern in different tissues. The nerve fibers are more dense in T-cell zones as compared to the B-cell zone. These nerve fibers makes neuroeffector junctions with lymphoid cells like macrophages to exert effect on immune systems. It has been known that any inturruption of this pathway can lead to impairment in immune response [5]. The function of sympathetic innervation is to modulate the innate immune response in such a way that a specific immune response is in proportion to the stimulus strength and not to continue beyond what is needed. The noradrenergic innervated areas within the lymphoid cells are also rich with neuromoulatory neuropeptides like somatostatin, substance P, neuropeptide Y, calcitonin gene-related peptide, opiate peptides, and vasoactive intestinal peptide [5, 6].
The release of norephnephrine within lyphoid cells can activate different receptors like β- adrenergic receprtors to influence the direction of stress response in certain way thus fine tunning the immune response to a particular offender. Norepinephrine has shown to modulate immune resonse by modulating thymocyte mitogenesis, lymphocyte proliferation in some lymph nodes, cell expression of antigens, antibody response, deters complement activation, and inhibits macrophages mediated lysis of certain cancerous or infectious cells. Lymphoid tissues have catecholamine and various neuropeptide-specific receptors. Catecholamines and other neurotransmitters released from nerve fibers can activate theses receptors and can modulate the immune response via intracellular signals influencing a particular cell line proliferation, antibody and cytotoxin production etc. This can lead to vasodilation and adhesions of leukocytes which can further modulate local inflammatory response in response to stress Watson and Nance [6].
The third pathway the CNS mediated stress response is through microglia that are inactive or resting magrophages found all over the brain and spinal cord. In response to a stress stimuli, these resting microglia can become active. Activation of microglia can leas to expression of cell-surface markers such as major histocompatibility complex (MHC) molecules, complement receptors, and CD4 cells. Microglia then morphologically change to become active phagocytes. These microglia/macrophages are weak phagocyt when compared to the peripheral macrophages. However, when over activated they release certain pro-inflammatory cytokines such as platelet-activating factor, reactive oxygen molecules, and nitric oxide that can lead to neuronal injury [6].
Endocrine Response to Stress
The endocrine system plays a vital role in maintaining homeostatis in response to acute or chronic stress. The relationship of stress and disease expression in different organ system is well established. The HPA is a multilevel endocrine system playing the central role in defending body from stessful stimuli. Stress response starts from the hypothalamus leading to a synchronized activation or down regulation of pituitary and adrenal glands which is the vital system of body to respond and adapt to all kinds of stress. HPA axis have a cause and effect relationship with many skin diseases. When HPA axis is looses its ability to maintain basal and stress related homeostasis it can results in disease expression especially in skin diseases [7].
At the anterior pituitary gland the stress response is co-mediated by arginine vasopressin (AVP) and other nonapeptides. Corticotropin releasing hormone (CRH) and AVP are secreted in near synchronized pulses, inducing the secretion of adrenocorticotropin hormone (ACTH) [7]. Stress triggers CRH release from the hypothalamus in starting hormonal cascade of HPA axis. CRH receptors has a wide distribution of in various neural circuits like limbic system, and sympathetic arousal system both in the brain and spinal cord. Once these receptors are stimulated it leads to a well-coordinated chain of events including physiologic, behavioral changes like changes in appetite, arousal, sexual and activity levels Kyrou and Tsigos [7].
The CRH stimulate secreation of ACTH in a diurnal fashion with highest peak secreations occuring between 6:00 AM to 8:00 AM and lowest trough happening at midnight. This diuranal pulse secretion of ACTH is greatly affected by levels of stress. ACTH exerts its action by binding with melanocortin receptors 2 (MC2) found in all three layers of adrenal cortex, stimulating adenyl cyclase and generating cAMP that activates downstream enzyme pathways in steroidogenesis [7] Glucocorticoid synthesis mainly takes place in the zona fasciculata of the adrenal cortex; this in turn is responsible for initiating the negative feedback loop to put a brake to the stress response at the level of suprahypothalamic centers, hypothalamus, and pituitary gland.
This self-regulatory stress response cycle prevents adverse consequences of prolonged adaptive changes such as catabolism and immunosuppression [7]. When stress is chronic and unrelenting the self regulatory negative feedback does not occur leading to continual hypersecretion of CRH, perpetuating a constant activation of HPA-axis. The constant excitation of HPA-axis result is a syndromal state characterized by behavioral disturbances such as depression, anxiety disorders, eating disorders as well as many systemic sequelae that include central obesity, hyperthyroidism, diabetes mellitus, metabolic syndrome, osteoporosis, atherosclerosis, immunosuppression, and increased susceptibility.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree