Fig. 21.1
Vicious cycle: stress responsible for the onset and exacerbation of psoriasis and psoriasis causes psychological stress
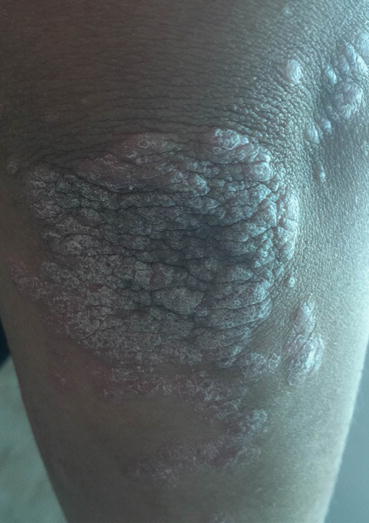
Fig. 21.2
Erythematous and violaceous scaly plaque of psoriasis over the elbow in a skin of color patient
Patients with psoriasis may experience different symptoms that include itching, irritation, burning and stinging, sensitivity, pain and bleeding [6]. The etiology of psoriasis is not fully understood. It is considered a multifactorial disease that involves both genetic environmental influences. Among these factors, stress has been considered as an important role in the onset and exacerbation of psoriasis [7]. Psychological stress may be also a consequence of psoriasis. The psychosocial impact of this disease is greatest among women, young people and minorities [8, 9] (Fig. 21.1).
Stress and Psoriasis
Stress has been reported to be a trigger for many dermatologic conditions including acne, urticaria, atopic dermatitis among others [10–12]. Patients with these conditions usually report a close chronologic association between the stressful event and the exacerbation of the skin condition. Like many other dermatological diseases, psoriasis can also worsen with stress [7].
A study performed with a large sample of Nordic patients investigated the perceived influence of stress on psoriasis onset and disease severity and compared stress reactors and non-reactors with respect to psoriasis-related stress, disease severity, family history of psoriasis and socio-demographic factors. Seventy-one percent of 5795 members of the Nordic psoriasis association and 66 % of 702 patients recruited from Nordic dermatologists or university clinics reported that their psoriasis was exacerbated by stress, and 35 % in both groups reported that the onset of their psoriasis occurred during a stressful period. Patients experiencing higher levels of stress also reported greater disease severity, psoriasis-related stress and impairment of disease-related quality of life. Interestingly, these patients also reported more frequent use antidepressants, tranquillizers and tobacco. And they were more likely to have a family history of psoriasis [13]. Two prospective studies performed by Verhoeven et al. and Evers et al. showed that higher level of stress experienced by patients modulated the disease course. Daily stressors were associated with increased Psoriasis Area and Severity Index (PASI) scores as well as more complain of itch [14, 15]. Malhotra et al. [16] evaluated the stressful life events within 1 year preceding onset or exacerbation lesions in 50 patients of psoriasis vulgaris and 50 patients chronic urticaria. These patients were examined clinically and administered Gurmeet Singh’s presumptive stressful life events scale. The researchers found the presence of Stressful life in 26 % of the patients in the psoriasis vulgaris group and 16 % of the patients in the chronic urticaria group within 1 year preceding onset or exacerbation of skin disease. Among patients with psoriasis, the most common stressful life event reported was financial loss or problems (8 %), followed by death of close family member (4 %), sexual problems (4 %), family conflict (2 %), major personal illness or injury (2 %), and transfer or change in working conditions (2 %), failure in examinations (2 %), family member unemployed (2 %), illness of family member (2 %), getting married or engaged (2 %), miscellaneous (2 %). It is interesting to observe, that the experience of a stressful event is subjective. An event like getting married or engaged can be positive for some individuals but cause a significant amount of stress to others.
Immune regulation plays an important role in the development of psoriatic lesions. Early studies focused on understanding of psoriasis as a T lymphocyte mediated autoimmune condition with the production of cytokines, T helper (Th1) cells, interferon (IFN)-γ and tumor necrosis factor (TNF)-α [17]. More recently studies focus on the Th17 cytokine network including interleukin (IL) 17 and IL23, as a central role for the deployment of this disease [18]. Maese, explains that in genetically predisposed individuals, internal or external factors that include biomechanical stress and or immunologic dysregulation increased the expression of IL23 and this stimulates the differentiation and activation of Th17, and induces their production of IL-22, which regulates proliferation and differentiation of keratinocytes. Activated Th17 cells leads to increased levels of IL-17 and these are responsible for attracting neutrophils to the tissue site [17, 19, 20]. The hypothalamic-pituitary-adrenal axis (HPAA), which may be dysregulated in these patients, is one potential mediator of the stress and psoriasis [21]. Loite et al. have performed gene expression analysis studies and found an increased expression of HPAA mediators in lesional and non-lesional psoriasis skin samples compared to normal skin samples [21, 22]. Richards et al. performed a study with forty patients and found that stress responsive patients exhibit an altered HPAA response to acute social stress [23]. Karanikas et al. performed a study with the objective of investigating any alteration of the neuroendocrine profile of psoriatic patients through stimulation of the hypothalamic-pituitary-adrenal axis with corticotropin releasing hormone in 40 patients with psoriasis comparing to a control group of also 40 patients. Contrary to previous studies they found no particular neuroendocrine profile of HPAA axis responsiveness [24]. More studies are needed to clarify the role of the HPPA axis as a mediator of stress and psoriasis.
Oxidative Stress
In the recent years, studies have been suggesting that compromised function of antioxidant system and increased reactive oxygen species (ROS) production are involved in the pathogenesis of psoriasis. Kadam et al. performed a study with 90 psoriasis patients and compared with 30 healthy controls. The researchers investigated serum levels of malondialdehyde, nitric oxide end products and the activities of antioxidant enzymes such as erythrocyte-superoxide dismutase, catalase and total antioxidant status. They found increased serum malondialdehyde, nitric oxide end products with decrease in erythrocyte-superoxide dismutase activity, catalase activity and total antioxidant status in patients with psoriasis. This study showed a possible relation of psoriasis and the enhancement of Reactive Oxygen Species production and a decreased antioxidant potential [25].
The relationship between smoking-induced oxidative stress and the clinical severity of psoriasis was investigated by Attwa et al. [26] These researchers found that smoking-induced oxidative damage that results from increased reactive oxygen species production along with insufficient capacity of antioxidant mechanisms could be involved in the pathogenesis of psoriasis. Urinary biopyrrin levels have been studied as an indicator of oxidative stress in patients with psoriasis. A study published in 2016 involving 85 patients, being 55 cases with chronic plaque psoriasis and a control group with 30 age, gender and body mass index-matched normal subjects measured urinary biopyrrin levels using enzyme immunoassay. The study found increased levels of biopyrrins in patients with psoriasis, and this level was correlated with the disease severity. Further studies are needed to validate this finds as well to understand the clinical usefulness of antioxidants for patients with psoriasis [27].
Psychological Stress as a Result of Psoriasis
Psoriasis is probably the most widely studied psychodermatological disorder due to its association with stress and having strong psychosocial impact on patients’ lives. Psoriasis has higher associations with psychiatric illness than do other dermatologic conditions. Despite the visible evidence for psychiatric morbidity in patients with psoriasis, most guidelines for the treatment of psoriasis do not include screening for anxiety and depression and other psychosocial parameters. Numerous instruments could be used to evaluate psychiatric comorbidity among psoriasis patients. Skindex-29, particularly its emotions and functioning scale, general health questionnaire and dermatological HRQoL (health related quality of life) are the most common instruments used in the evaluation of psychosocial impairment in psoriasis and many other psychodermatologic disorders.
Social stigmatization, rejection by the family and friends with consequent profound effect on self-confidence, self-image and sense of well being are most commonly seen in psoriasis patient. Sampogna et al. [28] conducted a study on 936 patients to evaluate the psychosocial functioning of psoriasis patients. The authors concluded the most common psychosocial problems experienced by psoriasis were shame, anger, worry, difficulties in daily activities and social life. Patients with psoriasis suffer from depression frequently and it is estimated to be up to 30 % [29]. Various studies have demonstrated significant depression, worries and suicidal ideations in psoriasis patients. A United Kingdom based cohort study of patients with psoriasis demonstrated increased incidence of diagnoses of depression, anxiety and suicidal ideations. The authors estimated that over 7 % diagnoses of depression, about 5 % diagnoses of anxiety and 0.3 % diagnoses of suicidality are attributable to psoriasis each year [30]. A recent Danish study found limited evidence to suggest an increased risk of self-harm and non-fatal suicide attempts in psoriasis patients [31].
Generally psychiatric comorbidity in psoriasis patients runs parallel with disease severity, however many studies have demonstrated that although psoriatic lesions were cleared by various treatment approaches, anxiety, depression, persistent worrying remained either same or decreased to some extent but not completely. This lack of correlation between psychological impact and physical severity has been explained by Kimball et al. [32] They suggest that the lack of correlation in some patients may be due to the cumulative impact of living with psoriasis. Some authors suggest that the maintenance of distress is related to maladaptive coping responses and schemas [33]. On the other hand lower levels of distress have been reported with longer disease duration indicating psychological acceptance or reflecting long-term adaption [34]. Kleyn et al. [35] conducted a FMRI study which demonstrated reduced signal responses to disgusted faces in psoriasis patients compared with controls. The authors hypothesize that patients with psoriasis develop a coping mechanism to protect them from stressful emotional responses by blocking the processing of disgusted facial expressions. A recent prospective cross-sectional study [36] on Singaporean patients demonstrated significant psychiatric comorbidity in psoriasis patients. The authors reported anxiety disorder in 17 %, while a depressive disorder was suggested in 15 % of the study population.
Besides stigmatization and social isolation and rejection, patient with psoriasis have also difficulties with relationships. The family members of patients with psoriasis were interviewed by Eghlileb et al. 57 % of family members reported psychological distress, 55 % social disruption, 44 % limitations to leisure activities and 37 % reported deterioration of close relationships [37]. Sexual functioning in psoriasis has been studied in many cross-sectional surveys. Gupta and Gupta [38] conducted a cross sectional survey on 120 inpatients. 40 % reported decline in sexual activity since the onset of psoriasis. In another study conducted by Sampogna et al. [39] reported about 35 % of patients with psoriasis confirmed impaired sexual life secondary to psoriasis. Increased prevalence of erectyl dysfunction was reported in study of 92 patients. The psoriasis patients were matched with controls with other skin conditions. The authors reported prevalence of erectly dysfunction in 58 % of patients with psoriasis as compared to 49 % of patients with other skin diseases [40]. Substance abuse is fairly common but under-reported in patients with psoriasis impairing social life and affecting treatment. Mills et al. [41] reported that twice as many patients with psoriasis smoked compared to controls. Another study [42] found that alcohol exacerbated psoriasis severity and pruritus and impaired treatment response.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree