Fig. 34.1
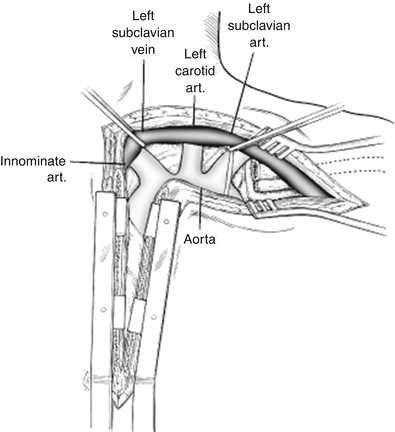
The anatomy of the thoracic outlet showing the relations of the subclavian vessels
The Subclavian Artery
On the right side, the subclavian artery arises from the innominate artery behind the sternoclavicular joint; on the left, it comes directly from the arch of the aorta. Each subclavian artery is divided into three parts for descriptive purposes. The first part extends from its origin to the medial border of the scalenus anterior muscle, the second part lies behind this muscle, and the third part extends from its lateral border to the outer aspect of the first rib where it becomes the axillary artery. The first parts of the right and left subclavian arteries differ with respect to course, length, and relation to neighboring structures and require separate descriptions. The second and third parts of the two arteries are essentially similar and will be described together:
First Part of the Right Subclavian Artery
Arising from the innominate artery behind the right sternoclavicular joint, it passes in a superolateral direction to the medial border of the scalenus anterior muscle. The extent to which it ascends above the clavicle varies. This can influence the ease with which it can be accessed via a supraclavicular incision. It is covered anteriorly by the skin, superficial fascia, platysma muscle, deep fascia, the clavicular head of the sternocleidomastoid muscle, and the sternohyoid and sternothyroid muscles. It is crossed by the internal jugular and vertebral veins, the vagus nerve, and a loop of the sympathetic trunk. Posterior and inferior lie the pleura and apex of the right lung as well as the sympathetic trunk and first thoracic vertebra. The recurrent nerve winds around its inferior and posterior aspect.
First Part of the Left Subclavian Artery
This arises from the aortic arch posterior and lateral to the left common carotid artery and ascends to the root of the neck and then inclines laterally to the medial border of the scalenus anterior muscle. Its anterior relations are similar to the right side and posteriorly lies the esophagus and thoracic duct. Medially lie the esophagus, trachea, thoracic duct, and left recurrent nerve. Laterally, the left pleura and lung are to be found.
Second Part of the Subclavian Artery
This lies behind the scalenus anterior muscle, is short, and is the most superiorly located part of the vessel. The phrenic nerve runs from lateral to medial over the muscle. Posterior to the vessel are the scalenus medius muscle and pleura, superior the brachial plexus, and inferior the pleura. The subclavian vein lies below and in front of the artery, separated from it by the scalenus anterior muscle.
Third Part of the Subclavian Artery
This part runs in an inferolateral direction from the lateral border of the scalenus anterior muscle to the outer aspect of the first rib where it becomes the axillary artery. It is covered by the skin, platysma muscle, supraclavicular nerves, and the deep cervical fascia. The external jugular vein and tributaries cross the anterior and medial to it. The distal part of the artery lies behind the clavicle and the subclavius muscle, with the subclavian vein anterior and at a slightly lower level than the artery. Posteriorly lies the brachial plexus which intervenes between the artery and the scalenus medius muscle. Superiorly and to the lateral side are the upper trunks of the brachial plexus and the omohyoid muscle and inferiorly the first rib.
34.1.1 Branches of the Subclavian Artery
First Part:
Vertebral artery:
Internal mammary artery
Thyrocervical trunk
Second Part:
Costocervical trunk
Third Part:
Dorsal scapular artery
34.1.2 Anatomical Anomalies:
The right subclavian artery can arise as a separate trunk from the arch of the aorta as the first, second, third, or last branch of the arch.
If it arises as the last branch, it passes from left to right behind the trachea, esophagus, and right carotid or sometimes between the trachea and esophagus.
It can pass anterior to the scalenus muscle, perforate it, and can ascend as high as 4 cm above the clavicle.
The left subclavian artery generally does not reach as high in the neck as the right.
34.1.3 The Subclavian Vein
The subclavian vein is a continuation of the axillary vein, extending from the outer aspect of the first rib to the manubrial head of the clavicle. Here it unites with the internal jugular vein to form the innominate vein behind the manubrio-clavicular joint. Its relations are as follows: anterior, the clavicle; posterosuperior, the subclavian artery separated by the phrenic nerve and the scalenus anterior muscle; and inferior, the first rib and the pleura.
34.2 Clinical Presentation, Preoperative Care, Diagnosis, and Management Principles (Fig. 34.2)
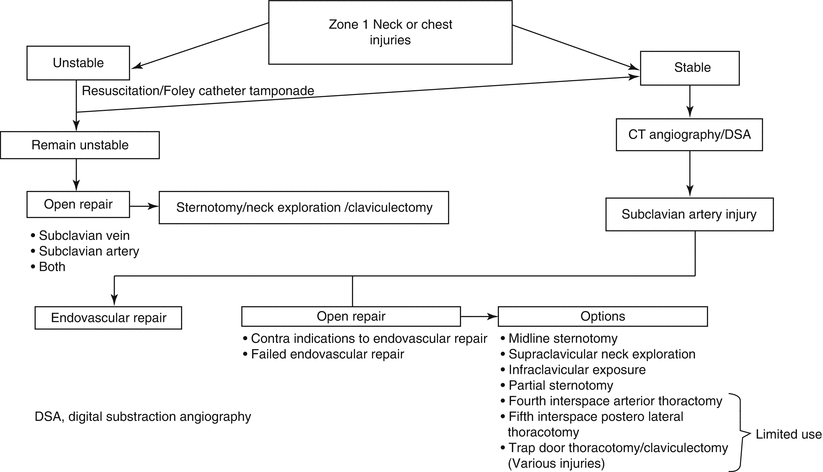
Fig. 34.2
Algorithm for the treatment of patients with potential subclavian vessel injuries
Patients with subclavian vessel injuries can present in hypovolemic shock with active bleeding or in a stable condition with a Zone I or II neck or infraclavicular anterior chest wounds. Zone I is defined as the area between the clavicle and the cricoid cartilage and Zone II the area between the cricoid and the inferior border of the mandible. Resuscitation should be managed according to ATLS guidelines and adjunctive measures to control active bleeding include Foley catheter tamponade (Fig. 34.3) and manual compression. If local control cannot be achieved or if the patient bleeds into the pleural cavity as evidenced by continuous blood loss from a chest drain, the patient should be transferred to the operating room immediately. In this case, we prefer a midline sternotomy, with appropriate extension, if needed, to provide access to most mediastinal and thoracic outlet structures. Stable patients or patients that remain stable after resuscitation should be evaluated for arterial injury. In the stable or stabilized patient, you should proceed to diagnostic imaging. Controversy exists with regard to routine investigation of these surface wounds if no significant other signs of arterial injury are present. We currently favor routine CT angiography to exclude arterial injuries. When hard signs of arterial injury are present, it allows assessment of the extent of the injury and planning of intervention. When only soft signs are present, it acts as a low morbidity screening investigation to exclude arterial injuries. If an arterial injury is diagnosed in this case, you should note the exact position and extent of arterial injury and evaluate the patient for endovascular or open surgery.
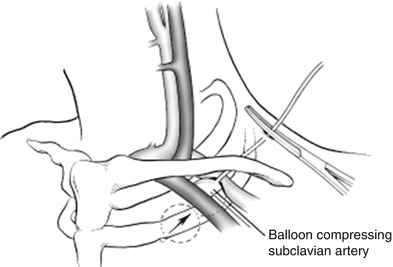

Fig. 34.3
Balloon tamponade controlling bleeding from an injured subclavian artery
In our practice, we prefer endovascular treatment by stent grafts whenever possible as we believe that it greatly benefits the patient by limiting surgical morbidity and mortality. The relative contraindications that can preclude endovascular management include clinical and angiographic factors. Clinical factors are active uncontrollable hemorrhage, critical limb ischemia, airway or brachial plexus compression, concomitant aero-digestive injuries, and infected wounds. Angiographic factors include excessive luminal discrepancy proximal and distal to the injury, an inability to traverse the lesion by guide wire, and a dominant vertebral artery on the injured side. Transfemoral endovascular management is our first choice if no contraindications are present.
If any of the above mentioned are present, consider open surgical repair. The basic approaches available for the exposure and proximal and distal control of subclavian vessel injuries include a full or limited upper median sternotomy, a supraclavicular incision, an infraclavicular incision, a limited anterolateral third-interspace thoracotomy, a full fifth-interspace posterolateral thoracotomy, a medial partial resection of the clavicle, and a trapdoor thoracotomy. The extent of the injury, pathology, the presence of a venous injury, the part of the vessel, and surgeon preference will dictate which approach or, more usually, combination of approaches to be used. In our practice, clavicle resection and trapdoor thoracotomy are very rarely used, only for subclavian vein injuries that cannot be controlled via any of the other approaches. This will usually be an extension of an existing sternotomy and supraclavicular or infraclavicular incision.
34.3 Surgical Exposures
34.3.1 Midline Sternotomy in the Unstable Patient with No Diagnostic Imaging (Fig. 34.4)
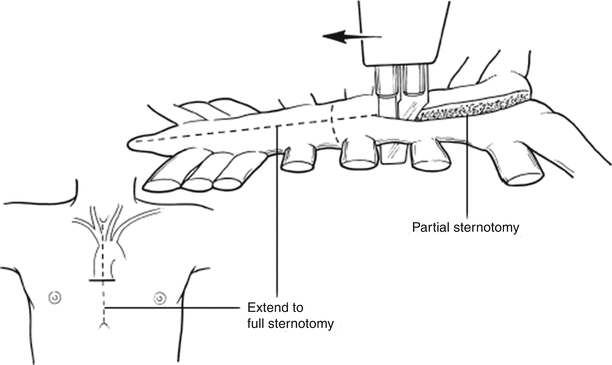
Fig. 34.4
Upper mediastinal access via a partial or full midline sternotomy
Here the source of bleeding could be from a number of large vessels in the mediastinum and thoracic outlet, or even from the heart. In this scenario, it is best to position the patient for a midline sternotomy with a small sandbag between the scapula, with the ipsilateral arm in 30° lateral abduction, allowing for the manipulation of the thoracic outlet and better access to the distal subclavian/proximal axillary arteries. If time permits, it is prudent to clean a proximal thigh for harvesting saphenous vein, should this be required.
This preparation should be effected within minutes. It is also a good practice to ascertain that a working pneumatic saw and a vascular instrument tray are available in the operation room. While pressure on or in the wound is maintained, you can, with good suction and two Langenbeck retractors, coordinate the release of pressure and a “quick peep” into the wound can sometimes be of value. A visible vessel (subclavian or a large branch) can sometimes be glimpsed and clamped with one or two straight atraumatic vascular clamps. This should happen in seconds and you should not attempt more than two “peeps”; otherwise the patient is in danger of exsanguinating. With luck, control, or partial control, it can be achieved in this fashion. You can complete the procedure by formal supraclavicular neck exploration.
If control cannot be achieved in this way, the best option is to proceed to a midline sternotomy. A vertical midline incision is made from the suprasternal notch to 2 cm distal to the xiphoid process. You can extend the incision superiorly along the anterior border of the sternocleidomastoid muscle, or in the case of a true subclavian artery injury being identified, continue obliquely over the two heads of this muscle laterally about 2 cm above the clavicle for supraclavicular exposure. The sternal incision is deepened to the periosteum with electrocautery. In the sternal notch, deepen the midline space between the two sternal heads of the sternocleidomastoid muscles with a combination of sharp and blunt dissection. One or two large but unimportant veins may be encountered. Entry to the retrosternal space is effected with blunt finger dissection between the strap muscles, which implants on the posterior aspect of the sternum. Inferiorly the xiphoid is mobilized and a plane should be developed retrosternally, in an upward direction. The anesthesiologist should arrest ventilation in expiration (to prevent lung injury), and the sternum is divided in the midline using a pneumatic saw or Lebsche knife. Bleeding from the sternal edges is controlled by electrocautery and bone wax. The latter is used to prevent infection and impaired wound healing. Insert a sternal retractor and open it carefully, a few turns at a time to prevent sternal and rib fractures.
In the fully retracted position, a divided sternum reveals the structures of the anterior, superior, and middle mediastinum (Fig. 34.5). The thymus gland is encountered first. Divide it vertically to expose the left innominate vein that runs obliquely from the left to its confluence with its right-sided counterpart to form the superior vena cava. This vein can be mobilized by dividing its numerous tributaries, and exposure of the arch can thus be achieved without dividing it. In the emergency situation with active bleeding, you can divide it and ligate it without any morbidity. The aortic arch with the origin of the innominate artery and the left common carotid is now visible.
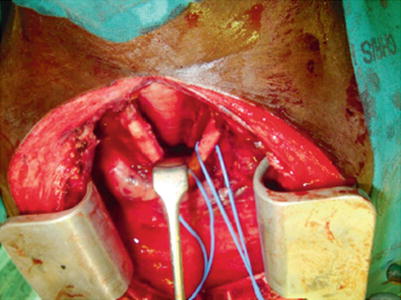

Fig. 34.5
The mediastinal structures exposed at sternotomy. Note blue vascular loops around both common carotid arteries. The trachea can be seen at the back between both vessels
On the right, the origin of the innominate artery at the aortic arch is identified and then carefully followed cranially for about 3–5 cm, where it will divide into subclavian and common carotid arteries. At this bifurcation, the right vagus nerve crosses the anterior to the first part of the subclavian artery and then descends into the mediastinum posterior to the right innominate vein. The recurrent laryngeal branch of the right vagus nerve loops around the inferior border of the subclavian artery and ascends medially in the neck between the trachea and the esophagus. When exposing and controlling the short first part of the right subclavian artery, take care to avoid injury to these nerves. In the event of overwhelming bleeding from the right subclavian artery, the origin of the innominate artery can be temporarily clamped to facilitate dissection with immediate transfer of the clamp upon exposure of the proximal subclavian artery. Take care in the case of the “bovine arch” where both the carotid arteries and the right subclavian artery originate from the innominate artery. This congenital anomaly is present in about 10 % of cases and can result in major brain damage if the innominate artery is clamped for any extended duration.
Depending on the rotation of the aortic arch, the origin of the left subclavian artery can vary from anterior to far posterior in the left half of the sternotomy wound (Fig. 34.6). In the latter situation, it can be difficult to get good exposure of this vessel and you should take care to avoid inadvertent clamping the left common carotid artery, thereby impeding cerebral blood flow. In the acute bleeding situation, the left pleural space can be entered before mediastinal dissection to facilitate compression of a subclavian artery, that is, bleeding into the pleural space. To locate the origin of the left subclavian artery, you should follow the aortic arch posterolaterally to the left past the origin of the left common carotid artery, taking care to prevent injury to the left vagus nerve as it descends between the carotid and left subclavian arteries to cross anteriorly over the left side of the aortic arch. The left recurrent laryngeal branch passes under the aortic arch and then courses medially to the tracheoesophageal groove.