Acne vulgaris presenting from birth to preadolescence can be confusing to diagnose and even more challenging to evaluate and manage. The differential diagnosis of acne varies by age and, in some cases (especially when it presents in midchildhood), deserves a thorough evaluation to rule out underlying systemic abnormalities. Acne management strategies, including factors affecting adherence to the treatment regimen, may be influenced by the patient’s age. This article presents an overview of the clinical presentations of acne by age and our approach to evaluation and management of this common condition.
Key points
- •
Neonatal acne, which may be clinically distinct from neonatal cephalic pustulosis, can present with true comedones.
- •
Infantile acne has the potential to cause scarring and may be a predictor of more severe adolescent acne.
- •
Midchildhood acne (ages 1–7 years) may herald the presence of a hyperandrogenic state (eg, underlying tumor, adrenal enzyme deficiency) and warrants prompt evaluation.
- •
Preadolescent acne presents at around 7 to 12 years of age; it is usually considered normal and may be the first sign of pubertal maturation.
Introduction
Rare is the patient who achieves adulthood without having had some degree of acne. Although the prevalence of acne may reach 95% in the adolescent population, acne should not be considered solely a teenage problem. In a poster presentation at the American Academy of Dermatology Annual Meeting (Boston, MA, August 2012), Sandoval and colleagues reported, as part of the National Ambulatory Medical Care Data Survey, some 55 million pediatric acne visits in a 6-year period. The data showed that neonatal/infantile acne compromised approximately 3% of visits overall; midchildhood acne accounted for 0.9% of cases; and preadolescent acne constituted 4.8% of total acne visits. In contrast with neonatal acne, for which pediatricians treated approximately 75% of cases, pediatricians and dermatologists treated preadolescent acne cases almost equally (38% and 34% of cases, respectively).
Managing patients with pediatric acne can be a challenge in daily clinical practice. The wide spectrum of differential diagnoses, the possibility of underlying systemic disorders, and the potential for side effects from medications demand vigilance and should incite humility from even the most seasoned acneologist. However, acne management in this population comes with great reward for patients and providers alike. This article provides a practical approach to acne, reviewing the current perspectives on underlying causes, evaluation, and treatment from birth to preadolescence ( Fig. 1 ).
Introduction
Rare is the patient who achieves adulthood without having had some degree of acne. Although the prevalence of acne may reach 95% in the adolescent population, acne should not be considered solely a teenage problem. In a poster presentation at the American Academy of Dermatology Annual Meeting (Boston, MA, August 2012), Sandoval and colleagues reported, as part of the National Ambulatory Medical Care Data Survey, some 55 million pediatric acne visits in a 6-year period. The data showed that neonatal/infantile acne compromised approximately 3% of visits overall; midchildhood acne accounted for 0.9% of cases; and preadolescent acne constituted 4.8% of total acne visits. In contrast with neonatal acne, for which pediatricians treated approximately 75% of cases, pediatricians and dermatologists treated preadolescent acne cases almost equally (38% and 34% of cases, respectively).
Managing patients with pediatric acne can be a challenge in daily clinical practice. The wide spectrum of differential diagnoses, the possibility of underlying systemic disorders, and the potential for side effects from medications demand vigilance and should incite humility from even the most seasoned acneologist. However, acne management in this population comes with great reward for patients and providers alike. This article provides a practical approach to acne, reviewing the current perspectives on underlying causes, evaluation, and treatment from birth to preadolescence ( Fig. 1 ).
Pediatric physiology
The stereotypical timing of pediatric acne onset reflects physiologic changes that normally occur as people develop from fetus to teenager. Starting in utero and continuing until about the first 6 to 12 months of life, both boys and girls produce high levels of dehydroepiandrosterone (DHEA) and its sulfated form (DHEAS), the result of a prominent zona reticularis in the fetal adrenal glands, which leads to stimulation of sebaceous glands. In addition, boys during this time show increasing levels of luteinizing hormone (LH) and secrete high levels of testicular testosterone, helping to explain why acne occurs more frequently in boys than in girls during the first year of life. At around 1 year of age, hormonal activity decreases with progressive involution of the fetal adrenal glands, highlighting that new-onset or persistent acne in this age group warrants evaluation for a more serious underlying medical disorder. With normal onset of adrenarche at around 7 years of age, DHEAS levels increase once again. This change correlates with the emergence of preadolescent acne, which may be the first sign of pubertal maturation.
Neonatal acne
Neonatal acne may be present at birth or appear shortly thereafter, usually during the first 4 to 6 weeks of life ( Table 1 ). Most commonly seen in boys, neonatal acne has been reported to affect up to 20% of newborns, although it is not certain that all these eruptions are true acne. Clinical presentation within this age group is likely associated with several causal factors: increased sebum production, hormonal stimulation of sebaceous glands by both maternal (primarily through the placenta rather than via lactation) and neonatal androgens, and colonization of sebaceous glands by lipophilic species of the genus Malassezia .
| Differential Diagnosis | Neonatal cephalic pustulosis; infectious agents; transient neonatal pustular melanosis; nevus comedonicus; erythema toxicum neonatorum; sebaceous gland hyperplasia; milia; miliaria; maternal medications (eg, lithium, phenytoin, corticosteroids); congenital adrenal hyperplasia; virilizing tumor; other underlying endocrinopathy |
| Age at Onset | In utero to ∼6 wk |
| Morphology | Comedones Inflammatory papules Pustules Nodules/cysts Scarring |
| Distribution | Forehead Cheeks Nose Less commonly: neck, chest, back |
| Clinical Pearls |
|
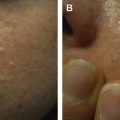
The presence of small closed comedones typically limited to the face (forehead, nose, and cheeks) confirms the diagnosis of true neonatal acne. These acneiform lesions may progress to more extensive inflammatory forms with erythematous papules, pustules, and scarring cysts over the neck and upper trunk ( Fig. 2 ).
A topical retinoid with or without benzoyl peroxide is typically all that is needed to help treat true neonatal acne. Referral to a pediatric dermatologist is warranted if acneiform lesions persist, especially in the clinical setting of scarring. In those rare cases when the diagnosis is unclear, a thorough family history helps to rule out an underlying acneiform drug reaction, and laboratory investigations may occasionally be required to exclude infectious causes. When an underlying cause of true virilization, such as congenital adrenal hyperplasia or virilizing tumor, is suspected a careful physical examination that includes developmental and growth parameters, blood pressure, and investigation for additional signs of hyperandrogenism, like precocious sexual maturation, should be performed. Complementary work-up assessing adrenal function and androgen excess with DHEAS and free testosterone, usually directed by or in conjunction with pediatric endocrinology, is recommended in these rare cases.
Differentiating true neonatal acne from the entity called neonatal cephalic pustulosis (NCP) remains controversial, because the two terms have historically and confusingly been used interchangeably. NCP generally appears within the first several weeks of life as a mild inflammatory papulopustular eruption, primarily localizing to the forehead, eyelids, cheeks, and chin; less commonly, NCP may also involve the scalp, neck, chest, and upper back. NCP has been reported to be a transient disorder that occurs in up to 25% of newborns and often resolves spontaneously, typically without scarring, in days to weeks. The absence of true comedones, either closed or open, in NCP is a useful distinctive clinical feature.
Malassezia species ( Malassezia furfur , Malassezia globosa , and Malassezia sympodialis ), a normal flora of infant skin, have long been suspected of playing a causative role in the development of NCP. Given the presence of this yeast in lesional skin smears of affected infants, some studies suggest an association between cutaneous colonization with Malassezia and the pustular condition in newborns. However, not all patients with NCP have positive microbiological findings for Malassezia . In addition, not all culture-positive neonates develop NCP-like skin lesions. Ayhan and colleagues found no significant differences in skin colonization with Malassezia between patients with NCP and healthy neonates. One plausible explanation for these findings is that NCP may be a hypersensitivity response to the presence of the yeast in predisposed individuals rather than a pathologic disease caused by an increase in the number of microorganisms. Alternatively, other pustular eruptions of the neonate may present similarly to Malassezia -associated NCP, which may confound the reported results.
Because of its typical self-limited course, aggressive treatment of NCP is often not required. Application of topical ketoconazole cream has been reported to expedite clearance of lesions and reduce fungal colonization; however, more rigorous investigations are necessary before formal, evidence-based recommendations can be made.
Infantile acne
Infantile acne typically begins between 6 weeks to 1 year of life ( Table 2 ). Lesions consist of closed and open comedones, inflammatory papules, and pustules, primarily localizing to the face and, less commonly, to the chest and back. Severe cysts leading to scarring may be present ( Fig. 3 ). Exceptional cases of acne conglobata with large sinus tracts and keloid scars have also been reported among this age group. More than 80% of patients experience only a mild to moderate course that resolves spontaneously by 1 or 2 years of age; however, infantile acne may have an unpredictable course with active lesions lasting for several years, even up to puberty, and may be a predictor of more severe adolescent acne.