Non-surgical rejuvenation of the periorbital area is becoming increasingly popular given the downtime and risks associated with surgical procedures. Dermabrasion and chemical peels were first used along with neuromodulators and dermal fillers. Over the past few decades, laser treatments have emerged as the gold standard for periorbital skin resurfacing. The laser treatments are categorized by ablative and non-ablative lasers and further subcategorized into fractionated and non-fractionated lasers. Radiofrequency-based devices have also emerged as a beneficial non-surgical treatment for the periorbital area. Within this section, the authors explore the various non-surgical treatments for periorbital rejuvenation.
Key points
- •
Non-surgical management of the periorbital area is becoming increasingly popular as it provides an avenue for improvement without the downtime or side effect profile of traditional blepharoplasty.
- •
The gold standard of non-surgical periorbital rejuvenation is fully ablative carbon dioxide (CO 2 ) or erbium lasers.
- •
Fractionated lasers and non-ablative lasers have less downtime and fewer side effects than fully ablative lasers, making them an appealing alternative for patients.
- •
Neuromodulators, dermal fillers, dermabrasion, chemical peels, and radiofrequency-based devices can lead to mild to moderate improvement for periorbital aging.
Introduction
The periorbital region is the one of the earliest to show visible signs of aging. Periorbital skin aging is caused by both intrinsic and extrinsic factors. Degradation of collagen and elastic fibers, vascular and fat atrophy, and reduced epidermal thickness lead to skin laxity, dermatochalasis, rhytides, textural changes, and telangiectasias. , Structurally, there is volume loss from fat pad atrophy and bone resorption, resulting in a hollowed appearance. Genetics play a role as well. Extrinsically, ultraviolet (UV) radiation is the primary driver for periorbital aging. UV exposure hastens the degradation of collagen resulting in textural changes in the periorbital skin. ,
The periorbital area is a marker of age, emotion, and character traits. , Studies show that those with aged periorbital skin are perceived with more negative character traits. A study by Boonipat and colleagues demonstrated that patients treated with surgical blepharoplasty were rated more highly in terms of attractiveness, trustworthiness, sociability, health, and capability than preoperative controls. Thus, the periorbital region is often the target for skin rejuvenation as patients seek to look younger, more attractive, and warmer. ,
The eyelid skin is the thinnest in the body. It can be as thin as 800 μm. Historically, surgical intervention has been the gold standard of therapy. Surgical blepharoplasty is one of the most common procedures for periorbital rejuvenation. Given the downtime and potential risks associated with surgical intervention, non-surgical techniques are becoming increasingly popular for periorbital rejuvenation.
Neuromodulators, dermal fillers, dermabrasion, and chemical peels have been used for many years for facial rejuvenation. Since its introduction in the late 1980s, the CO 2 laser has remained the gold standard for periorbital rejuvenation. , Other laser and energy-based technologies that have emerged include fractionated and non-ablative lasers and radiofrequency-based devices. In this section, the authors will explore non-surgical management of the periocular area.
Discussion
Neuromodulators
The neuromodulators utilized in facial rejuvenation are derived from botulinum toxin A. Botulinum toxin A binds the neuronal presynaptic membrane at the neuromuscular junction where it is internalized via endocytosis and translocated to the neuronal cytosol. Cleavage of the soluble N-ethylmaleimide sensitive factor activating protein receptor protein synaptosomal-associated protein of 25 kDa prevents acetylcholine release. This chemical denervation process takes about 24 to 48 hours; this is when the first effects will be noticed on the muscles. The neuromodulating effect lasts 2 to 6 months.
Neuromodulators can be utilized to improve periorbital rhytides and mild skin laxity. , While the development of rhytides is multifactorial, the movement of the orbicularis oculi muscle plays a central role. The orbicularis oculi is responsible for eyelid closure, both involuntary and voluntary movements. The main depressors of the eyebrow are the orbicularis oculi, procerus, corrugator supercilli, and depressor supercilli. By targeting the eyebrow depressors, the depressor contraction will diminish, and the eyebrow will lift. In general, treating the glabellar complex and the lateral superior orbicularis oculi will elevate the eyebrow. The primary elevator of the eyebrow is the frontalis muscle. Providers need to be cautious of the frontalis in older individuals as the frontalis acts as an elevator. If a patient recruits their frontalis muscle to assist with upper eyelid elevation, the frontalis should not be paralyzed as this can lead to upper eyelid hooding. Eyelid ptosis can occur if the neuromodulator inadvertently disperses to the levator palpebrae superioris muscle.
Types of neuromodulators used for periorbital rejuvenation.
- a.
Onabotulinumtoxin A (Botox)
- b.
Abobotulinumtoxin A (Dysport)
- c.
Incobotulinumtoxin A (Xeomin)
- d.
Prabotulinumtoxin A (Jeaveau)
- e.
Daxibotulinumtoxin A (Daxxify)
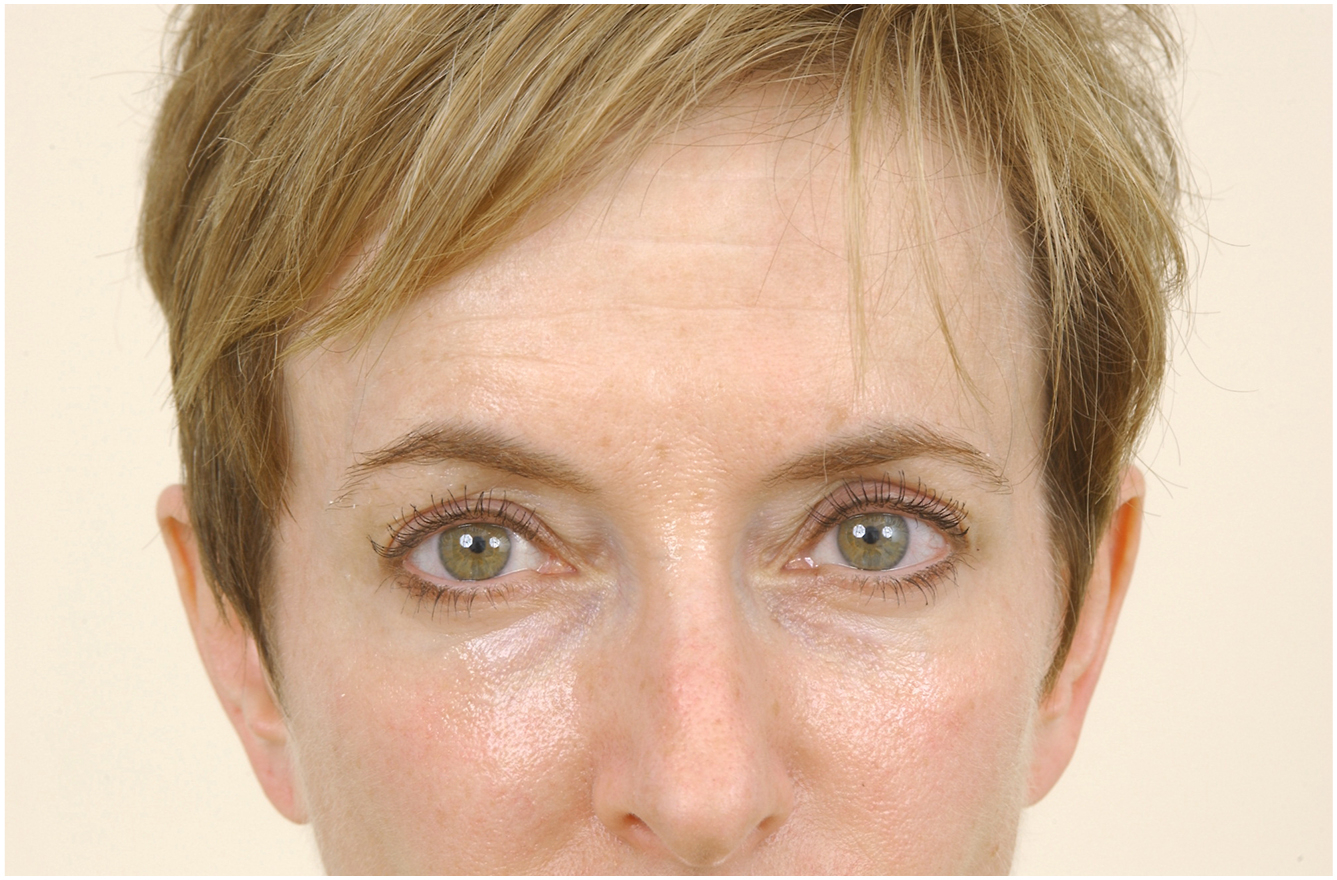
All of the neuromodulators are effective but not interchangeable. They are different in terms of reconstitution, dosage, and placement. Neuromodulators are beneficial in that they are less invasive and less expensive than surgical blepharoplasty and laser treatments. On the other hand, their effect is temporary, so repeated treatments are needed ( Figs. 1 and 2 ).

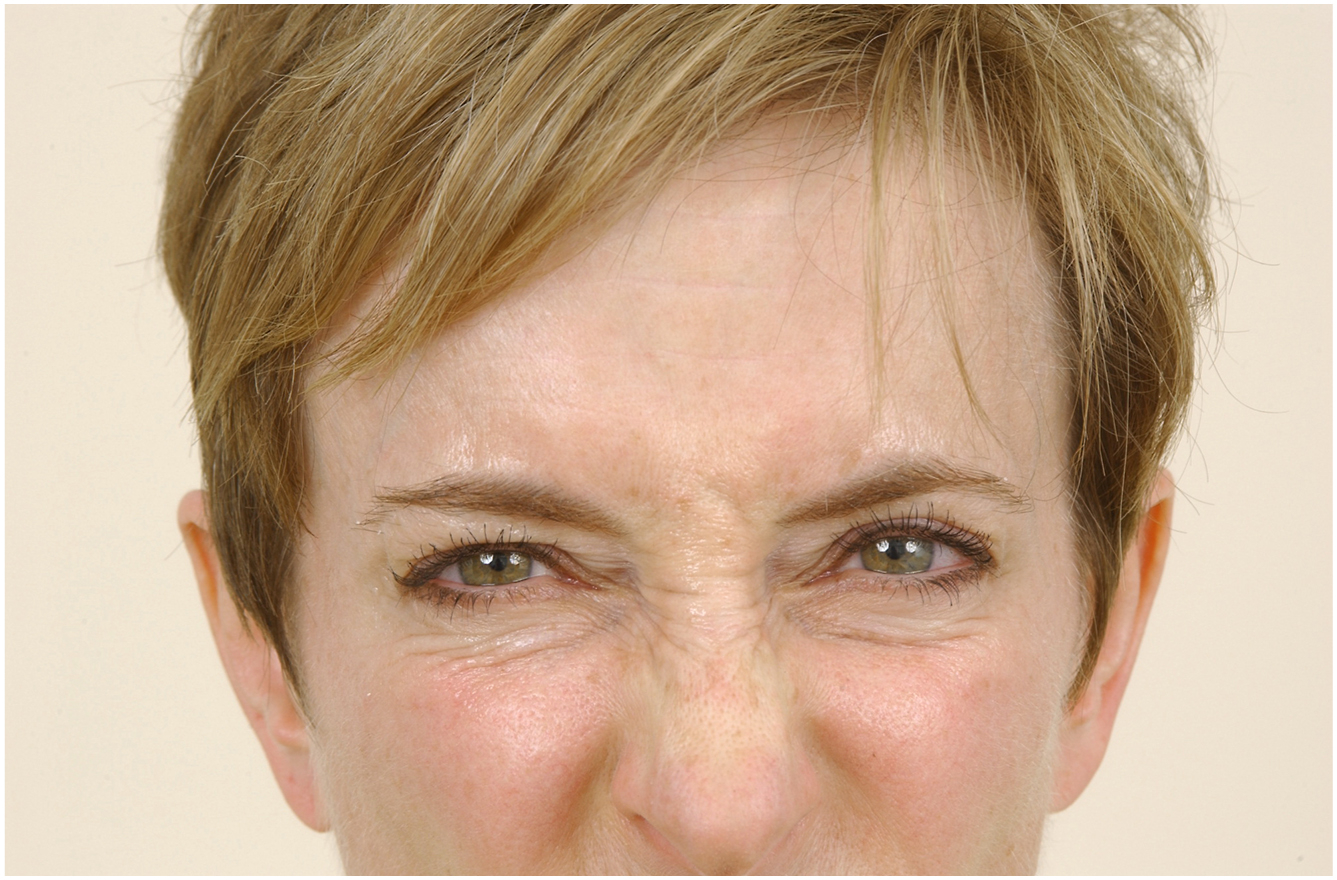
Minor side effects include pain at injection sites, temporary bruising, erythema, edema, and headache. , Less common side effects include eyelid ptosis, asymmetry, diplopia, and dry eye. Caution should also be used when using neuromodulators around the lower eyelid as neuromodulators can worsen fat herniations in that area. Contraindications to neuromodulators include hypersensitivity to any botulinum toxin product, neuromuscular disorders, pregnancy, and breastfeeding. Caution should be used in patients with a history of keloidal scarring.
Dermal Fillers
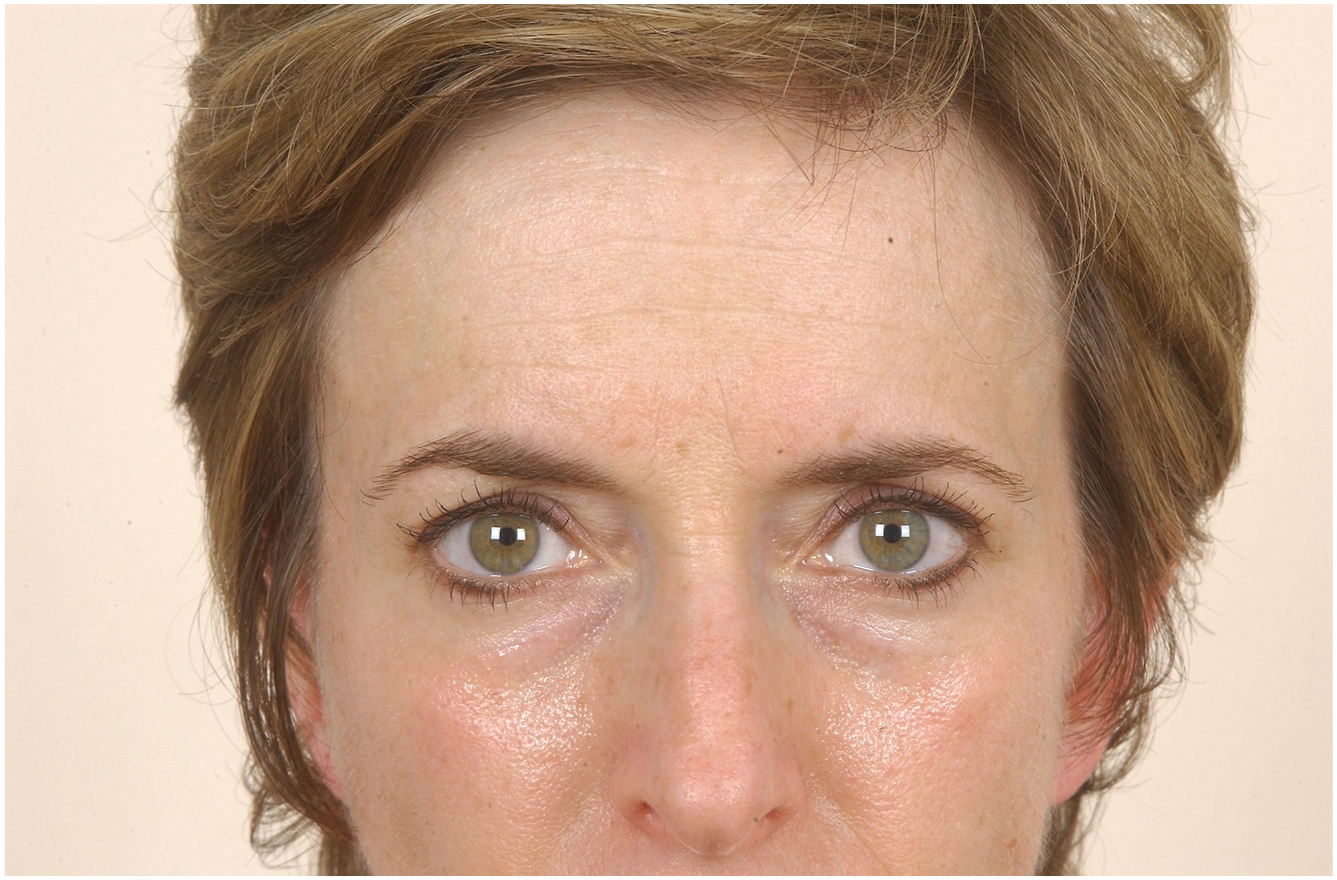
Physiologically, collagen degradation, fat atrophy, and bone resorption lead to periorbital aging. Dermal fillers can be used to regenerate volume. The most common dermal filler for the periorbital region is hyaluronic acid. Hyaluronic acid fillers can be used in the tear trough region to decrease skin laxity and shadowing (undereye “bags”). When used for the correction of the tear trough, the authors commend deep (supraperiosteal) injection using a blunt needle and a hyaluronic acid filler ( Figs. 3 and 4 ). Although controversial, a number of authors believe that the blunt needle makes inadvertent vascular canulation less likely. A small amount of local anesthetic with epinephrine will minimize bruising and should not be confused with an intravascular injection. It can also be used near the lateral eyebrow for a lifting effect. Using hyaluronic acid periorbitally has a higher risk given the potential for vascular occlusion. Rare but devastating complications include skin necrosis due to vascular occlusion and, even rarer, blindness can occur if filler is injected intravascularly and emobolizes to the ophthalmic artery. Thus, periorbital dermal fillers should be performed by experienced clinicians, in an office setting, with hyaluronidase on hand, and an ophthalmologist on call. Autologous fat can also be used as a filler. It has the benefit of a longer lasting effect than synthetic fillers and is generally used as a volumizer in and or around the brow and upper eyelid. Synthetic dermal fillers do not assist with actinic damage or textural improvements of the skin. Dermal fillers also complement other non-surgical periorbital rejuvenations, such as neuromodulators, resurfacing lasers, and radiofrequency-based devices.
Laser
Lasers target various chromophores in the skin, such as melanin, hemoglobin, and water; thus, laser selection is based on the target chromophore. Lasers utilize selective photothermolysis; the light emitted by the laser is absorbed by the target chromophore(s) resulting in heating or even destruction of the target. For skin resurfacing, water is typically the chromophore targeted. Lasers allow for a more predictable and uniform depth of penetration, in contrast to techniques such as dermabrasion and chemical peels.
Skin resurfacing lasers can be ablative or non-ablative and further subdivided into non-fractionated or fractionated. Ablative lasers vaporize the epidermis and superficial dermis causing thermal injury. This generates neocollagenesis and skin remodeling in the epidermis and dermis. Non-ablative lasers surpass the epidermis and deliver thermal energy to the dermis. Thus, the dermis is injured, and the epidermis is spared. Fully ablative lasers provide treatment to the entire targeted area. Fractionated lasers utilize fractional photothermolysis, which creates thousands of microscopic zones of thermal injury. The skin surrounding the channels of ablation speeds tissue recovery and healing in comparison to full field ablation.
Ablative lasers target water more strongly than non-ablative lasers. Ablative fractional lasers (AFLs) are superior to non-ablative fractional lasers (NAFLs) in the treatment of eyelid rhytides and skin texture. A study by Tierney and colleagues investigated the histologic and radiologic changes to the skin for both AFLs and NAFLs. The results showed superiority of AFLs. Generally, the more aggressive the treatment, the greater the benefit, however, more aggressive treatments come with increased downtime and higher risk of side effects. Less aggressive treatments, such as NAFLs, offer less cosmetic improvement but also less downtime and fewer side effects.
Fully ablative lasers
Fully ablative lasers target water causing vaporization of the epidermis and superficial dermis and varying degrees of thermal damage. This stimulates collagen contraction, remodeling, and tightening. Remodeling continues for several months post-treatment. A study by Orringer and colleagues showed increased messenger RNA for collagen I and collagen III after treatment with fully ablative CO 2 laser. Levels peaked at 21 days and remained elevated at 6 months post-treatment. The ablative lasers include the carbon dioxide laser (CO 2 ) and the erbium-doped yttrium aluminum garnet (Er:YAG) laser ( Table 1 ). Fully ablative CO 2 and Er:YAG lasers demonstrate efficacy in the treatment of moderate-to-severe periorbital rhytides and dermatochalasis.
| Laser | Wavelength | Depth of Penetration | Thermal Damage Depth |
|---|---|---|---|
| CO 2 | 10,600-nm | 20–60 μm | 100–150 μm |
| Er:YAG | 2,940-nm | 3–5 μm | 10–40 μm |
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree