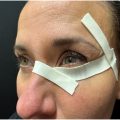
Lower eyelid blepharoplasty has historically been approached from one of only two techniques, either the anterior subciliary incision or from the posterior transconjunctival approach. Both have been used with subtractive techniques of skin and fat resection in most cases and both have had issues with post operative lower lid retraction with scleral show, albeit less with the posterior approach. Lateral acces recontouring does not transgress either the anterior or posterior functional muscles of the lower lid and avoids damaging the innervation of the lower lid orbicularis. Thus the technoque has resulted in a zero incidence of slceral show in this series beginning in 2007. When combined with muscle lifting and fat preservation as recontouring techniques, and canthal support when indicated, it also provides excellent blending of the lid cheek junction for effective rejuvenation.
Key points
- •
Lateral access avoids lagophthalmos.
- •
Recontouring versus skin resection.
- •
Fat preservation causes lid-cheek blending.
- •
Muscle lifting provides support.
- •
Canthopexy when indicated.
Introduction
Surgical rejuvenation of the lower eyelids has undergone significant evolution over the past several decades to improve esthetic outcomes while minimizing comorbidities and complications. Advances in anatomic understanding of the critical lower eyelid structures have led to the development of new, innovative procedures and approaches. Traditionally, lower eyelid blepharoplasty was subtractive in nature, involving removal of excess skin, orbicularis oculi, and fat via skin or skin-muscle flaps. Today’s techniques, in contrast, generally seek to preserve orbital fat and transpose it over the infraorbital rim for improved lid-cheek junction contour, and skin and muscle excision is minimal. These maneuvers may be performed through transcutaneous or transconjunctival incisions and are often combined with lower lid support procedures such as canthopexy or canthoplasty and muscle lifting in appropriate patients. However, due to occasional incidence of lower lid retraction, the senior author began using a lateral access only approach in 2007 which has resulted in lowering the incidence of post opearative lower lid retraction to zero.
Pathologic anatomy of the aging lower eyelid
The aging lower eyelid is characterized by several anatomic changes related to both the skeletal and soft tissue structures. In younger patients, there is a smooth convexity from the tarsus to the cheek with no underlying sign of the orbital rim or other bony landmarks. As aging progresses, attenuation of the orbital septum leads to pseudoherniation of orbital fat over the orbital rim, resulting in the appearance of bulging fat bags. A depression develops between the fat bags and cheek, resulting in a double convexity, with one smaller convexity overlying the orbital fat and the other larger convexity over the cheek.
Initially named the tear trough deformity by Flowers, Stutman and Codner have previously outlined the complicated terminology regarding this condition as well as the history surrounding the improved understanding of its anatomy. Ultimately, they suggest that the term tear trough deformity be applied to the medial periorbital hollow extending from the medial canthus to the medial limbus. Lateral to this, the depression contour irregularity should be referred to as the palpebromalar groove, nasojugal groove, or lid-cheek junction . , It was the anatomic work of Haddock and colleagues that showed the tear trough to correlate superficially with the junction between the preseptal and preorbital portions of the orbicularis oculi. Furthermore, they found that medially the orbicularis oculi fibers were attached firmly to their maxillary origin at the location of the tear trough deformity.
However, laterally, over the lid-cheek junction, there was a ligamentous attachment between the orbicularis oculi and maxilla. This attachment was first described by Kikkawa and colleagues, who termed it the orbital malar ligament . Mendelson and colleagues have since referred to this as the orbicularis retaining ligament because of its identified attachments to the zygoma. Muzaffar and colleagues have detailed additional anatomy of the orbicularis retaining ligament, noting that it separates the preseptal and orbital portions of the orbicularis oculi as it courses superficially. Furthermore, the length of the ligament was greatest at the arcuate expansion of the orbital septum where it was 10 to 14 mm and also 1.5 to 5 mm in thickness. The ligament itself does not lie at the orbital rim or arcus marginalis, but instead lies caudal to the rim, being 4 to 6 mm below the rim at the midpupillary line and 2 to 4 mm below toward the lateral canthus.
This clarification of terminology regarding the tear trough deformity, lid-cheek junction, and orbicularis retaining ligament along with their detailed anatomy are critical in understanding surgical treatment options and required operative maneuvers. Indeed, selection of a specific technique should be tailored to addressing the underlying anatomic abnormality. In young patients with pseudoherniation of lower eyelid fat pads but with minimal skin laxity, there will almost always be early tear trough formation. Most surgeons will recommend a judicious fat pad removal as all that is required, which is generally performed via a retroseptal, transconjunctival approach. However, we believe this approach unnecessarily reduces fat volume and can make the patient actually look hollow and more aged, especially in later years. Patients who have only mild skin excess in addition may be managed with procedures such as skin pinch excision, laser resurfacing, or chemical peel.
With more advanced periorbital aging, including substantial pseudoherniation of fat pads, tear trough deformity, and midface volume loss and descent, more intensive procedures may be indicated. Described techniques include orbital fat repositioning, muscle and midface lifting, fat and other soft tissue grafts, implants, and hyaluronic acid fillers. The traditional skin-muscle flap popularized by Rees and Dupuis in 1969 addressed lower eyelid bags through direct excision using a transcutaneous, subciliary incision. Several investigators have since used this incision and approach to improve the contour of the tear trough and lid-cheek junction by different maneuvers. Transposition of lower eyelid fat pads has proved to be a powerful technique for blending the lid-cheek junction and correcting the tear trough deformity. Loeb was the first to describe fat transposition over the medial infraorbital rim to address nasojugal grooves, and he also used free fat grafts for middle and lateral depression treatment. Hamra extended this procedure to include a complete arcus marginalis release with fat pad transposition of all 3 compartments and fixation below the entire infraorbital rim. He further evolved his technique to include orbital septum reset.
Nonetheless, others, including this author, have had difficulty reproducing those results. Goldberg introduced fat transposition into the subperiosteal plane via a transconjunctival incision to decrease the potential visibility of the edges of the transposed fat as well as for ease of dissection in a bloodless plane. Several fixation techniques have been described, including internal fixation with absorbable or nonabsorbable suture or temporary transcutaneous fixation with or without bolsters. The authors have performed this approach with our lateral access-only incision but found it to be fraught with bleeding issues in the medial aspect where it was necessary to transpose the medial fat pad.
Other investigators have advocated for correction of lower lid deformity with implants or autologous fat grafting. Flowers introduced the alloplastic tear trough implant with several different designs. Loeb used free fat grafts transplanted through an incision over the nasojugal groove. Later, Coleman described injection of small aliquots of fat for tear trough deformity correction through blunt-tipped cannulas. This author has not been able to produce consistent results with fat grafting in this area, and it should be noted that Yoshimura and Coleman followed up their early reports with significant complications in the lower eyelid from fat grafting methods, which can be very difficult to correct.
Common adjunctive procedures include lateral canthal suspension and muscle lifting. Canthal suspension techniques are generally indicated either to address lower eyelid malposition or as a preventative measure in lower eyelid surgery. Canthopexy or canthoplasty may be required in patients who need restoration of canthal tilt, who have a negative vector, those with a poor preoperative snap-back test, in those with lower lid laxity (>6 mm of distraction), or to support the lower eyelid in the early postoperative healing period. Flowers advocated for the routine use of canthopexy because it helps restore youthful tone of the lower eyelid and may reduce or eliminate the need to resect lower eyelid skin. Several investigators have also recognized the significant role of malar support of the lower eyelid. , Orbicularis oculi muscle lifting and fixation in the appropriate vector may also be performed in conjunction with canthal tightening or in isolation to improve lower lid contour and to provide midface lift.
Lateral access recontouring of the lower eyelid
Surgical lower eyelid rejuvenation procedures combining several of these individual techniques are often performed depending on indications. Most surgeons consider only the transconjunctival approach (posterior) or the skin-muscle flap approach (anterior). However, having performed both skin-muscle flap and transconjuctival approaches for years, I continued to find occasional patients who would experience lower lid retraction after these procedures, although this complication was low at approximately 2% for both methods. I found it interesting that a posterior approach was just as much of an issue as the anterior approach and surmised that the problem was not the septum, as noted by Massry, but was most likely due to transgressing functional muscle, orbicularis from the front and the retractors from behind. Indeed, I (Core) agree with these investigators because my experience has been that the septum plays little role, if any, in lid retraction issues and a complete release of the septum all the way across has not led to increased lid retraction in my practice. It was also frustrating because even one patient with scleral show was discouraging and potentially could result in litigation. Early in my experience I had come to prefer the skin muscle flap approach with fat pad transposition, which allowed me much more room to blend the lid-cheek junction using fat transposition techniques introduced by Loeb, and also to perform a midface lift over the fat transfers if needed. I termed this technique the “transblepharoplasty midface lift,” presented in 1996 at the Emerging Technologies meeting at New York University (NYU). Despite excellent cosmetic results in most patients, I continued to experience a consistent rate of mild scleral show of 5%. I finally decided to find a procedure that could avoid transecting functional layers in the central lid area, the orbicularis anteriorly and the retractors posteriorly. The only approach in which central lid functional structures were not located was laterally, so after experimenting with a lateral endoscopic approach, which turned out not to be feasible due to the small suborbicularis space, I discovered that a lateral access incision of 2 cm could be used to visualize the entire field with the use of 4.5 power loupes. Essentially, I found I could accomplish everything I could through this minimally invasive approach using this small lateral access incision.
We initially only offered this approach for mild contour deformities with deep nasojugal groves and available fat to transpose. I also added to this laterally based orbicularis muscle lifting with canthopexy, which significantly improved contour. This approach was presented in Boston at the 2010 meeting of The American Society of Aesthetic Plastic Surgery. In the ensuing years we expanded the indications to include more extensive deformities of aging as well as in revision cases and now use this approach almost exclusively. The technique was developed in 2007 and published in 2013 after a 6-year experience, and now we have a 16-year experience detailed herein.
Patient selection
Because we use the technique for most cases it would benefit the reader more if we outlined the contraindications, which include prior surgery with excision of fat pads, which would now preclude lateral access and muscle lifting but would require fat grafting as opposed to fat pad transfer. Patients who are good candidates are those with deep nasojugal grooves and/or bulging lower lid fat pads, in other words, not only those with skin laxity but also those with contour deformities, hence the name of the procedure ( Table 1 ).