In an effort to prevent post-operative eyelid complications, lower blepharoplasty requires taut approximation of the lower lid to the globe. This is routinely accomplished with lid tightening procedures and/or canthal fixation. Multiple techniques can be utilized in combination to appropriately and aesthetically reposition the lower eyelid during cosmetic blepharoplasty. These techniques include simple canthopexy, canthoplasty, drill hole fixation, and complete tarsoligamentous sling reconstruction. In this article, we examine the unique anatomy of the lateral canthus as well as the indications for utilizing diverse options for canthal fixation.
Key points
- •
To understand the anatomic considerations of the lateral canthus and its interplay with lower lid positioning.
- •
To perform a comprehensive lower eyelid examination to choose the appropriate canthal fixation technique.
- •
To evaluate the indications for diverse types of canthal fixation.
Video content accompanies this article at http://www.plasticsurgery.theclinics.com .
Introduction
The eyes represent a focal point during interpersonal conversation. Even the most minor complications of subtle lid retraction or scleral show (1 mm) can be noticed aesthetically by the untrained eye. Extensive lower eyelid descent, malposition or ectropion can portray an appearance of aging, fatigue, or sadness.
When assessing techniques for lower eyelid rejuvenation, the surgeon clearly approaches the procedure with a primary goal of maintaining aesthetic contour. However, preservation of anterior and posterior lamellar structures should be approached with a goal of maintaining lower eyelid position and function. In light of these indications, we examine the pivotal role of canthal fixation in reproducing consistent aesthetic results in lower blepharoplasty.
Anatomy
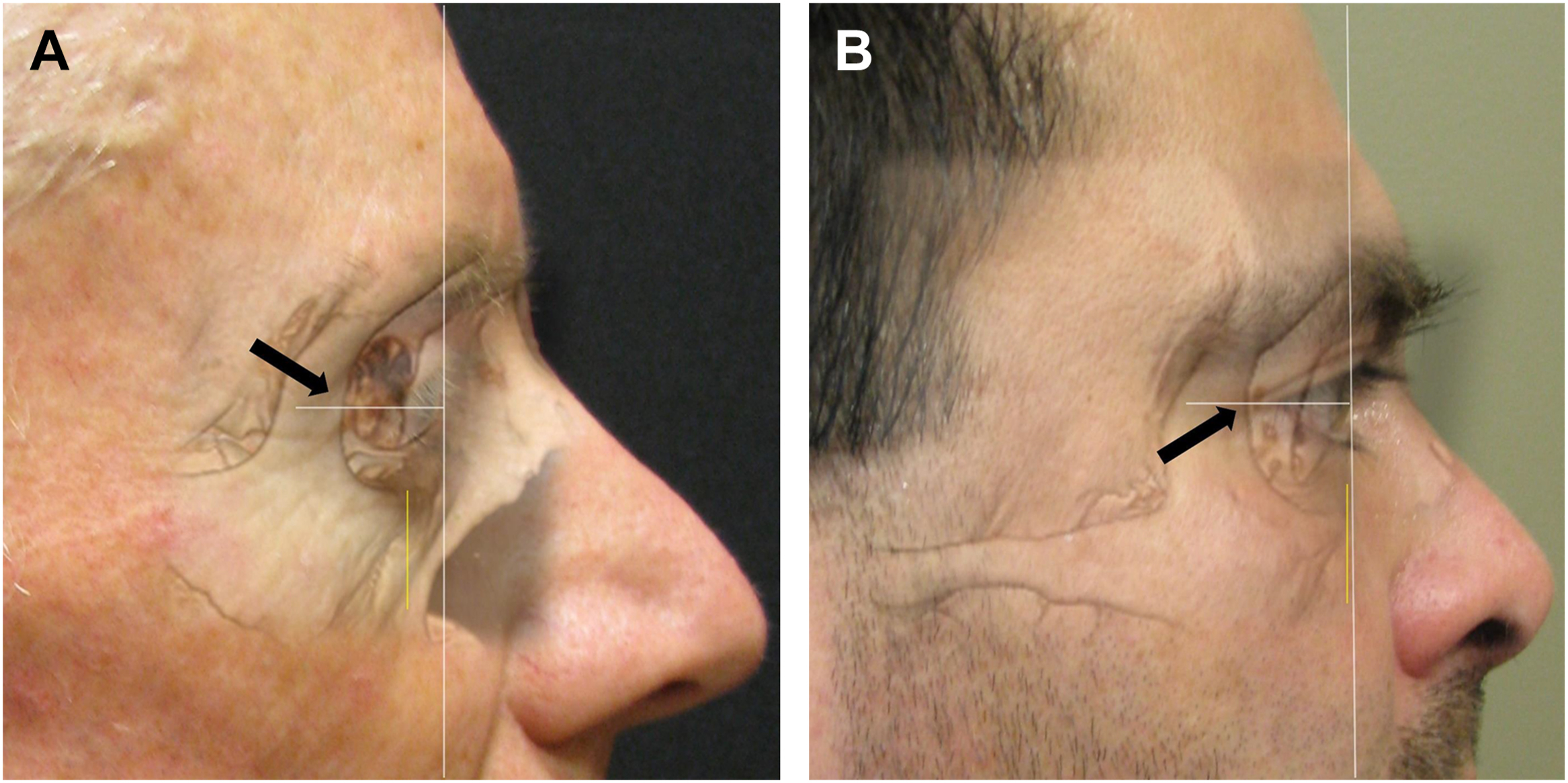
Aesthetically, the lower eyelid position is ideally placed 1 to 2 mm above the inferior cornealscleral limbus as the patient is looking directly forward. In a horizontal position, the lateral canthus lies approximately 2 mm above the medial canthus to create an appropriate canthal tilt ( Fig. 1 ). Excessive overcorrection of the canthal tilt can result in a “slanted eye” appearance that can lead to difficulties in eyelid closure or lagophthalmos.
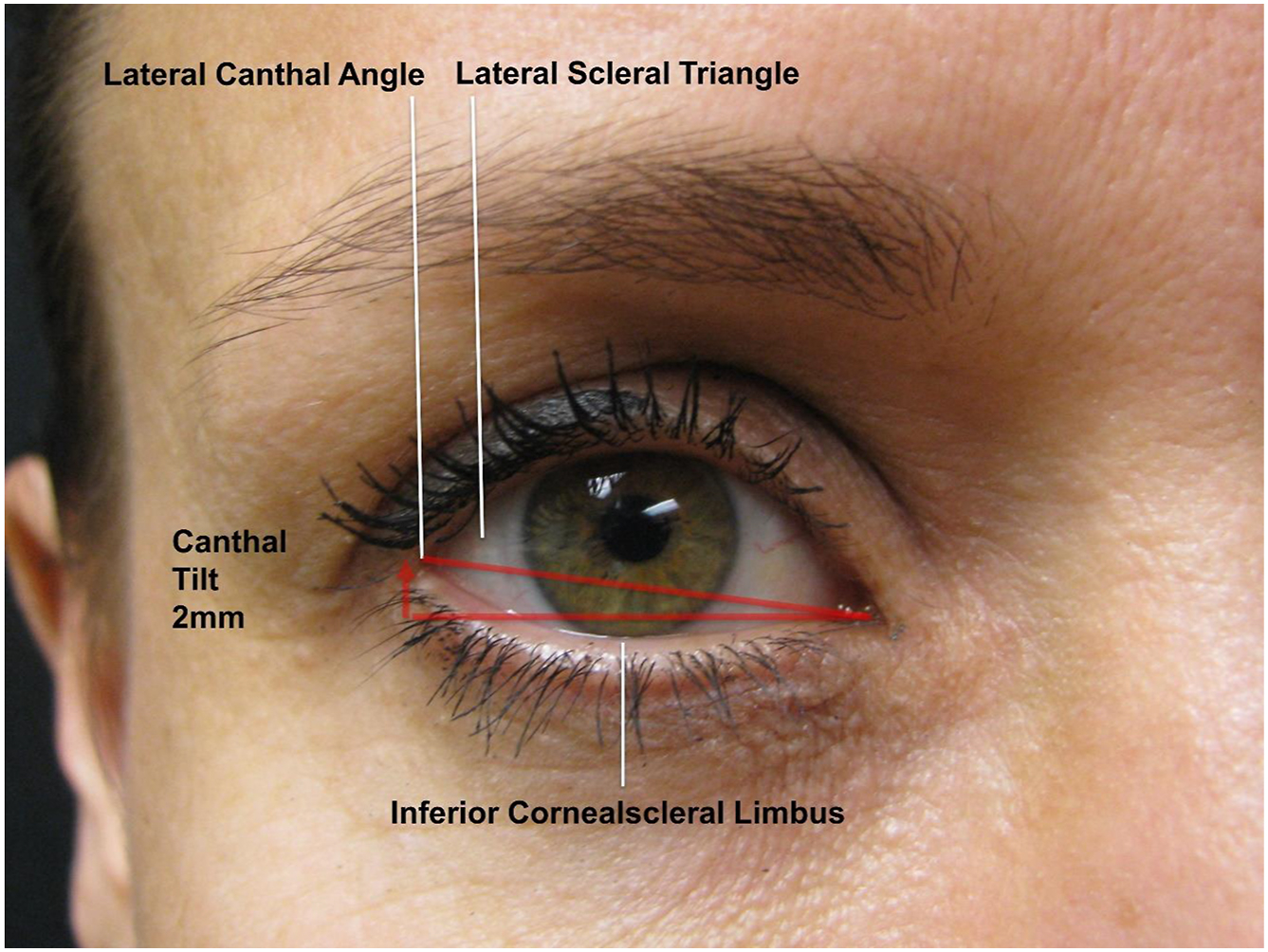
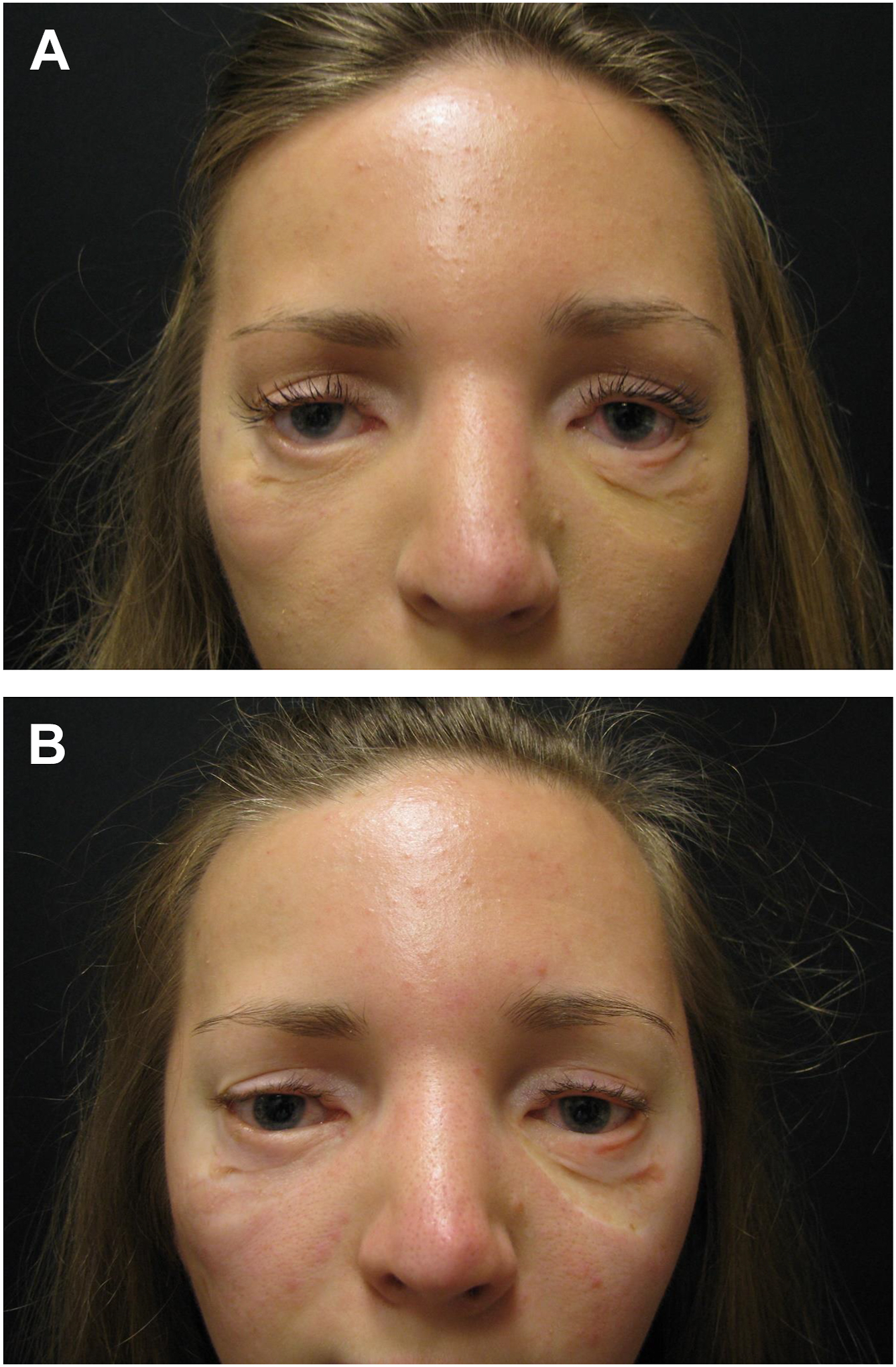
It is often difficult for the surgeon to specifically assess or measure the lower eyelid position in relation to the cornea. Patient’s eyes may involuntarily move or postoperative scleral chemosis may inhibit appropriate measurement. In addition to observing the position of the lower eyelid in relation to the cornea, I have found that a qualitative description of the lateral scleral triangle often provides insight into the position of the lower eyelid as well as the integrity of the tarsoligamentous sling (see Fig. 1 ). While the angle of the lateral canthus and the dimensions of the lateral scleral triangle may vary significantly among patients, an assessment of the symmetry of the lateral scleral triangle comparing both eyes will provide guidance as to the origin of the anatomic discrepancy ( Fig. 2 ).
Medial and lateral canthal tendons form fibrous connections between the tarsal plates and the bony orbit. The continuous construct of these connections is referred to as the tarsoligamentous sling . This is arguably the most important structure in eyelid anatomy. The tarsoligamentous sling creates the internal skeleton of the eyelid ( Fig. 3 ).
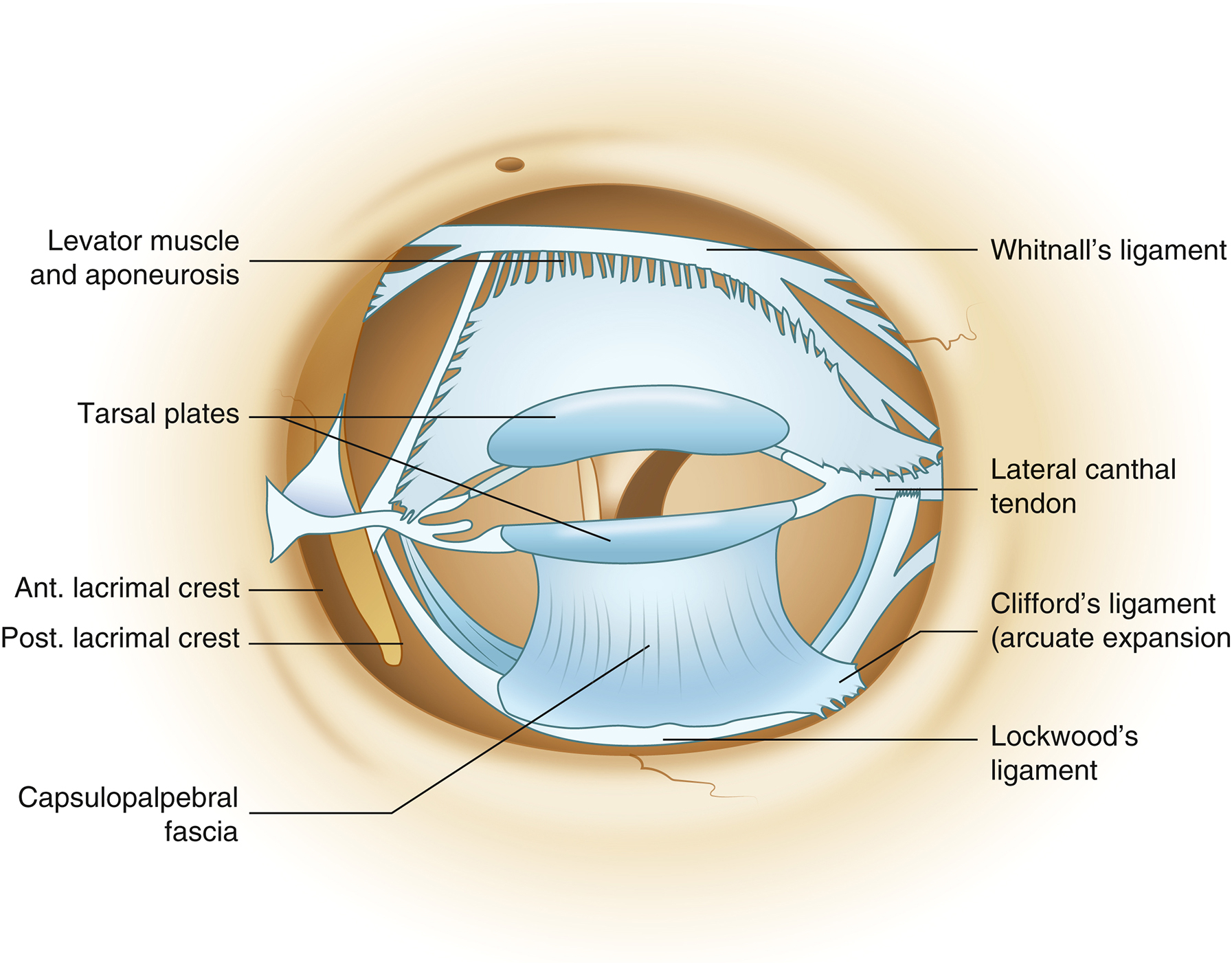
The inferior tarsal plate and the conjunctiva form the posterior lamella. The inferior tarsal plate has a height of 4 mm, which is significantly shorter than the superior tarsal plate. Repair of tarsal continuity and alignment of the lower eyelid margin must be designed perfectly to maintain the tension and anatomic support of the lower eyelid.
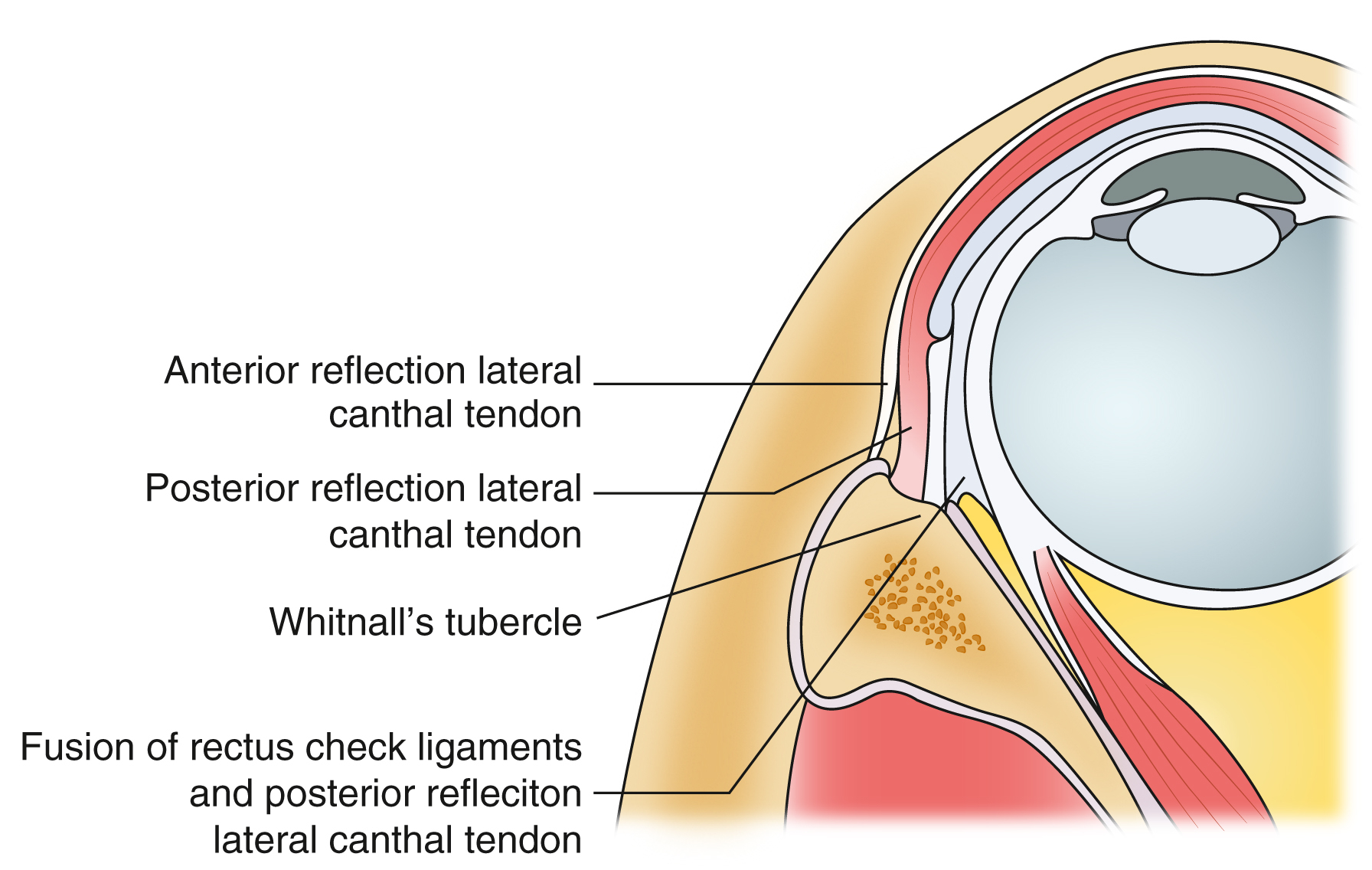
The lateral canthus is a complex structure that has a unique conformity in 3 dimensions. The posterior reflection of the lateral canthal tendon inserts onto Whitnall’s tubercle, which is located 8 to 10 mm posterior to the orbital rim, allowing the eyelid to remain tangent to the globe through this posteriorly oriented vector ( Fig. 4 ). This posterior point of attachment is critical in canthal fixation to reproduce an aesthetic and functional lid position. When planning canthal resuspension, the position of the posterior reflection must be placed along this vector in order to prevent separation of the lateral canthus (ie, canthal dystopia) away from the globe ( Fig. 5 ).
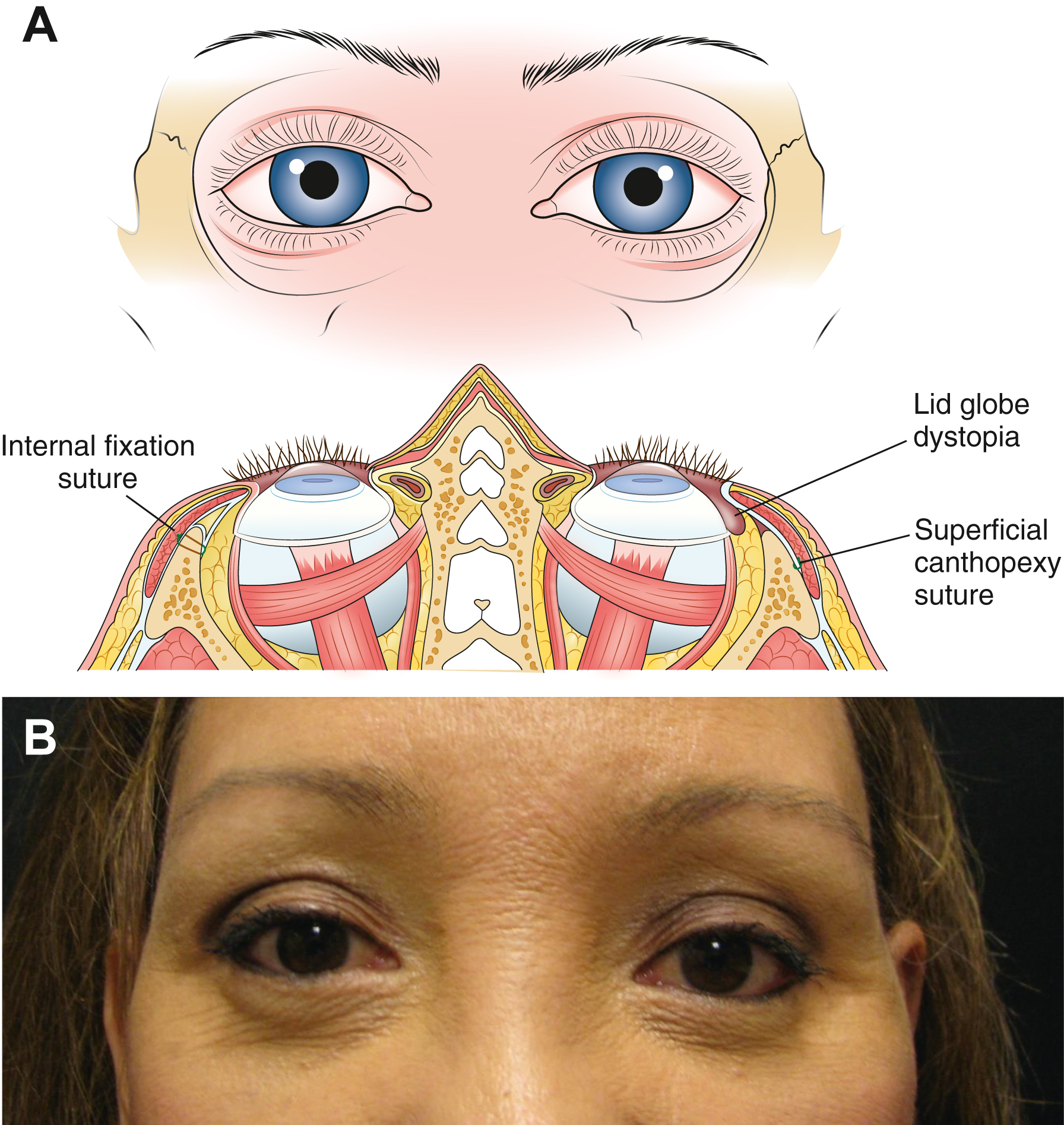
During blinking and eyelid closure, the lower eyelid is often static, whereas the upper eyelid is very dynamic. Any rejuvenation procedure of the lower eyelid should be performed with moderate tension and slight overcorrection. The literature has demonstrated that routine (and preventative) lateral canthal fixation in primary blepharoplasty is associated with substantially low risk of lid malposition and/or ectropion. , Consequently, there is rarely a blepharoplasty (from simple transconjunctival with no skin resection to advanced skin-muscle flap procedures) that should be performed without some technique for canthal fixation. In patients with demonstrated canthal dehiscence, canthal suspension is a requirement.
Patient evaluation
In any blepharoplasty procedure, the surgeon should first assess the static position of both the upper and lower eyelids. In addition to skin excess and skin quality, an anatomic inventory should be assessed noting the extent of skin excess, the condition of the lashes, the position of the brow and the static adherence of the lid to the globe.
Even more importantly is the surgeon’s ability to perform a manual examination to assess the integrity of the tarsoligamentous sling and the lateral canthus. Omitting a manual eyelid examination will invariably cause the surgeon to miss physical characteristics which are clearly indications for advanced types of canthal fixation ( [CR] ).
I routinely utilize a modification of the “four-finger test” first described by Patipa in 2000. During this test, the surgeon performs a lid-snap back test and assess the integrity of lid approximation. The surgeon then places an index finger at the corner of the canthus, mimicking the effect of canthal fixation ( Fig. 6 ). Invariably, the lateral canthus may have some degree of loss on integrity in most patients over the age of 30. Subsequent manual/digital tests can predict the utility and need of anterior lamellar augmentation, spacer grafts or complete tarsoligamentous sling reconstruction.
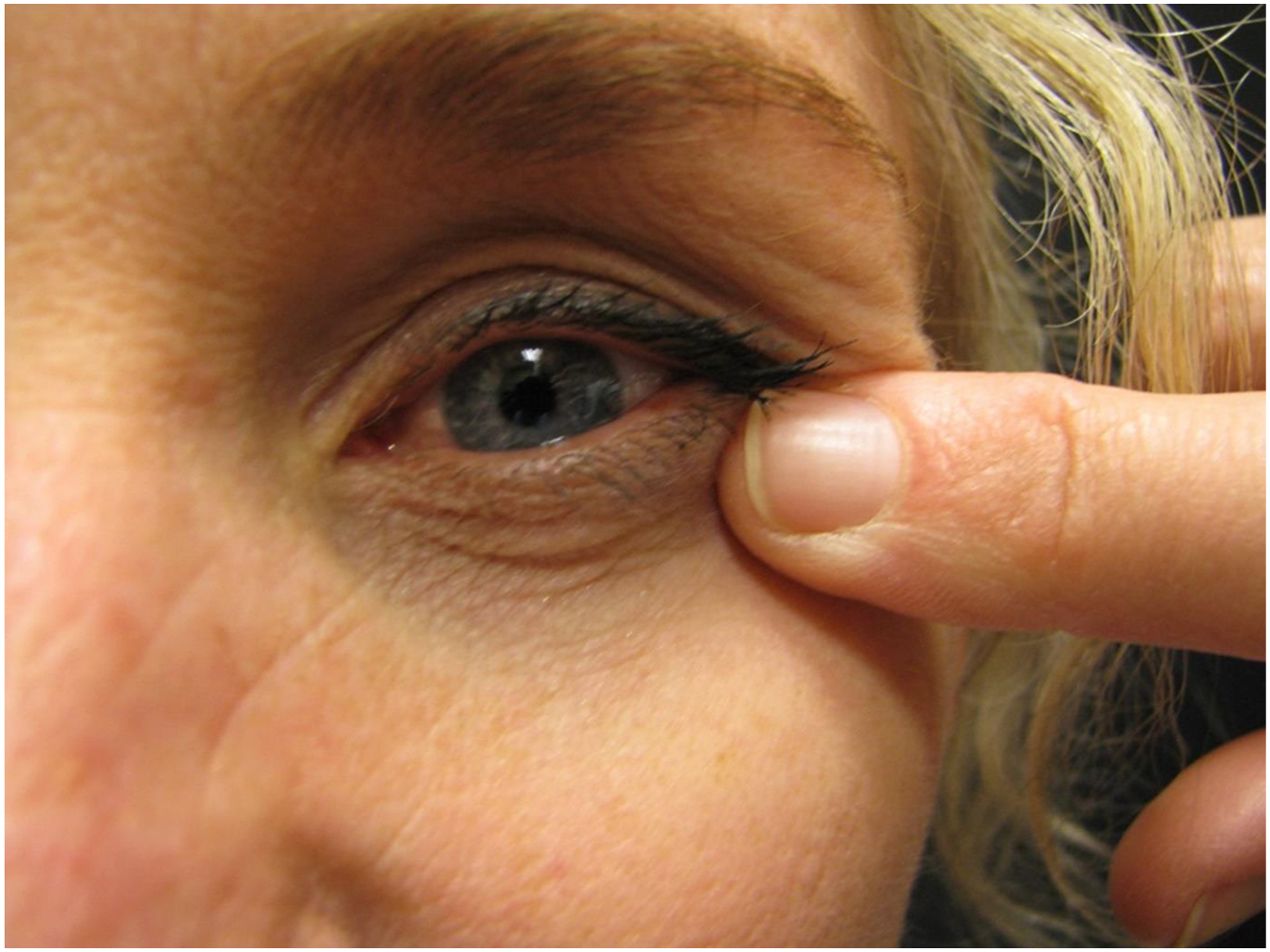
If the mimicked procedure (after finger placement) appears have some degree of continued laxity, the surgeon should consider a lid shortening procedure such as a tarsal strip technique and/or canthoplasty. A preoperative assessment of lateral canthal position and strength, with careful planning of an appropriate canthal suspension technique is critical in maintaining appropriate lid position.
Technique
Instrumentation
Fine instrumentation that is routinely utilized in oculoplastic surgery is preferred. These include fine pickups such as Bishop forceps. Large Adson or Brown forceps should be avoided as these tend to crush tissue. Webster-style needle holders (that were designed for larger procedures), when in hand, utilize an arc of rotation that is rotated at the wrist. This is a gross motor movement that lacks fine precision. Castro-Viejo style needle holders, which can be rotated with finger dexterity, are preferred ( [CR] ).
Canthopexy
When performing a canthopexy or canthal suspension, it is of critical importance to preoperatively determine the vertical position of the canthal fixation point. Preoperatively, the patient should be assessed for eye prominence to assist with planning the fixation point. Eye prominence is determined by examining the anterior position of the corneal surface in relation to the zygoma and cheek projection. I have found the traditional “vector” descriptions of eye position in relation to the malar projection to be confusing and ambiguous. Therefore, I favor utilizing descriptive monikers such as “prominent eyes” (ie, negative vector) or “deep-set eyes” (ie, positive vector).
In patients with prominent eyes, the fixation point should be placed slightly higher than neutral. This will prevent a “clotheslining” effect of the lower eyelid against the globe. In patients with very deep-set eyes, the fixation point is placed slightly lower than neutral. This prevents a compensatory orbicularis misalignment that can lead to lagophthalmos ( Fig. 7 ).