Introduction
Composite tissue allotransplantation (CTA) involves transplantation of various complex tissues embryologically derived from different layers that can include musculoskeletal structures (nerve, bone, muscle, etc.), skin and mucosa, and their adnexal extensions. These differ from well-known solid organ allotransplantations, which are lifesaving procedures, intended to improve quality of life. These have benefited from the introduction of more specific immunosuppressive agents, with fewer adverse effects and greater efficacy, resulting in a significant improvement in the outcomes of solid organ transplantation over the past few decades. Striking successes in the field of kidney, liver, and heart transplantation have encouraged further investigation into these more multifaceted transplants.
Although theoretically any part of the body could be transplanted as a composite tissue, in practice, only the hands, face, larynx, lower extremity, uterus, and abdominal wall have been transplanted to date, and in relatively limited numbers. The first clinical success with hand transplantation, and recent exceedingly high rates of patient satisfaction with hand and face, have fueled the desire to start composite tissue transplantation programs in many medical centers around the world. Although this public demand for reconstructive transplantation is increasing due to early promising results, composite allotransplantation is far more complex and difficult than other forms of organ transplantation. The main challenge facing CTA is the high risk of immunosuppression, which is worthwhile in solid organ transplantation in terms of the risk–benefit ratios. Drugs used for immunosuppression still broadly suppress the immune system and are associated with development of opportunistic infections, a high risk of neoplastic formations, and vital end-organ toxicities. In addition, the medical ethics of composite allotransplantation have also been the subject of debate.
Despite relatively wide experience with the hand, which has been exceptionally favorable from both a physician and patient standpoint, and recent experiences with face allotransplantations, clinical applications for other CTAs are still limited in number and are only performed in a few respected centers worldwide.
Laryngeal Allotransplantation
Absence of a larynx is associated with the loss of a human-sounding voice, an impaired sense of taste and smell, a disposition to a high risk of lower bronchoalveolar infection, and psychosocial disintegration. There is no ideal method for substituting the larynx, either with a like tissue using any organic tissue transfer with the help of microsurgical techniques or prefabrication and replacement by prosthetic materials. Although there have been many recent developments in the fields of tissue engineering, nanotechnology, and regenerative medicine, larynx allotransplantation seems to be the only method capable of reproducing all the properties of a functional original larynx, in current practice.
The first clinical attempt at laryngeal transplantation was in 1969. A 62-year-old man with carcinoma of the larynx was the recipient of a larynx from a 40-year-old donor. He survived well in the early postoperative period and experienced a well-treated acute rejection. Unfortunately, the patient died due to tumor recurrence at postoperative month 8.
The first successful laryngeal allograft procedure took place in 1998. The recipient was a 40-year-old man who had been in a road accident 20 years previously, resulting in laryngeal dysfunction. A laryngopharyngeal complex, including thyroid, parathyroid, and five rings of the trachea was transplanted. The patient now swallows normally, and there has been an evident improvement in his quality of life. Objective voice measurements are within normal limits for intensity, maximum phonation time, and airflow for age.
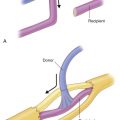
Arterial Anatomy ( Fig. 66.1 and Fig 10.4 , Fig 10.5 )
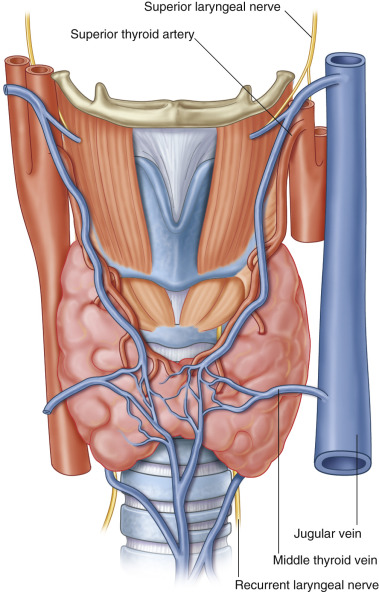
The human larynx is perfused by the superior and inferior thyroid arteries together with branches of the dorsal lingual branch of the lingual artery. Barium latex injection studies have shown that the superior laryngeal artery, the first branch of the superior thyroid artery, can nourish all laryngeal tissues. Injection of the unilateral main superior thyroid artery showed that this perfuses all laryngeal tissues and upper tracheal rings.
The superior thyroid arteries are 1.5–2.5 mm in diameter, and length can be adjusted based on the desired pedicle length in cadavers, extending even to common carotid arteries.
Venous Anatomy
Venous return is consistent with concomitant veins and can again be adjusted based on the pedicle length required, extending to the branch of the internal jugular vein to the main trunk of the internal jugular vein ( Figs 66.1 and 10.5 ).
Neural Anatomy
Reinnervation is essential in order to successfully restore a functional larynx unit with normal laryngeal speech and breathing. Laryngeal muscles could be described as “clever muscles,” since the high density of motor fibers in the recurrent nerve innervates these small-sized muscles.
All muscles within the larynx are innervated by the recurrent laryngeal nerve ( Fig. 66.1 ), except for the cricothyroid muscle, which is innervated by a branch of the superior laryngeal nerve known as the “external laryngeal nerve.” The laryngeal mucosa are innervated by different nerves above and below the vocal cords. While the upper part is innervated by the internal laryngeal nerve branch of the superior laryngeal nerve, the recurrent laryngeal nerve innervates the lower part. Providing sensorial innervation is essential in eliciting cough in order to prevent aspiration of saliva, food, and liquids, and in order to ensure normal mobility of the vocal cords.
Indications
The procedure itself is not a lifesaving one and is only intended to improve quality of life. The ideal recipients are young trauma victims. Other recipients might be patients who have suffered a large benign tumor or low-grade malign tumor resection. However, the latter indication should be well investigated due to the high incidence of tumor recurrence in immunosuppressive patients.
Laryngeal Composite Tissue Component ( Fig. 66.1 )
The transplanted tissue includes the cartilage structure of the larynx and upper trachea, functional muscles of the larynx, mucosal lining of the larynx and trachea, the pharynx, and the neurovascular pedicle of the larynx.
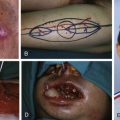
Flap Design
Donor Procedure
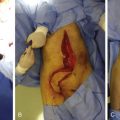
The entire pharyngolaryngeal complex together with upper 5–6 tracheal rings and thyroid and parathyroid glands is harvested, leaving the neurovascular pedicle intact. The vascular pedicle of the harvested tissue includes the superior thyroid arteries, the internal jugular veins as an extension of the superior and middle thyroid veins, the superior laryngeal nerves, and the recurrent laryngeal nerves bilaterally.
Recipient Procedure
The entire vascular and neural structure of the larynx is delineated. An orthotopic position for transferred tissue is created by removing the strap muscles. If present, it is essential to keep the hyoid bone in place in order to ensure that the tongue base and laryngeal elevation are normal. Depending on the presence of a defect in the recipient pharynx, a part or whole pharynx can be transplanted, together with the larynx. Based on the size of the defect, and considering the prevention of the fistula or stricture, a relatively large size of pharynx can be transplanted. A pouch is created for the pharynx and larynx and pharyngeal anastomosis is established in the upper part, the upper part of the tracheal stroma is revised, the donor trachea is sutured to this in an end-to-end manner, and the stoma is re-created superiorly.
Both superior thyroid arteries are anastomosed to the recipient arteries, or to a branch of the external carotid arteries, in an end-to-end manner, or directly to the external carotid arteries in an end-to-side manner. Donor internal jugular veins or branches that drain the transferred tissue are anastomosed to the recipient internal jugular veins or their related branches in an end-to-end or end-to-side manner, based on size match and recipient venous drainage maintenance. Both superior laryngeal nerves and recurrent laryngeal nerves of the transplanted tissue are sutured to their recipient matches.
Flap Modifications
The concept of partial laryngeal transplantation has recently been introduced due to potential problems such as wound healing, adaptation, and aspiration difficulties. However, it is likely that improved functional results will emerge in the future.
Postoperative Care
Tracheostomy tubes and drains can be removed a few days after surgery. After removal of the tracheostomy tube, because of the lack of sensorial and motor innervation, the possibility of aspiration should be kept in mind and all preparations should be made ready. Salivary secretion is reduced using glycopyrrolate and atropine. Nasogastric or gastric tubes can be used for feeding for at least 2 weeks.
Vascularity of the transplanted tissue is monitored as routine microvascular tissue transfer using clinical parameters such as direct examination, with the help of endoscopic imaging bleeding, control of tissue tonus, etc. and with Doppler flowmeters.
Any possible rejection attack should be identified and checked again using direct imaging under endoscopic examination and microscopic examination of the mucosal parts.
Patients should be closely monitored for metabolic, infectious, or organic complications of the drugs used for immunosuppression, such as hypertension, diabetes mellitus, renal toxicity, osteoporosis, and avascular femoral head necrosis.
Immunosuppressive Protocol
The immunosuppressive protocol for the first successful case was as follows: muromonab-CD3 (5 mg/day); cyclosporine (500 mg/day); methylprednisolone (50 mg/day, decreasing to 20 mg in 4 days); and mycophenolate mofetil (MMF) (1 g twice a day). The patient suffered a rejection attack 15 months postoperatively, and this was overcome using a high dose of steroid. Cyclosporine was changed to tacrolimus 4 mg twice daily, together with 1 mg of MMF daily and 7.5 mg of prednisolone/day.
Wide-spectrum antibiotic therapy should be administered for the first 10 postoperative days. Sulfadoxine pyrimethamine was administered to prevent Pneumocystis carinii pneumonia. CMV prophylaxis is performed with valganciclovir.
Future Landmarks
Research for laryngeal transplantation will proceed on the basis of organ-specific immunosuppression, with functional improvements in neuromuscular-specific innervation, partial laryngeal transplantation, and, more importantly, transplantation without the use of any immunosuppressive drug.
Abdominal Wall Allotransplantation
Intestinal allotransplantation is a current and challenging method for treating complicated intestinal failure, with recent advances in immunosuppression and surgical techniques, resulting in improved survival for patients. Although considerable experience exists in the most respected centers, one of the main technical problems is closure of the abdomen without tension. Many potential patients have lost natural anatomic orientation of the abdominal compartment. Additionally, most of these patients suffered repeated laparotomies, enterocutaneous fistulas, wound infections, etc. that cause severe abdominal wall integrity problems. Failure with proper closure of the abdominal wall after allotransplantation leads to a large open wound. The aim is then to close the wound in a staged manner, despite a high risk of complications, such as infection, tissue exposure problems (mechanical problems that may leave tissues unprotected, fistula formation, bleeding, and electrolyte imbalance), and delayed rehabilitation.
The cadaveric composite abdominal wall myofasciocutaneous flap has been described in order to address this problem.
Arterial Anatomy (see Fig. 66.2 and Fig 11.3 , Fig 11.6 )
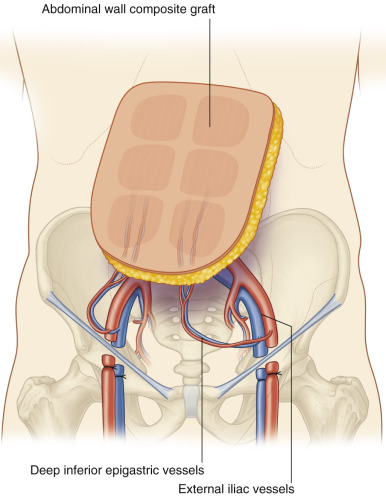
The composite abdominal wall flap is perfused by the inferior epigastric vessels. These are left in continuity with the common femoral or iliac arteries.
Venous Anatomy (see Fig. 11.8 )
Venous drainage is achieved by the concomitant veins.
Neural Anatomy (see Fig 11.9 , Fig 11.10 )
Since only structural tissue coverage is needed, no nerve trunk is included in the transferred tissue.
Indications
The main indication is impossible or high-risk direct abdominal closure in patients undergoing intestinal allotransplantation.
Abdominal Wall Composite Tissue Component ( Fig. 66.2 )
The transplanted tissue includes one or both rectus abdominis muscles, overlying fascia, underlying sheet and abdominal subcutaneous tissue, and skin.
Flap Design
The surface area may range from 150 cm 2 –500 cm 2 , based on patient age and size.
Donor Procedure
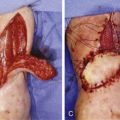
The donor does not need to be matched with the recipient in HLA typing. ABO blood identification should be considered, as with other allotransplantations. The composite abdominal wall tissue can be transplanted in the same session as the intestinal allotransplantation or in a different session a few days later, harvesting from a different donor. Composite flap harvesting has been performed as part of a combined multi-organ procurement procedure in a heart-beating donor. The procedure starts with an upper part incision, a Mercedes-like incision, which starts from median sternotomy to extend to the bilateral subcostal line. Then a continuous vertical bilateral incision is made in the lateral borders of both rectus abdominis muscles. In the groin region, the two incisions are connected transversely in the midline. Both inferior epigastric vessels are dissected and followed until common femoral vessels are identified. The length of the vascular pedicle is determined based on the desired length obtained. If necessary, dissection can be extended to obtain iliac vessels as the donor pedicle. The composite abdominal wall flap is flushed with perfusion solution and packed with ice, as with other donor organs.
Recipient Procedure
After reperfusion of the intestinal or multivisceral allograft, the composite allograft is transferred as a separate tissue. Vessels of the composite tissue are anastomosed to the iliac vessels in an end-to-side manner. The length of the pedicle is adapted in a smooth curve to prevent uneven tension or kinking. The transplanted abdominal tissue is incorporated into the edges of the recipient abdominal wall defect.
Flap Modifications
The composite flap can be harvested based on a cuff of external iliac or femoral vessels in such a way as to contain the deep circumflex iliac, deep inferior epigastric, superficial epigastric, and superficial circumflex vessels for a larger flap with more reliable circulation.
The posterior rectus sheath fascia can be transplanted in continuity with the falciform ligament of the liver in the case of liver transplantation. In this situation, the flap is nourished by the hepatic artery, which has been anastomosed to the recipient artery as a standard procedure in liver transplantation.
Postoperative Care
The perfusion of the flap is monitored as routine clinical follow-up of the free flap in terms of color, tonus, blood refill, needle puncture, and bleeding nature and, if necessary, monitoring of vascular anastomoses using a Doppler flowmeter.
Any possible rejection attack should be identified and checked by taking routine biopsy specimens and evaluated by microscopic examination.
The patient should be closely monitored for metabolic, infectious, or organic complications involving the drugs used for immunosuppression, such as hypertension, diabetes mellitus, renal toxicity, osteoporosis, or avascular femoral head necrosis.
Immunosuppressive Protocol
The immunosuppressive protocol at the best-known center is as follows: induction consists of administration the anti-CD52 monoclonal antibody alemtuzumab (0.3 mg/kg) immediately preoperatively, immediately postoperatively, and on postoperative days 3 and 7. Maintenance immunosuppression is based on tacrolimus with a targeted serum level of 10 µg/L. In rejection attacks, corticosteroids are used in high doses.
All other prophylactic antibiotic protocols are similar to those used in other allotransplantations.
Future Landmarks
In the light of improvements in immunological modalities, composite allografts may be transplanted without using any immunosuppressive drugs. They also may be used more rationally as an isolated composite tissue without any other visceral organ in the case of massive abdominal wall defects occurring after massive trauma, resections, or complicated surgical procedures.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree