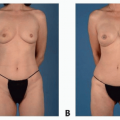
Index Finger Pollicization for Hypoplastic Thumb
Amir H. Taghinia
Brian I. Labow
Joseph Upton
DEFINITION
The thumb is the functional keystone of the hand. The basic hand unit has three main elements: a thumb, a web space, and a prehensile post. Severe hypoplasia or aplasia of the thumb leads to significant functional impairment.
Index finger pollicization is the procedure of transposing the index finger into the position of the thumb. It is the quintessential operation of hand surgery, incorporating key principles and requiring meticulous technique and execution.
ANATOMY
The normal thumb is perfectly adapted for pinch and grasp. It is broad with osseous and articular structures that move in multiple planes. Its intrinsic muscles provide a short moment arm, powering the movement enabled by the osseoarticular column.
The normal first web space has a gentle curve spanning from the thumb metacarpophalangeal (MP) joint to the index finger MP joint.
A thumb is considered hypoplastic if any of its osseous, musculotendinous, or articular components is deficient or if the web space that it forms with the index finger is shallow.
The modified Blauth4 classification system provides a surgically useful basis for categorizing thumb hypoplasia. Most surgeons agree that Blauth types I, II, and IIIA thumbs can be reconstructed, whereas Blauth types IIIB, IV (pouce flottant), and V (aplasia) hypoplastic thumbs require index finger pollicization.
The differentiating factor between Blauth type IIIA and IIIB thumbs is the presence (IIIA) or absence (IIIB) of a functional carpometacarpal (CMC) joint.
The preoperative state of the index finger is the greatest determinant of long-term postoperative function after pollicization.1,5 Patients with normal index fingers will have the best function. Abnormal index fingers are typically seen in patients with radial longitudinal deficiency. Abnormalities include stiffness, joint hypoplasia, incomplete intrinsic muscles and/or extrinsic tendons, and hypoplastic or anomalous vessels and nerves.
PATHOGENESIS AND NATURAL HISTORY
Thumb hypoplasia occurs as a result of multiple potential factors, including genetic (associated syndromes), environmental, teratogenic (thalidomide), and idiopathic causes.
It is considered to be a malformation, based on the Oberg, Manske, and Tonkin classification of 2010.6
Thumb hypoplasia occurs in 1 out of 100 000 live births.
A large number of patients with thumb hypoplasia have associated conditions such as cardiac or hematologic anomalies.
PATIENT HISTORY AND PHYSICAL FINDINGS
Patients are usually seen in infancy. In severe cases such as type IV or type V, the diagnosis is clear. Nevertheless, the difference between type IIIA and IIIB can be difficult to ascertain in a newborn. The integrity of the CMC joint is sometimes not obvious on plain film radiographs. Functional differentiation can be made by allowing the child to grow and watching the toddler at play—if the thumb is not used, the joint is likely nonfunctional.
Indeed, most children with severe thumb hypoplasia will scissor pinch using the index and middle fingers in lieu of the nonfunctional thumb. With time, the web space between the index and middle fingers widens and the index finger starts to pronate. These patients are ideal candidates for pollicization.
The hand surgeon should be aware of the conditions associated with thumb hypoplasia, and have a low threshold to refer if suspicions arise.
In particular, roughly 50% of patients with Fanconi anemia (an inherited defect in DNA repair leading to bone marrow failure and premature malignancy) manifest thumb hypoplasia, along with a variety of other anomalies. The diagnosis of Fanconi anemia can be made via a blood test early in life.
Other associated conditions include Holt-Oram syndrome, VACTERL association, radial longitudinal deficiency, and thrombocytopenia-absent radius (TAR).
IMAGING
Plain radiographs help to determine the status of the CMC joint, any abnormalities of the index finger, and the status of the distal radius and ulna (presence of radial longitudinal deficiency).
The authors do not routinely perform angiography.
DIFFERENTIAL DIAGNOSIS
Differentiate type IIIA and IIIB thumbs by functional assessment of the child.
SURGICAL MANAGEMENT
The authors perform index finger pollicization in toddlers around 2 years of age, but the timing is more dependent on size, weight, and other medical comorbidities that may delay intervention.
The procedure is technically easier if performed in a toddler, rather than an infant.
Manske5 has shown that pollicization can be functional and effective even if performed later in childhood.
The main objective of the operation is to shorten and reposition the index finger into a recessed, pronated, and palmarly abducted position, as well as to simultaneously create a well-contoured web space.
The main steps of the procedure are as follows:
Make incisions in a modified Y to V fashion that will allow the index finger to be recessed and rotated.
Isolate the index finger as a neurovascular island.
Disinsert and isolate the intrinsic muscles of the index finger.
Excise the metacarpal, ablate the metacarpal growth plate, and secure the metacarpal head in a hyperextended position into the cut metacarpal base.
Rebalance the extensor tendons.
Rebalance the intrinsic muscles.
Adjust skin flaps to create an aesthetically pleasing outcome.
Almost always, there is sufficient skin to transpose the index finger and close all the wounds without needing skin grafts.
Any open wounds or flaps under tension are the result of poor incision planning or execution.
Simultaneous bilateral index finger pollicization is not performed.
Preoperative Planning
Again discuss risks, benefits, and expectations with parents on the day of surgery.
Specifically outline the risks of flap loss (partial or complete), ischemia of the digit, poor positioning, and suboptimal function and the potential need for revisional or adjunct procedures later in childhood.
The surgeon needs fine surgical instruments and vessel loops for tagging and dissection of important structures.
Positioning
The patient is positioned supine with the arm out on a small hand table.
Approach
Incisions are planned carefully prior to use of the tourniquet. Dorsal and palmar approaches are needed.
TECHNIQUES
▪ Index Finger Pollicization
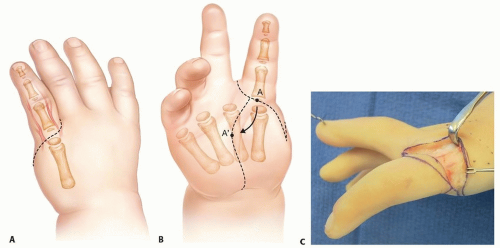
Markings and Dissection
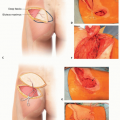
Place two small round marks, one at the base of the index finger and the other at the position where the new thumb base will be placed. Mark a racquet-shaped incision around the base of the index finger. Extend these markings onto the proposed new thenar flexion crease; this will be the recession incision.
The markings for the incisions should be planned so they extend through the round marks (TECH FIG 1A,B).
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree