Apocrine sweat gland
Eccrine sweat gland
Structure
Coiled tubular
Coiled tubular
Location
Axilla and perianal areas
All over the body
Odorous
Yes
No
Method of secretion
Secreted from canals of hair follicles
Directly onto surface of the skin
Timing of secretion
Emotional stress
Elevated body temperature
Function
Thermoregulation, hormonal balance
Thermoregulation, protection, secretion
Psychological Influence on Hyperhidrosis
The exact mechanism behind hyperhidrosis remains unknown, but an underlying neurological disorder may be involved. The disorder is likely secondary to a disordered, response to the sympathetic nervous system. Emotional stimuli from the limbic system and cortex trigger a hormonal imbalance in the hypothalamic sweat center [9, 13]. Thus, psychological triggers can contribute or exacerbate the signs and symptoms of hyperhidrosis. Several theories exist regarding the pathophysiology of hyperhidrosis with relation to stress and are explained below [16].
One theory is the increased sympathetic activity of the autonomic nervous system when over-stimulated by the hypothalamic-pituitary-adrenal (HPA) axis during times of psychosocial stress [17]. The hypothalamus’s corticotrophin-releasing hormone (CRH) and arginine-vasopressin stimulates the anterior pituitary’s production of adrenocorticotropic hormone (ACTH), which stimulates the adrenal gland secretion of cortisol, a stress hormone [17]. Cortisol levels can be quantified and used to help determine a correlation between stress and hyperhidrosis [17]. Furthermore, everyday activities may worsen and add psychological stress [17, 18].
Other studies suggest that hyperhidrosis is triggered by different psychological disorders including social anxiety disorder (SAD), olfactory reference syndrome (ORS), and obsessive-compulsive disorder (OCD). SAD is a social phobia characterized by persistent fear of regular social interactions that affects up to 13 % of the population [19]. Patients with this disorder have increased daily stress and anxiety levels [18]. There is controversy over whether SAD and hyperhidrosis are co-existent disorders. While some propose that patients with hyperhidrosis are no more at risk for anxiety and psychopathological disorders than the general population, Weber et al. discovered that symptoms of SAD was particularly common amongst patients who had been diagnosed with treatment-resistant hyperhidrosis. They also noted the potential correlation between OCD and hyperhidrosis. The excess sweat produced by hyperhidrosis patients may increase their paranoia about repulsive body odor and hygiene thereby increasing the likelihood that they develop ORS or OCD [20, 21].
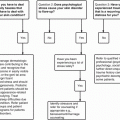
Studies have also investigated the affects of depression and anxiety in the etiology of hyperhidrosis. Braganca et al. sought to determine the levels of anxiety, depression, and irritability in hyperhidrosis patients. All patients in the study were assessed by the same doctor and were asked to answer the questionnaire, “Hospital Anxiety and Depression Scale” (HADS) in an air-conditioned, private clinic. The results showed that prevalence of anxiety among hyperhidrosis patients was 49.2 %, approximately four times that for depression symptoms at just 11.2 %. They also discovered that age, gender, and skin tone were not significant variables related to hyperhidrosis [22]. In a study by Ruchinskas et al., hyperhidrosis patients were administered the Minnesota Multiphasic Personality Inventory-2 (MMPI-2) and State-Trait Anxiety Inventory. The objective was to determine the degree of psychopathology in those patients by comparing their test results with established norms. The results were within the range of established norms, indicating that anxiety and depression were not significant and was likely not the primary cause of hyperhidrosis. Eighty-eight percent of the patients in this study demonstrated regular psychological profiles; the 12 % of the sample that scored above the average range of MMPI-2 results on the anxiety scale may be unique to hyperhidrosis patients, or may simply reflect the upper limits of anxiety in the general population, not exclusive to those with hyperhidrosis.
Krogstad et al. compared the variation of sweating between twenty patients with primary palmar hyperhidrosis and twenty healthy controls. Both groups self-reported their sweat patterns 24 h a day for 1 week. They were instructed to rate their perspiration with a subjective evaluation scale (SES) ranging from 0 (no sweat) to 10 (sweaty). A significant difference in the rate of sweating was found between the two groups. Although both groups demonstrated increases by scores of 2–5 with daily stress and exercise, there was a greater increase in patients with hyperhidrosis than controls. The time of day the self-assessment was conducted also fluctuated the SES scores; in hyperhidrosis patients, scores varied from 0 to 2 in the mornings and evenings, and rose to 5–6 around mid-day. During the same time period, control subjects reported SES scores close to 0. Krogstad et al. successfully demonstrated that sweating patterns of hyperhidrosis patients are not consistent; yet fluctuate throughout the day, especially during physical and emotional stimuli [23].
Treatment
Various treatment options exist to help alleviate the symptoms of hyperhidrosis. The clinical effectiveness, quantified by a variety of standardized scales including the Hyperhidrosis Disease Severity Scale (HDSS) and the Dermatology Life Quality Index (DLQI), are used to evaluate patients’ quality of life. Invasive surgery is currently one of the only permanent solutions for primary axillary hyperhidrosis (PAH) patients, however other treatment options offer temporary relief and a brief period of decreased symptoms for 4–18 months, often requiring multiple treatments to yield optimal results [2, 7]. A few of the available treatment options include aluminum chloride antiperspirants, oral administration of anticholinergic drugs such as glycopyrronium bromide (glycopyrrolate), iontophoresis, botulinum toxin type A (BTXA) injections, and endoscopic thoracic sympathectomy [2–7].
Topical Therapy
Treatment with over-the-counter antiperspirants containing topical aluminum chloride or zirconium salt, is an easy option for patients with mild-to-moderate hyperhidrosis. Aluminum, or zirconium in some antiperspirants, precipitates with mucopolysaccharides in the eccrine duct, thus obstructing the secretory coils of the lower dermis and preventing secretion of any fluids, providing temporary relief [10]. Patients with mild-to-moderate hyperhidrosis can purchase these antiperspirants with 10 % aluminum chloride concentration without a prescription, but those with more severe hyperhidrosis require concentrations of 20 % aluminum chloride in ethyl alcohol [24, 25]. Initial application should be during the night as sweat glands are less active during sleep. A stable sweat gland allows the metal salts in the antiperspirant to be absorbed easily. Haider et al. conducted a study with application of 20 % aluminum chloride in ethyl alcohol on the palms and axillae regions. Within 48 h there was substantial improvement, but the effect lasted only for another 48 h. These investigators study noted efficacy of topical treatment in 98 % of cases [26]. Topical application may result in adverse side effects like skin irritation, dry skin, and itchiness. Persistent treatment may reduce the skin irritation and pruritus [12]. Applying aluminum chloride in combination with 2–4 % salicyclic acid gel also may help reduce skin irritation and promotes penetration of the treatment [27]. Hydrocortisone cream is another method that has been reported to alleviate irritation [24, 28].
Oral Medication
Administration of oral anticholinergics such as glycopyrrolate is another available treatment. Bajaj et al. performed a retrospective analysis on 9 patients with generalized hyperhidrosis and 15 patients with localized hyperhidrosis and reported the efficacy of oral glycopyrrolate 2 mg twice daily, with dosages adjusted according to patients’ ability to control sweating. Of the original 24 patients enrolled in the study, only 19 committed to follow up. 79 % (15/19) of hyperhidrosis patients responded well to oral glycopyrrolate. Adverse effects of glycopyrrolate included dry mouth, headaches, and urinary retention. There was no correlation between increasing dosages and adverse side effects [10, 12, 29].
Iontophoresis
Iontophoresis uses a direct electrical current to pass an ionized substance through the skin [30]. The mechanism of action of this treatment is poorly understood, though several theories have been proposed. Iontophoresis is indicated in patients with palmar and plantar hyperhidrosis whose symptoms persist despite treatment with topical therapy [10]. Physicians initially administer treatment, but eventually patients can self-administer iontophoresis once properly trained for appropriate home-use. In addition to the convenience of home application, patients prefer iontophoresis because of a financial incentive. Many insurance companies view treatment for hyperhidrosis medically necessary when topical therapies have failed and will pay for iontophoresis therapy. An observational study of 113 patients with palmoplantar reported a 91 % response rate [30]. The side effects of iontophoresis are mild and include redness of skin, vesiculation in the affected area, burning sensations, and dryness. Many of the side effects can be prevented with proper knowledge of the procedures and precautionary measures are taken. In general, patients should refrain from touching the electrodes to prevent electrical shock [10, 12, 30].
Botox
Botulinum toxin type A (BTXA), Botox, is popularized for its beneficial, cosmetic effects on unwanted wrinkles and creases, however it can also be used to treat both axillary and palmar hyperhidrosis. In many studies, intradermal injections of BTXA demonstrates efficacy of 80–90 % [3, 31]. This toxin directly stimulates the eccrine glands, irreversibly obstructing acetylcholine release from presynaptic bulbs at postgangiolinc nerve endings, leading to anhidrosis for up to 6 months [12]. In each palm, 100 U are injected intradermally; 50–100 U are injected per axilla [31]. Although not a cure-all treatment for hyperhidrosis, many patients seek out this modality because it is less invasive with minimal side effects, which include slight discomfort during the procedure. and slight bruising immediately post-injection. Some patients have noted that application of ice and topical anesthesia alleviated their discomfort during injection [32, 33]. A significant downside of this option is the frequency of treatments the patient must endure to maintain efficacy; botox treatment of PAH calls for at least 15 injections per axilla, every few months [12, 31, 34].
Surgery
Surgical treatment is reserved for treatment of severe, recalcitrant hyperhidrosis. Several surgical methods such as the complete excision of sweat glands, subcutaneous curettage, and endoscopic thoracic sympathectomy can be employed. Complete excision of the sweat glands significantly reduces sweat production, but routinely results in unpleasant scars, the risk of infection, and restricted arm movement [12]. The risks and benefits of surgical removal of sweat glands should be thoroughly discussed with the patient.
Another surgical alternative for patients, one of few that renders a permanent solution is subcutaneous curettage. This option is simpler than complete excision of sweat glands, as it requires fewer preoperative preparative measures. First, the target axillary region is washed with antibacterial soap to ensure the axillary regions are free of dirt and other bacteria. Shaving is recommended prior to surgery, as the surgeon will have better visualization of the area, but this is not necessary. To prevent infection stemming from contamination of the incision, a precautionary dose of intravenous antibiotics should be administered. It is imperative that the patient’s system be clear of any anticoagulant medications as these may induce excessive bleeding and lead to additional complications in an otherwise simple procedure [35]. Before incision, the region of the patient’s maximal sweating is marked with the starch and iodine method followed by marking the patient’s skin to clearly outline the sweating area. An elliptical excision is made and subcutaneous fat and lower dermis in the targeted region is removed. Scarring is reduced if the coils of sweat glands at the lower dermis are removed. Ten of the 13 patients treated in this manner in a test conducted by Munro et al. experienced significant benefit [13]. Other side effects include bleeding, pain, hematoma, infection, seroma, and brachial plexus damage [12].
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree