Being a team physician is a unique opportunity afforded to orthopedic surgeons or medical doctors who have undergone appropriate subspecialty training and certification. Requirements include specialized skill and expertise in diagnosing and treating various medical and musculoskeletal conditions in the acute sideline setting in addition to the standard clinical setting, and furthermore requires, excellent communication and the ability to coordinate care among a curated care team. Those strongly desiring to be a team physician should seek employment in a position that supports this pathway by way of team contracts, although other opportunities may exist on a volunteer basis.
Key points
- •
Team physicians have important medical and administrative duties aimed at ensuring the health and wellbeing of their athletes.
- •
The best pathway to becoming a team physician is to choose one’s job wisely based on existing team coverage contracts and conversations regarding opportunities to be involved in that coverage.
- •
Local high school or recreational sport coverage may be available on a volunteer basis, but certain liability risks must be assumed and covered by the provider.
- •
National team coverage may be available on a volunteer basis but requires superb understanding of the sport being covered and as well as time volunteered away from one’s practice which may impact one’s wages.
Introduction
Many individuals who pursue a career as a sports medicine provider do so with an interest in becoming a team physician in some capacity. With professional, amateur, and recreational sports fulfilling such an integral part of American culture, there can be a special allure to being on the sideline and carrying out an important role for your respective team. Being a team physician is a unique opportunity that differs considerably from the typical daily workflow encountered within the clinic, hospital, or operating room and comes with its own unique set of challenges and rewards.
Defining the Role
In order to get involved as a team physician within your career, it is important to first understand the role and function of a team physician. Team physicians can have a variety of backgrounds including orthopedic surgery, family medicine, internal medicine, emergency medicine, or physical medicine and rehabilitation, and are required to be licensed to practice medicine within the state of their medical practice and the team that they cover resides. In addition to specialty board certification, it is highly recommended to have further certification specifically in sports medicine, such as the Subspecialty Certificate in Orthopedic Surgery offered by the American Board of Orthopedic Surgery. The American Board of Family Medicine also offers a Certificate of Added Qualification in Sports Medicine (CAQ), which is cosponsored by boards for physical medicine rehabilitation, emergency medicine, and internal medicine.
The team physician fulfills both medical and administrative roles, with both domains being essential to administering care to and protecting athletes. The team physician’s medical role requires appropriate knowledge of medical injuries and ailments affecting athletes, injury prevention strategies, injury evaluation and treatment, and return to sport decision making. Gametime sideline coverage relies heavily on the prompt diagnosis and recognition of both medical and musculoskeletal injuries, with an emphasis on determining whether an athlete is safe to return to play. Although rare events, true medical emergencies do occur, and as such, team physicians must be well-trained and up-to-date on Advanced Cardiac Life Support and Advanced Trauma Life Support certifications. The medical role of the team physician extends beyond the sideline as well, with the physician either seeing athletes for assessment within the training room or as referrals into the physician’s clinic. When a player’s injury does require surgical treatment, the team physician should provide treatment and a rehabilitation plan based on the player’s injury and the demands of their sport, or, when appropriate, facilitate this treatment with another provider. A skilled team physician’s medical role is as much about getting the appropriate medical providers involved in the care of the athlete as it is about providing direct care for oneself.
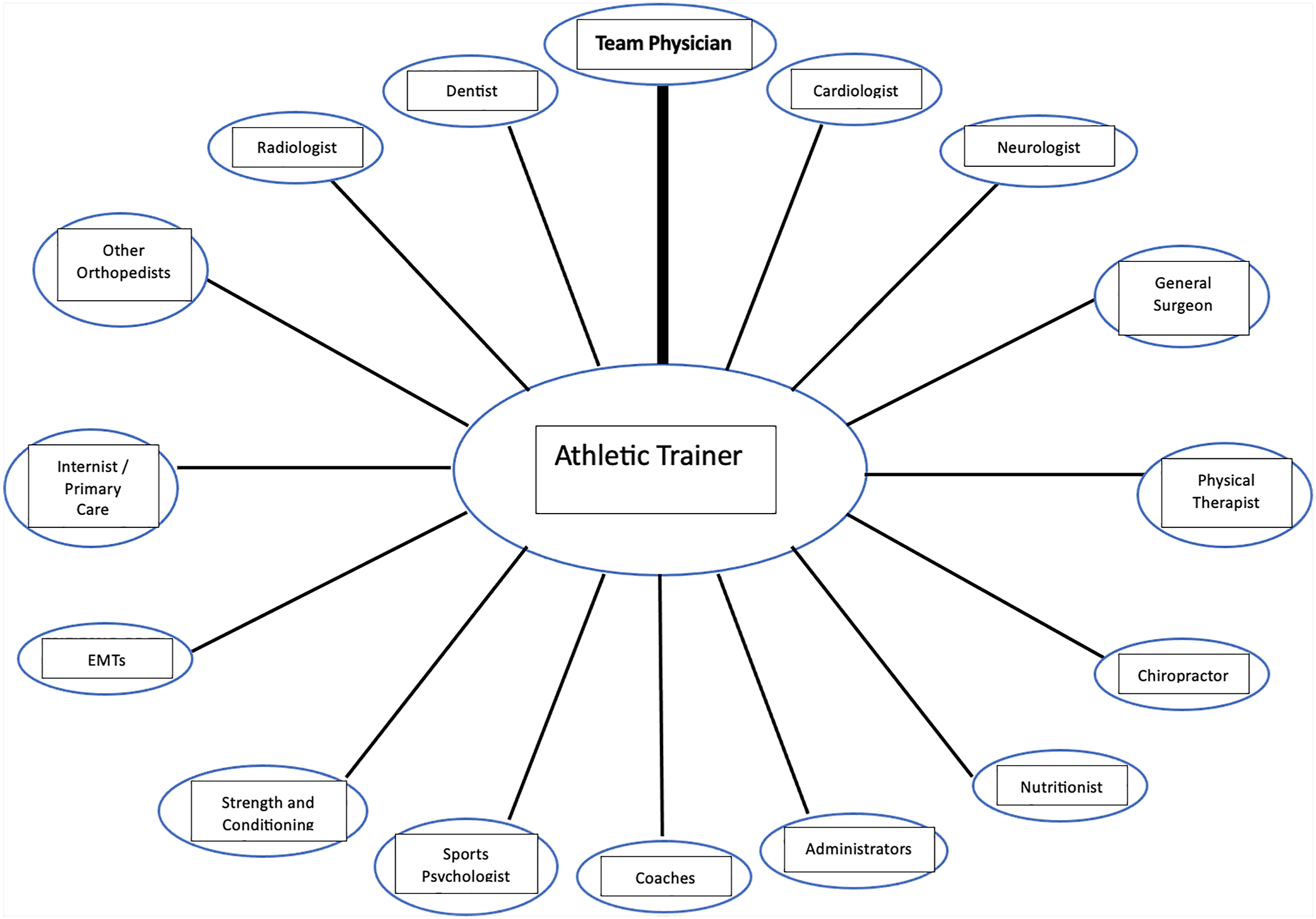
The team physician’s administrative role includes ensuring sideline preparedness and a functional emergency action plan (EAP), close collaboration and prompt communication with the team’s certified athletic trainer(s) (ATC), and building a network of other care providers and facilities who are readily available to help with player needs outside of those that would be addressed by the core medical team–for example, ophthalmologists, cardiologists, dentists, nearby hospital/imaging centers, and so forth. The importance of having a comprehensive network of medical providers and capabilities was illustrated clearly with the recent COVID-19 pandemic, in which outside laboratory testing was often required, as was the ability to get echocardiograms and cardiac evaluations in patients infected with post-COVID-19 returning to play. Oversight of communications with the patient-athlete is a central role for the team physician. This includes taking on the primary responsibilities for the coordination of care that occurs off-field or outside of the training room and may serve a role in regulatory and oversight processes as well. For most athletic care teams, the head ATC serves as the focal point of communication, with the head team physician being the initial point of contact for the ATC in most cases. This has been described as a wheel communication strategy or the hub-of-the-wheel model and helps to ensure clearly delineated pathways of communication that can prevent errors occurring with a more haphazard model of communication between parties ( Fig. 1 ). The team physician forms the base of the hub of the wheel and may communicate with spokes of the wheels, such as other medical providers, coaches, athletic directors, agents, and other administrators, but communication always includes or travels back to the head ATC at the hub. It is important to maintain adherence to ethical principles regarding the patient-physician relationship when communicating with regard to injured athletes. Conflicts of interest are a known challenge to navigate, particularly at higher levels of competition, but ethical duties to respect physician-patient confidentiality and the physician’s role to act in the best interest of the patient should be guiding principles. As the team physician has the professional duty and liability for the treatment of his or her patients, the decision as to whether an athlete is safe for return to play rests with the team physician. , Furthermore, appropriate documentation should be performed for all patient encounters performed in a nontraditional clinical setting, for example, a training room, locker room, or on the field/court/playing surface.