14
Hand and Wrist Fractures and Dislocations
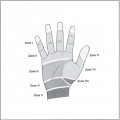
 The Hand
The Hand
Physical Examination
A complete physical examination to determine the integrity of the neurovascular, musculoskeletal, and cutaneus system is warranted. Dedicated hand series radiographs should include AP, true lateral, and oblique views. In selected cases of carpal fractures and wrist injuries, a CT scan may be indicated.
Fracture Classification
• Open versus closed
• Displaced versus nondisplaced
• Transverse versus oblique versus spiral versus comminuted or avulsion
• Traumatic versus pathologic
• Adult versus pediatric
 In pediatric patient: Green stick versus epiphyseal plate
In pediatric patient: Green stick versus epiphyseal plate
 In epiphyseal plate: Salter-Harris classification
In epiphyseal plate: Salter-Harris classification
Fracture Treatment
In general, hand fractures can be treated in the emergency room with closed reduction and splinting. However, if the fracture is open, displaced, unstable, or if the angulation is not acceptable, then operative treatment may become necessary.
Open Fractures
• Perform a finger or wrist block
• Culture and irrigate open fractures profusely
• Administer IV antibiotics (ER treatment or inpatient)
 Ampicillin 500 g IV q8h + gentamycin 3 to 5 mg/kg q.d. divided 8 hours (check peak and through serologic levels)
Ampicillin 500 g IV q8h + gentamycin 3 to 5 mg/kg q.d. divided 8 hours (check peak and through serologic levels)
 Vancomycin 1 gm IV q 12h + Ceftriaxone 1 to 2 gm IV q24h
Vancomycin 1 gm IV q 12h + Ceftriaxone 1 to 2 gm IV q24h
 Outpatient prophylactic antibiotic for patients with plan for later surgery includes Bacitracin DS and PO b.i.d.
Outpatient prophylactic antibiotic for patients with plan for later surgery includes Bacitracin DS and PO b.i.d.
• Irrigate the wound and splint the patient in preparation for operative reduction
Phalangeal and Metacarpal Fractures
Indications for Operative Treatment
• Intraarticular fracture
• Irreducible fractures
• Malrotation
• Subcapital phalangeal fractures
• Open fracture if displaced or angled
• Bone loss
• Multiple fractures
• Fractures with soft-tissue injury
Phalangeal Fractures
Distal Phalanx Fractures
Distal phalanx fractures are the most common fractures in the hand. The thumb and middle finger are most likely involved. Patients present with tuft fractures, shaft fractures, and intraarticular injuries due to crush.
Tuft Fractures
Open Fractures
• Perform finger or wrist block
• Remove nail
• Irrigate
• Repair nail bed with 6.0 to 7.0 chromic and stent the nail matrix (see Chapter 17, Fig. 17–2)
• Immobilize DIP joint in extension with tongue blade or aluminum splint for 3–4 weeks with PIP free
• In cases of severe comminution, soft-tissue repair is adequate for splinting fractures
• Treat with Bacitracin DS and PO b.i.d. × 5 days
Closed Fractures
• Perform finger or wrist block
• If a hematoma is present under the nail, drain it with a drill (sterile 18-gauge needle tip), heated paper clip, or electrocautery
 If the hematoma >50% of nail bed, likely nail bed injury
If the hematoma >50% of nail bed, likely nail bed injury
 Remove and repair nail bed and splint with piece of foil from chromic package or use the nail itself (see Chapter 17, Fig. 17–2)
Remove and repair nail bed and splint with piece of foil from chromic package or use the nail itself (see Chapter 17, Fig. 17–2)
• Splint finger for 2 weeks
• Treat with outpatient antibiotics × 5 days
Shaft Fractures
• Nondisplaced
 Repair soft tissue
Repair soft tissue
 Splint 3 weeks
Splint 3 weeks
 Bacitracin DS and P. O. b.i.d.
Bacitracin DS and P. O. b.i.d.
• Displaced
 Likely nail bed laceration
Likely nail bed laceration
 Repair nail matrix (see Chapter 17, Fig. 17–2)
Repair nail matrix (see Chapter 17, Fig. 17–2)
 Stabilize fracture with K-wire or 18-gauge needle
Stabilize fracture with K-wire or 18-gauge needle
 Splint finger with PIP free for 3 weeks
Splint finger with PIP free for 3 weeks
 Outpatient antibiotics × 5 days
Outpatient antibiotics × 5 days
Intraarticular Fractures
• Open fracture
• Closed fracture
 Splint DIPJ in extension
Splint DIPJ in extension
Dorsal Base
An intraarticular fracture of the dorsal base (mallet fracture) is a hyperflexion injury in which a portion of the dorsal bone breaks off with extensor mechanism. It causes extensor lag with a mallet finger deformity. Treatment requires strict patient compliance. In pediatric population this may require a K-wire through DIPJ.
• Treat with splint in extension for 6 to 8 weeks
Volar Base (FDP Avulsion)
An intraarticular fracture of the volar base is a hyperextension injury in which the flexor digitorum profundus (FDP) pulls off the distal phalanx.
• Treat with ORIF because FDP may retract into palm
• Splint hand in emergency room with tongue blade or aluminum splint
• If open, wash out, repair nail bed, start antibiotics, and splint
Middle and Proximal Phalanx Fractures
Middle and proximal phalanx fractures are caused by crushing forces rather than direct blow, twisting, or angular forces. If these fractures are nondisplaced or stable, simply buddy tape or splint with IP extended for 3–4 weeks. A comminuted, displaced fracture of the middle or proximal phalanx proximal to the articular surface is called a pilon fracture.
Articular fractures
• In ER setting
 Fracture of single digit: ensure involved joint is in extension
Fracture of single digit: ensure involved joint is in extension
 Aluminum or tongue blade splint
Aluminum or tongue blade splint
 Multiple fractures: Splint hand in intrinsic plus
Multiple fractures: Splint hand in intrinsic plus
 Follow up in clinic for operative management
Follow up in clinic for operative management
• Non-displaced: Inherently unstable.
 Operative management using either closed or open reduction and fixation by multiple k-wires or screws or a combination.
Operative management using either closed or open reduction and fixation by multiple k-wires or screws or a combination.
 If non-operative management chosen then close follow up required
If non-operative management chosen then close follow up required
• Displaced
 Dorsal base fractures of middle phalanx
Dorsal base fractures of middle phalanx
 ORIF to avoid Boutonniers defect
ORIF to avoid Boutonniers defect
 Dorsal base fractures of proximal phalanx
Dorsal base fractures of proximal phalanx
 Requires ORIF
Requires ORIF
• Unicondylar (Displaced)
 Inherently unstable either closed or open reduction and fixation with multiple K-wires or screws
Inherently unstable either closed or open reduction and fixation with multiple K-wires or screws
 Extension splint 2–3 weeks
Extension splint 2–3 weeks
• Bicondylar
 Requires ORIF
Requires ORIF
 Non-comminuted
Non-comminuted
 Fix condyle to condyle first then to the shaft with K-wires or screws
Fix condyle to condyle first then to the shaft with K-wires or screws
 Comminuted
Comminuted
 Difficult to treat
Difficult to treat
 DIPJ:
DIPJ:
• Minimal displacement: Closed reduction.
 Splint 2 weeks in extension
Splint 2 weeks in extension
 Physical therapy in 2 weeks
Physical therapy in 2 weeks
• Displaced:
 ORIF with K-wire/screw fixation
ORIF with K-wire/screw fixation
 Early motion at 2 weeks
Early motion at 2 weeks
 PIPJ:
PIPJ:
• Skeletal traction of the middle phalanx for 3–4 weeks with forearm splint.
• Active flexion of PIPJ immediately
Nonarticular fractures
• Shaft
 Non-displaced and stable- not rotated, angulated, or comminuted
Non-displaced and stable- not rotated, angulated, or comminuted
 Splint the finger in extension with an aluminum splint
Splint the finger in extension with an aluminum splint
 Must cover proximal and distal joint
Must cover proximal and distal joint
 Duration of 1 week
Duration of 1 week
• Once pain and swelling resolve then buddy tape to adjacent finger and begin range of motion
 Displaced but amenable to stable closed reduction
Displaced but amenable to stable closed reduction
 Usually transverse fractures not oblique or spiral
Usually transverse fractures not oblique or spiral
 Attempt reduction and stabilization
Attempt reduction and stabilization
 Perform digit block (See Chapter 13, Fig. 13–1)
Perform digit block (See Chapter 13, Fig. 13–1)
 Flex MPJ maximally
Flex MPJ maximally
 Flex distal fragment to correct volar angulation
Flex distal fragment to correct volar angulation
 Dorsal splint in intrinsic plus position
Dorsal splint in intrinsic plus position
 Plaster should be placed dorsally for extension blocking. MP 90°, IP extended, include adjacent digits in splint for stabilization
Plaster should be placed dorsally for extension blocking. MP 90°, IP extended, include adjacent digits in splint for stabilization
 Splint for 3 weeks, then buddy tape for additional 2 weeks
Splint for 3 weeks, then buddy tape for additional 2 weeks
 Unstable—if potential for rotation or angulation exists
Unstable—if potential for rotation or angulation exists
 Open, oblique, spiral, comminuted fractures
Open, oblique, spiral, comminuted fractures
 Radiographically angulated
Radiographically angulated
 Assess by having patient flex finger
Assess by having patient flex finger
 Fingers overlap
Fingers overlap
 Plan closed reduction with percutanous pinning with in 3–4 days
Plan closed reduction with percutanous pinning with in 3–4 days
 Use 0.035–0.045 inch
Use 0.035–0.045 inch
 Unstable transverse fractures
Unstable transverse fractures
 Intramedullary longitudinal fixation through metacarpal head with k-wire
Intramedullary longitudinal fixation through metacarpal head with k-wire
 Extension block splint in intrinsic plus position with IP joints free for 3–4 weeks
Extension block splint in intrinsic plus position with IP joints free for 3–4 weeks
 Comminuted fractures
Comminuted fractures
 Require operative management
Require operative management
 External fixation device often indicated
External fixation device often indicated
 Preserves length
Preserves length
 Assists with management of soft tissue injuries
Assists with management of soft tissue injuries
 For unsuccessful percutaneus pinning perform ORIF with plates or interaosseous wireing
For unsuccessful percutaneus pinning perform ORIF with plates or interaosseous wireing
Base fractures of proximal phalanx
• Extraarticular
 Angulation of 25° in adults and 30° in children requires treatment
Angulation of 25° in adults and 30° in children requires treatment
 To reduce:
To reduce:
 Flex MP maximally
Flex MP maximally
 Flex distal fragment to correct volar angulation
Flex distal fragment to correct volar angulation
 Splint in intrinsic plus (dorsal plaster) for 3 weeks
Splint in intrinsic plus (dorsal plaster) for 3 weeks
 Failed closed reduction
Failed closed reduction
 K-wire fixation
K-wire fixation
Metacarpal Fractures
Head Fractures
• Open fractures 2° to closed-fist injury (fight bite)
 Wrist or local block
Wrist or local block
 High-pressure irrigation and débridement
High-pressure irrigation and débridement
 Leave wound open
Leave wound open
 Delay fixation until sign of fixation subsided
Delay fixation until sign of fixation subsided
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree


 Repair nail bed
Repair nail bed Splint DIPJ in extension for 6–8 weeks
Splint DIPJ in extension for 6–8 weeks Outpatient antibiotics
Outpatient antibiotics