Fig. 27.1
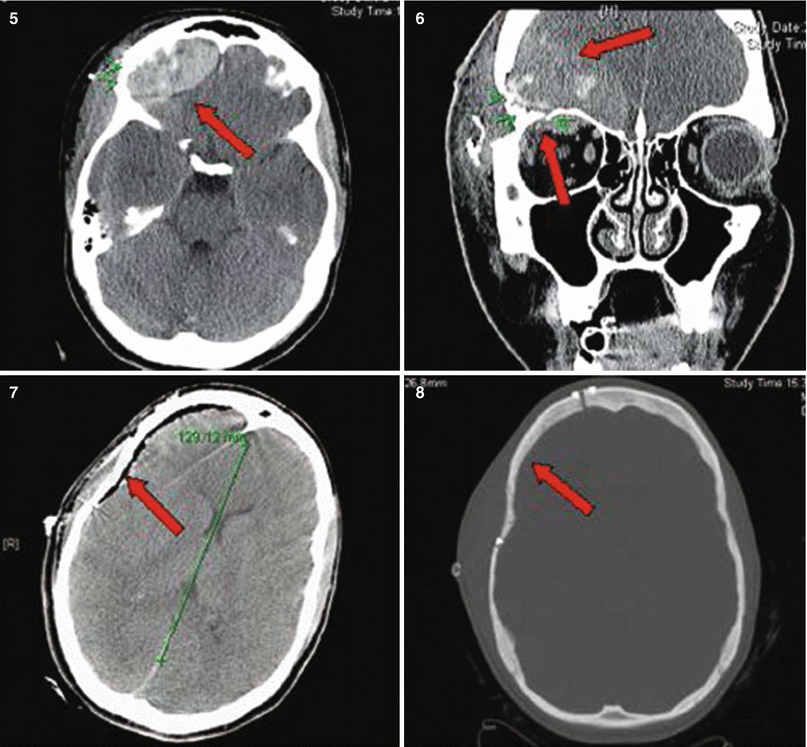
Patient No. 1: a 22-year-old female crime victim, who sustained multiple GSW with a single non-penetrating GSW to the head. Entry wound at R cheek, exit wound on R supraorbital forefront. Plates 1 and 2: scout images A/P and lateral without evidence of bullet. Plates 3 and 4: preoperative images (bone windows) demonstrating R frontal skull fracture with pneumocephalus and orbital roof fracture. Plates 5 and 6: axial and coronal views of large R epidural hematoma and infraorbital hematoma. Plates 7 and 8: axial views of postoperative results status post evacuation of hematoma and autologous cranioplasty. Plates 9 and 10: reconstructed orbital roof status post transfrontal evacuation of retro-orbital hematoma
27.1 Some Rules for Workup Leading to Operative Management
The most important rule to memorize at the very beginning is Time is brain.
As profane as it may sound: Clear thinking and a high speed of coordinated action is crucial and it requires a well pre-instructed and well-drilled team.
What we really mean here is: Swiftly coordinated actions are vital in the true sense of the word and will define the outcome for such challenging endeavors and are an absolute requirement if you want to succeed. This applies to all parts of the care-provider chain: from Advanced Life Support-trained EMTs, who pick up and transport the patient, their management en route, to the presentation upon arrival in the ER. Admission exam and timely workup is critical and potentially lifesaving (with its bedside decisions) until a possible intervention in the OR can be performed. The latter can only be successful with a premeditated and very well-carried-out surgical plan.
Here are my (EMK) rules:
No. 1: DO NOT PANIC! In many ways, it is a case like many others; therefore RUN YOUR ROUTINE. Do all the workup and related decision like a tree and according to a protocol.
No. 2: DO NOT WASTE TIME – and save it where you can do it safely. This means: When the hospital is notified about the arrival of such a GSW patient, GET READY BEFORE THEY ARRIVE. Call the OR upfront to get a room setup. Announce the most likely scenario (e.g., 20-year-old male; RT craniotomy/supine or suboccipital craniotomy/prone, etc.). Ask to assemble a team for the OR that you already know/can work with, not newcomers (Fig. 27.2).
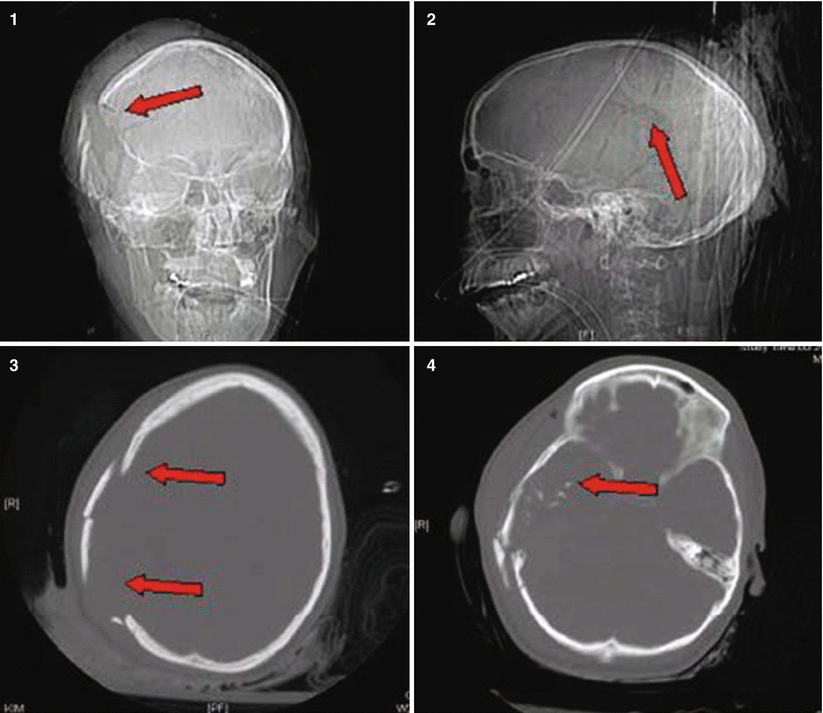
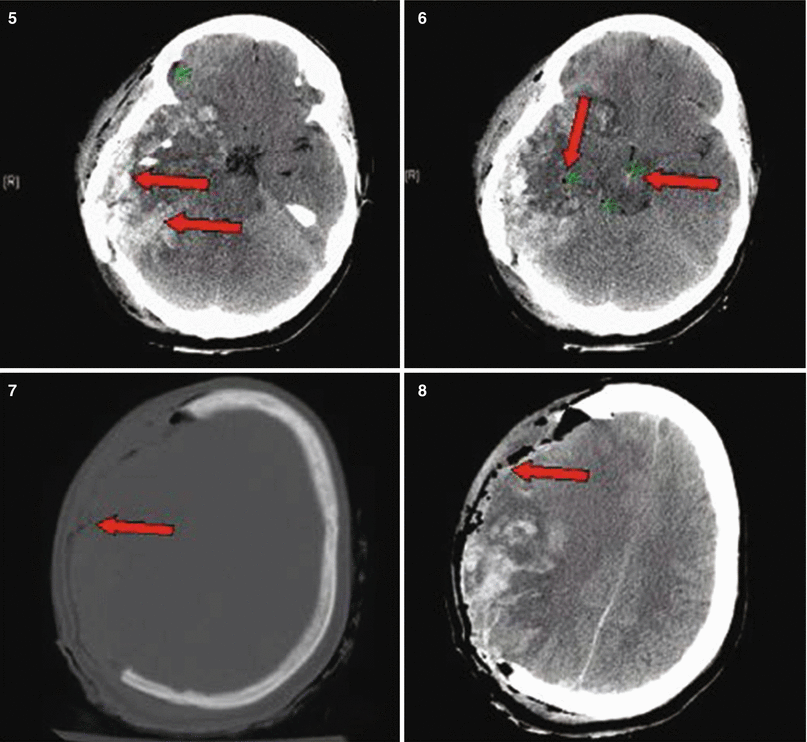
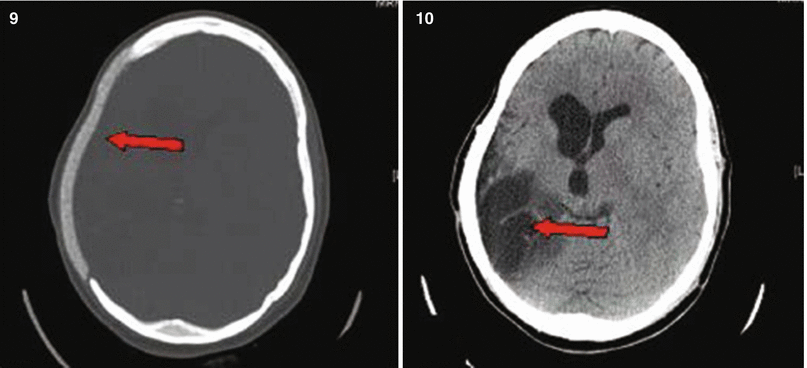
Fig. 27.2
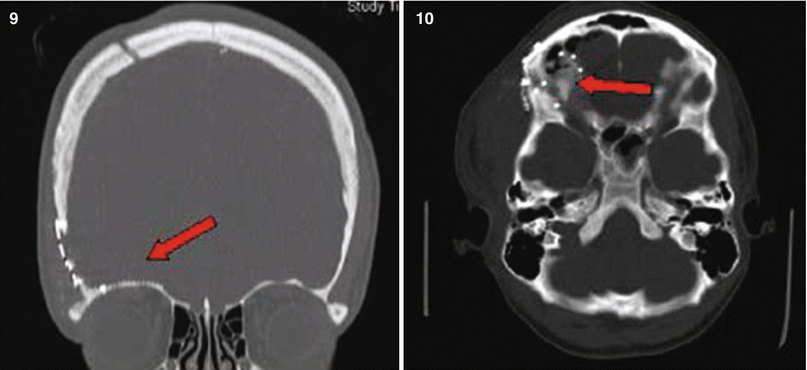
Patient No. 2: a 23-year-old female, who sustained a solitary GSW to the head from close range. Entry wound on the R cheek, exit wound R parietal. Arrows in plates 1 and 2 of this figure illustrate the blow out fracture of the right sided calvarium as seen on CT scout images; This creates a hemispheric decompression. Arrows in plate 3 and 4 indicate the corresponding bony defect with multiple fragments as seen in bone windows of the axial CT scan. Arrows in plates 5 and 6 indicate the hemorrhagic contusion and SAH. Arrows in plates 7 and 8 indicate the hemicraniectomy site (7) and evacuated subdural hematoma site (8). Arrow in 9 points at the inserted hemicranioplasty allograft.Arrow in 10 points at the cystic portion of the encephalomalacia from the bullet tract
No. 3: GO TO THE ER AND WAIT IN THE TRAUMA BAY FOR THE PATIENT TO ARRIVE. If you are out of the hospital, start driving in NOW. Meanwhile organize things by phone on your way. These are most valuable minutes that you can save for later (Fig. 27.3).
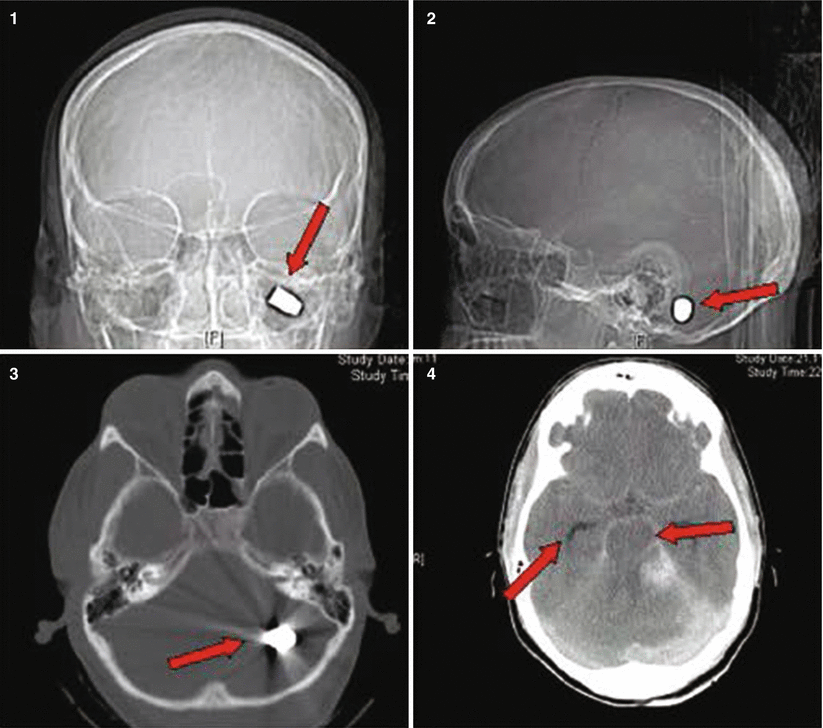
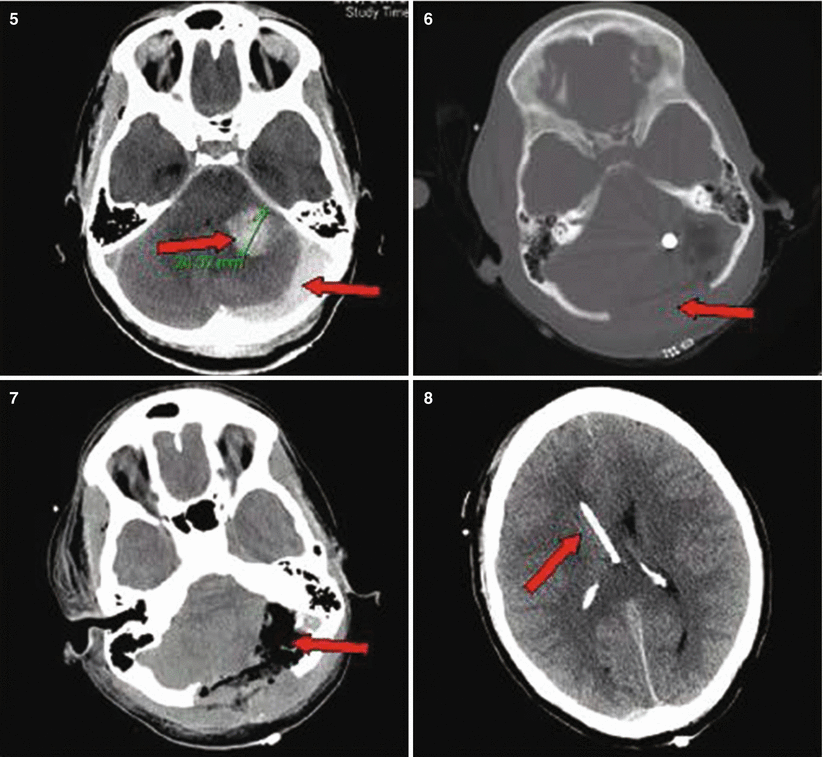
Fig. 27.3
Patient No. 3: a 30-year-old female, who sustained a solitary GSW to the back of her head from close range. Entry wound on the occiput and no exit wound. Arrow in plates 1 and 2 points at the retained bullet case. Arrow in plate 3 shows the bullet case as seen in the corresponding head CT on axial CT bone window. Arrows in plate 4 point at a dilated right lateral ventricle and at left perimesencephalic hemorrhage. Arrows in plate 5 show the enlarging hematoma in the CP angle and a hematoma in the left sided posterior fossa. Arrow in plate 6 shows the bilateralsuboccipital craniectomy site that was created to gain access for evacuation. Arrow in plate 7 points at the evatuation side of the previously seen hematoma in 5. Arrow in plate 8 points at the R frontal EVD catheter inserted to treat the occlusive hydrocephalus
No. 4: Touch base with the ER attending. In an experienced setting, the ER will get prepared early and have identification labels/numbers and a trauma team assigned prior to arrival (Fig. 27.4).
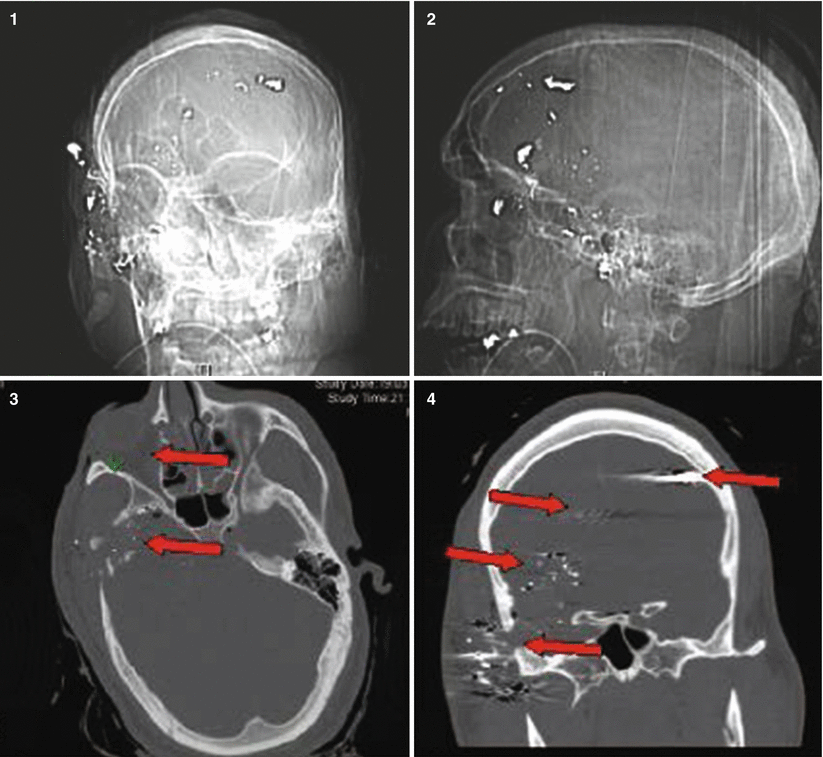
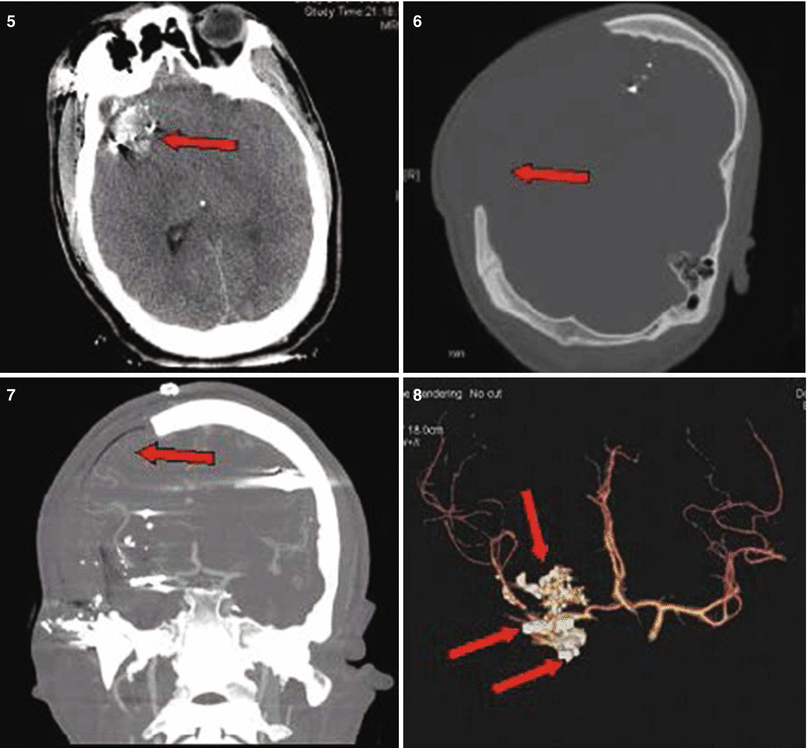
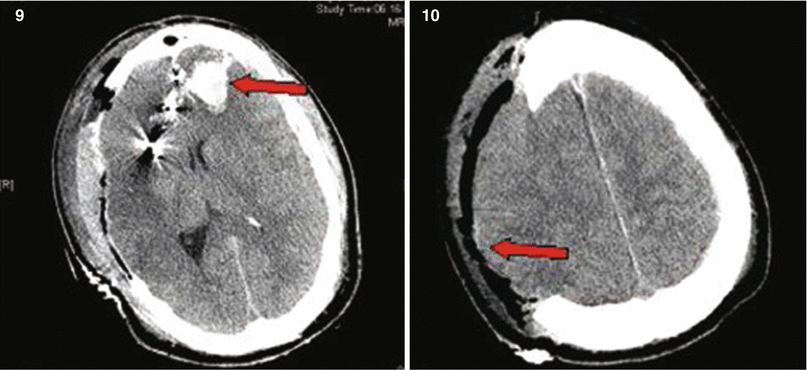
Fig. 27.4
Patient No. 4: a 26-year-old male, who sustained a solitary GSW to the head from distant range. Entry wound at the R ear canal, no exit wound. Plates 1 and 2: scout images A/P and lateral with evidence of multiple bullet fragments on the R extracranially and bilaterally intracranially. Note the large R-sided skull fracture. Arrows in panel 3 an 4 point at the bullet tract as seen on head CT with axial bone windows (3) and in matching coronal reconstructions (4). There are interspersed metal bullet fragments visible with their streak artifact. Arrow in plate 5 points at the temporal lobe hematoma. Arrow in plates 6 and 7 points at the hemicraniectomy site. Arrow in plate 8 points at the R MCA bifurcation with multpiple retained bullet fragments and a surgical clip for the traumatic avulsion site. Arrow in plate 9 indicates the allograft cranioplasty. And plate 10 shows a small left frontal inraparenchymal hematoma
No. 5: Make sure they notify the blood bank for possible need of products with “emergent release.” Make sure they have vasopressors and mannitol/Lasix IV ready and a respiratory therapist to initiate hyperventilation. Remember the rule of 30s: height of bed 30o and hyperventilation with f = 30 for a goal pCO2 < 30.
No. 6: Get the trauma team ready in the bay and assign tasks by talking to the senior/attending running the case. THIS IS NOT THE PATIENT TO PRACTICE ON. Newcomers can stand by and watch, but should stay at a distance and out of the way! Try to pass all preliminary information around as it can be gathered from the EMT-call-in from the scene or en route (ask about patient age, single wound or systemic injury, patient awake or with loss of consciousness (LOC)/comatose; patient intubated, patient stable; blood loss at the scene; other issues).
No. 7: Call the CT scanner upfront that you will bring a critically ill patient ASAP so they keep the scanner FREE for your case!
No. 8: Listen well to what the transport team has to say upon presenting the case; they sometimes know important details (downtime, seizures at the scene, difficulties with the airway, etc.).
No. 9: WATCH if there is any sign of life upon arrival. Get a good glimpse at the patient (I recommend you stand behind the chief running the case at the head end of the patient) and once the primary survey is done.
No. 10: You should get a 10–30–s neuroexamination yourself.
NOW MAKE THE RUN AGAINST THE CLOCK!
27.2 Preoperative and Intraoperative Management
For most TBI strategies, you will find very little class 1 or 2 recommendations. To get a good grip on how to run these scenarios and treat your patient well, watch as many cases as you can during training. Take home the pivotal steps of decision making from seasoned staff. You can often not randomize patients in critically ill settings since it often poses an ethical dilemma; therefore, remember the following points to increase the possibility of a satisfying discharge status of a patient injured by gunshot or a stab wound:
In all trauma patients, let the trauma team perform systematic reviews in the bay and stanch blood ASAP; get the patient lined up (two peripheral 16 G IVs) and treat abnormal vital signs (e.g., hypotension, hypoxia/hypothermia!) before you move to the radiological examinations, and consider any surgical intervention. The minutes spent here are WELL SPENT and make your part SAVE. No one wants to rush the GSW patient to the scanner and see them crashing there. And remember: NO GSW TO THE HEAD goes to the OR without films EVER!
Have one team member assigned as liaison to the relatives if you do not have the time to communicate during the need of swift action. They will be extremely grateful and less anxious. Once you have obtained your scans, make a swift decision: Patients with a GCS of 3–5 AND a devastating scan (bilateral global injury with transventricular bullet trajectory, massive blood or swelling with near-complete herniation, tram track signs) may not be salvageable and warrant conservative treatment alone with ICP-bolt placement and medical management only. Other patients with either improved post-resuscitation GCS > 5 and limited supratentorial injury and a vector that does not show involvement of the fatal zone should be considered for surgery.
NOW TO THE POINTS THAT MATTER:
27.3 Operative Management
Always ask yourself:
“How can I do the best intervention the fastest possible way?”
Here are the 15 most important points on the road to success:
- 1.
Transport the patient yourself from the CT scanner straight to the OR.
- 2.
Position the patient by transferring him from the stretcher onto the OR bed (which has been preplaced correctly in the room since you called from the CT scanner).
- 3.
Apply only the utmost necessary padding to save time (this is not the time to search for pneumoboots or gel rolls).
- 4.
Pin the patient in a Mayfield headrest at straight angles! (either supine or fully lateral). This helps to keep your orientation once you are deep inside.
- 5.
Shave the entire hemiconvexity (be generous!).
- 6.
Scratch the skin to keep your landmarks and pay attention to especially the midline!
- 7.
Use a quick prep solution: e.g., soaking beta-iodine sponges followed by Prevail®; this is not the time to go through six sponges of your three soap elective crani routine.
- 8.
Do not waste the time to wait for using local anesthesia/epinephrine for better hemostasis.
- 9.
Incise with the goal of creating a generous flap to allow for post-OP swelling.
- 10.
Perform a really good sized hemicraniectomy for optimal decompression and do not forget to prepare in all p-fossa lesions a Frazier burr hole so you can place an external ventricular drain (EVD) any time.
- 11.
Save the bone flap on the back table to be used in a freezer-storage protocol, and do not waste time on a second (abdominal) incision! You want to get out of the OR ASAP.
- 12.
Always irrigate copiously with antibiotic solution: e.g., bacitracin®.
- 13.
Perform your wide durotomy BEFORE you place any dural tenting stitches since this decompresses the brain earlier and you save the brain some more vital minutes.
- 14.
Close the dura provisionally, e.g., with an onlay dural allograft (e.g., DuraGen®) to prevent adhesion scarring from the brain surface to the undersurface of the muscle flap. A subgaleal CSFoma is of no concern here, since you will be back for a regular cranioplasty.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree