Introduction
The gastrocnemius flap is one of the most useful flaps. Described very early, it has been proven to be easy to raise and very reliable. Typically, it can be used by non-specialized reconstructive surgeons, since its field of application concerns the area of the knee and upper part of the leg, which is frequently involved in injury and is an area in which prosthetic surgery is frequently performed. As is the latissimus dorsi flap for the upper limb, the gastrocnemius is the mainstay of the armamentarium of flaps that can be used for lower extremity reconstructions and should be known by surgeons in orthopedic and plastic surgery. Although the musculocutaneous flap has significant potential as a functional muscle transplant to restore elbow flexion, the main indication is the use of the medial head as a proximally based pedicled muscle flap for reconstructing defects around the knee. With the increasing number of knee prostheses and the existing risk of skin disunion or infection, especially in the elderly, the medial gastrocnemius flap is the “cornerstone” of the strategy for dealing with problem cases of prosthetic knee replacement.
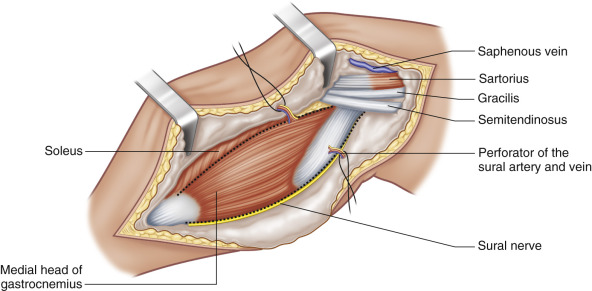
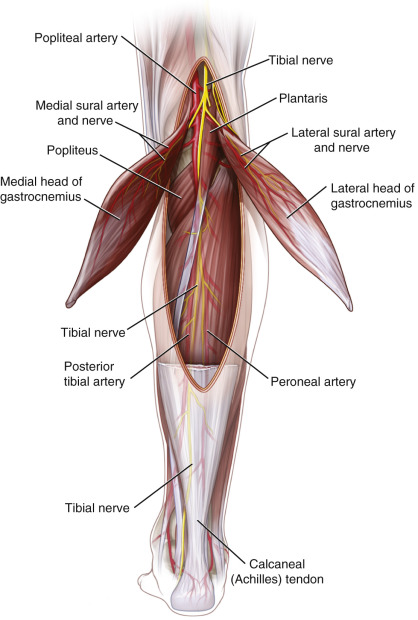
Flap Anatomy ( Figure 50.1 and see Ch. 13 and Fig 13.3 , Fig 13.6 , Fig 13.9 , Fig 13.10 , Fig 13.11 , Fig 13.19 )
The gastrocnemius muscle has two heads: medial and lateral. The medial head originates on the posterior surface of the femur superior to the medial condyle and posterior to the insertion of the adductor magnus muscle. The lateral head originates in the lateral epicondyle of the femur. Both insert into a long common muscle aponeurosis that forms the Achilles tendon with the aponeurosis of the soleus.
- •
The proximal part of the muscle forms the lower triangle of the popliteal fossa, the upper triangle being formed by the diverging hamstring muscles.
- •
The muscle bellies extend from the popliteal fossa to the mid- to distal third of the leg.
- •
The plantaris muscle and tendon lie between the medial gastrocnemius and the soleus muscle and can be used to clearly identify the plane of separation.
- •
The medial and lateral head run side by side and are separated by a fibrous septum.
- •
The gastrocnemius muscles contribute to plantar flexion of the foot through their pull on the Achilles tendon. These muscles also contribute to knee flexion.
Arterial Supply of the Flap ( Figs 50.1 and Fig 13.3 , Fig 13.6 , Fig 13.9 )
The vascular supply is type I in the Mathes and Nahai classification, and each head, lateral or medial, can be mobilized individually on its own neurovascular pedicle. One muscle head can survive totally based on the vascular communications between the two muscle bellies. The dominant vessel in most patients is the medial sural artery.
Medial Gastrocnemius Muscle
Dominant:
medial sural artery
Length: 5.1 cm (range 1.6–9.5 cm)
Diameter: 2.5 mm (range 1.8–4 mm)
Minor:
branches from the lateral sural artery
These branches have variable length and diameter. They are located in the distal half of the muscle and communicate between the two muscle heads.
Minor:
branch from the posterior tibial artery
The branches have variable length and diameter. The distal part of the medial head receives a vascular pedicle from a musculocutaneous artery issuing from the tibialis posterior artery at the midleg. This pedicle gives off a direct skin branch and a muscular branch that divides into two small branches, one for the soleus and the other for the distal part of the medial aspect of the medial head. Not infrequently, this branch is well developed and permits the raising of an inferiorly based portion or the entire muscle based only on this pedicle. It provides an elegant solution to cover the middle or the distal third of the leg.
Lateral Gastrocnemius Muscle
Dominant:
lateral sural artery
Length: 4.8 cm (range 1.8–9 cm)
Diameter: 2.2 mm (range 1.2–3.7 mm)
Minor:
branches from the medial sural artery
These branches have variable length and diameter. They are located in the distal half of the muscle.
Venous Drainage of the Flap
All arteries to these flaps are accompanied by venae comitantes.
Primary:
venae comitantes of the medial and lateral sural artery
Two venae comitantes are found with each artery. The diameter of the veins is approximately 3.5 mm (range 3–4 mm).
Secondary:
superficial veins such as the lesser saphenous vein ( Fig. 13.19 )
This vein can be included with the flap to augment drainage or to serve as primary drainage of the flap. This is particularly useful when a large skin island is included with the flap.
Flap Innervation (see Fig. 50.1 and Fig 13.9 , Fig 13.10 , Fig 13.11 , Fig 13.19 )
Motor:
medial and lateral sural motor nerves that come off the tibial nerve
These nerves are approximately 4–5 cm in length and enter the muscle on its deep proximal surface with the sural vascular pedicle. As the gastrocnemius is a rapid-contraction muscle, it is preferable to cut the nerve when raising a pedicled flap to avoid muscle contraction on the donor site.
Sensory:
skin overlying the medial gastrocnemius muscle
Posterior femoral cutaneous nerve and saphenous nerve (L3–L4) innervate this area. The saphenous nerve follows the course of the greater saphenous vein and can be found near the medial side of the gastrocnemius muscle.
Sensory:
skin overlying the lateral gastrocnemius muscle
The sural nerve (S1–S2) supplies the skin in this part of the calf and the nerve can be found running along the lesser saphenous vein. The nerve runs in a subfascial plane and pierces the fascia in the posterior calf to travel more superficially and supply the skin.
Flap Components
The gastrocnemius flaps are harvested as muscle flaps. They can include the overlying fascia and skin. A strip of tendon can be included with the flap. The flap can be harvested as a chimeric flap with the skin island and muscle harvested based on the same common pedicle.
Advantages
- •
Muscle dissection is rapid in case of a proximally based pedicled flap.
- •
The external diameter and length of the pedicle are suitable for microsurgical transplantation.
- •
Contour deformity following the use of one head is acceptable.
- •
When only one head is raised, functional loss is negligible, compared with the benefit of the procedure.
- •
The medial or the lateral head can be transposed distally by extending the pedicle length. However, this technique is no longer so popular after the recent description of fasciocutaneous flaps for covering the distal leg.
- •
The length of the distal tendon, the length of excision of the body muscle, and the strength of contraction make functional transfer an interesting possibility.
Disadvantages
- •
In case of a free transfer, the prone position is more suitable for dissecting the pedicle but makes transplantation to an anterior recipient site more difficult.
- •
The posterior incision is not desirable in females.
- •
The elevation of a pedicled flap in supine position can be difficult in case of stiffness in hip or knee.
- •
The donor site following the transplantation of an extended musculocutaneous flap is not cosmetically acceptable.
Flap Design and Flap Markings
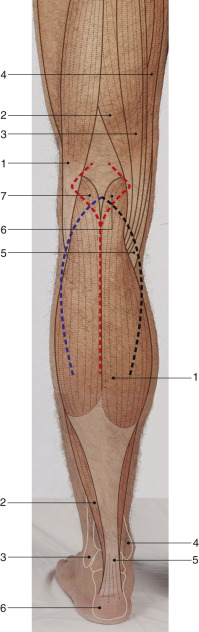
Anatomic Landmarks ( Fig. 50.2 )
A transverse line is marked in the posterior knee crease; this coincides with the level of the takeoff of the medial and lateral sural vessels. The midline raphe separating the medial and lateral heads and the distal ends of the muscles are marked. These landmarks can be palpated in most patients.
General Thoughts About Flap Design
The skin over the calf can be harvested in its entirety, encompassing the entire width of the calf and from the popliteal fossa to approximately 10 cm past the distal end of the muscle bellies. In order to close the defect primarily, <6 cm of skin can be included.
Skin grafting is required for defects >8 cm and should be performed without hesitation in order to prevent the occurrence of compartment syndrome.
The proximal part of the skin island should be at least 4 cm beyond the popliteal crease in order to avoid discomfort with knee motion.
Many of the branches off the sural artery, supplying the overlying skin, exist in the distal medial half of the muscle bellies. Therefore, when harvesting an overlying skin island, it is preferable to design the island to include this region.
Special Considerations
If a small skin island is to be included with the flap, a handheld Doppler can be used to map the location of the skin vessels prior to beginning the surgery. The medial incision is performed and the skin vessels are located; then the skin island design is adjusted as necessary.
Differences in Design, if Any, When Performing the Flap as Pedicled or Free
No difference exists when the muscle is harvested as a free flap or pedicled flap. In order to extend the arc of rotation of a myocutaneous gastrocnemius flap, the skin island can be designed more distally.
Flap Dimensions
Muscle Dimensions
Medial Head
Length: 15 cm (range 13–20 cm)
Width: 7 cm (range 5–9 cm)
Lateral Head
Length: 12 cm (range 11–16 cm)
Width: 5 cm (range 4–7 cm)
Skin Island Dimensions
Length: 10–15 cm (maximum 20 cm)
Width: 6–10 cm (maximum 15 cm)
The skin over the medial and lateral head is supplied by musculocutaneous perforators that can each supply a large area of skin. Most perforators exist in the proximal part of the calf, over the muscle; however, the skin can be included based on some of the skin vessels that supply the skin distal to the muscle heads. The dimensions for skin islands over the lateral gastrocnemius muscle are adjusted to be slightly smaller than described above. However, depending on the actual size of the musculocutaneous branch, large flaps can be harvested.
Patient Positioning
The best compromise is the supine position with the knee flexed and the hip abducted, flexed, and externally rotated. In this position, even a free transfer of the medial head can be raised. Free transfer of the lateral head requires the prone position but this procedure is not often used.
The prone position is used when the defect requires this position. The harvest of the flap is simple and straightforward in this position.
If the patient suffers from severe hip stiffness, the prone position may be chosen or the patient can be placed in a lateral decubitus position with the flap donor leg down.
Preoperative Preparation
In case of previous injury to the lower extremity with suspicion of injury to the popliteal vessels or its branches, an arteriogram, magnetic resonance angiogram, or computed tomography (CT) angiogram are performed to assess the permeability of the main vessels and the presence of the sural arteries.
The contour of the muscle can be assessed clinically by asking the patient to flex the ankle against resistance. This allows an evaluation of the length and chiefly the volume of the body of the muscle. One should keep in mind that the thinner the muscle, the easier transplantation will be. A thick-bodied muscle is always more difficult to mobilize.
Anesthetic Considerations
If the defect to be reconstructed is in the same extremity, spinal or epidural anesthesia may suffice; otherwise, general anesthesia is instituted. Generally speaking, we prefer general anesthesia as it is more comfortable for the patient. In cases where the flap is to be transferred to the upper extremity, the procedure can be performed under regional blocks with sedation of the patient.
Technique of Flap Harvest
Elevation of the medial and lateral heads is discussed separately.
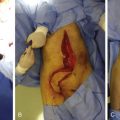
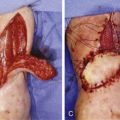
Proximally Based Pedicled Medial Gastrocnemius Muscle Flap ( Figs 50.3 , 50.4 )
The incision starts at midcalf, 2 cm behind the posterior border of the tibia on the medial aspect of the leg, and curves proximally to reach the popliteal fossa that it crosses by an angulated incision. Care should be taken to avoid injury to the great saphenous vein and saphenous nerve. The crural fascia is incised in line with the skin incision and the fascia and overlying skin of the calf are elevated off the muscle as far laterally as the plane between the two heads of the gastrocnemius. It is advised to begin the elevation by separating the two heads in the midline. The sural nerve and lesser saphenous vein are identified on the lateral border of the medial head in the aponeurotic sheet between the two heads and are usually covered by a thin layer of muscle fibers from the medial head. The nerve and vein are dissected and retracted posterolaterally. The aponeurotic plane between the two heads is identified and progressively incised while separating the two muscle bellies from distal to proximal. The space between the proximal part of both heads is identified, taking care to preserve the neurovascular pedicle, which lies on the lateral aspect of the medial gastrocnemius muscle. Before detaching any part of the muscle, the plane between the soleus and the gastrocnemius muscle is identified on the medial border of the gastrocnemius and developed with a finger. This plane houses the plantaris tendon, which lies between the gastrocnemius and soleus muscles. Skin vessels traversing this plane must be ligated or cauterized and cut. Finally, the distal tendon is severed and the flap is raised from distal to proximal. Usually the distal tendon of the gastrocnemius can be split for a few centimeters from the soleus component in the context of the Achilles tendon and included in the flap if necessary for patellar or quadriceps tendon reconstruction. The muscular body of the medial head is long and the arc rotation of the transfer allows easy coverage of the proximal third of the leg and the medial and anterior aspects of the knee.