Introduction
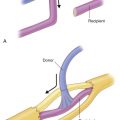
Reconstructive surgery has, as its premise, the principle of restoring form and function utilizing surrounding or distant tissues while minimizing morbidity at the donor site. While muscle flaps remain a viable option for reconstructive surgery, their use has become less important in recent years with the advent of perforator flap surgery. No longer is it necessary to take muscle as a carrier of blood supply to the overlying structures; vessels supplying skin flaps can be dissected in a retrograde fashion through their intramuscular course or in the fascia between muscles until the adequate length and caliber required are reached. The extensive development of perforator flap surgery has also allowed for the harvest of tissue in a free-style manner from any part of the body where a perforator or skin vessel is found ( Fig. 62.1 ). This has led to an increase in the number of flaps available, a greater versatility, and even better outcomes in reconstructive surgery. Locating these vessels can be performed safely and reliably with the use of Doppler signal mapping or other imaging study techniques. This tool allows for mapping of all skin vessels over 0.5 mm in size in the area where the flap is to be harvested from. The donor site for tissue transfer is selected, based on the type of tissue desired and required at the recipient site, the volume necessary to fill the defect, the pliability desired, and the color that best matches the recipient site.
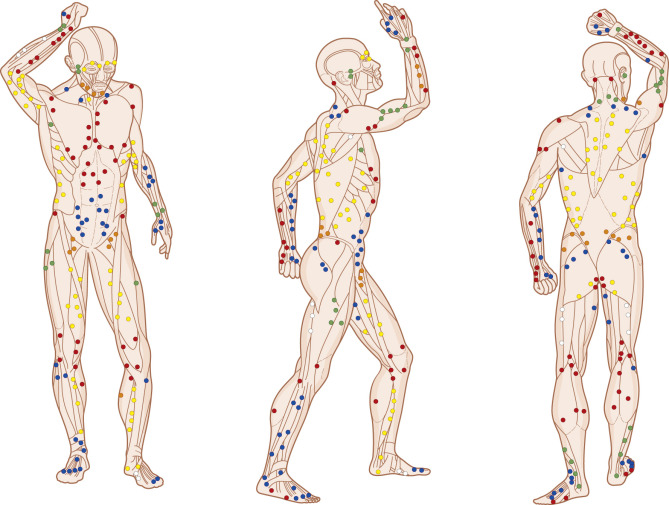
Once the vessels are mapped in a given area, even if the surgeon is unfamiliar with the region, flap harvest can begin by surgically exploring the region for vessels of a suitable size. The concept and approach have been termed “free-style flap harvest” and a flap harvested in this manner is termed a “free-style flap.”
In fact, the concept of free-style flap harvest has been introduced in one form or another over many years. Many surgeons have used this approach in cases where anatomic variations were met, or when problems arose during flap harvest such as trauma to the vessels. Taylor and Daniel in 1975 dissected the perforators of the gastrocnemius musculocutaneous flap back to the sural vessels. During Wei and colleagues’ anatomic study of the fibula osteoseptocutaneous flap, they performed intramuscular dissection of perforators through the soleus muscle when they were encountered. What they were performing at the time was essentially a free-style flap harvest. Koshima introduced an innovative concept and the surgical technique of “supramicrosurgery.” He harvested flaps from the paraumbilical region and based them on the suprafascial component of skin vessels. The free-style flap harvest principle has some similarity to the previously mentioned approaches, and the vessels supplying the flap are traced in a retrograde fashion through whatever course they take until the appropriate size and length are reached.
Free-style flaps can be harvested as local or free flaps, and can be composed of a variety of tissue types. Reconstructive surgery will continue to rely on flaps that have been studied anatomically and have been proven clinically to be reliable and safe. In addition to being a way of providing tissue as a flap, free-style flap surgery has played a role where anatomic variations are encountered or unexpected situations are met. More recently, it has been used to allow for a flap to be “recycled” and used for the reconstruction of a second defect following a previous reconstruction with a flap. The area is explored for vessels with the use of either Doppler mapping or immediate exploration, the flap is designed based on a set of principles that are discussed later in this chapter, and the flap is harvested. We believe that having had experience with perforator flap surgery has allowed surgeons to feel comfortable in performing free-style flaps, and this in turn has aided in alleviating anxiety when approaching any flap harvest, particularly when it is less familiar to the surgeon. This allows the surgeon to begin flap surgery knowing that many alternative plans are available if an unexpected situation is encountered.
Flap Anatomy
Knowledge of anatomy of the region where a free-style flap is to be harvested is still important. In order to safely carry out the harvest of any block of tissue from any region, it is essential that the surgeon avoid critical structures in order to minimize damage at the donor site. Detailed regional anatomic landmarks, however, play a role that is less significant when dealing with free-style flaps. Ideally, “back-up” flaps can be available in the region where a free-style is to be harvested. This is particularly important when the surgeon begins to explore a new region for free-style flaps. In the authors’ experience, the thigh was used initially as the region to explore the reliability and safety of free-style flaps. Given the large experience acquired over the years with flaps from the thigh, it became clear that the thigh is an ideal location to realize this concept. We always marked the anatomic landmarks for the anterolateral thigh flap in the event we encountered problems with the free-style flap. The incisions were planned so that the back-up flap could be used in case the skin vessels to the free-style flap were found to be short or small, or were injured during the dissection. The main landmarks are the location of Dopplered skin vessels. Because our experience and that of others has proven that dissection and anastomosis of vessels ≥0.5 mm is technically feasible and reliable, all 374 vessels that were mapped by Taylor and colleagues can theoretically provide reliable pedicles for a free-style flap.
The area that is selected for a flap donor site is chosen based on the defect to be reconstructed and on a donor site that allows for a well-healed scar in an inconspicuous location. The flap is chosen that allows for versatility in flap design; provision of tissue volume that is adequate to reconstruct the defect; and good match in color, texture, and pliability at the recipient site. Additionally, if sensory reinnervation is desired, the flap is chosen from an area that had sensory nerves that can be harvested with the flap. Whenever possible, the location of the donor site should allow for a two-team approach.
Flap Components
Any type of tissue can be harvested as part of a free-style flap. Typically, free-style flaps are harvested as cutaneous flaps. Other components such as muscle, nerve, or bone can be harvested based on the same vessels if branches also supply those tissues. However, predicting the course of these vessels is difficult. If bone, muscle, or nerve is required to reconstruct a defect, known flaps are recommended for use.
Advantages
- •
Free-style flaps can be harvested from any location where a skin vessel is found.
- •
The type of tissue can be selected based on the requirement at the recipient site. The region of the body that is most similar in color, texture, pliability, and thickness is chosen and a flap is harvested from that region.
- •
This technique is particularly useful in patients with limited flap donor sites such as in burn patients.
- •
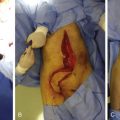
The free-style approach can be applied to “recycling” a previously used flap. The same flap can be reused by finding a vessel within the flap through the use of Doppler ultrasonography and a free-style flap is harvested. This achieves the goal of reconstructing a defect as well as debulking of a previously used flap ( Case 62.2 ).
- •
Although free-style flaps may seem unpredictable initially, with experience in harvesting flaps in a given region such as the thigh or lower leg, the surgeon quickly becomes familiar with the size and location of vessels and the amount of tissue that can be carried reliably based on those vessels.
- •
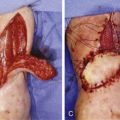
Dissection of free-style flaps is usually performed in the suprafascial plane, which preserves more structures such as nerve and fascia at the donor site while allowing the surgeon to obtain a thinner flap. The fascia is entered at the point where the skin vessel pierces the fascia and followed only to the point where adequate length and vessel caliber are achieved. Subfascial dissection is also possible and usually easier and quicker ( Case 62.3 ).
Disadvantages
- •
Pedicle size, course, and length are less predictable.
- •
The amount of tissue that can be harvested based on a given skin vessel is difficult to assess. The surgeon must acquire a feel for how much tissue can be carried based on a given size of perforator and this depends on the size and amount of pulsatility in a given vessel.
- •
Free-style flap harvest requires accurate localization of the skin vessels utilizing Doppler mapping, which requires familiarity through learning.
- •
The surgeon may have to anastomose vessels of small caliber.
Flap Design
Anatomic Landmarks
The main landmark for a free-style flap is the location of the Dopplered skin vessel. Other landmarks are those for known flaps in the region from which the free-style flap is harvested. In the thigh, the anterolateral thigh flap is marked, in the chest the deltopectoral flap is marked, in the back the parascapular flap is marked, and so on. The nearest known flap is marked and an incision is made along the border between the free-style flap and the known flap. This is performed during the harvest of the first few cases in a given region. When success in harvesting free-style flaps from a given region is achieved, marking of back-up flaps becomes less necessary.
General Thoughts About Flap Design
- 1.
Each area of the body is perfused by a given perforator based on the perforasome theory. Each perforasome is connected to an adjacent perforasome through direct and indirect linking vessles.
- 2.
Vascular axis follows the axiality of the linking vessels that follow the long axis of the limbs. In the arm and leg the flap is designed along the length of the limb.
- 3.
Linking vessels in the trunk are commonly directed perpendicular to the midline and follow an oblique transverse direction.
- 4.
The surgeon determines the final flap design based on the location of the skin vessel as determined by the intraoperative findings. The markings can change to place the located skin vessel in either a more central location or a more eccentric location based on the location and the distance between the recipient vessels and the defect or, in the case of a pedicled flap, based on the arc of rotation necessary to reach the defect. If, during the exploration, a larger skin vessel is found, this vessel may be chosen instead of the originally mapped one.
- 5.
When the free-style flap is harvested from the limb, the surgeon must realize which vessels are considered major and are not amenable to sacrifice. We therefore mark the skin territory based on the most distal vessel that exists and the one that is farthest away from the vessels that cannot be sacrificed (superficial or deep femoral arteries). We also try to choose the ones that are not over fixed areas. In those areas, the vessel course is commonly more perpendicular. In the thigh, for example, we choose the perforator that is farthest from the superficial femoral artery. The skin vessel can be placed in an eccentric position to increase the reach of the flap. Theoretically, the shortest pedicle will be at least the straight distance between the Dopplered vessel and the vessel that cannot be sacrificed.
- 6.
There is no set algorithm for deciding how much tissue can be harvested based on a given skin vessel. The size of the vessel and the number of vessels dictate how much volume can be harvested. More than one skin vessel is included whenever possible, to ensure better circulation.
- 7.
When beginning the process of exploring a given region for free-style flaps, the free-style flap is marked, so that it shares a common border with the “back-up” flap. The procedure is begun by incising the common border. Vessels supplying the free-style flap are located and the rest of the harvest is performed. If no vessels are found, the back-up flap is used. Once the surgeon is comfortable with the procedure of harvesting free-style flaps based on Doppler mapping of a given region, having a back-up flap in the immediate surrounding region becomes less important.
After performing several free-style flaps, the technique and the entire procedure become much quicker.
Special Considerations
Characteristics of skin requirements at the recipient site must be considered when designing free-style flaps. For example, if hairless skin is required, then free-style flaps should be harvested from areas such as the ulnar aspect of the forearm or back, etc. The area where the flap is taken from is based on finding tissue that matches the recipient site skin color, pliability, and bulk. Also, the skin vessels of the flap should match the recipient vessels’ size and should reach the recipient vessels without vein grafts.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree