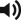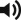
Introduction
With an outstanding length available for harvest, a solid and sizable bone stock, a reliable blood supply, an allowance for manipulation of the components of the flap while maintaining adequate blood supply, and the ability to carry bone, skin, muscle, and fascia, the fibula flap has become one of the most commonly used vascularized osseous and osteocutaneous flaps for reconstruction of osseous defects around the body, particularly the mandible, radius, femur, and tibia. Ueba and O’Brien evaluated the fibula as a donor site for free microvascular bone flap transfer prior to Taylor et al’s report in 1975 of the first two clinical cases of microvascular fibula flaps used for reconstruction of tibia bone gaps. Bovet’s work, which followed, demonstrated that muscle could be carried along with the fibula bone. It was not until Wei and colleagues’ anatomic and clinical study in 1989, that surgeons were convinced of the reliability of the skin paddle of the osteoseptocutaneous fibula flap. Since then, the skin has served a critical role in providing a cutaneous component when necessary, and for providing a good monitor for the bone component. In 1989, Hidalgo was the first to report on a significant series of vascularized fibula grafts for mandibular reconstruction. Free vascularized bone flaps were shown to heal more rapidly, with fewer complications and earlier functional recovery, and their use for larger defects, particularly in radiated beds, has been found to be superior to that of non-vascularized grafts.
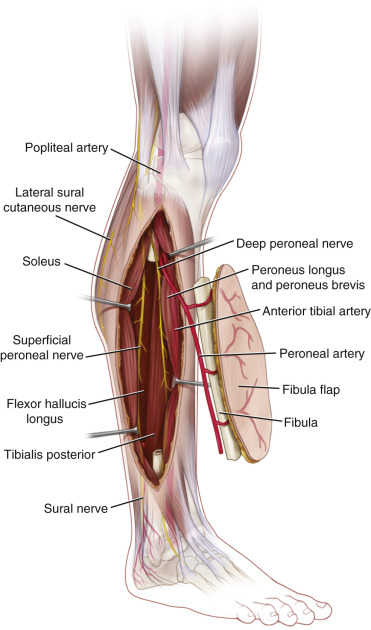
Flap Anatomy (see Fig. 52.1 and Fig 13.6 , Fig 13.7 , Fig 13.8 , Fig 13.19 )
The fibula is a long, thin bone with anterior, posterior, medial, and lateral surfaces. The head articulates with the tibia. The biceps femoris and the lateral collateral ligament attach to the fibula.
Arterial Supply of the Flap (see Fig. 52.1 and Fig 13.6 , Fig 13.7 )
The arterial supply of the fibula flap is via both a dominant nutrient endosteal and minor periosteal septal and muscular branches from the peroneal artery. The external diameter of the peroneal artery is 1.5–2.5 mm and the pedicle length is between 2 cm and 6 cm. The pedicle length varies with the amount of bone that is resected.
Dominant:
nutrient artery from peroneal artery
Length: 1–2 cm
Diameter: 1.0 mm
The nutrient artery arises as a branch of the peroneal artery and enters the fibula posterior to the interosseous membrane into the nutrient foramen approximately 15 cm below the styloid process in the posterior medial edge of the mid-fibula two-fifths of the way down. The vessel length is 1–2 cm and the average diameter is 1.0 mm. After traversing a short intracortical path, the nutrient artery divides into an ascending and a descending branch. The descending branch is often longer than the ascending. Occasionally, there are two nutrient arteries.
Minor:
periosteal and muscular branches from peroneal artery
Diameter:
vessel diameters at their origin range from 0.8 mm to 1.7 mm
Periosteal and muscular branches to the fibula. They are derived from the peroneal artery located along the fibular origin of musculature and posterolateral septum. Musculoperiosteal vessels course primarily through the flexor hallucis longus and tibialis posterior muscle. There are typically 4–8 cutaneous arteries arising from the peroneal artery. These vessels are segmental, consisting initially of periosteal and musculoperiosteal branches, entering from a distance of 4–27 cm below the fibular head and continuing within the posterior crural septum, between the soleus and peroneus muscles, or back through the flexor hallucis longus muscle to supply the lateral leg skin. The middle third of the fibula shaft contains the greatest number of these periosteal branches. When there are no septocutaneous branches, musculocutaneous branches can supply adequate circulation to the same skin area.
Venous Drainage of the Flap (see Fig. 13.19 )
Primary:
venae comitantes of the peroneal artery
Length: 2–6 cm
Diameters: 2–4 mm
Comment: often there are two venae comitantes
Secondary:
superficial venous system
Length: 2–6 cm or longer
Diameter: 2–4 mm
Note: In the case of a fibular osteoseptocutaneous flap a superficial vein (commonly the lesser saphenous) draining the skin paddle may sometimes be used as adjunctive drainage of the flap. This is particularly useful when a large skin island is harvested.
Flap Innervation
Sensory:
The lateral sural nerve and terminal sensory branch of the superficial peroneal nerve (see Figs 13.8 , 13.19 ). Sensory innervation to the corresponding lateral calf skin territory is largely supplied by the lateral sural nerve, which is of adequate size to allow microscopic anastomoses. Although not routinely performed, lateral sural sensory or superficial peroneal nerve coaptation may be performed, and this sensory feedback may improve oral function or tactile penile sensation if a phalloplasty is performed.
Motor:
Although a muscle segment can be harvested with this flap, there are no indications for harvesting a functional muscle with this flap.
Flap Components
The fibula flap is harvested as a bone flap and may include regional musculature (soleus or flexor hallucis longus), and/or overlying skin.
Advantages
- •
Provides vascularized bone that is suitable in cases of recipient site wound contamination, scarring, radiation, or infected bone cases following debridement.
- •
A long segment of straight, triangular, high-density cortical bone (20–26 cm in adults) may be harvested, which is capable of bridging long osseous defects and resisting angular and rotational stresses, considered ideal for extremity axial skeleton reconstruction.
- •
Fibula size matches the size of the radius and ulna, and snugly fits into the medullary cavity of the humerus, femur, and tibia.
- •
As an osteoseptocutaneous flap, the overlying skin connected to the bone by the posterior crural septum, may be readily manipulated, allowing greater versatility in wound closure compared with other osteocutaneous flaps (i.e., iliac crest and scapular osteocutaneous flaps).
- •
Well-defined vascular supply allows for multiple osteotomies (2–3 cm bone segments), which is particularly important in craniofacial contouring procedures.
- •
Suitable donor vessels (peroneal artery, 1.5–2.5 mm; vein, 2–4 mm) allow for anastomoses to large vessels in the head and neck, and upper and lower extremities.
- •
Acceptable donor site morbidity due to tolerable loss of peroneal artery and venae comitantes without the need for reconstruction and limited functional disability in most cases
Disadvantages
- •
Obvious donor scar, particularly when a skin component >4 cm is included and skin grafting is necessary. This is even less desirable in females.
- •
The technique of flap harvest requires a steep learning curve and can be lengthy and tedious in inexperienced hands.
- •
Noticeable limitations and discomfort in ankle function and range of motion with aggressive physical activity may result after fibula harvest, particularly if tibiofibular fusion is performed.
Preoperative Preparation
Preoperative assessment to determine whether a patient is a candidate for a vascularized fibula transfer begins with a careful medical history to identify any conditions that could indicate unreliability of the peroneal artery as a pedicle for free tissue transfer. These conditions include peripheral vascular disease, deep vein thrombosis, trauma, venous stasis disease, or arteritis. The knee and ankle joints should be assessed for range of motion and laxity. A foot Allen’s test should be performed with a Doppler probe ensuring a signal for the dorsalis pedis and posterior tibial artery with occlusion of the other vessel. Peronea magna, which is associated with hypoplasia or absence of both the anterior and posterior tibial arteries with the peroneal artery as the sole arterial supply for the foot, must be ruled out and may occur in up to 8% of the population. In most centers around the world, in the absence of trauma to the lower extremity and previous surgery, clinical examination is used to evaluate the blood flow to the extremity prior to flap harvest. CT angiograms are used routinely in our center for evaluation of patients’ extremities prior to fibula harvest, particularly in patients with a history of trauma. Duplex ultrasonography provides a potential compromise for preoperative evaluation, without the invasiveness, potential risk, and expense associated with angiography. Intraoperatively, prior to transecting the peroneal artery distally, the surgeon should visualize the posterior tibial artery in order to make sure it exists and appears to be normal.
Flap Design ( Figs 52.2 , 52.3 )
Anatomic Landmarks
The head of the fibula, the lateral malleolus, and posterior border of the fibula connecting the head of the fibula and the lateral malleolus are marked. The mark at the posterior border of the fibula identifies the posterior intermuscular septum that carries the vessels supplying the skin. A point 4 cm below the head of the fibula and a point 6 cm above the lateral malleolus are the most superior and inferior margins of the bony stock that can be harvested without causing significant instability of the knee and ankle.
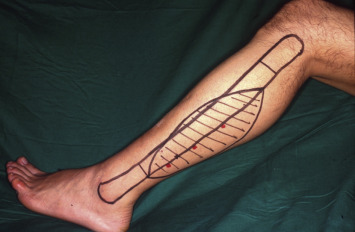
General Thoughts About Flap Design
The fibula bone receives its blood supply from endosteal and periosteal vessels. The nutrient artery provides the endosteal supply, and the periosteal branches of the peroneal artery provide the periosteal supply. When designing the flap, an attempt should be made to include the nutrient vessels whenever possible (in most cases there is only one). If the segment of bone required is short, and the pedicle required is short, the flap can be centered over, or designed to include the predicted location of the nutrient vessel. If the bone required is long, or if the pedicle length required is long, the majority of the bone stock may have to come from the distal leg and therefore rely on periosteal blood supply only.
The right leg or the left leg can be used as a source for the fibula flap. When a bone flap is required without the skin, there is no preference of one over the other as far as the recipient site is concerned. Unlike the iliac crest flap, when harvesting a fibular osteoseptocutaneous flap, the skin paddle can be rotated over the bone due to the fact that the septum is thin and mobile and allows for this to happen. However, if muscle is included during the dissection of the skin vessels, the arc of rotation of the skin paddle over the bone may be more limited. In that situation, the side to use for flap harvest should be carefully planned. The left side is preferable in most patients because it is the less dominant leg in most individuals and is used less during driving a car.
The peroneal nerve (see Fig. 13.8 ), lying inferior to the head of the fibula, can be palpated during the marking of the patient; this can more clearly identify the location of the nerve and avoid injury to it during the dissection.
When the skin island is small, the anterior incision will most likely lie over the lateral compartment and the subfascial dissection can start at that point. However, when the skin island is large, the anterior incision may lie over the anterior compartment. In that case, it is easier to dissect in the suprafascial plane posteriorly until the surgeon is over the lateral compartment. At that point, the fascia is incised and the dissection continues in a subfascial plane. Otherwise, if the dissection in a posterior direction proceeds in the subfascial plane over the anterior compartment muscles, the surgeon will have to pass through the anterior intermuscular septum before reaching the lateral compartment and eventually the posterior intermuscular septum which contains the skin vessels. This will cause confusion during the dissection and may increase the difficulty of the dissection.
When designing the skin island, it is centered over the posterior crural septum, which contains the Dopplered perforators. Occasionally, the perforators do not pass through the septum and actually pass through the FHL and/or soleus muscles and may therefore lie posterior to the septum.
Special Considerations
- •
At least 4 cm of fibula bone is preserved proximally (below the head of the fibula) in order to preserve the stability of the knee. This is achieved by maintaining the attachment of the tibia to the fibula, and the biceps femoris muscle and the fibular collateral ligament to the head of the fibula. The proximal portion of the fibula hosts parts of the origins of the peroneus longus muscle, extensor digitorum longus muscle, extensor hallucis longus muscle, soleus muscle, and the tibialis posterior muscle. Additionally, minimizing dissection at that level will help avoid injury to the peroneal nerve.
- •
A two-team approach is performed whenever feasible (i.e., head and neck and upper extremity reconstructions).
- •
Although not recommended, including the FHL and the tibialis posterior can be harvested with the flap; and including parts of the soleus muscle may lower the chance of injury to the skin vessels. The skin vessels either travel within the posterior intermuscular septum, or pass through the soleus muscle on their way to the skin. In the latter case, they can be dissected from the muscle by using perforator techniques or a segment of the muscle can be included with the flap.
- •
Preoperative CT angiography is required in patients who have abnormal or absent pulses or Doppler signals on physical examination, in trauma victims with severe crush or cutting injuries, and in patients suspected of having severe atherosclerosis. Conventional angiography can be performed if CT angiography is inadequate.
- •
Although the dissection described for the osteocutaneous flap begins with the anterior incision first, beginning the dissection with the posterior incision is acceptable and has the advantage of decreasing the chance of confusion about the location of the skin vessels. Care is taken not to injure the lesser saphenous vein and sural nerve, particularly when the skin paddle is large.
- •
The superficial peroneal nerve is located in the proximal part of the peroneus longus muscle running under the deep surface and should be avoided during the dissection unless sensation is needed in the skin paddle (i.e., fibula flap phalloplasty).
- •
There are two ways to work with the fibula after harvest. This is performed on the back table and the segment to be used is selected and marked. At that point, the rest of the bone needs to be excised without injuring the pedicle. In order to perform this excision, the bone and the pedicle need to be separated. The separation can be performed in two ways. An incision using a knife can be performed longitudinally over the bone on the side opposite the pedicle and a subperiosteal dissection can be performed circumferentially. The bone is exposed and cut in the appropriate location. This method will leave the blood supply intact; however, it will leave a large periosteal muscular segment that may be bulky during the inset. This tissue can be used as vascularized tissue for coverage of parts of the wound, or exposed bone, or can be wrapped around the fibula to create a pseudo-joint. The second method is to cut the periosteum at the level of the mark (bone cut level), and denude the fibula circumferentially except for over the pedicle. This is easier; however, it may have a higher chance of injuring the pedicle.
- •
If an osteocutaneous flap is used to reconstruct a defect and the vessels thrombose and cannot be salvaged, the skin island is debrided and replaced with another skin flap and the bone is kept in place. The patient can be sent to hyperbaric oxygen (HBO) therapy to increase the chance of bone revascularization.
- •
During inset, bone-to-bone contact of the fibula flap bone and native bone ends at the defect should be maximized. The opposition and stability can be maximized by creating steps, wedges, or any method that articulates the bone ends together, or the bone is telescoped into the recipient bone when the size is appropriate. Good opposition will allow for bone healing without the need for placing many screws into the fibula bone flap. The plate spans the fibula flap and one or two screws only into each fibula bone segment of 2–3 cm are adequate for fixation.
Difference in Design, if Any, When Performing the Flap as Pedicled or Free
When using the fibula flap as a pedicled flap, the arc of rotation can be up to 180° if care is taken during the inset to avoid torsion of the pedicle. Careful design of the flap allows for fewer complications during the inset. The defect location should be measured carefully in relation to the fibula bone. The location of the bone to be harvested depends on the distance of the defect from the fibula bone, on the size of the defect, and on the location of the nutrient vessel supplying the fibula bone (the nutrient vessel is included if possible but it is not required for a successful reconstruction). The bone stock required for reconstruction is harvested as distal as possible to optimize pedicle length. Proximal osteotomies on the fibula allow for a wider arc of rotation.
Flap Dimensions
Skin Island Length
Average 12 cm, maximum 32 cm
Skin Island Width
Average 6 cm, maximum 14 cm
Bone Length
Average 16 cm, maximum 30 cm
Note: Maximum bone length is harvested (total minus 4 cm in the upper part and 6 cm in the lower part) in most cases in order to expose and achieve as much pedicle length as possible. The bone to be used for the reconstruction is later chosen based on the pedicle length required and on the location of the nutrient vessel in relation to that.
Flap Markings
The outline of the fibula, including the lateral malleolus and head of the fibula, is marked. This posterior aspect of the bone marks the posterior intermuscular septum that carries the vessels supplying the skin. A point 4 cm below the head of the fibula and a point 6 cm above the lateral malleolus are the most superior and inferior margins of the bony stock that can be harvested without causing significant instability of the ankle. When marking the skin island, it is centered over the posterior crural septum, which contains the Dopplered perforators.
Patient Positioning
Position the patient supine on the operating table with the patient’s knee flexed 90° and the foot fixed to the table, with the pelvic girdle interiorly rotated with the assistance of a roll placed under the ipsilateral hip. A tourniquet is used around the mid-thigh and the flap is commonly raised under ischemia. A stack of sterile towels should elevate the heel so that the leg is not resting on the operating table, which allows the muscles and tissues to fall away from the fibula. The flap may also be raised with the patient in the prone position, if necessary, using a roll under the anterior ipsilateral hip and bending of the leg is not required.
Anesthetic Considerations
General anesthesia is commonly required for flap harvest due to the pain involved with a thigh tourniquet, length of the procedure, and the need for immobility during the pedicle dissection. A regional block may be considered in cases of lower extremity reconstructions or upper extremity reconstructions where blocks of the lower and upper extremities can be performed. However, due to the usual length of the entire operative procedure and delicacy in the steps of flap harvesting, inset, and microvascular anastomoses, regional anesthesia is not advised and a general anesthetic is recommended.
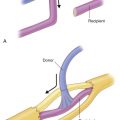
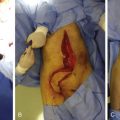
Technique of Flap Harvest ( Fig. 52.3 )
Osseus Flap
A line is drawn from the fibular head to the lateral malleolus indicating the submuscular and subcutaneous course of the fibula. The mid-point of this line is marked indicating the approximate location of the nutrient vessel. The desired length of fibula is typically 15–16 cm in an adult, and this is marked using the approximate location of the nutrient vessels as the central point of the donor osseous segment.

Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree