Deltopectoral Skin Flap As A Free Skin Flap Using The Internal Mammary Vessels, Revisited: Further Refinement in Flap Design, Fabrication, and Clinical Usage
K. SASAKI
M. NOZAKI
T. HONDA
K. MORIOKA
Y. KIKUCHI
T. HUANG
EDITORIAL COMMENT
This chapter shows how anatomic analysis can be used to make a previously difficult free flap anastomosis more reliable.
The deltopectoral skin flap described by Bakamjian (1) in 1965 is an axial flap; therefore, it can be harvested as a free skin flap for distant transfer by means of a microsurgical technique (2, 3). This skin flap was useful for facial resurfacing because of excellent color and texture match. Shortness of the vascular pedicle and smallness of the vessel caliber, on the other hand, render flap revascularization technically difficult. The method is further plagued by problems attributable to bulkiness of the skin flap and morbidities associated with donor-site deformity. These problems have been ameliorated by extending the pedicle to the internal mammary vessel and defatting the flap.
INDICATIONS
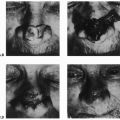
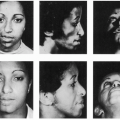
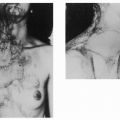
Between 1985 and 1998 at our hospital, a total of 27 patients underwent reconstruction of head and neck deformities due to various causes, using a free deltopectoral skin flap. There were 14 men and 13 women. The youngest patient was 11 years old, and the oldest was 66 years of age; the average age of this group was 36 years. Twelve patients had burn deformities of the face. A large facial hemangioma was seen in seven individuals. The flap was often used to reconstruct defects consequential to cancer extirpation. The indications and the number of patients with head and neck deformities managed with a free deltopectoral flap were as follows: burn contracture, n = 12; hemangioma, n = 7; malignant tumors, n = 4; pigmented nevus, n = 1; neurofibroma, n = 1; epidermal nevus, n = 1; and silicone granuloma, n = 1. Although the flap was sufficient to cover any defect around the face and the neck, it was never used to reconstruct the upper eyelid deformity. Resurfacing of the facial defect, however, did not follow the concept of facial aesthetic units. The distribution of the 31 recipient sites was as follows: frontal scalp forehead, n = 5; orbital area, n = 1; nose, n = 1; cheek, n = 13; mouth, n = 2; and chin/neck, n = 9. For three patients, the defect involved more than one area of the face.
ANATOMY
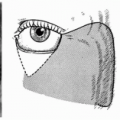
The lateral edge of the flap is bound by a line drawn 2 to 3 cm beyond the deltopectoral sulcus, alias Mohrenheim’s fossa. The boundary is especially important in individuals for whom a concomitant defatting/thinning of the skin flap is contemplated at the time of initial flap harvesting. The medial boundary of the flap is located usually at the sternal edge on the same side. The medial boundary of the flap can be expanded by 3 to 4 cm beyond the ipsilateral parasternal line, especially where a segment of the internal mammary vessel is included in fabricating a vascular pedicle.
Length and size of the vessel can vary depending on the location of the flap marked over the upper chest and the distance from the parasternal line. Diameter of the arterial pedicle can be increased from 0.9 to 2.9 mm by incorporating a segment of the internal mammary artery. Similarly, elongation of the vascular pedicle can be achieved by removing the skin and the soft tissues surrounding the vessels at the medial edge of the flap (Fig. 128.1).
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree