CHAPTER 24 Deformity
Femoral deformities pose many technical challenges for the surgeon. Deformities can make total hip arthroplasty exposure difficult, can increase the risk of femoral fracture or perforation, and can lead to implant malposition. Deformities may, in some cases, compromise implant fixation. Hip instability caused by bony impingement or implant malposition may occur in hips with femoral deformity. Finally, deformity can alter hip biomechanics, thereby causing problems with abductor power and limp.1
Proximal femoral deformities, although uncommon, are not rare in patients who require total hip arthroplasty and occur for many reasons. Proximal femoral deformity may be present as a result of developmental problems such as developmental dysplasia of the hip (DDH) or congenital coxa vara or be secondary and occur after proximal femoral osteotomy or failed total hip arthroplasty.2 In addition, deformity of the proximal femur may be the result of proximal femoral fracture malunion or nonunion, Paget disease of the femur, and femoral fibrous dysplasia.3 Berry1 has proposed an anatomic classification based on the deformity site: greater trochanter, femoral neck, metaphyseal level, and diaphyseal level. Further categorization can be established by the geometry of the deformity: angular, rotational or translational, abnormal bone size, or a combination thereof.
The surgeon faces certain technical difficulties during primary or revision total hip arthroplasty in patients with distorted proximal femoral anatomy.4 When planning hip replacement in these patients, three surgical attitudes are possible. First, if the deformity is very proximal it simply can be eliminated. Second, if the deformity is not very severe, the surgeon may be able to adapt the procedure to the altered anatomy by modifying the technique or the implant. Third, there are situations in which the deformity is so significant that the surgeon needs to correct it, either simultaneously with the arthroplasty or as a preliminary step before arthroplasty.
DEVELOPMENTAL DYSPLASIA OF THE HIP
DDH without Previous Surgery
There are two main technical problems associated with hip joint replacement in severely dysplastic or dislocated hips.5,6 The first involves the proximal femur, which typically shows anteversion exceeding 20 to 30 degrees. If cemented replacement is chosen, a small femoral component is used to reduce the anteversion to a more physiologic level. The void left in the anterior metaphyseal area then is filled with cement. However, cement fixation of the femoral component carries a significant incidence of symptomatic mechanical failure in dysplastic hips of young persons with a high level of physical activity.7 This has led most surgeons to use uncemented femoral components in these young patients.8–10 However, using an uncemented metaphyseal-filling femoral component may result in the insertion of an implant with an unacceptable degree of anteversion that could compromise joint stability; if a smaller uncemented metaphyseal-filling component is used to “counter” the increased anteversion, prosthetic fixation may be compromised. Often, distally fixed uncemented components with a modified narrower proximal geometry or modular components allow the surgeon to “cheat” the anatomy and provide reliable uncemented fixation.
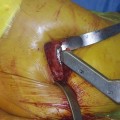
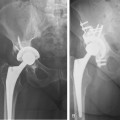
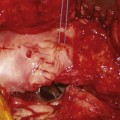
An additional problem is the position of the acetabular component, which must be seated near the anatomic center of rotation of the hip to obtain reliable fixation and to achieve the abductor strength necessary to balance the pelvis.11 Especially in hips with high dislocation, shortening procedures of the femur are valuable to bring the prosthetic head low enough for reduction.11–13 In these complex cases, a reasonable alternative is the use of a proximal femoral subtrochanteric osteotomy combined with distal advancement of the greater trochanter or segmental metaphyseal shortening osteoplasty.4,13
DDH with Previous Femoral Osteotomy
Satisfactory results have been reported in patients with DDH and a previous Schanz osteotomy treated by uncemented total hip arthroplasty with femoral shortening and advancement of the greater trochanter.13 The incidence of complications is greater than in primary total hip arthroplasties, however.
Total hip arthroplasty in combination with a subtrochanteric double chevron derotation osteotomy showed satisfactory early results in the treatment of complete congenital dislocation of the hip in adults.14 In all seven cases, an uncemented femoral component was inserted. There have been no nonunions, dislocations, or nerve palsies. The average femoral shortening was 4.5 cm (range: 3.2-7.1 cm), and the average limb lengthening was 1.2 cm (range: −0.3-1.9 cm).
The results of total hip arthroplasty for DDH with different forms of femoral osteotomy have been reported with short- to midterm follow-up. Reikeraas and associates15 reported on 25 dislocated hips that were treated with femoral shortening through a subtrochanteric transverse osteotomy with an uncemented stem. After follow-up of 3 to 7 years, one delayed union and one malunion were reported but there were no mechanical failures.
The senior author and his colleagues4 reported 14 primary hip replacements in patients with DDH, 8 of them with previous failed proximal femoral osteotomy. Shortening and correction of angular and rotational deformities were performed at the osteotomy site. Two of the four patients treated with femoral shortening required revision surgery for osteotomy nonunion and aseptic loosening of the femoral component. Overall, subtrochanteric osteotomy has provided satisfactory results in at least 80% of cases.14–16 However, malunion and nonunion occasionally occur and can be associated with fatigue failure of the stem15 or aseptic loosening.
Yasgur and associates16 reported the results of a transverse osteotomy, for subtrochanteric femoral shortening and derotation, in eight patients with Crowe type IV hips who had replacement with fully coated (six hips), modular (one hip), or cemented (two hips) stems combined with a transverse subtrochanteric osteotomy for shortening and retroversion. At a mean follow-up of 3.6 years (range: 2 to 7 years), eight patients were followed for an average of 43 months with good to excellent results in seven. Eight of nine osteotomies (89%) demonstrated radiographic evidence of healing at an average of 5 months. One hip required revision, and an asymptomatic patient developed radiographic nonunion.
Chareancholvanich and colleagues17 reported 15 hips in 11 patients with complete congenital dislocation treated by total hip arthroplasty and femoral shortening with a subtrochanteric double chevron derotation osteotomy at 5.5 years. An excellent result in 5 and a good result in 7 were recorded (80% success rate). The location of the hip center was lowered by a mean of 8.3 cm (range: 5.7-10.4 cm). Leg length discrepancy in 7 patients with unilateral involvement was reduced from a mean of 3.9 cm (range: 1.7-8.2 cm) before surgery to a mean of 1.4 cm at the latest follow-up (range: 0-4 cm). The Trendelenburg sign was corrected from a positive preoperative status to a negative postoperative status in 8 of 10 hips. The only complications were a supracondylar fracture below the femoral component and loosening of the cemented titanium-backed acetabular component 1.5 years after surgery.
Uncemented femoral fixation in conjunction with a subtrochanteric derotational osteotomy has been described in a small series of patients by Zadeh and coworkers.18 In seven patients with a mean age of 49 years, an uncemented femoral prosthesis in conjunction with subtrochanteric derotational osteotomy allowed the restoration of the normal proximal femoral anatomy, including the abductor muscle lever arm, without resorting to greater trochanteric transfer. Correction of the excessive femoral anteversion avoided the tendency for postoperative anterior instability. A computer-assisted design/computer-assisted manufacturer design included a close intramedullary proximal fit, with collar, lateral flare, and hydroxyapatite coating to achieve early proximal fixation and a longitudinally cutting fluted stem to provide immediate rotational stability across the osteotomy site. With a mean follow-up period of 31 months, all cases had a satisfactory outcome with evidence of union at the osteotomy site.
More recently, a new technique of subtrochanteric shortening with the prosthesis in situ has been described.19 The technique minimized complications, allowed correction of severe femoral neck anteversion, and gave excellent rotational stability, while preserving the proximal femur for better press-fit uncemented fixation. Significant pain relief and functional improvement were reported in nine patients, and all osteotomies appeared to be healed on radiographs by 12 weeks.
Perka and colleagues,20 in 2000, described the implantation of an uncemented straight stem in 15 patients using a simultaneous, derotating, and shortening osteotomy. Advantages included a shorter duration of surgery, a lower complication rate, and a more rapid consolidation of the osteotomy. Femur fractures, pseudarthroses, stem loosening, paresis, and deep infections were not present at 4 years.
Recently, Eskelinen and associates13 reported 68 uncemented total hip replacements in 56 consecutive patients with high congenital hip dislocation. The cup was placed at the level of the true acetabulum, and a shortening osteotomy of the proximal part of the femur and distal advancement of the greater trochanter were performed in 90% of the hips. At a mean follow-up of 12.3 years, the rate of survival for the femoral components with congenital hip dislocation, with revision because of aseptic loosening as the end point, was 98.4% at 10 years.
PREVIOUS INTERTROCHANTERIC OSTEOTOMY
Intertrochanteric femoral osteotomy can cause significant deformity in the metaphyseal area of the femur; it is logical to expect that conversion to hip replacement can be more difficult and, therefore, one should expect more perioperative complications and also an influence on the quality of the long-term results. The role of cortical defects caused by screw removal in causing prosthetic loosening is uncertain but seems to be implicated in some cases.21
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree