Cosmetic Surgery of the Face
Canice E. Crerand PhD
Thomas F. Cash PhD
Linton A. Whitaker MD
In 2004, over 9.2 million cosmetic surgical and nonsurgical procedures were performed in the United States (1). Rhinoplasty, blepharoplasty, and rhytidectomy (facelift) were among the most popular surgical procedures, as they typically are. Nonsurgical or minimally invasive procedures, such as botulinum toxin (Botox®) injections, are becoming even more popular than these surgical procedures. Of the 9.2 million cosmetic procedures performed in 2004, over 7.5 million were minimally invasive procedures (1). The popularity of these and other facial procedures is not surprising, given that the face is often an individual’s most prominent and defining physical feature (2).
As the number of individuals who seek cosmetic facial procedures increases, so does the need to understand the psychological characteristics of the patients who seek them. Plastic surgeons and mental health professionals have long been interested in this issue, even before the recent rise in popularity. Understanding the psychological characteristics of patients who desire and undergo cosmetic procedures is important for practical reasons. Cosmetic procedures are often considered “psychological interventions,” as many patients report postoperative improvements in their self-esteem and satisfaction with their appearance (3). However, these procedures may not be appropriate for all individuals, particularly those with certain psychiatric disorders. Thus, an understanding of the psychological functioning of cosmetic surgery patients is important as it relates not only to who desires these procedures but potentially to their outcome.
This chapter will review studies of the psychological characteristics of patients seeking facial cosmetic treatments. Particular attention will be paid to studies of patients seeking rhinoplasty, anti-aging treatments, and facial skeletal procedures. The chapter will also discuss the psychological characteristics of patients who seek hair replacement and/or transplantation. The relationship between two psychiatric disorders (body dysmorphic disorder and social anxiety disorder) and facial cosmetic surgery will be reviewed. The chapter concludes with suggestions for future research and implications for clinical practice.
RHINOPLASTY
Historically, rhinoplasty has been one of the most popular cosmetic procedures. In 1992, rhinoplasty was the second most commonly performed cosmetic procedure with 50,175 procedures performed in the United States (4). Its popularity has endured, as evinced by the fact that 305,475 rhinoplasties were performed in 2004, again making it the second most commonly performed cosmetic surgical procedure (1). Over the past 50 years, the psychological characteristics of rhinoplasty patients have received as much attention as any cosmetic procedure. As observed by Sarwer et al. (2,5), these studies, as well as studies of patients who have undergone other procedures, can be grouped into three generations of research.
First Generation Studies
Early reports of the psychological characteristics of rhinoplasty patients date back to 1940s and 1950s. Many of these investigations, as well as studies conducted into the 1960s, relied heavily on clinical interviews and observations of patients. The results of these studies suggested that rhinoplasty patients were highly psychopathological (6, 7). One set of investigators went so far as to state that all patients desiring rhinoplasty were mentally ill (6). They described their sample of patients as suffering from a variety of psychiatric issues, ranging from feelings of inferiority to psychosis (6). In another study, 53% of patients received preoperative diagnoses of personality disorders (8). Following surgery, 10 patients were reported to have had “significant postoperative disturbances,” such as symptoms of anxiety, depression, and psychosis.
Many early investigators conceptualized the desire for rhinoplasty from a psychodynamic perspective, the prevailing theoretical orientation in psychiatry at the time. The nose was often thought to symbolize the penis, and the desire for rhinoplasty was conceptualized as the patient’s unconscious displacement of sexual conflicts onto his or her nose (9). For adolescent females, the desire for rhinoplasty was interpreted as an attempt to remove elements of her father’s personality from her own (10). In another investigation, female rhinoplasty patients were described as over-identifying with their fathers because of an ambivalent relationship with an inadequate mother, which led to conflicts about femininity (11). Rhinoplasty was thought to provide resolution to these conflicts.
These early reports suggested that the majority of rhinoplasty patients were psychologically disturbed. In some cases, surgery exacerbated, rather than eliminated, this psychopathology. These findings, however, must be viewed in light of several methodological limitations. The reliance upon unstructured, psychodynamically oriented interviews suggests that the observations may have been biased, particularly since, from a psychodynamic perspective, appearance concerns are thought to be symptoms of underlying psychopathology. The lack of description provided for the clinical interviews prohibits replication of these findings. The majority of studies had relatively small sample sizes and failed to incorporate appropriate control groups. Finally, at the time these early reports were published, cosmetic surgery was clearly not as socially acceptable or readily available as it is today. In light of this social context, it is possible that surgery patients from this generation were, in fact, more psychopathological than the patients who seek rhinoplasty today (3).
Second Generation Studies
During the 1970s and 1980s, “second generation studies” of rhinoplasty patients began to include valid and reliable psychometric measures (2,5). Many studies incorporated control groups as well as preoperative and postoperative assessments. In contrast to previous studies, the majority found less evidence of preoperative psychopathology (12, 13, 14, 15), and several noted postoperative benefits (13, 14,16, 17).
For example, Hay (12) investigated preoperative psychological characteristics in 45 patients seeking rhinoplasty using psychiatric interviews and several personality measures, including the Eysenck Personality Inventory. Compared to a control group, rhinoplasty patients reported higher levels of hostility, neuroticism, and obsessiveness. According to the psychiatric interviews, 26 of the 45 patients were considered to be “normal” or suffering from only mild personality reactions stemming from their appearance concerns. Postoperatively, 17 patients were asked to complete some of the same psychometric measures (16). The majority reported satisfaction with their surgery as well as reductions in levels of hysteria (16).
A subsequent study that administered clinical interviews and several psychometric tests, including the General Health Questionnaire, also found increased levels
of anxiety, obsessiveness, and paranoia preoperatively compared to age- and gender-matched controls (13). Following surgery, patients reported decreases in all of these symptoms, and there were no significant differences between the rhinoplasty and control patients (13). Another study similarly reported improvements in symptoms of depression and anxiety postoperatively in 25 patients (17). Studies incorporating the use of the Minnesota Multiphasic Personality Inventory (MMPI) reported that the personality profiles of rhinoplasty patients were essentially normal preoperatively (14, 15), and no changes in personality were noted postoperatively (14). Improvements in self-concept were reported (14).
of anxiety, obsessiveness, and paranoia preoperatively compared to age- and gender-matched controls (13). Following surgery, patients reported decreases in all of these symptoms, and there were no significant differences between the rhinoplasty and control patients (13). Another study similarly reported improvements in symptoms of depression and anxiety postoperatively in 25 patients (17). Studies incorporating the use of the Minnesota Multiphasic Personality Inventory (MMPI) reported that the personality profiles of rhinoplasty patients were essentially normal preoperatively (14, 15), and no changes in personality were noted postoperatively (14). Improvements in self-concept were reported (14).
Collectively, studies from the second generation of research suggest that rhinoplasty patients exhibited less psychopathology compared to earlier studies. Furthermore, postoperative assessments largely suggested that surgery produced improvements in psychological symptoms such as depression and anxiety. Nonetheless, many of these studies suffered from methodological problems, such as small sample sizes and the lack of appropriate control groups, which limit the generalizability of their findings.
Third Generation Studies
More recent studies (e.g., 1990 to present) of rhinoplasty patients have utilized improved methodologies, including reliable and valid self-report questionnaires and clinical interviews with established diagnostic criteria. Most studies have also included preoperative and postoperative assessments and appropriate control groups.
One study assessed 72 rhinoplasty patients preoperatively and postoperatively using two self-report instruments, the Maudsley Personality Inventory (MPI) scales for Extroversion and Neuroticism and the Inventory for Personality and Anxiety Testing (IPAT) scale for Anxiety (18). Anxiety and neuroticism scores decreased postoperatively, and patients also reported increases in extraversion. In a subsequent study, 79 rhinoplasty patients were assessed preoperatively and postoperatively with the MPI and IPAT (19). Decreases in neuroticism and anxiety were found postoperatively at the 6-month and 5-year follow-up assessments. However, increases in extraversion were present at the 6-month follow-up only.
Interestingly, 34% of the sample had higher than normal scores on the MPI and IPAT preoperatively and showed symptoms of mild to moderate dysmorphophobia (more commonly referred to as body dysmorphic disorder), somatization disorders, social phobia, and personality “abnormalities” (19). For the majority of these patients, psychological symptoms were still apparent at both follow-up assessments. Overall, these results suggest that some psychological changes may be short-lived, as in the case of extraversion. Furthermore, surgery may not improve more significant psychological symptoms.
Other third generation studies suggested that rhinoplasty patients did not experience inordinate levels of psychiatric symptoms. Goin and Rees (20) administered the Brief Symptom Inventory, a measure of psychological symptoms, to a sample of 121 rhinoplasty patients. Preoperatively, patient responses fell within the normal range. Postoperatively, patients reported reductions in anxiety, depression, and obsessiveness.
Hern et al. (21) evaluated 27 rhinoplasty or septorhinoplasty patients and a group of patients seeking septoplasty using the CORE questionnaire, a standardized measure designed to assess dimensions of psychological status, including well-being, symptoms or problems, and life/social functioning. No differences between groups were reported for the well-being and symptoms/problems dimensions, although rhinoplasty patients reported more problems with life functioning. A related study found that rhinoplasty patients were no more likely to report problems with interpersonal relationships compared to septoplasty patients (22).
Another recent study investigated psychopathology among 25 patients presenting for septorhinoplasty compared to two control groups: outpatients from an otolaryngology practice seeking nonsurgical treatment and outpatients awaiting noncosmetic nasal surgery. Pre- and postoperative psychiatric interviews and standardized psychological measures (e.g., Beck Depression Inventory, Symptom Checklist-90) were administered (23). No preoperative differences were found between septorhinoplasty patients and both control groups on the psychometric tests. Psychiatric interviews suggested that patients were “psychologically normal” although a few patients had mild adjustment disorders. Postoperatively, patients reported satisfaction with their surgical results and improvements in social desirability. Half of the patients with adjustment disorders reported symptom reductions following surgery.
Rankin and Borah (24) assessed quality of life in a sample of 105 patients, 21 of whom sought rhinoplasty. Preoperatively, rhinoplasty patients reported high levels of appearance dissatisfaction on a measure of quality of life. Significant improvements in appearance satisfaction and reductions in appearance-related embarrassment were noted postoperatively.
Within this third generation of research, the psychological construct of body image has received increased attention (2,5). Although, intuitively, body image is often thought to refer to the body as a whole, facial appearance clearly influences an individual’s body image. Sarwer et al. (3) proposed a model of the relationship between body image dissatisfaction and cosmetic surgery. Briefly, the model contends that physical and psychological factors influence attitudes toward the body and, therefore, interest in changing the body through cosmetic surgery. These attitudes are thought to consist of two parts: (i) valence, or the importance of body image to an in-dividual’s self-esteem, and (ii) value, defined as the degree of body dissatisfaction (2, 3,5). These two dimensions are comparable to what Cash, in Chapter 4 of this volume, terms body image investment and body image evaluation, respectively. It is theorized that persons who derive much of their self-esteem from their appearance (high valence or investment) and who also report high levels of body image dissatisfaction (high value or negative body image evaluation) may be more likely to seek cosmetic surgery (2, 3,5).
To date, only one study has specifically examined the body image concerns of rhinoplasty patients. Preoperatively, the body image concerns of 32 female rhinoplasty patients were compared to those of 97 women who sought rhytidectomy and/or blepharoplasty (25). Patients completed two standardized self-report measures of body image: the Multidimensional Body-Self Relations Questionnaire (MBSRQ) (26, 27) and the Body Dysmorphic Disorder Examination, Self-Report (BDDE-SR) (28). Rhinoplasty patients reported greater dissatisfaction with their noses, as assessed by the BDDE-SR, compared to the degree of concern with facial appearance reported by the rhytidectomy and/or blepharoplasty patients.
Conclusions
It is difficult to reconcile the findings from the three generations of research, largely because of methodological differences. First generation studies, which relied heavily on psychodynamically oriented interviews, suggested that the majority of rhinoplasty patients were psychologically disturbed and that surgery may exacerbate psychopathology. Studies from the second generation of research incorporated standardized assessments of psychological symptoms. These studies mostly indicated that rhinoplasty patients were less psychopathological and that surgery could produce improvements in psychological symptoms.
Third generation studies, which have addressed some of the methodological weaknesses of earlier studies, found that most rhinoplasty patients are psychologically healthy individuals. The one investigation of body image in rhinoplasty patients
provides preliminary evidence that these patients experience heightened body image dissatisfaction specifically focused on their noses. While earlier generations of studies suggested that the desire for rhinoplasty was a symptom of psychopathology, this study offers a more plausible explanation, namely that patients seek rhinoplasty as a means of improving specific body image dissatisfaction (2). These results are also more consistent with the clinical experiences of most present-day cosmetic surgeons.
provides preliminary evidence that these patients experience heightened body image dissatisfaction specifically focused on their noses. While earlier generations of studies suggested that the desire for rhinoplasty was a symptom of psychopathology, this study offers a more plausible explanation, namely that patients seek rhinoplasty as a means of improving specific body image dissatisfaction (2). These results are also more consistent with the clinical experiences of most present-day cosmetic surgeons.
ANTI-AGING PROCEDURES
Rhytidectomy and Blepharoplasty
Rhytidectomy and blepharoplasty are two of the most popular cosmetic surgical procedures for those interested in restoring or maintaining a youthful appearance. In 2004, 114,279 facelifts and 233,334 blepharoplasty procedures were performed in the United States (1). Because these procedures are often performed concurrently, studies of patients who seek these anti-aging procedures will be reviewed together.
Early reports suggested that facelift patients were highly psychopathological. Patients were frequently characterized as dependent and depressed (29). For example, one study reported that nearly 70% of patients received a preoperative psychiatric diagnosis, most commonly neurotic depressive reactions or chronic personality disturbances (29). However, the majority of patients reported postoperative improvements in well-being and did not experience any postoperative “emotional disturbances” (29).
Like studies of rhinoplasty patients, studies of aging face patients that incorporated standardized self-report measures found lower rates of psychopathology. In one study, postoperative psychometric assessments revealed decreases in psychological symptoms such as depression (30). Another study assessed preoperative and postoperative quality of life and depression using standardized measures in a sample of 105 patients seeking a variety of cosmetic procedures, including rhytidectomy (24). These patients rated dissatisfaction with appearance and loss of self-confidence as the most important factors contributing to their current quality of life. Following surgery, they reported significant increases in appearance satisfaction and confidence. Overall, they did not report preoperative depression, with scores falling significantly below the population norms.
Recent studies examined the body image concerns of patients seeking anti-aging procedures. In an investigation of the preoperative body image concerns of 100 women seeking cosmetic surgery, nearly half (n = 46) sought facelift or blepharoplasty procedures (31). Patients reported higher levels of dissatisfaction for the feature for which they sought surgery, but they did not report increased dissatisfaction with overall body image (31). Postoperatively, patients reported decreases in body image dissatisfaction for the feature that was treated, but no changes in overall body image (32). Rhytidectomy and/or blepharoplasty patients have reported greater investment in appearance as well as greater satisfaction with overall body image as compared to women who sought rhinoplasty (25).
Dunofsky (33) investigated body image, narcissism, self-esteem, and anxiety among women who had facial cosmetic surgery. Women who underwent cosmetic surgery had significantly higher levels of narcissism and less body image dissatisfaction compared to a control group. No differences were found between groups on measures of self-esteem and anxiety. Because preoperative assessments were not obtained in this study, the significance of this finding is unclear.
In summary, recent studies of rhytidectomy and blepharoplasty patients indicate that these patients are not as psychopathological as earlier studies suggested. Body image studies indicate that patients seeking anti-aging procedures may place greater
emphasis on their appearance and report less dissatisfaction with their overall body image as compared to patients who seek other procedures. However, these patients may seek surgery to decrease body image dissatisfaction specifically associated with aging facial features.
emphasis on their appearance and report less dissatisfaction with their overall body image as compared to patients who seek other procedures. However, these patients may seek surgery to decrease body image dissatisfaction specifically associated with aging facial features.
Minimally Invasive Anti-aging Procedures
In 2004, over 7 million minimally invasive procedures were performed in the United States (1). These treatments have surpassed the popularity of the more traditional anti-aging surgical procedures in part because they offer subtle appearance improvements without the associated cost and risks of surgery.
Nearly 2.3 million Botox® injections were performed in the United States in 2004, making this procedure the most popular of all cosmetic treatments (1). The toxin is typically injected into areas of the face (i.e., forehead creases, crow’s feet) in order to reduce the appearance of wrinkling. It is also effective at treating excessive sweating. Other popular minimally invasive procedures include fat injections, collagen injections, chemical peels, dermabrasion, and laser resurfacing. Like Botox® injections, these procedures can improve the appearance of wrinkled, scarred, or sun-damaged skin. In 2004, the Food and Drug Administration approved a new product specifically designed to improve lipoatrophy in persons with HIV disease. In addition, new generations of customized facial implants are being used to treat this condition (34). It is quite possible that these products will also be used for cosmetic purposes in persons without HIV disease in the near future.
Despite their popularity, little is known about the psychological characteristics or body image concerns of the patients who seek these and other minimally invasive procedures. A German study of 30 patients who received Botox® injections for facial lines examined posttreatment social outcomes and attitudes toward appearance using two self-report measures (35). Nearly 50% of the sample reported greater confidence in their appearance, and over half reported increases in attractiveness (35).
Recently, a report described the phenomenon of “botulinophilia,” a term used to describe a potential subtype of body dysmorphic disorder (BDD) characterized by persistent demands for Botox® injections to treat excessive sweating (hyperhidrosis), despite any clinical evidence of a physical problem (36). Thirteen patients requesting Botox® for assumed hyperhidrosis were evaluated for BDD with a semistructured interview utilizing DSM-IV criteria. Twenty-three percent met formal diagnostic criteria for BDD (36).
Few studies have investigated the psychological characteristics of patients who sought other minimally invasive facial procedures. A recent study of 178 patients seeking laser skin resurfacing reported that 18% received prior treatment for depression (37). Another study evaluated the psychosocial benefits associated with alpha hydroxy acid, a topical treatment that is used to reduce roughness and fine wrinkling. Patients noted significant improvements in appearance and relationship satisfaction following treatment (38). Given their popularity, studies of the psychological concerns of patients who seek these treatments are needed.
OTHER FACIAL PROCEDURES
Facial Skeletal Procedures
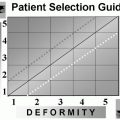
Requests for “atypical” facial cosmetic procedures have also been reported in the literature. These procedures involved bone contouring, bone grafting, or the insertion of cheek, chin, or other facial implants. Edgerton, Langmann, and Pruzinsky (39) described 15 patients who sought extensive symmetrical facial skeletal recontouring procedures in order to address discontent with facial width. These “facial width
deformity” patients reported concerns with minor, largely unnoticeable anatomic deviations, such as their heads being too wide or too thin.
deformity” patients reported concerns with minor, largely unnoticeable anatomic deviations, such as their heads being too wide or too thin.
Preoperative psychiatric interviews revealed that the majority of these patients experienced significant impairment in psychosocial functioning. Only three patients received a formal psychiatric diagnosis. However, the clinical descriptions of these patients suggest that some may have been suffering from BDD. Postoperatively, patients reported improvements in body image and psychosocial functioning although psychometric measures were not utilized to assess these changes (39).
While requests for facial skeletal cosmetic procedures may be atypical, more patients are requesting procedures such as cheek and chin implants in order to change the structural appearance of their faces. In 2004, over 25,000 chin or cheek implantation procedures were performed (1). Comparatively, only 1,741 cheek implant and 4,115 chin augmentation procedures were performed in 1992 (4). The increase in popularity of these procedures underscores the need for more research regarding the psychological characteristics and body image concerns of patients who seek these procedures.
Acne Treatment
Patients with facial skin conditions have had a long-standing interest in improving their appearance. Many complain of active acne or acne-related scarring. This is not surprising, considering that acne affects at least 80% of adolescents (40). The prevalence of acne typically decreases with age; however, it may persist through adulthood, affecting at least 8% of adults aged 25 years to 34 years, and 3% of adults aged 35 years to 44 years (41).
In the past, the psychosocial effects of acne were often dismissed, largely because acne has long been considered a non-life-threatening, age-related, cosmetic condition (42). However, more health professionals now recognize the impact acne may have on the psychological and social well-being of its sufferers. Studies suggest that 30% to 50% of adolescents experience psychological difficulties associated with acne, including body image concerns, embarrassment, social impairment, anxiety, frustration, anger, depression, and poor self-esteem (43). Several studies evaluated the psychological characteristics of patients seeking treatment for acne. These studies indicate that depression, social anxiety, low self-esteem, and body image dissatisfaction commonly occur among these patients (42,44, 45, 46). Suicidal ideation and suicide attempts also have been documented (45,47).
Patients presenting with facial acne appear to be particularly vulnerable to the psychological effects of the disease. Compared to patients with truncal acne, facial acne patients reported lower self-esteem and greater body image dissatisfaction (46). At least one study (48) has pointed to a focused dissatisfaction with facial appearance (rather than overall appearance dissatisfaction), the magnitude of which is related to self-perceived (not objective) severity of the acne and, in turn, to the experience of social inhibition and distress. This is consistent with studies of cosmetic surgery patients, which have typically found increased dissatisfaction with the specific feature considered for surgery, rather than the more global body image (2,5).
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree