Conjoined twins have long been of interest to the medical community. Evaluation is complex and tailored to the unique variant. A thorough multidisciplinary work-up, including surgical specialties, nursing, anesthesia, and critical care, must be performed prior to proceeding with surgical separation. Outcomes have become more predictable with certain advances such as tissue expansion and three-dimensional modeling. A number of important lessons learned from previous cases can be used to improve future outcomes.
Key points
- •
Conjoined twinning is a rare phenomenon.
- •
Once a decision has been made to proceed with separation, a thorough work-up involving a multidisciplinary team, advanced imaging, and three-dimensional modeling is essential.
- •
Each case must be approached individually, while still adhering to basic plastic surgery principles.
- •
Outcomes have improved in recent years due to improvements in technology, a better understanding of conjoined twin physiology, and surgical experience.
Introduction
Conjoined twins are characterized as the union of 2 identical twins who share at least one organ system. The estimated incidence of this phenomenon is 1.3 to 2 per 100,000, with approximately half being stillborn or dying shortly after birth. Therefore, the true incidence approaches 1 in 200,000 live births.
Embryology
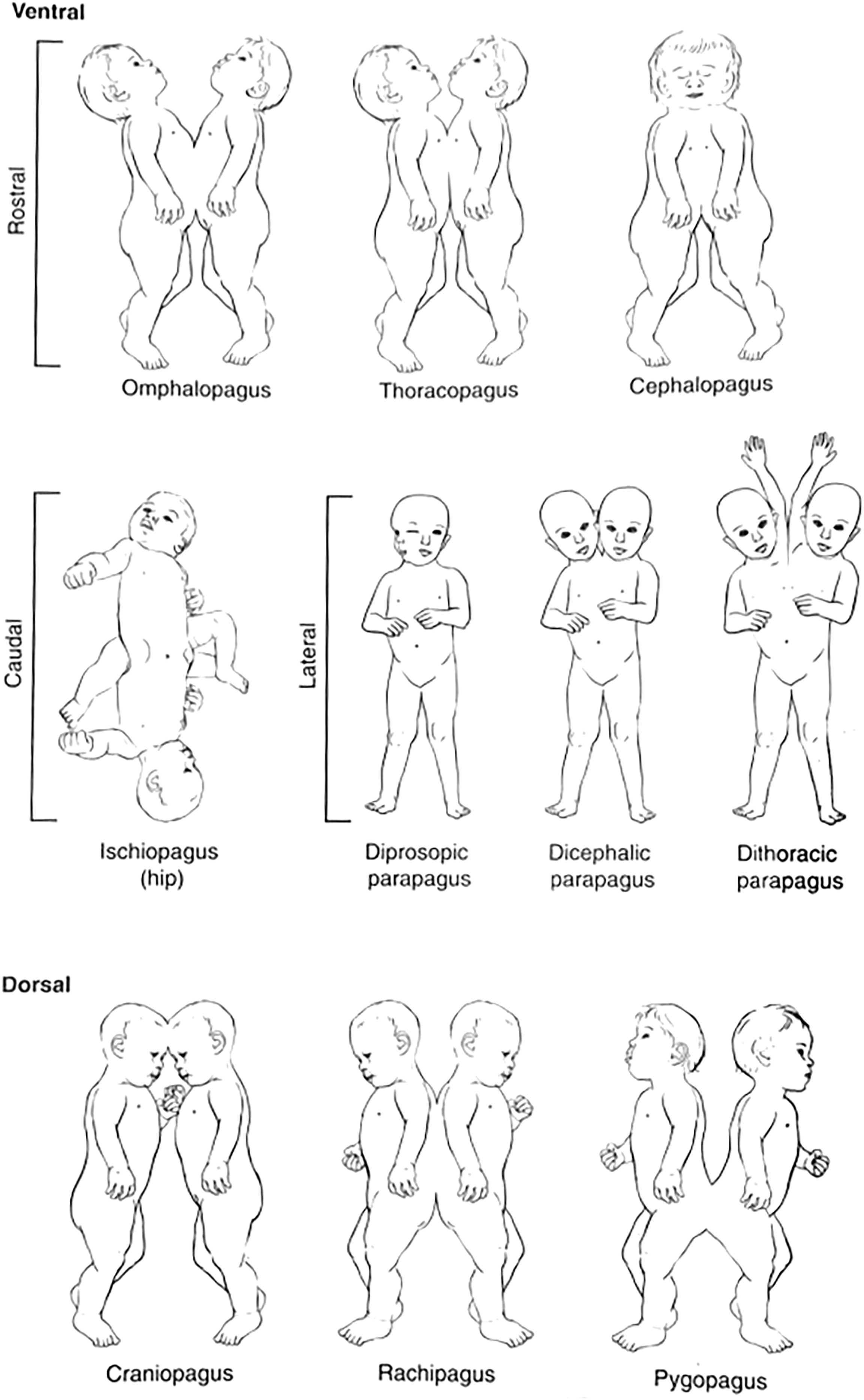
The earliest theories of conjoined twinning date back to Greek and Roman times, in which Hippocrates and Aristotle believed that a confluence of external factors, such as the quantity of semen (or “seed”), were responsible for the observed phenomena. , Hippocrates, as reported by Ambroise Pare, believed that “too great a quantity of seed” was responsible for conjoined twinning, whereas Aristotle theorized that a small womb constrained the “seed,” causing fusion of the twins. , However, 2 modern theories have been put forward: fission and fusion. The fission theory proposes that incomplete division of a fertilized ovum (or “partially separated zygote”) results in conjoined twinning. However, this has been largely refuted by the more plausible theory of fusion, put forth by Spencer. , Fusion postulates that conjoined twinning is the result of the secondary union of 2 originally separate embryonic disks. , In her analysis of more than 1200 cases, Spencer noted that the conjoined twins could be divided into 2 uninterrupted series, encompassing 8 patterns of fusion: those united ventrally and those united dorsally ( Fig. 1 ). A number of important conclusions were drawn from this analysis to lend support for the fusion theory, summarized in Table 1
| Conclusion | Explanation |
|---|---|
| 1 | Fusion occurred only at specific sites whereby ectoderm was absent or destined to become disrupted |
| 2 | Certain embryologic sites that were initially inaccessible later became available for fusion |
| 3 | Twins united dorsally always had a duplicated abdomen and umbilicus, whereas those united ventrally typically shared one abdomen and one umbilicus |
Classification
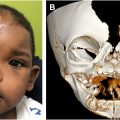
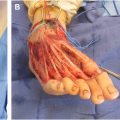
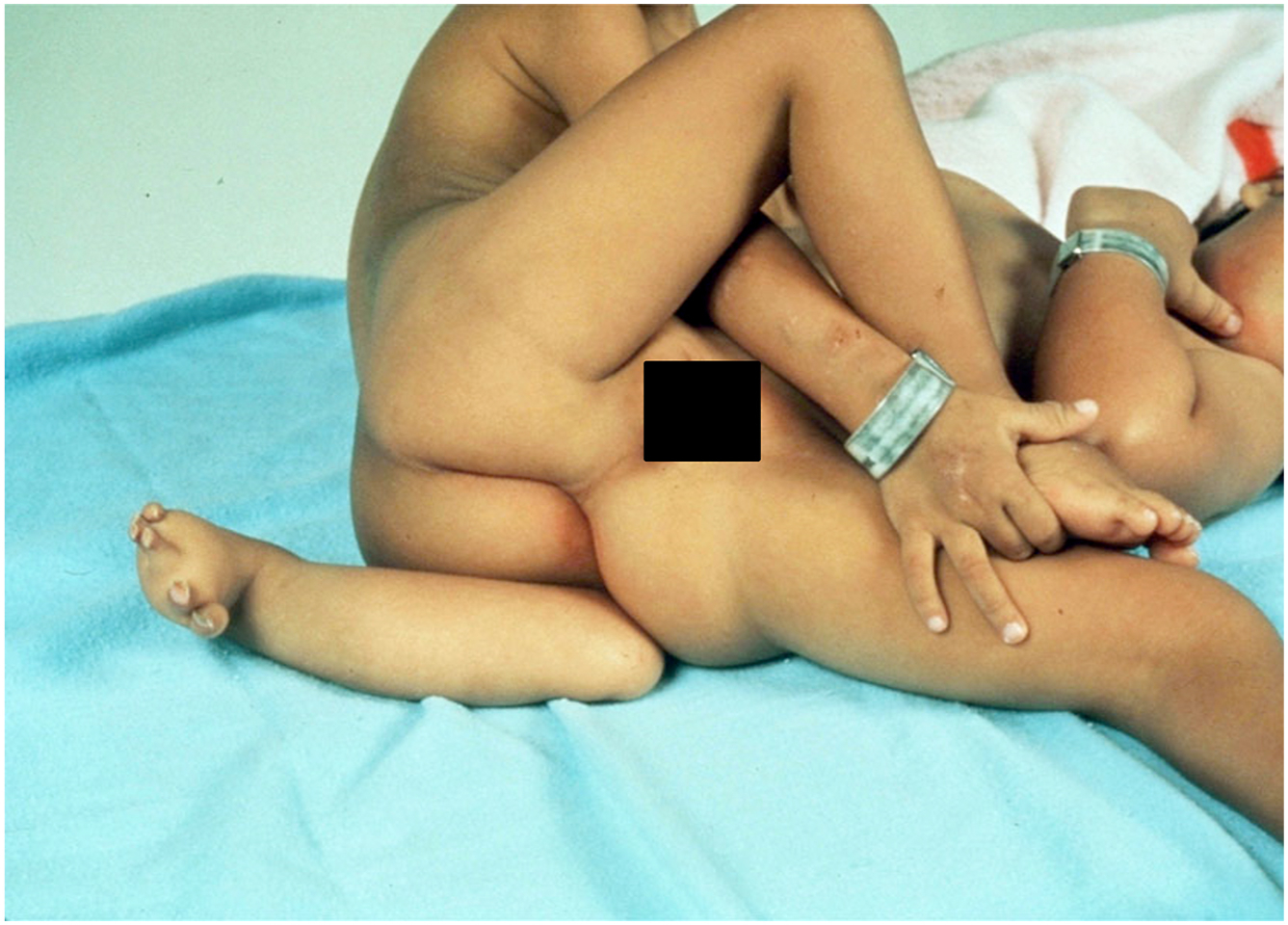
Conjoined twins are typically classified according to their most prominent site of attachment, followed by the suffix pagus , which is the Greek term for fixed or joined. There are 8 types of twins, as described by Spencer, and they are outlined as follows: omphalopagus (umbilicus), thoracopagus (chest), cephalopagus (head), ischiopagus (hip), craniopagus (helmet), rachipagus (spine), pygopagus (rump), parapagus (side). In addition, the number of united structures can be further described with the prefixes di-, tri-, and tetra-, together with the involved part , , ; – prospus (face), -brachius (arm), and -pus (leg), for example, ischiopagus tripus tetrabrachii ( Fig. 2 ).
Historical perspectives
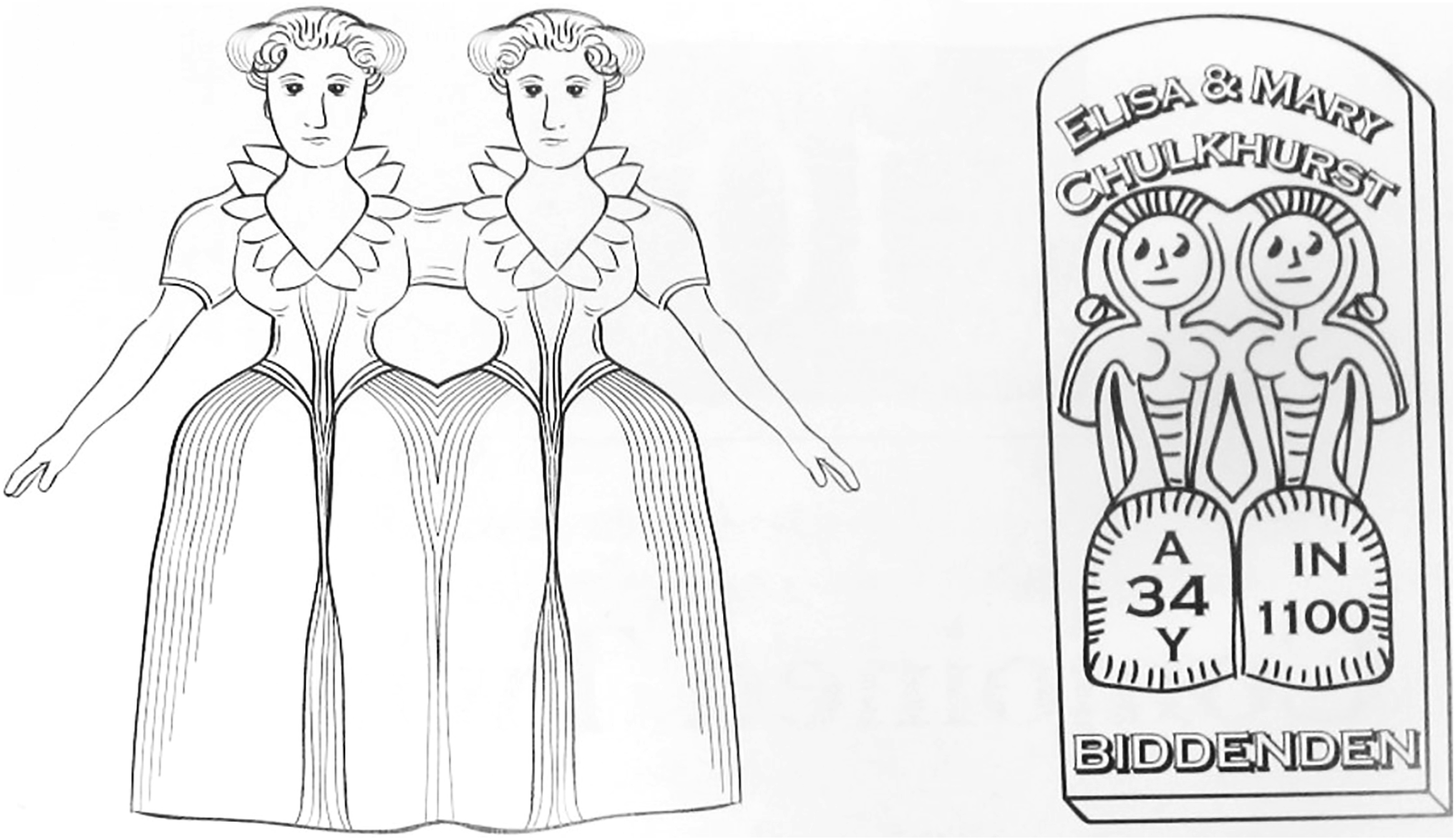
The earliest depictions of conjoined twins date back to the 6th century BC, which is a marble statue in the Anatolian civilization museum in Ankara portraying parapagus twins, or the “double goddess,” known as the sisters of Catalhoyuk. Similar clay sculptures dating back approximately 3000 years have also been found in the ancient Mexican village of Tlatilco, depicting diprosopus and dicephalic twins, and are notable for their accurate biologic and developmental proportions. , The first well-documented case of conjoined twins is the Biddenden Maids, Mary, and Eliza Chulkhurst, who were born in England in 1100. Although often depicted as being joined at the hips and the shoulders, they were likely pygopagus twins and joined at the buttocks ( Fig. 3 ). At the age of 34, Mary became ill and died. When surgical separation was proposed, Eliza famously refused, stating, “As we came together we will also go together,” and subsequently died 6 hours later.
Chang and Eng, a set of omphalopagus twins born in 1811 in Siam, modern-day Thailand, are perhaps the most widely recognized conjoined twins. They were discovered by a merchant named Robert Hunter, who brought them to Americn in 1829. They subsequently joined P.T. Barnum’s circus and were exhibited around the world as “Siamese Twins.” They adopted the surname Bunker after moving to North Carolina and ultimately took up farming, a trade in which they were quite successful. They expressed a strong desire for separation, although they were denied by a number of physicians who deemed it unfeasible. They died at the age of 63, after succumbing to heart failure ( Fig. 4 ). , , ,
The first successful attempt at conjoined twin separation was made by Johannes Fatio in 1689 in Basel Switzerland. Omphalopagus twins, Elizabeth and Catherine Mayerin, were separated using the serial tightening of a suture ligation of the bridging umbilical vessels. , However, Koenig is often credited with the procedure, as he later published the results. , The separation of Carol Anne and Catherine Anne Mouton in 1953 is considered the first successful procedure in modern times.
Clinical evaluation and surgical separation
Given the enormous variation in clinical presentation, as well as the associated complexity of separation procedures, a number of important ethical principles arise in the evaluation of this entity. These have been outlined by Spitz and others. , , , As stated by Thomas and colleagues, decision-making regarding separation must take into account the family’s values and goals, the expected short-term and long-term prognoses for each infant, as well as the benefits and burdens of separation. Palliative care is generally recommended for those patients not expected to survive beyond 6 months. In the event of complex cardiac fusion without any possibility for the reconstruction of a functional heart, no separation is offered. Similarly, surgery would not be offered if the degree of morbidity that would result is unacceptable to the parents.
Emergency separation encompasses another cohort of patients. Separation on an emergent basis is offered when the survival of one twin is threatened by the other twin who is dead or dying. However, one twin must not be sacrificed to save the other. Shared organs and tissues, as well as tissues belonging to the deceased twin, are generally considered available to use for the benefit of the surviving twin. Additionally, emergent separation is justified by the presence of a congenital anomaly that is not compatible with life if left unrepaired. Finally, serious damage to the fused area, such as a ruptured omphalocele, may necessitate emergent intervention.
In stable infants, planned separation is carried out once they have been medically optimized and all necessary work-up and investigations have been performed. This also provides additional time for complex multidisciplinary discussion and planning meetings. However, surgical separation is not permitted if both twins remain alive conjoined, but one or both twins are expected to pass from the separation procedure.
Principles for separation
Once a decision has been made to move forward with a separation procedure, a number of general principles apply, together with unique considerations for each variant of conjoined twins. In general, all relevant stakeholders must be involved early in the planning period with regular multidisciplinary meetings. A comprehensive surgical and peri-operative management plan should include the various surgical subspecialties, ethicists, neonatologists, anesthesia, the intensive care unit, and nursing. In addition, the relevant surgical anatomy must be delineated in great detail. Simulation and rehearsals are advocated in the preoperative phase, and it is important to identify the critical steps in the procedure as well as contingency plans. In a similar vein, the team should dedicate time to anticipating and planning the reconstructive needs during the preoperative period.
Unique considerations for each variant
In accordance with the aforementioned classification of conjoined twins, a number of individualized anatomic factors are present for each variant. Thoracopagus twins are the most common, with cardiac involvement present in up to 90% of cases. A large proportion of these anomalies are considered inseparable, with the exception being a tubular atrial connection or mild ventricular myocardial fusion. Extensive cardiac imaging is recommended preoperatively, including echocardiography and cardiac MRI, as subtle anatomic differences can determine suitability for separation. Cardiopulmonary bypass is needed on standby if separation is undertaken.
In omphalopagus twins, morbidity is often dictated by the extent of intestinal and hepatic fusion. It is of critical importance to delineate the biliary drainage and hepatic vascular patterns. Preoperatively, the team must also determine whether an adequate liver mass will be present for each twin postseparation, as well as the adequacy of vascular drainage. Postnatal imaging with contrast can define this anatomy.
Parapagus twins are joined for portions of the spine and pelvis. Given the interconnections of dorsal structures, a challenge exists to perform separation without neurologic morbidity. Genitourinary and gastrointestinal anomalies are also prevalent. These anomalies, together with spinal cord fusion, pelvic/sacral anatomy, and a plan for intestinal reconstruction must all be defined preoperatively.
Ischiopagus twins often have anomalous genitourinary, pelvic, and intestinal anatomy. Extensive work-up often includes fluoroscopy and endoscopy and will help to guide the separation of intestinal and genitourinary structures. A plan must also be made for abdominal wall and pelvic floor reconstruction, as significant defects can result from the separation procedure.
Pygopagus twins frequently demonstrate vertebral or sacral anomalies, genitourinary abnormalities, and a shared anus. Rectal incontinence may be experienced postoperatively. Dedicated imaging is necessary for the urologic abnormalities, as this will dictate the reconstructive plan.
Craniopagus twins are the rarest type, and the arterial inflow is usually separate despite the venous drainage possibly shared between twins. These vascular inflow patterns are critical to delineate in the preoperative phase. , Brain parenchyma may also be shared, and the extent of union may be a large predictor of morbidity following separation.
Rachipagus twins require neurosurgical involvement given the fusion of vertebral and neural structures. Plastic surgeons are often required for issues of soft tissue coverage. Cephalopagus twins are rarely viable.
Planning for separation
As the understanding of conjoined twin physiology has evolved over time, coupled with technological advances in medicine, the outcomes of conjoined twin separation have dramatically improved since the 1950s. , Other factors that account for improvement in surgical outcomes include advances in anesthetic and surgical techniques that emphasize the minimization of blood loss, intensive care monitoring, and the accumulation of surgical expertise.
Prior to surgical separation, which may occur as early as 3 to 4 months of age, a number of important factors must be addressed. As outlined in numerous reports, nutritional optimization prior to surgery is of paramount importance, and in some cases necessitates close monitoring in an intensive care unit. , Preoperative imaging is essential to characterize the shared anatomy and any associated malformations, which will determine suitability for separation. If separation is feasible, this imaging becomes paramount in the creation of a surgical plan. , Prenatal imaging, such as fetal MRI, provides valuable information for familial counseling, delivery planning, and management immediately following delivery. Postnatally, however, computed tomography (CT) and magnetic resonance imaging (MRI) are cornerstones in the work-up of occult anatomic variants and improvements in multidisciplinary planning. , Advances in these imaging modalities have allowed for less invasive means of evaluation. However, the site of the union will dictate when more invasive modalities, such as endoscopy and genitourinary studies, are indicated.
During the planning stages, three-dimensional modeling has become the standard of care for the management of these patients. This includes both 3-D reconstructions of cross-sectional imaging as well as surgical simulation. , Numerous groups have reported on the added utility of such modeling, as they are able to more reliably inform tissue expander size and location, flap design, size of anticipated soft tissue defects, the plane of separation, and formulate the final operative plan. , For example, Trost and colleagues were able to use advanced modeling software in their successful separation of very complex thoraco-omphaloischiopagus twins. The modeling allowed for the accurate estimation of the postseparation defects. Custom tissue expanders were fabricated to meet this need. In their case of craniopagus twins, Heuer and colleagues used advanced modeling to devise a novel separation strategy using the sequential distraction and constriction of the bridging tissue prior to definitive separation. Underscoring these advances in preoperative imaging and three-dimensional modeling is the importance of a multidisciplinary team for the planning and execution of successful surgical separation, as mentioned above.
Anesthetic management will involve 2 completely separate teams, with color-coded lines for each twin. Full arterial and cardiac monitoring is essential. Adequate venous access will need to be established given the potential for large-volume hemorrhage and circulatory compromise. Drugs are typically administered using the total calculated weight of both twins combined.
Postoperatively, the twins should be managed in the intensive care unit, given the significant fluid shifts and potential cardiac/circulatory compromise that may occur following separation. Judicious replacement of fluid losses and medical optimization of cardiac function may be necessary.
Case examples
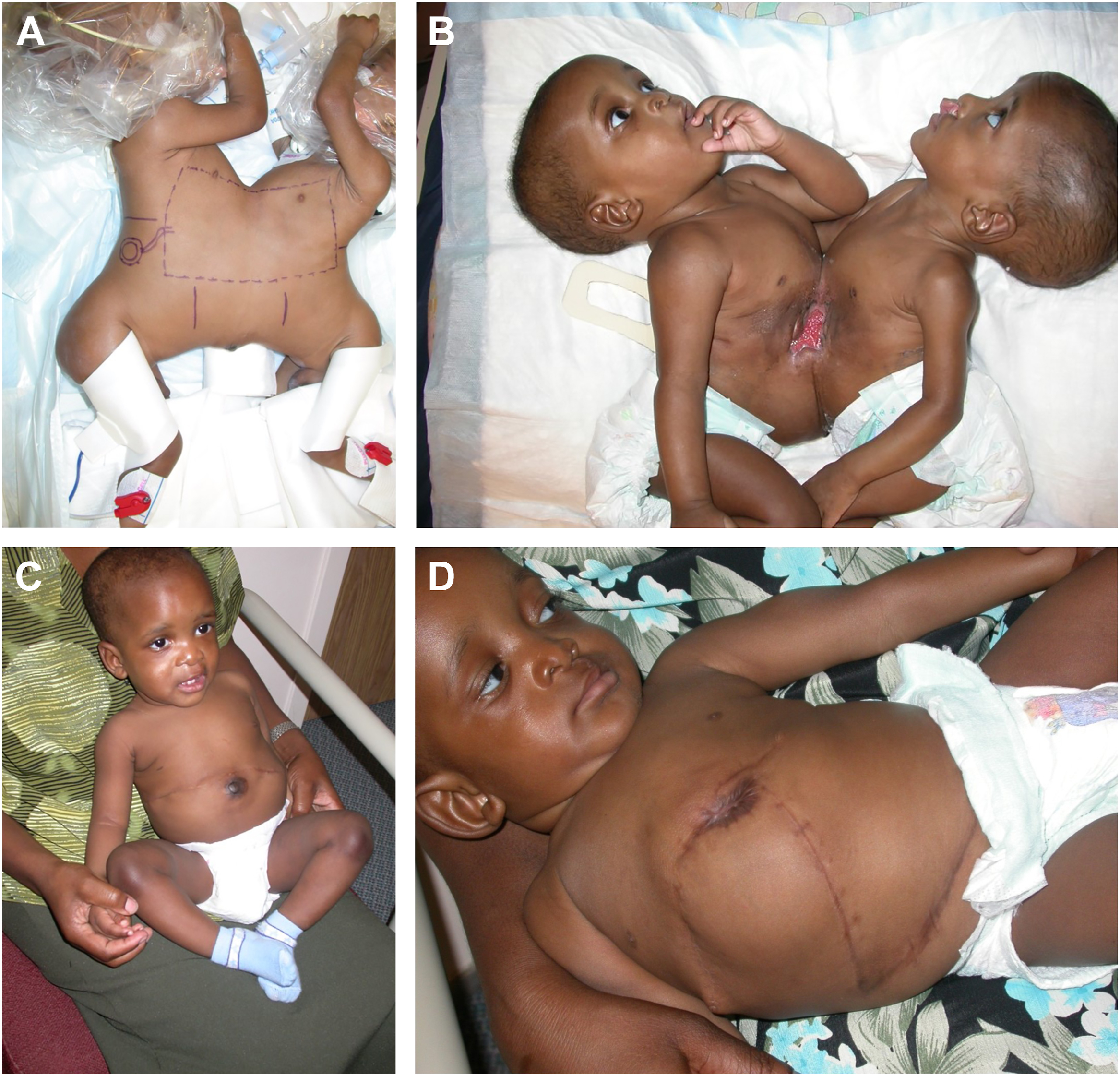
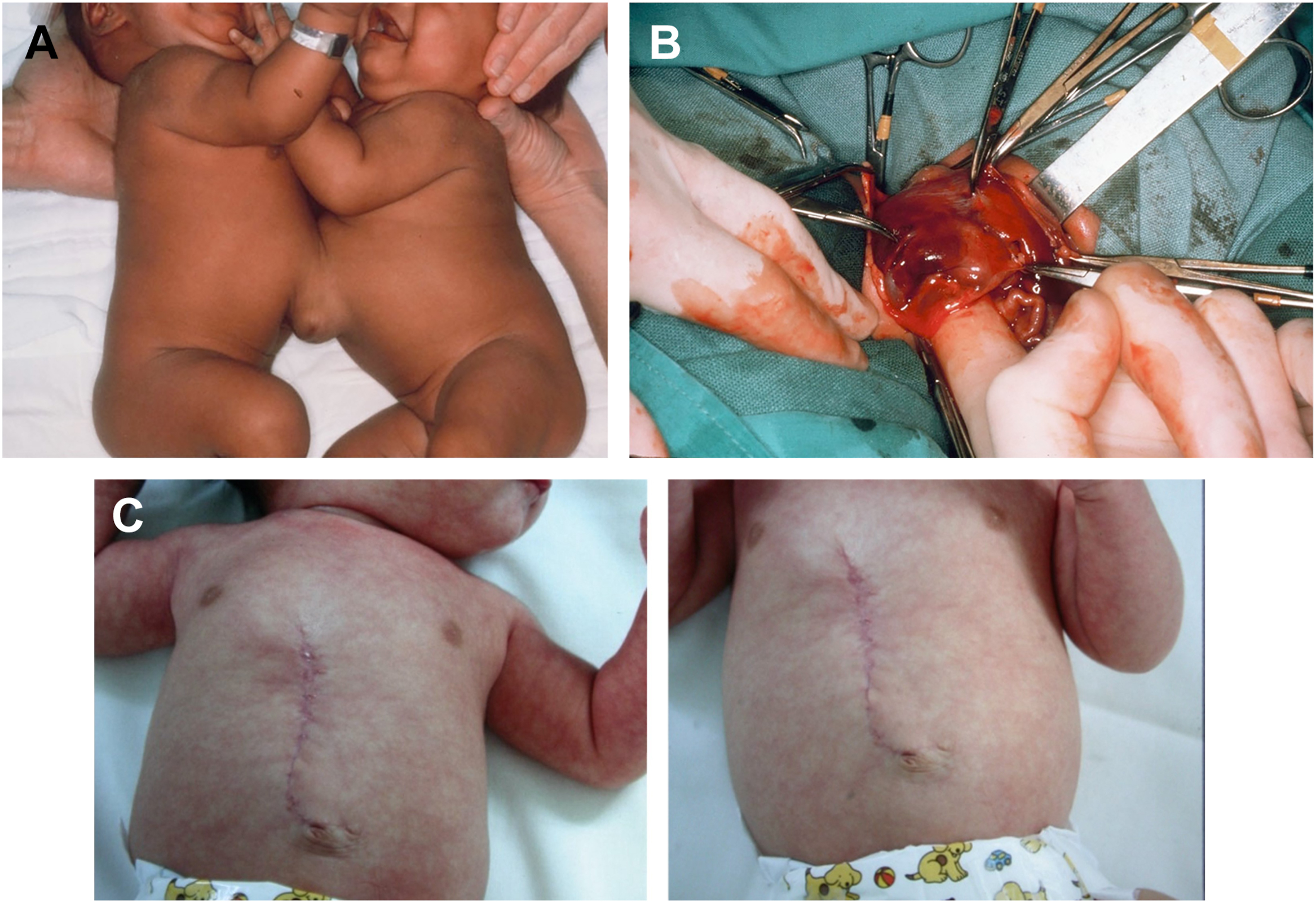
Case 1: Prenatally diagnosed omphalopagus male twins demonstrated independent anatomy apart from hepatic interconnections ( Fig. 5 A). Urgent separation was performed on the eighth day of life due to renal failure in Twin B. A midline incision was made across the site of abdominal union, followed by division of the liver ( Fig. 5 B). Fascial and skin closure was easily achieved in each twin and primary umbilicoplasties were also performed ( Fig. 5 C, D). Both twins were in good health at 6 years following surgery.