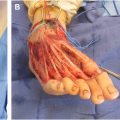
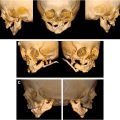
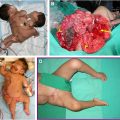
Congenital hand differences and brachial plexus birth palsy is a broad and extensive topic. Each of these conditions discussed in this article can vary in severity. The goal of treatment of these conditions is to optimize function of the limb. This review is meant to serve as an introduction to these complex conditions and their treatment.
Key points
- •
Congenital hand differences include a wide range of diverse conditions with highly variable impact on a child’s function and quality of life. Congenital hand differences reviewed include syndactyly, polydactyly, thumb hypoplasia, macrodactyly, aphalangia, symbrachydactyly, constriction ring sequence, central deficiency, cleft hand, clinodactyly, and camptodactyly.
- •
Treatment of congenital hand differences, especially surgical intervention when undertaken, is focused on improving function. Cosmesis is a secondary and subordinate aim.
- •
Pediatric brachial plexus birth palsies and traumatic brachial plexus injuries are uncommon and are best managed by an experienced multidisciplinary team; therefore, emphasis should be on early detection and referral to a comprehensive care center to maximize patient outcomes.
Introduction/history/definitions/background
Congenital hand and upper limb differences are quite common, with an estimated incidence of 1 per 626 live births. However, as many congenital upper limb differences are so mild that clinical evaluation is never sought, the incidence is likely even higher. , A thorough understanding of hand development and embryology is important in the diagnosis and treatment of congenital hand differences, but is out of the scope of this review. When considering congenital hand differences, the physician must recognize the delicate balance of treating and supporting both the child and their family. The primary objective of treatment should always be to maximize function. However, the surgeon must also be attentive to concerns about appearance and the social perception of hand differences. This review is by no means exhaustive of all the congenital hand entities a surgeon may face, and the information in this review is meant as a general overview to help guide clinicians in their understanding and the treatment of congenital hand differences.
Discussion
Congenital hand differences
Syndactyly
Syndactyly is one of the most common congenital hand differences, with an estimated incidence between 1:2,000 and 1:10,000 characterized by connections between digits, frequently the result of an inherited autosomal dominant mutation with incomplete penetrance and variable expresivity. , However, sporadic cases are also quite common. Syndactyly occurs as the result of failure of the physiologic apoptosis of the interdigital mesenchyme in utero. It is bilateral in about half of cases, affects males 2 times as often as females, and is most common between the long finger and the ring finger. , The distribution of affected digits is different in syndromic cases, as the first, second, and fourth web space are more likely to be affected in these patients.
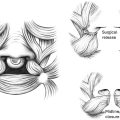
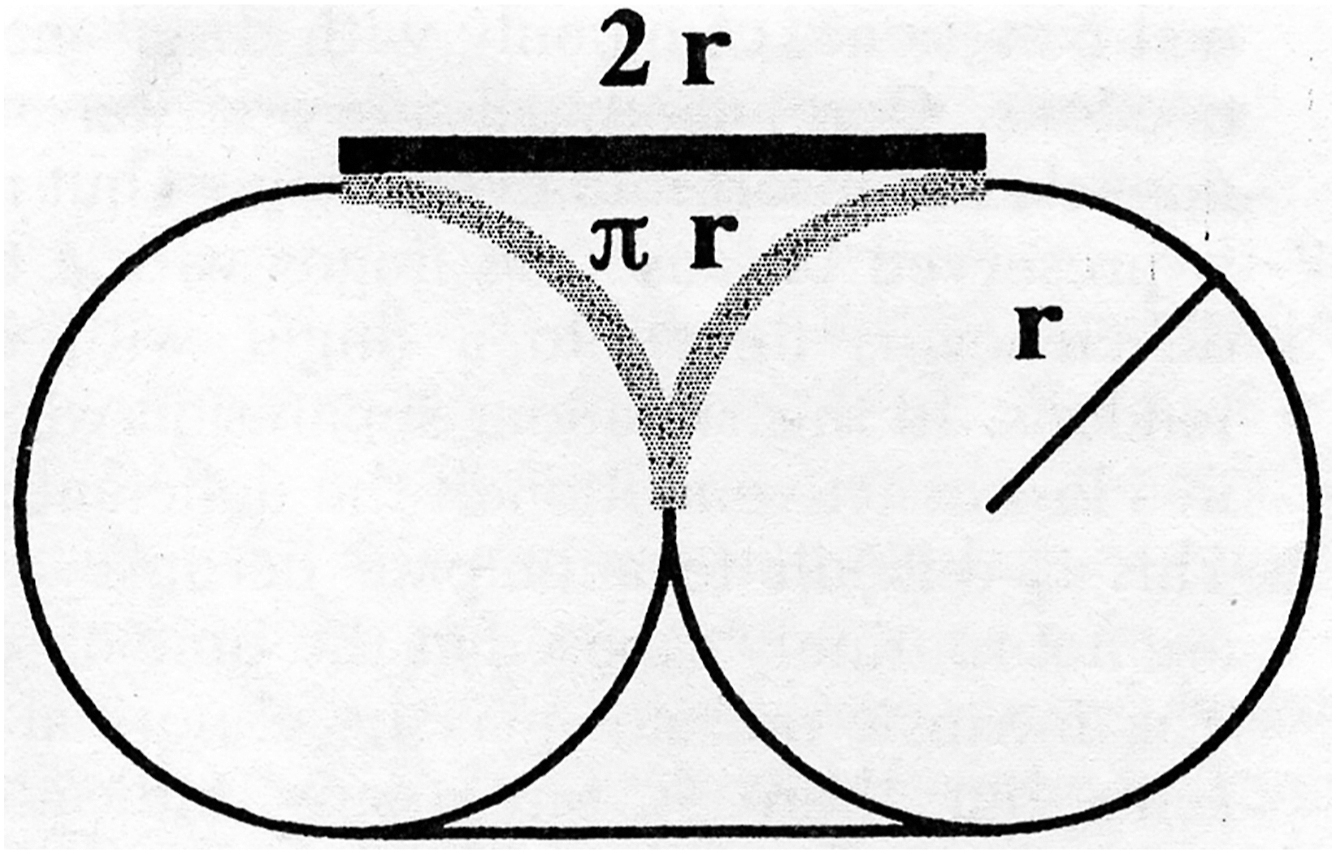
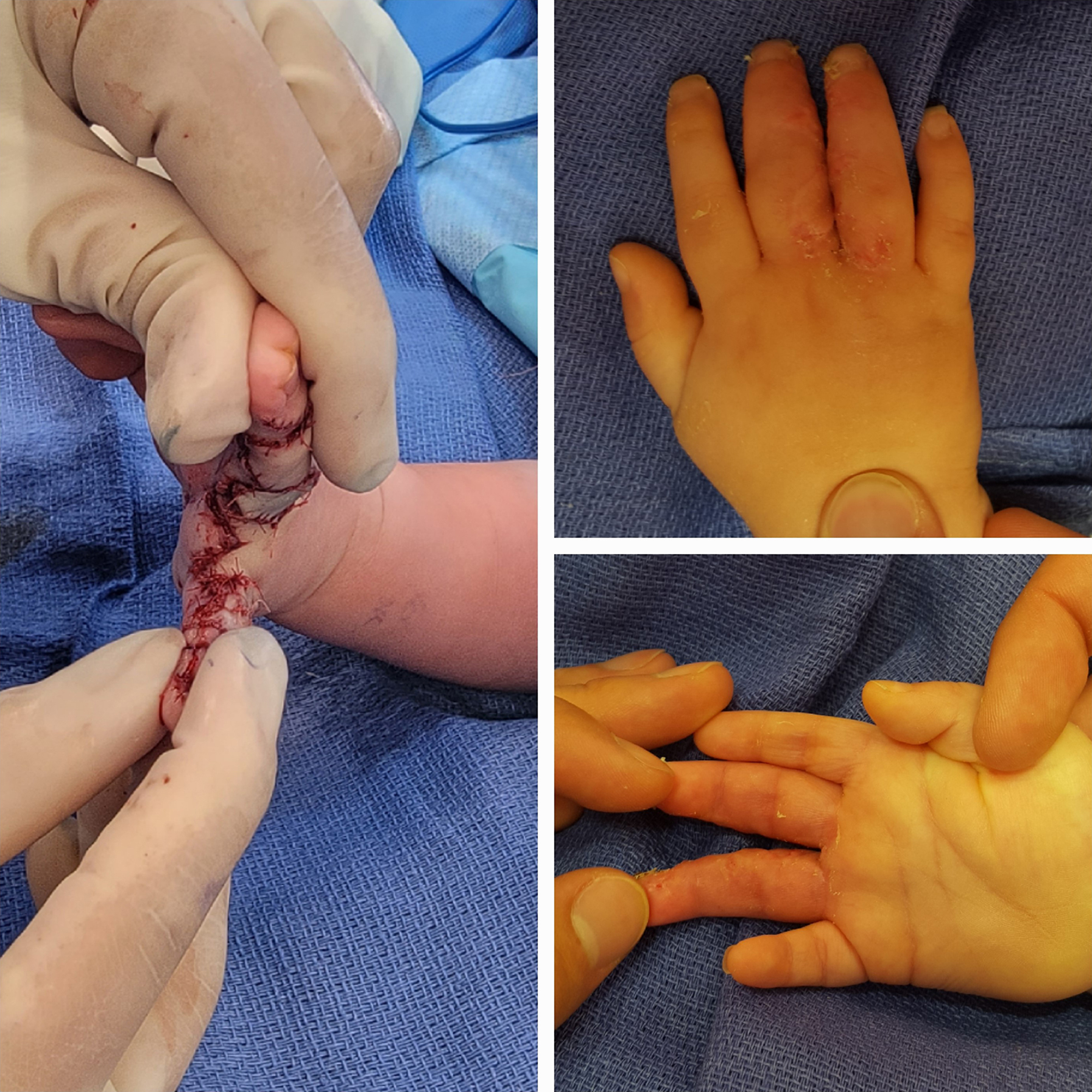
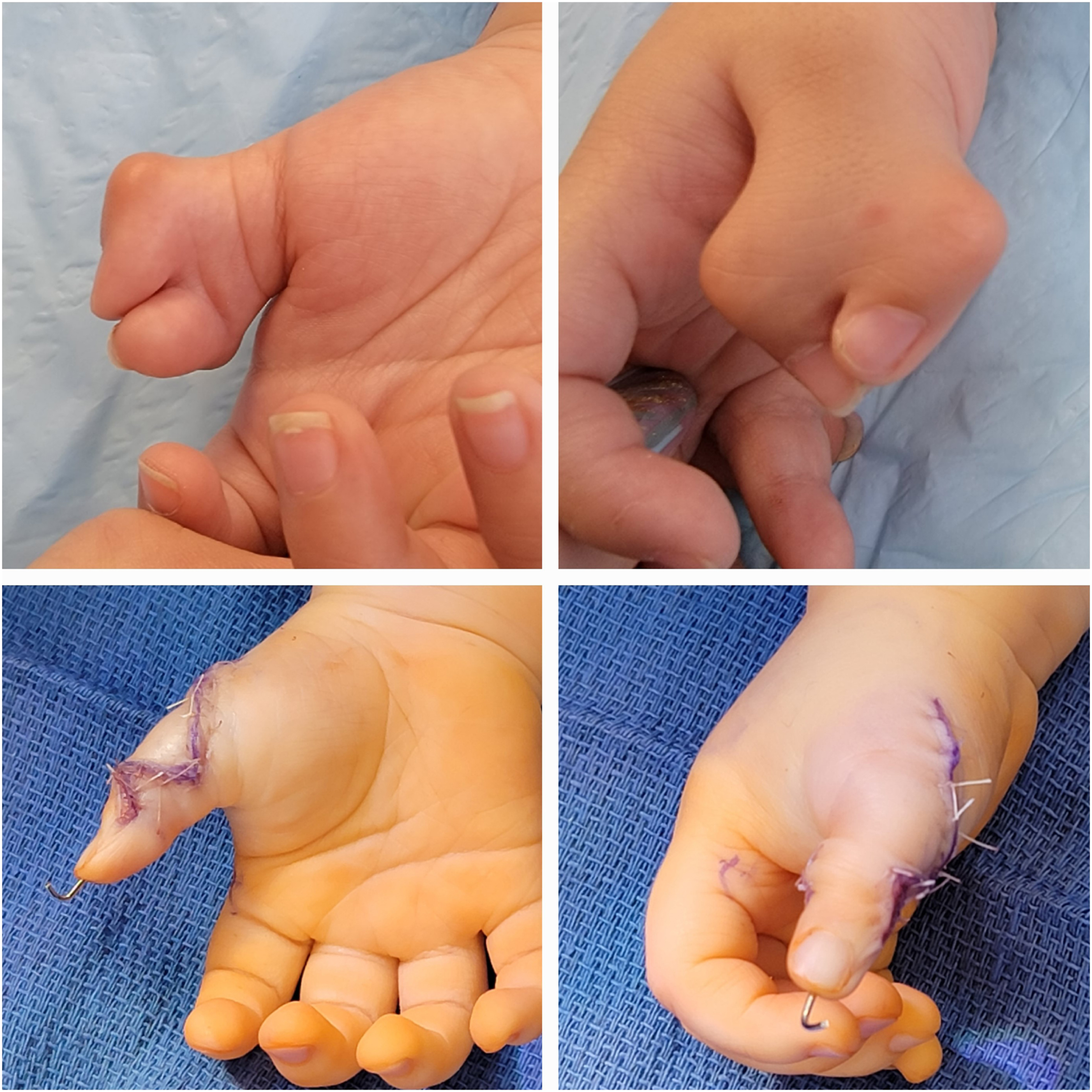
Syndactyly is a clinical diagnosis, classified as complete when the skin web involves the entire length of the affected digits and is otherwise considered incomplete ( Fig. 1 ). Radiographs allow for further characterization as simple when webs involve soft tissue only, as complex when there are osteochondral fusions of adjacent phalanges, and as complicated when there are interposed accessory phalanges. It is important to note that there is an approximately 30% deficiency of skin in syndactyly as seen in Fig. 2 , which depicts the difference in skin between digits with and without syndactyly. Treatment is typically surgical release of the syndactyly—with the use of a local flap to reconstruct the digital commissure, and with or without skin grafting, depending upon the amount of local skin available for closure. The timing of surgical care varies according to the affected digits, any underlying syndromes, and the specific type of syndactyly. Cases involving the first or fourth webspace should be followed closely for the development of clinodactyly. These webs are typically addressed between 3 and 9 months of age to prevent tethering, clinodactyly, and flexion contracture of the longer digit due to differential growth. , Syndactyly of the second or third web space can be successfully separated between 18 and 24 months, though some suggest that complex cases may also benefit from earlier release. , Full-thickness skin grafts may be employed for skin coverage, especially at the proximal aspect of the affected digits. Alternatively, dorsal metacarpal artery flaps can be employed to attempt graftless closure of the commissure. , Digital defatting and limited flap closure can also be utilized to facilitate low-tension closure without employing grafts . , ,
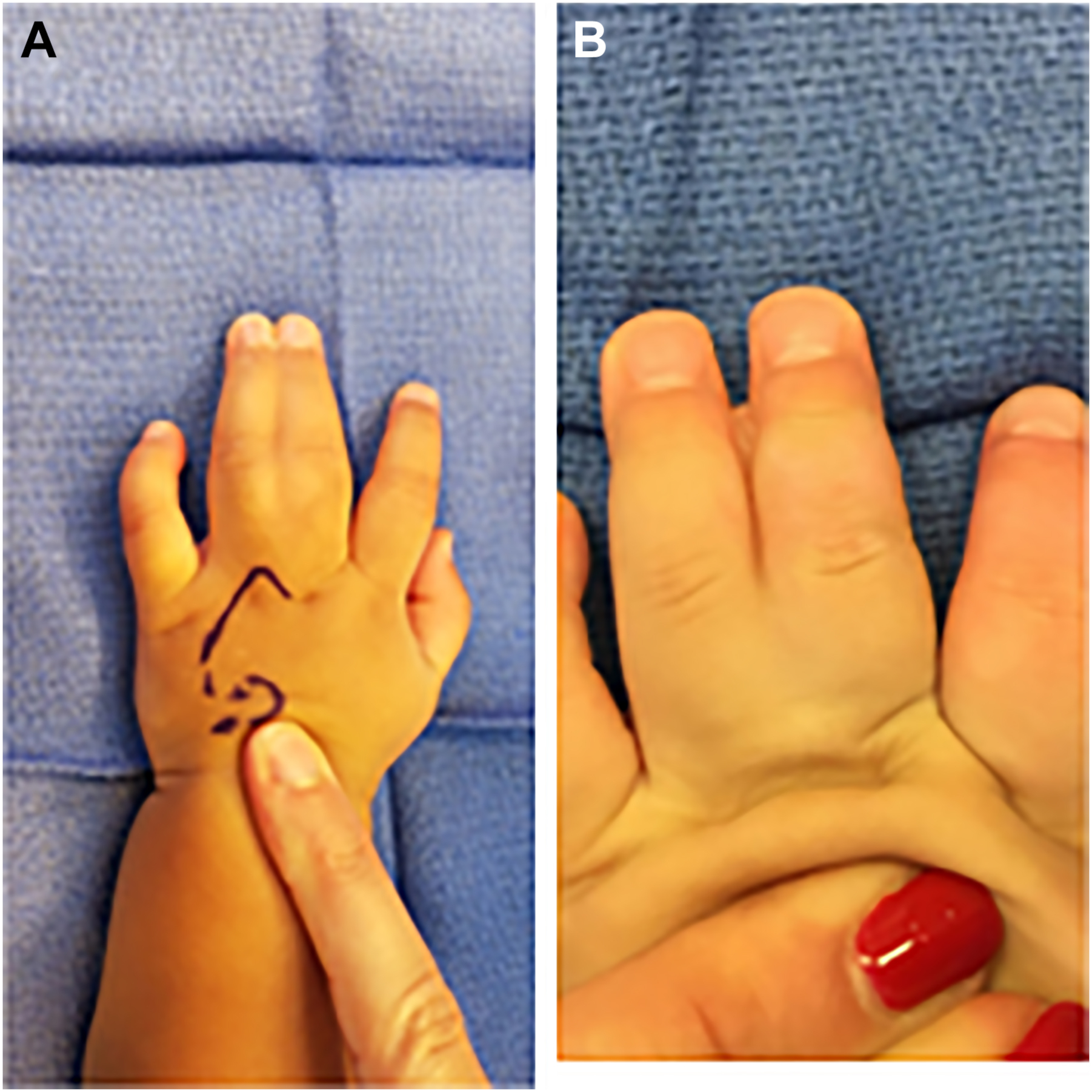
Syndactyly clinical care pearls
- •
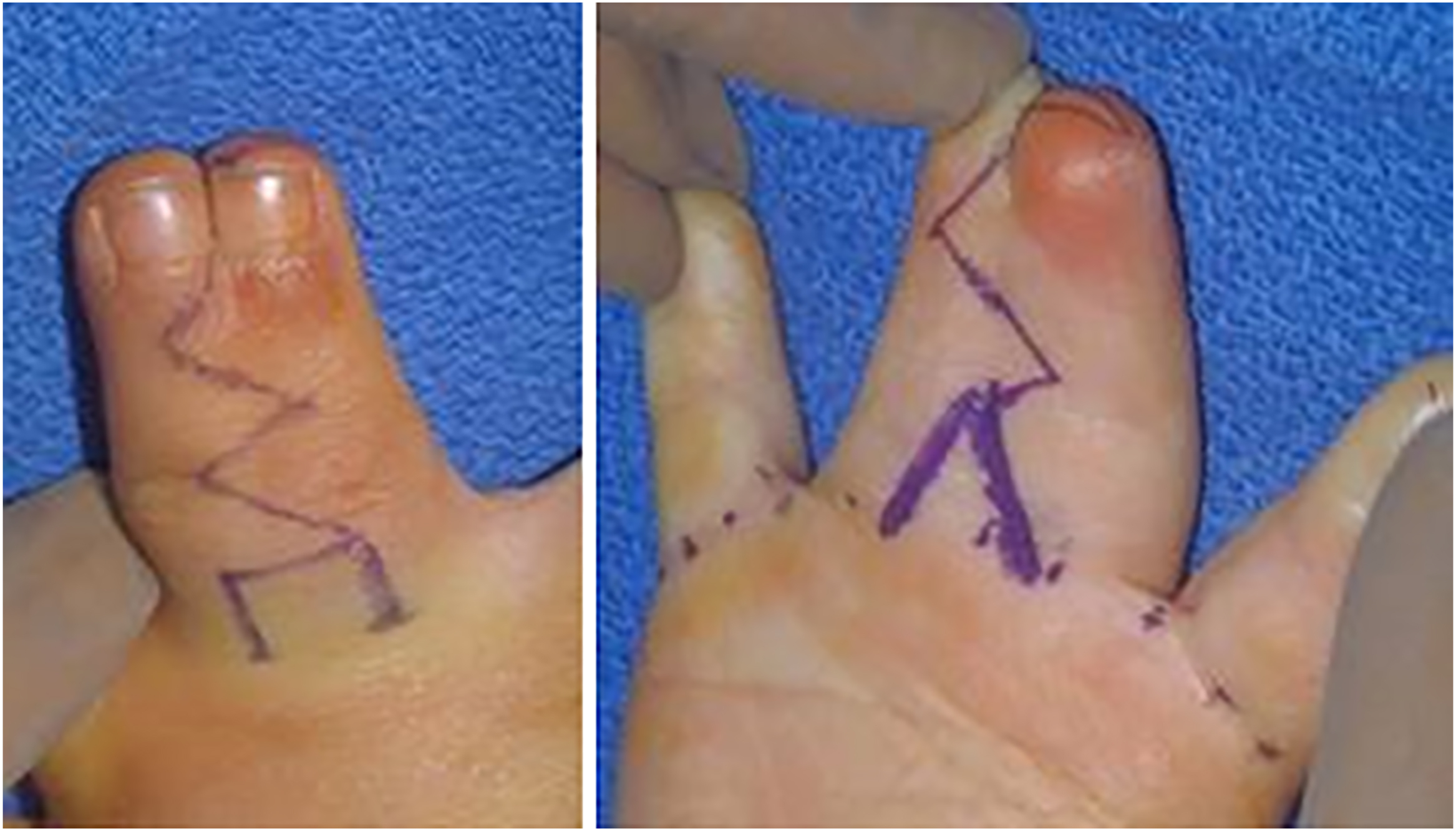
It is the senior author’s preferred technique to use interdigitating flaps with full-thickness skin grafts to cover defects. See Fig. 3 for suggested flap design.
- •
Marking the incisions requires strict attention to detail as this is a crucial component of the procedure.
- •
The base of volar flap should start at the metacarpophalangeal (MCP) crease, while the base of dorsal flap should start at metacarpal head. The interdigitating flaps should not cross the midline of the digits.
- •
The flap design in Fig. 3 is preferred by the senior author as it is felt to recreate the natural 45-degree slope to the webspace and avoids graft placement in the webspace. The horizontal component of the dorsal rectangular flap can be slightly angled to create a trapezoid. A vertical incision is made down the rectangle to inset the volar triangular flap ( Fig. 4 ).
- •
Skin graft can be obtained from the antecubital fossa (author’s preferred), groin, lower lateral abdomen—just medial to the anterior superior iliac spine, lateral foot, and wrist crease. The antecubital fossa is preferred by the senior author as it is in the surgical field, skin color is better matched, and the scar cosmetically hides well in the elbow crease.
Polydactyly
Postaxial polydactyly
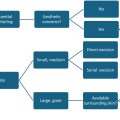
Postaxial, or ulnar polydactyly, is the most common form of polydactyly and is often associated with an inherited form transmitted in an autosomal dominant fashion with incomplete penetrance. , This is especially true among African American patients, for which the rate of syndromic etiology for ulnar polydactyly is under 1%. However, up to 10% of Caucasian children with ulnar polydactyly may have an underlying genetic syndrome; thus, these patients should be referred for genetic evaluation. The diagnosis of ulnar polydactyly is made clinically with radiographs used to differentiate between Type A postaxial polydactyly, when the digit contains osseous connection to the rest of the hand, and Type B, when the digit is connected by a skin bridge alone. , , Surgical removal is recommended for Type A, with options including corrective osteotomy, joint capsule reconstruction, and hypothenar muscle transfer. Cases involving the MCP joint of a preserved finger should include joint reconstruction to maintain digit stability. Meanwhile, Type B cases may be managed with ligation or with surgical excision. , , , , However, there is a paucity of rigorous research describing outcomes for ligation, and that which exists describes complications including neuroma formation, infection, and cyst formation as well as residual soft tissue prominences in an estimated 40% of patients treated with ligation; therefore, implementation of this technique requires judicious patient selection and family counseling. , , Many pediatric hand surgeons therefore prefer to surgically remove Type B postaxial polydactyly as a procedure in clinic or in the operating room.
Preaxial polydactyly
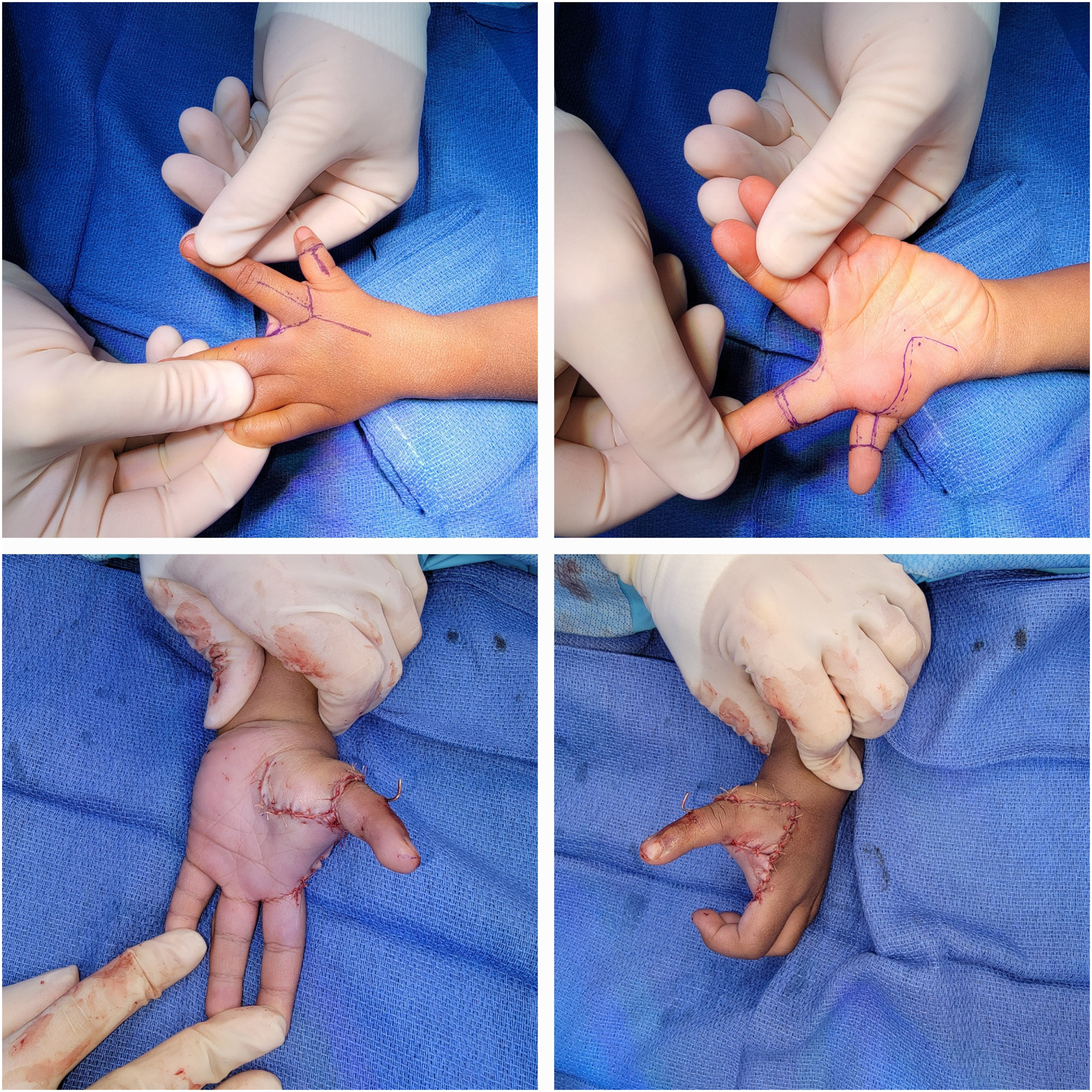
Preaxial, or radial polydactyly, is less common but often requires more intensive management to preserve the function of the thumb. Diagnosis is made clinically with the use of radiographs to further characterize the morphology ( Fig. 5 ). The Wassel-Flatt classification differentiates radial polydactyly according to the level of duplication, with type I describing a bifid distal phalanx, type II a duplicated distal phalanx, type III a bifid proximal phalanx, type IV a duplicated proximal phalanx, type V a bifid metacarpal, and type VI—the most common type accounting for 53% of cases in the original series of Flatt’s cases—characterized by a duplicated metacarpal. , Triphalangeal thumbs are classified as type VII. Treatment goals include recreation of a functional (stable) and cosmetic thumb , In particular, angulation of the interphalangeal joint after reconstruction is associated with decreased satisfaction while factors such as MCP joint angulation, reduced finger girth, or decreased nail width are more well tolerated. Reconstruction should typically be performed between 1 and 2 years of age. Techniques vary according to Wassel-Flatt type, but broadly can be characterized as excision with reconstruction, combination, or on-top plasty. Excision with reconstruction remains the most common approach, and typically includes collateral ligament transfer using periosteal flaps as well as flexor and extensor tendon centralization, with soft tissue flaps from the removed component to supplement the girth of the reconstructed digit. Corrective osteotomies can be used to correct residual extra-articular angulation while debridement of articular abnormalities including extra facets or cartilaginous bridges can re-align the articular surface. , Determining which of the duplicated digits to preserve and which to excise is made on a case-by-case basis though the ulnar digit is preferentially retained in type III or type IV polydactyly when possible to preserve the ulnar collateral ligament to preserve pinch strength; fortunately, the radial digit is also often more hypoplastic than the ulnar digit. , Postoperative pinning with Kirschner wire can protect ligament reconstructions during healing in conjunction with a postoperative thumb spica. , Type III and IV cases also often require muscle transfer, specifically for the abductor pollicis brevis which is commonly attached to the radial digit and must be transferred to the ulnar component to preserve abduction force and prevent ulnar angulation at the MCP joint. Reconstruction produces comparable grip strength and lateral pinch strength compared to the contralateral side with well-maintained range of motion, stability, and alignment over time; though, re-operation for painful residual instability is not uncommon. , ,
Combination surgery, or the Bilhaut-Cloquet procedure, for Wassel-Flatt Type II preaxial polydactyly is of historical interest, and was most applicable to cases with similar size between the 2 thumbs to preserve digit girth. This procedure involved resection of the central segment of the duplicated digit with reconstruction of the remaining components of the digit. However, initial techniques included combination of the articular surfaces and resulted in unpredictable outcomes with high rates of stiffness, growth disturbances, and cosmetic deformity with nail plate ridging or defects. , The Baek modification was made in an effort to produce improved outcomes by retaining a single interphalangeal joint and combining the non-articular components of the duplicated distal phalanx allowing for more precise reconstruction of the nail bed and preservation of interphalangeal joint motion and stability for Wassel-Flatt type II and sometimes III thumb duplications. Finally, on-top plasty can be employed for cases where one thumb is better developed proximally while the other is better developed distally, transposing the well-developed distal component of the one on a vascular pedicle to the well-developed proximal component of the other. , This technique can preserve a stable carpometacarpal joint of one digit and the stable MCP joint and interphalangeal joints of a duplicated digit, a phenotype sometimes seen with Wassel-Flatt V or VII thumb duplications. With appropriate patient selection, this technique has shown good functional outcomes including normal grip and pinch strength with normal distal sensation and favorable patient-reported outcomes with long-term follow-up.
Central polydactyly
Central polydactyly is the rarest form of polydactyly and has strong association with syndactyly and cleft hand bilaterally, such that this constellation is sometimes considered a single diagnosis of “abnormal induction of finger rays” related to abnormal development of the central apical ectodermal ridge. Epidemiologic studies on central polydactyly show strong family history, autosomal dominant inheritance patterns, and heritable gene mutations, like that of the homeobox gene HOXD13 on chromosome 2 responsible for ring finger synpolydactyly. , Central polydactyly can be classified into 3 types: type I, where duplicated fingers have no bony or ligamentous attachment to adjacent digits; type II, where the duplicated digit has normal anatomy distal to a joint or bifid metacarpal or phalanx from an adjacent digit; and type III, with a complete additional ray including the entire metacarpal. Treatment varies according to type. In type I and III, excision (with web space reconstruction and transverse intermetacarpal ligament reconstruction in type III) can be employed, often after 18 months of age to allow for the use of larger structures to aid with reconstruction. Management of type II central polydactyly is challenging due to joint stiffness and concurrent angular and rotation deformities, with many treatments leaving patients with limited motion and persistent deformity with minimal functional benefit. When performed, surgical intervention should include centralization and rebalancing of flexor and extensor tendons as well as reconstruction of collateral ligaments as needed for joint stability with reshaping of articular surfaces and corrective osteotomies for deformity of the metacarpals or phalanges. Treatment choices must be made on an individual basis and, especially in cases with complex deformity, should include careful consideration of nonoperative treatment or ray resection rather than digit reconstruction.
Polydactyly clinical care pearls
- •
In office excision of post-axial polydactyly is usually preferred by parents over anesthetic and operating room removal. The senior author prefers to use ligature clips in the office rather than suture ties. It is felt that the quick deployment of the staple allows closer approximation to the ulnar border of the hand. This decreases the incidence of forming a contour abnormality or neuroma in the senior author’s opinion.
- •
It is best to think of preaxial polydactyly as split thumbs rather than duplication. Neither thumb is completely normal. Even with surgery families should be counseled that the remaining thumb will likely be smaller, stiffer, and often slightly weaker than the contralateral unaffected thumb.
- •
Beware of divergent-convergent thumbs with a zig-zag configuration. These tend to regain angular deformity and often develop joint instability with time, and families should be advised of this possibility. What often looks like an immediately optimal result can change over time with follow-up.
Thumb hypoplasia
Thumb hypoplasia has tremendous phenotypic variability ranging from fully functional but undersized thumbs to complete absence of the digit, and is part of the spectrum of radial longitudinal deficiency with a strong association with underlying syndromic anomalies. All patients with thumb hypoplasia must be referred for genetic testing and medical evaluation, and early recognition and treatment for any underlying syndrome must take priority over management of digital deficiency; early recognition of underlying conditions such as Fanconi anemia can allow for early intervention and successful treatment of an otherwise fatal disease. Other associated conditions include Holt-Oram syndrome (linked with cardiac septal defects), vertebral defects, anal atresia, cardiac defects, tracheo-esophageal fistula, renal anomalies, and limb abnormalities association, and thrombocytopenia-absent radius syndrome .
Thumb hypoplasia is divided into 5 types ( Fig. 6 ) :
- •
Type I: Mild hypoplasia with small thumb.
- •
Type II: Thenar hypoplasia, MCP instability, and tight first web space.
- •
Type III: Features of type II with additional skeletal hypoplasia and loss of both intrinsic and extrinsic musculature. Further divided according to the stability of the carpometacarpal (CMC) joint as type III-A, with a stable CMC joint, and type III-B, with an unstable or absent CMC joint.
- •
Type IV: Rudimentary skeletal elements in an unstable thumb with only soft tissue connection to the hand.
- •
Type V: Thumb aplasia.
- •
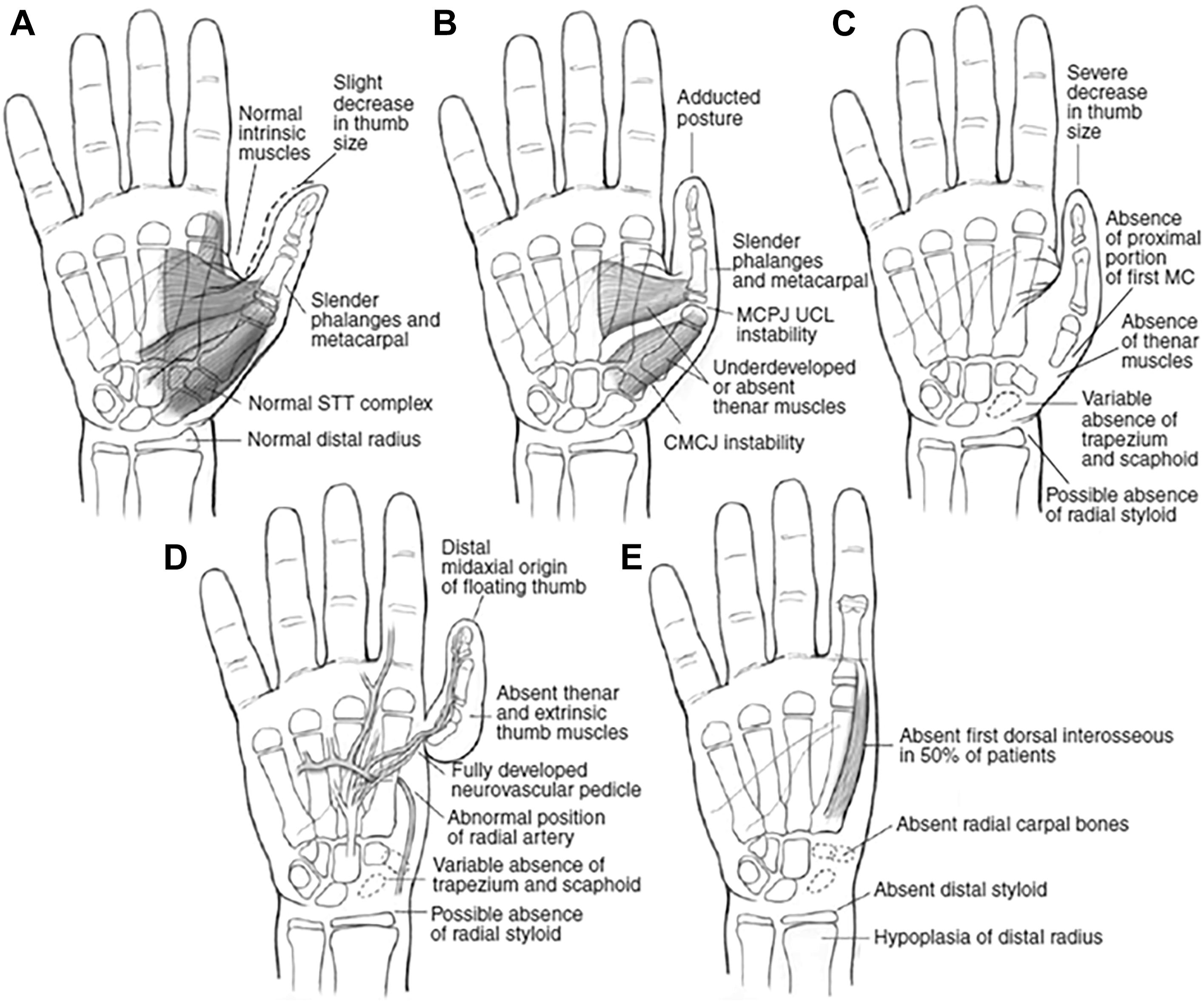
Treatment varies according to type. In cases of type I hypoplasia, no treatment is typically required, though some cases with weak opposition may benefit from tendon transfers to supplement the abductor pollicis brevis and opponens pollicis. Other cases with a tight first webspace may benefit from first webspace z-plasty. In type II, treatment often consists of some combination of release of web space contractures, ligament reconstruction for the MCP joint, and supplementation of hypoplastic thenar muscles with opponensplasty often using the flexor digitorum superficialis or the adductor digiti minimi (Huber opponensplasty). Treatment of type III hypoplasia is dependent on the stability of the carpometacarpal joint. Type IIIA hypoplasia is treated similarly to type II hypoplasia, with the addition of MCP joint reconstruction or arthrodesis for instability as well as division of any tendon interconnections and reorientation of misrouted extrinsic tendons coupled with pulley reconstruction, as well as flexor pollicis longus reconstruction (often with 2-stage procedure, or with ring finger flexor digitorum superficialis transfer) for cases with absent or grossly nonfunctional flexor tendon.
Pollicization
Type IIIB, IV, and V are treated with pollicization, with similar technique employed for all 3 types, with the goal of producing a thumb with about one-third the normal strength, intact sensation, and functioning opposition with pulp-to-pulp pinch. Pollicization may employ multiple skin incisions to allow for appropriate access to the index finger and adequate reconstruction of a first web space, in particular, exposure of the lateral bands is necessary to allow for access to the intrinsic muscles for transfer. When designing an incision, it is important to try and keep suture lines out of the first webspace or to use z-plasties to break up the linear scars to avoid contractures. During exposure, careful preservation of the skin veins in the dorsal skin flap is crucial to prevent postoperative venous congestion. Many cases may require intraneural neurolysis of the digital nerve to separate the index digital nerve from the long finger digital nerve proximally within the common digital nerve in the palm. The radial digital artery to the long finger will need to be ligated to alleviate tension on the neurovascular bundle after transfer of the index finger. To transpose the index finger, the metacarpal must be shortened, and is divided through the physis preserving only the distal-most articular surface. The physis is ablated to prevent overgrowth of the new thumb in the future. The index MCP joint is then secured to the carpus, doing so in a maximally hyperextended position can prevent subsequent “z” deformity using nonabsorbable suture. , The intrinsic muscles must then be transferred to repurpose the first dorsal interosseous as the abductor and the first palmar interosseous as the adductor. Finally, the extrinsic extensors including the extensor digitorum communis and the extensor indicis proprius are sometimes shortened and transferred, with the extensor digitorum communis acting as the abductor pollicis longus and the extensor indicis acting as the extensor pollicis longus. Manske and colleagues published long-term follow-up with an average of 8 years demonstrating functional outcomes for pollicization including grip strength, lateral pinch, tripod, pinch, and tip pinch averaging 21% to 26% normal values, but in 84% of cases, patients used the pollicized digit including for 92% of activities involving handling of large objects. These results were not associated with patient age at the time of surgery. Goldfarb and colleagues published a series of 73 cases showing 8 perioperative complications including 4 cases of marginal necrosis and 3 cases of venous congestion as well as 8 suboptimal outcomes of which 7 were scar contractures, ultimately leading to revision surgery in 26 patients—though 6 of these cases did not have extensor tendon shortening during their primary procedure .