Effective management of cleft lip requires a comprehensive interdisciplinary approach that addresses the multifaceted dimensions of care. Although treatment spans infancy to adulthood and outcomes are influenced by growth and development, the critical stage of care is at primary reconstruction. This review aims to integrate recent insights from data-driven 3D analysis of cleft lip and nasal deformities into our foundational approaches for primary reconstruction of both unilateral and bilateral cleft lip. It also aims to organize the many methods of repair of both lip and nose according to principles of surgery so that, similarities, differences, and controversies can be highlighted.
Key points
- •
The cleft lip and nasal deformity occurs from disruption of orbicularis oris muscle and uncoupled premaxillary growth. The severity occurs along a spectrum related to the extent of clefting along lines of fusion. The asymmetric disruption/uncoupling in a unilateral cleft produces a twist deformity. The symmetric disruption/uncoupling in a bilateral cleft results in unrestrained growth of the premaxilla.
- •
Goals of unilateral cleft lip repair are to level Cupid’s bow, centralize the prolabium and columella, and balance the alar base positions (by advancing the cleft alar base anteriorly and the noncleft alar base medially), in addition to reconstructing the orbicularis sphincter.
- •
Goals of bilateral cleft lip repair are to construct a philtrum using the prolabium, produce adequate central lip fullness to allow lip competence, and balance nasal base relationships (by advancing alar bases anteriorly), in addition to reconstructing the orbicularis sphincter.
Introduction
Management of cleft lip involves changing techniques and evolving principles. Meanwhile, comprehensive care has broadened to incorporate a multidisciplinary team approach with focus on the patient and family. The American Cleft Palate-Craniofacial Association has established standards of team composition, team management, communication, cultural competence, psychological/social services, and outcome assessment ( www.acpa-cpf.org ). While the focus of this review is on surgery, management by a specialized center with a concentration of expertise and interdisciplinary care is emphasized.
Cleft lip ( ± cleft palate), or CL/P, occurs in approximately 2 out of 1000 Asians, 1 out of 1000 Caucasians, and 0.5 out of 1000 African Americans with a 6:3:1 ratio of left:right:bilateral involvement. The condition is more common in boys and is usually sporadic (70%). Isolated cleft palate occurs in 0.5 out of 1000 newborns regardless of ethnicity, is more common in girls, and more frequently associated with syndromes (50%). Associated syndromes include van der Woude (lower lip pits); Stickler (type 2 collagen abnormality with myopia, retinal detachment, and glaucoma); 22Q11 deletion (multiple facial characteristics, developmental delay, and other associations); CHARGE; Goldenhar/oculo-auriculo-vertebral; ectrodactyly, ectodermal dysplasia, cleft; and Smith-Lemli-Opitz. When not syndromic, the etiology of CL/P is thought to be multifactorial. The risk of a future child with CL/P is 4% if 1 child or parent is affected, 9% if 2 children are affected, and 17% if a child and a parent are affected.
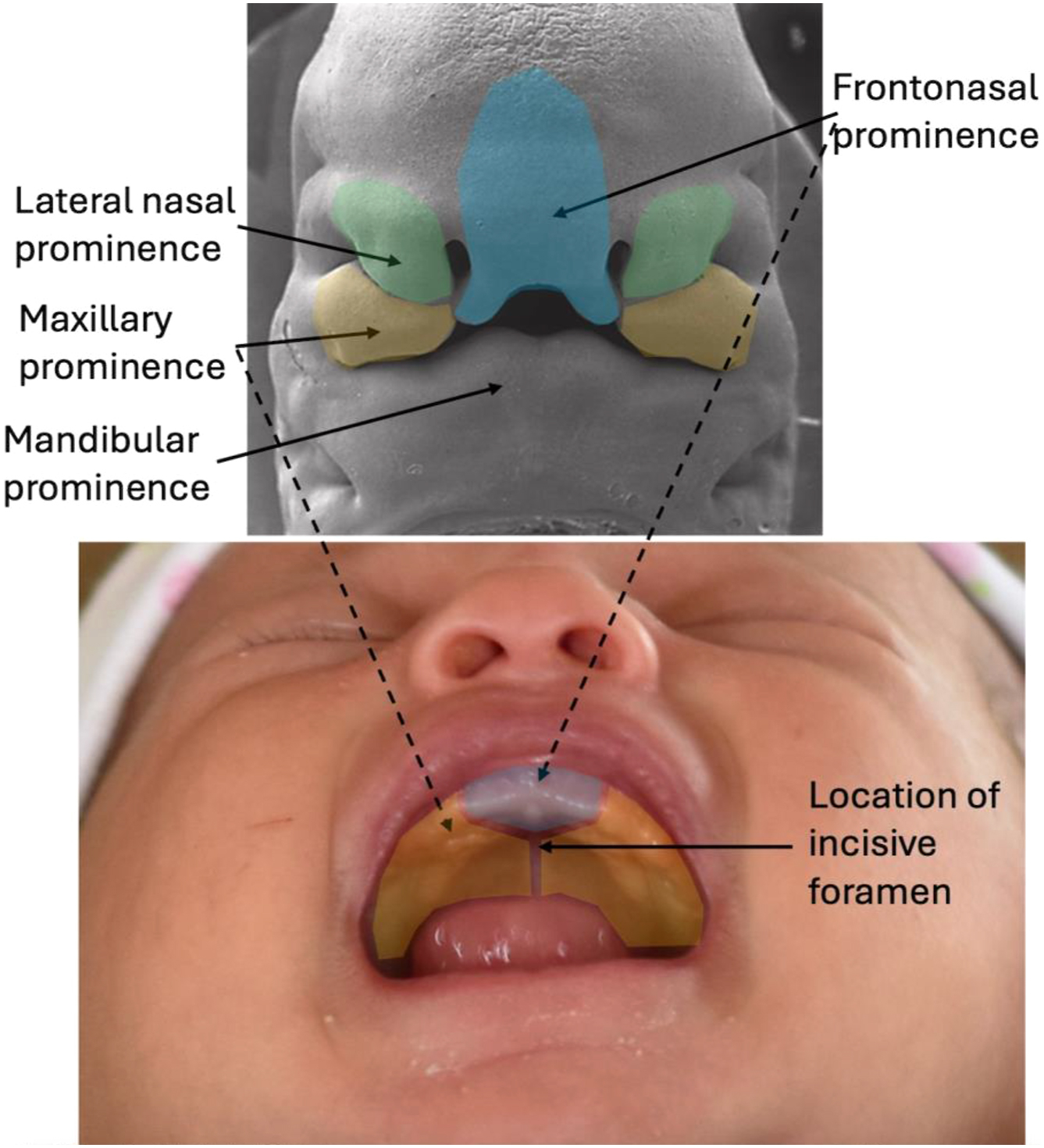
At 4 to 6 weeks of gestation, the medial nasal, lateral nasal, and maxillary processes fuse to form the nose, upper lip, and primary palate ( Fig. 1 ). Posterior to the incisive foramen, the secondary palate develops from fusion of lateral palatine processes at 6 to 12 weeks of gestation.
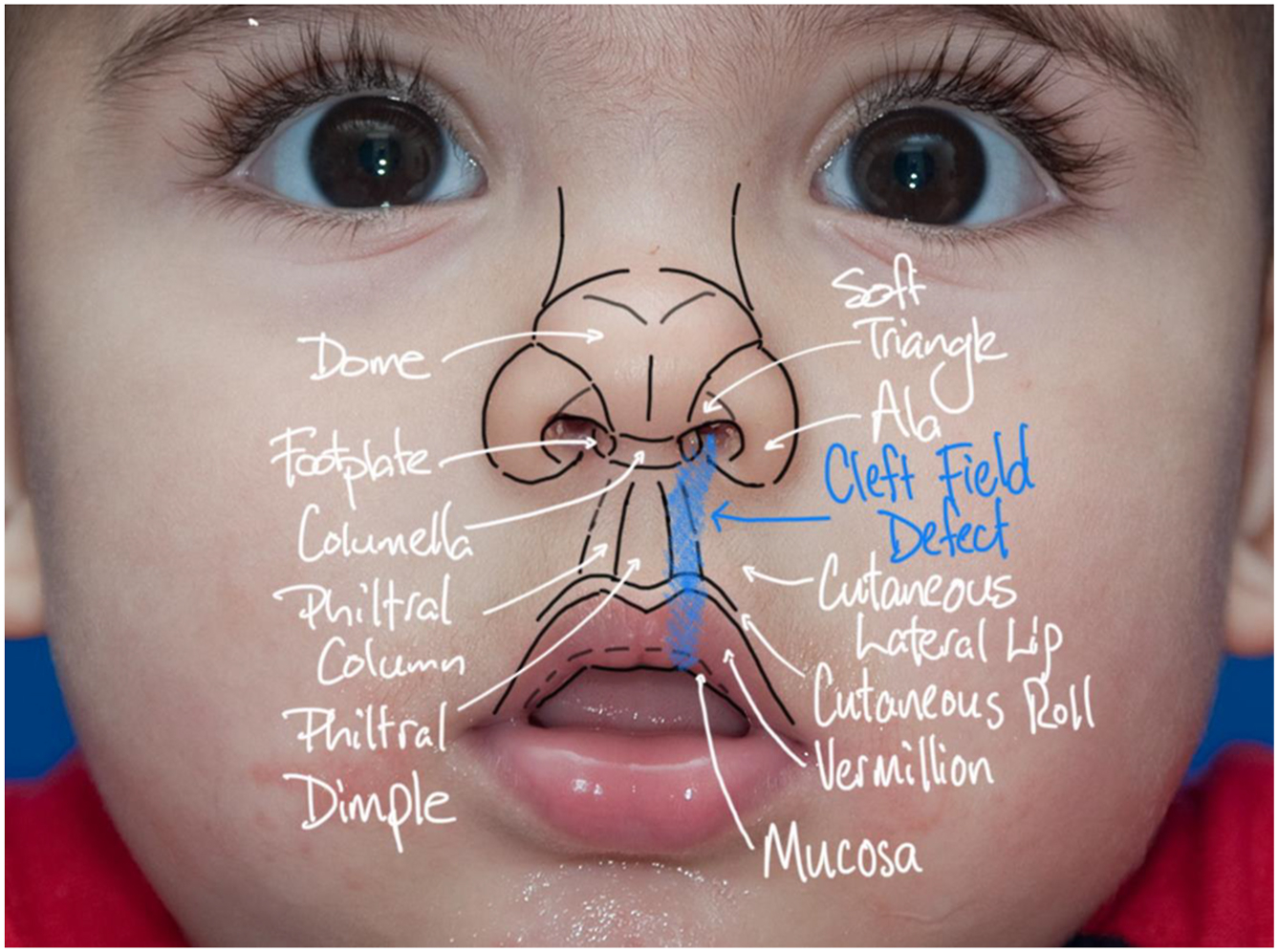
The nasolabial anatomic subunits are detailed in Fig. 2 . The cutaneous roll has a shiny convex appearance and is characterized by sparse vellus hair. The vermilion or “dry” red lip is keratinized squamous epithelium that contains an abundance of superficial capillaries. In contrast, the mucosa or “wet” red lip is nonkeratinized. Deep to skin the pars peripheralis of the orbicularis oris muscle forms a compact midline decussation with fibers inserting into skin on either side of the philtral ridges.
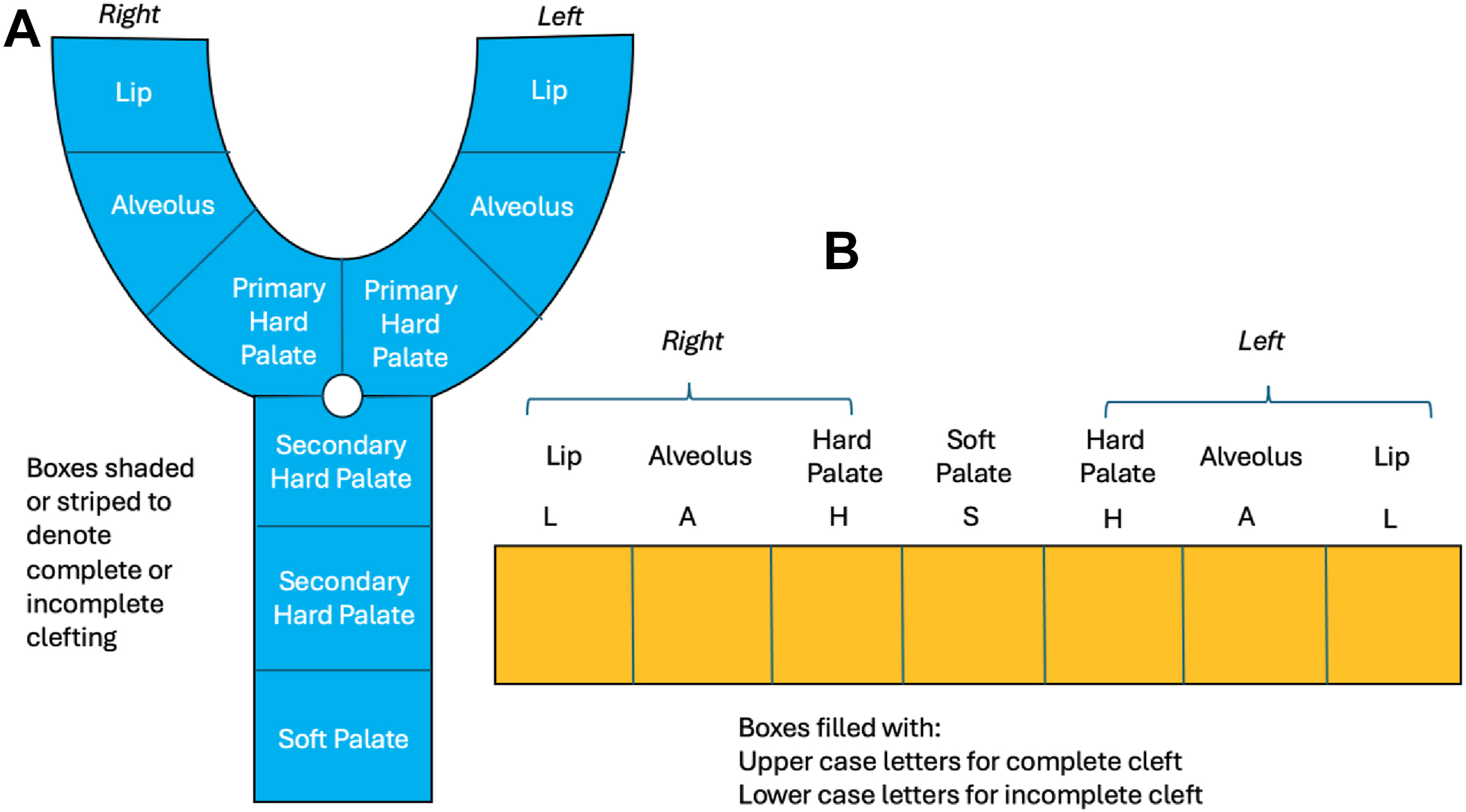
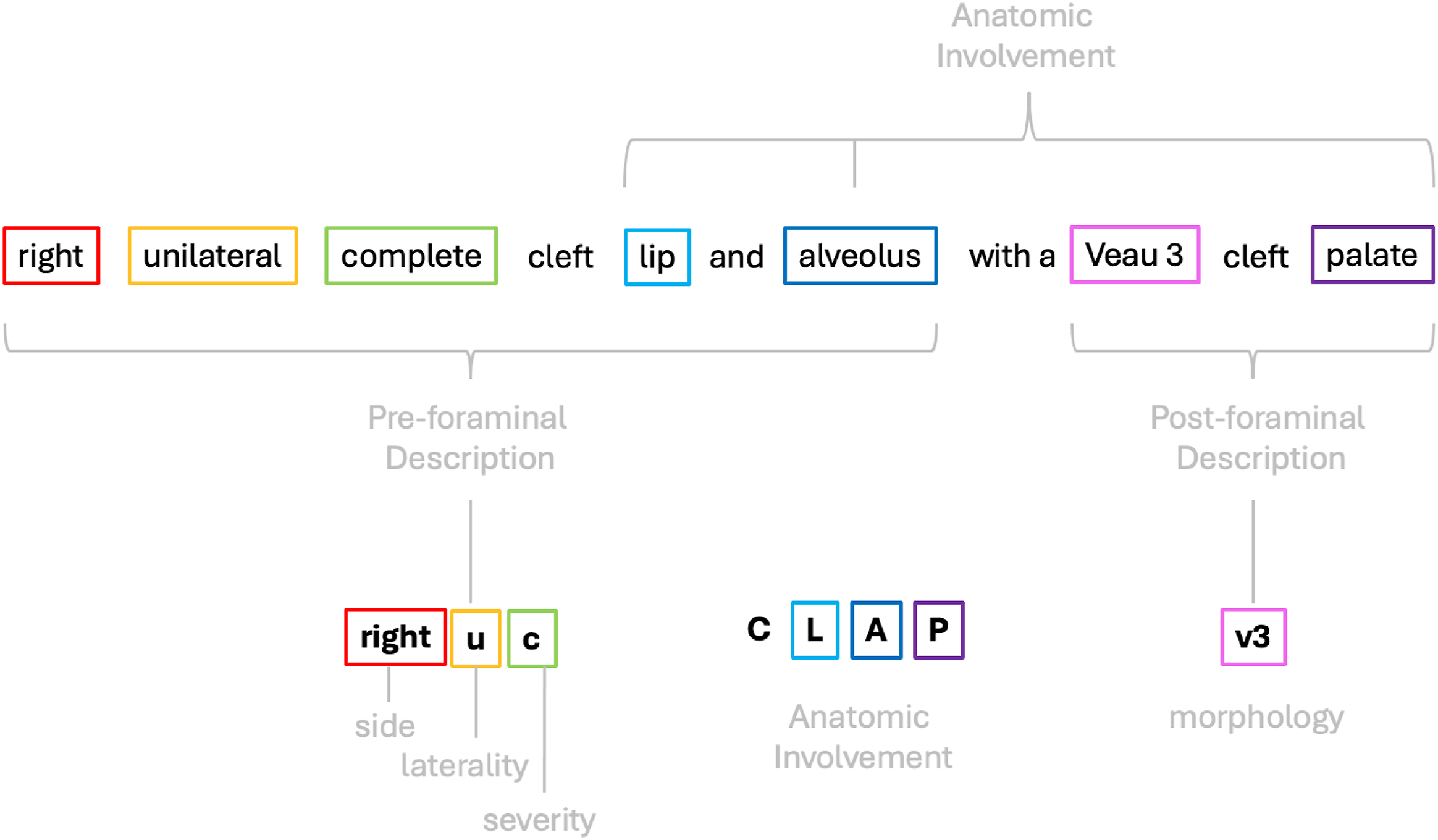
Failure of mesenchymal penetration along embryologic lines of fusion results in clefting. The extent of involvement typically progresses from anterior to posterior. Kernahan’s Y and the LAHSHAL notation provide means for classification ( Fig. 3 ), but are cumbersome. The “CLAP notation” is recently proposed as an alternative, which represents the involved structures (lip, alveolus, and palate, respectively), the lowercase prefix serves as a descriptor of cleft lip severity and laterality and the suffix provides information regarding the morphology of the palate ( Fig. 4 ).
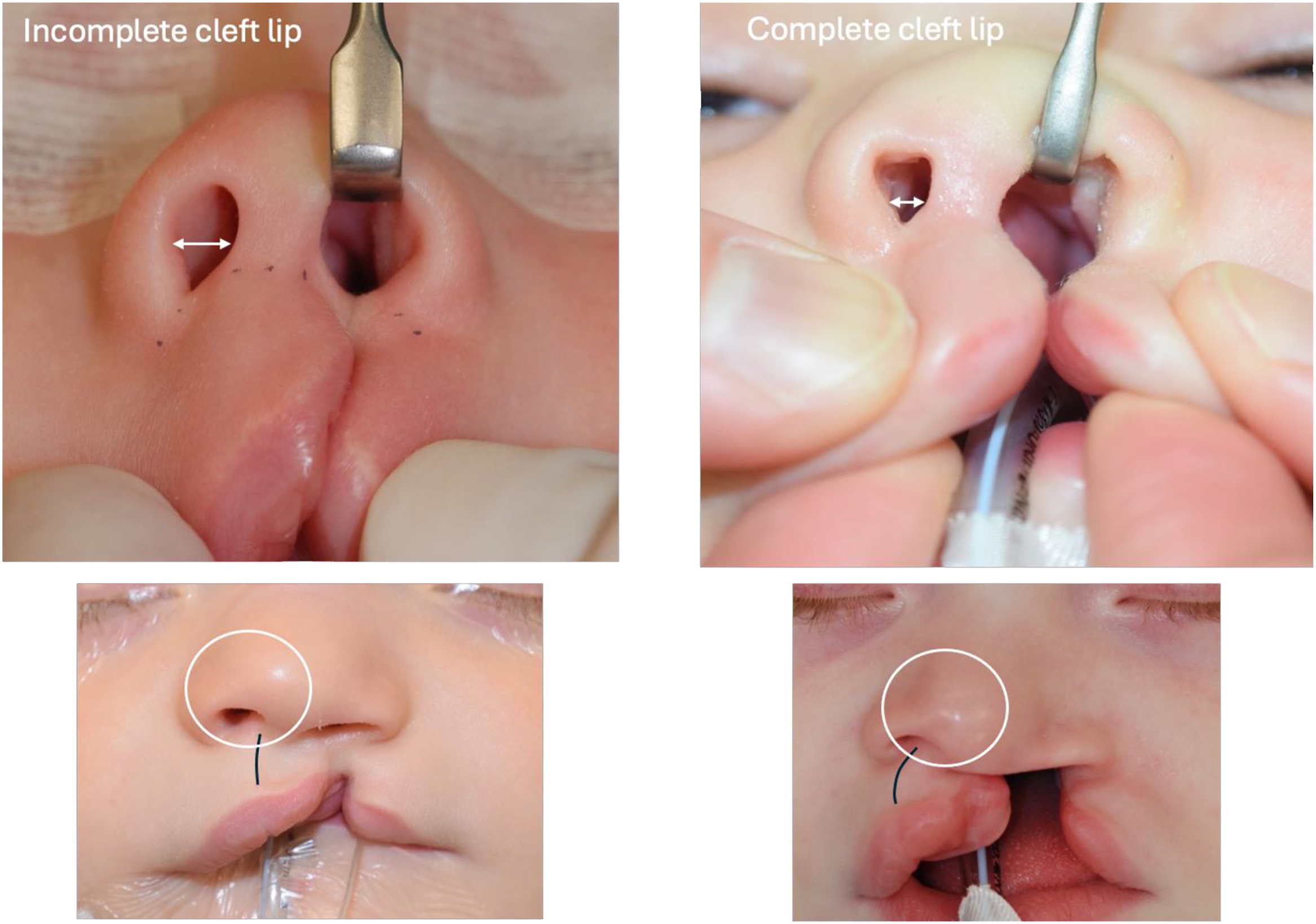
In addition to the extent of involvement, the severity of cleft lip ( Fig. 5 ) may be complete, complete with soft tissue band (where there is a complete alveolar cleft), incomplete, or microform (involving less than one-fourth of the lip height or <3 mm above the Cupid’s bow peak ).
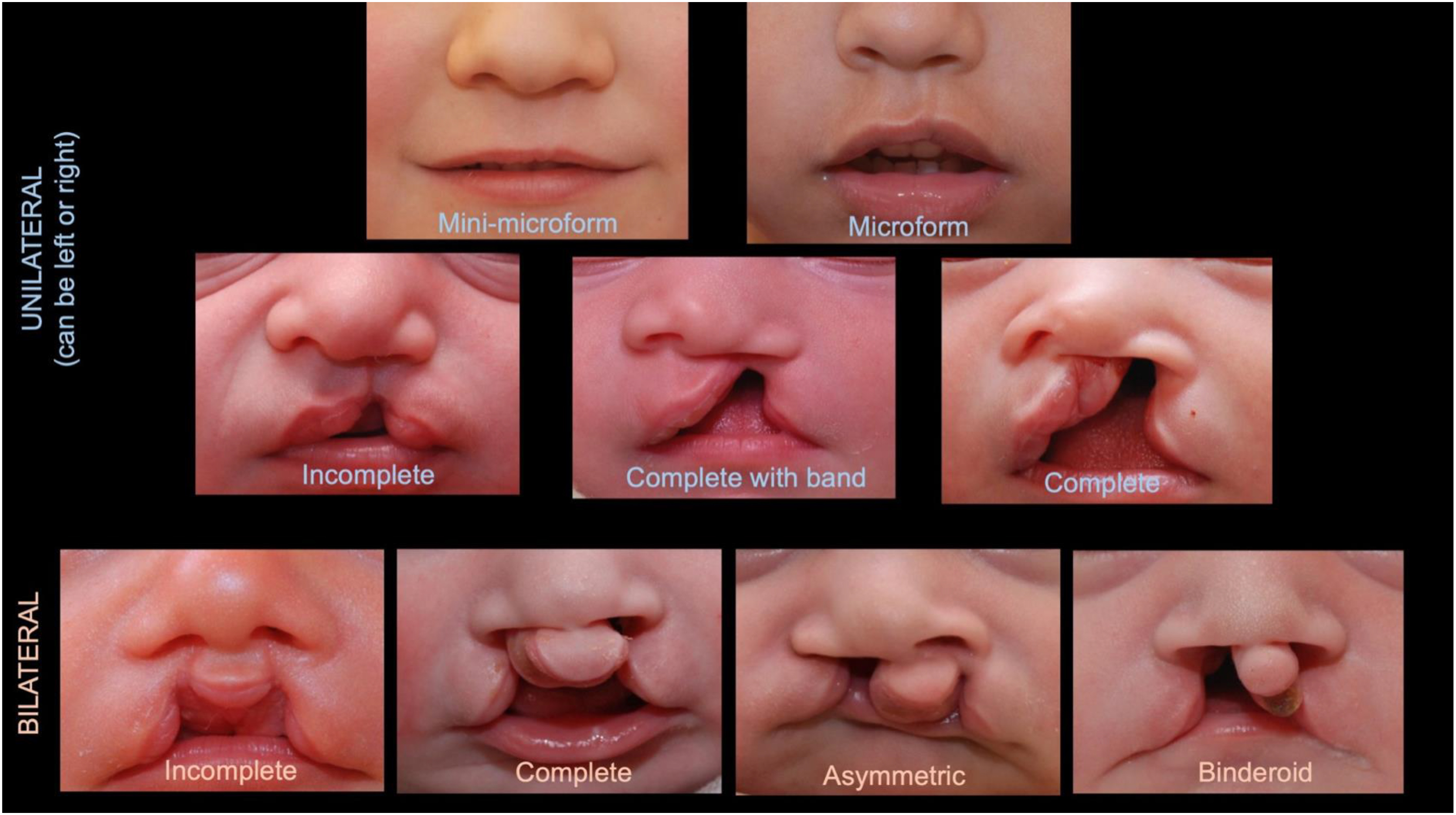
Note that these conventions for grading severity are limited because they rely upon external examination of the “ectodermal defect” (involving skin and surface tissues) when the underlying “mesodermal defect” (involving muscle and bone) can be more extensive. Patients presenting with a mild cleft lip deforming may also demonstrate a severe nasal deformity due to a more extensive subdermal/submucosal disruption of muscle or bone.
Presurgical molding
Malleable tissues and cartilage plasticity due to persistent maternal estrogen circulation as well as rapid facial growth provide an opportunity for molding to facilitate surgical repair. Molding sets out to align the alveolar segments/arch and improve the nasal shape. The role of molding for unilateral clefts continues to be debated there are few well-controlled long-term comparative studies to justify the additional costs and burden. Although there is even less evidence to support molding for bilateral clefts, clinical consensus is that it can be helpful to limit the protrusion of the premaxilla and, when a molding plate is used, reduce the collapse of lesser segments that can result in the premaxilla being “locked out” anterior to a U-shaped alveolar arch.
Passive Molding
Lip taping produces an indirect restraining force on the alveolar segments that is simple, inexpensive, and can reduce an alveolar gap. Alveolar molding employs a regularly adjusted custom appliance to guide palatal growth. It provides greater control but requires a skilled orthodontist and frequent visits, and it may not be tolerated. Nasoalveolar molding (NAM) combines an intraoral molding device with nasal stent(s) to guide both the alveolar arch and nasal cartilage. It may provide subtle long-term improvements but can be burdensome and risks producing a “mega-nostril” by overstretching an ala that remains tethered to the alveolus. An alternative to NAM that does not require frequent visits involves lip taping with nasal elevator/stent. Outcomes similar to NAM have been reported.
Active Molding
In the 1980s, Latham introduced a surgical procedure to place a pin-retained, screw-activated appliance. This has been shown to deproject the maxilla and expand the lateral alveolar cleft segments via mechanical means. While this type of presurgical treatment provides more control and prevents the child’s removal, it requires significant commitment by the caregivers, exposes the child to an additional anesthesia event, and may lead to growth restriction and malocclusion.
Lip Adhesion
A partial repair of the cleft lip can produce restraining forces that mold alveolar segments. The adhesion involves tissues along the cleft margin that would normally be discarded during definitive repair. Proponents advocate that conversion of a cleft to a less-severe form facilitates definitive repair while skeptics argue that the additional surgery is unnecessary and the scar compromises the ultimate outcome.
Surgical treatment
Timing of Repair
Traditionally, repair has been performed as early as 3 months of age; however, there is no evidence that early surgery enhances scar quality. Additionally, as children grow, their tissues become more robust and easier to manage, perioperative care can be less challenging for parents, and the risks associated with anesthesia are minimized. Consequently, some centers choose to postpone repair until 6 months of age, and in cases without an associated cleft palate, until 9 months of age.
In few areas of plastic surgery is a grasp of complex 3 dimensional anatomy as crucial as in cleft lip repair. While the nose is often viewed as distinct from the lip, they are inherently interconnected. The premaxilla is the growth center of the midface, and when the link between segments is disrupted by a cleft, the uncoupled growth results in distinct nasolabial manifestations. In a unilateral cleft, the uncoupling is asymmetric, thereby producing a twist deformity, while in a bilateral cleft, the uncoupling is symmetric, resulting in unrestrained premaxillary growth and a stretch deformity ( Fig. 6 ).
Unilateral Clefts
The deformity
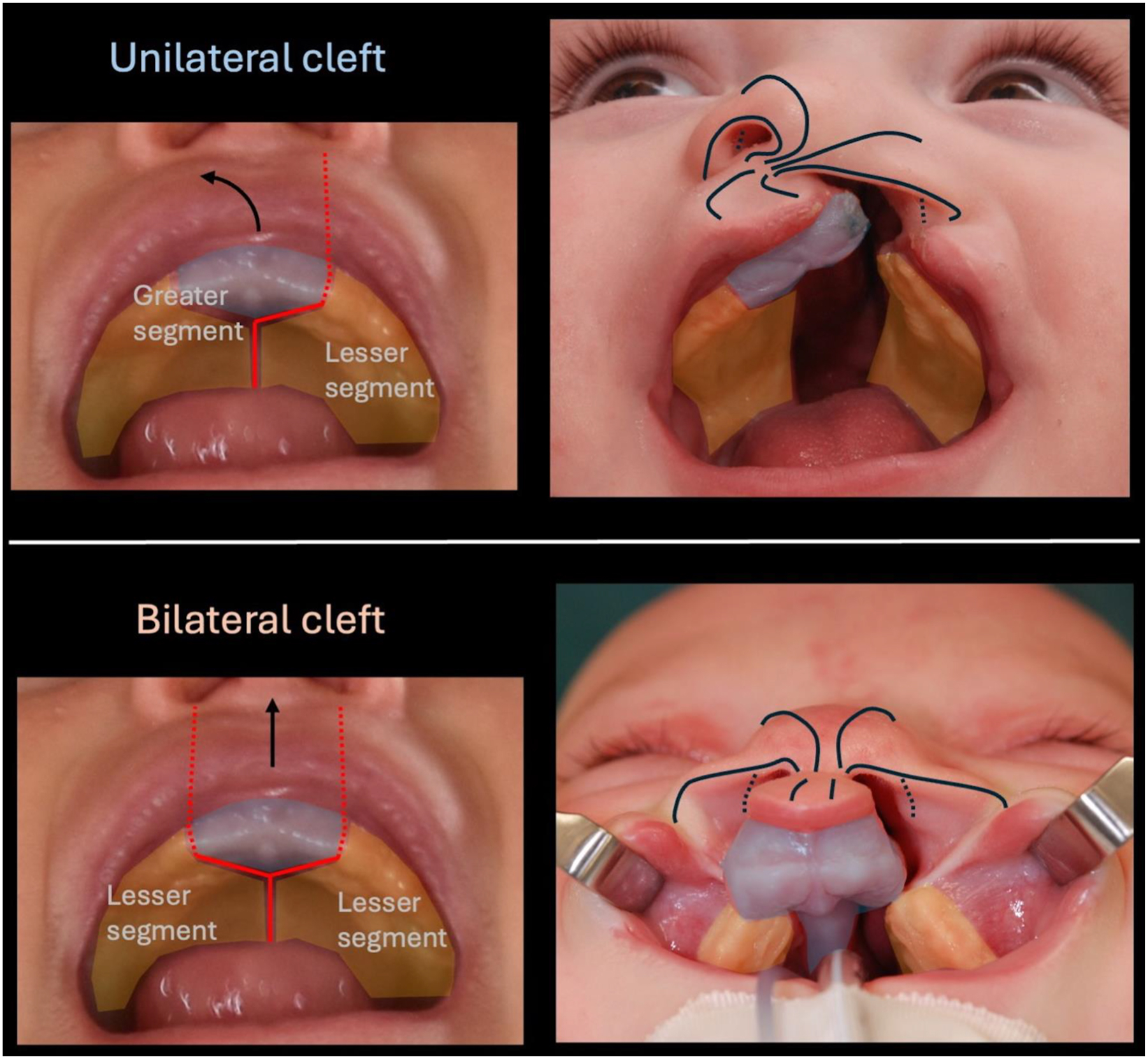
Understanding cleft lip nomenclature is essential for minimizing ambiguity and enhancing the comprehension and advancement of surgical techniques ( Table 1 ).
| Structure | Definition |
|---|---|
| Greater segment | The larger alveolar/palatal segment of the maxilla in a complete cleft lip and palate that includes the premaxilla. |
| Lesser segment | The smaller alveolar/palatal segment of the maxilla in a complete cleft lip and palate that does not include the premaxilla. |
| Lateral lip element | Upper lip tissue on the lateral side of the cleft |
| Medial lip element | Upper lip tissue of the prolabium. Depending upon the cleft, this may be on the medial side of the cleft, midline, or deviated into the non-cleft side of the face. This element will eventually be on the medial side relative to the site of closure along the cleft. |
Along the cleft margins, structures taper away, and tissues become hypoplastic. Disruption of the orbicularis sphincter results in abnormal muscle “insertions” at the cleft-sided alar base and columella, which accentuate the widened nasal sill on animation ( Fig. 7 ).
On the medial lip element, shortening of the philtral height on the cleft side (compared to the noncleft side) of the philtrum results in an upward tilt of Cupid’s bow. The peak of Cupid’s bow on the noncleft side has a convex contour, whereas on the cleft side, there is no distinct peak and the tissues taper toward the cleft.
On the lateral lip element, there may be a convex contour corresponding to the lateral side of the Cupid’s bow peak. At the medial extent of this contour is Noordhoff point , which was originally defined as the location along the lip where the vermilion height is the tallest and the vermilion-cutaneous junction (“red line”) begins to taper toward the vermilion border. Lateral to this point, the cutaneous roll is well defined, whereas medial to this point, it becomes less distinct.
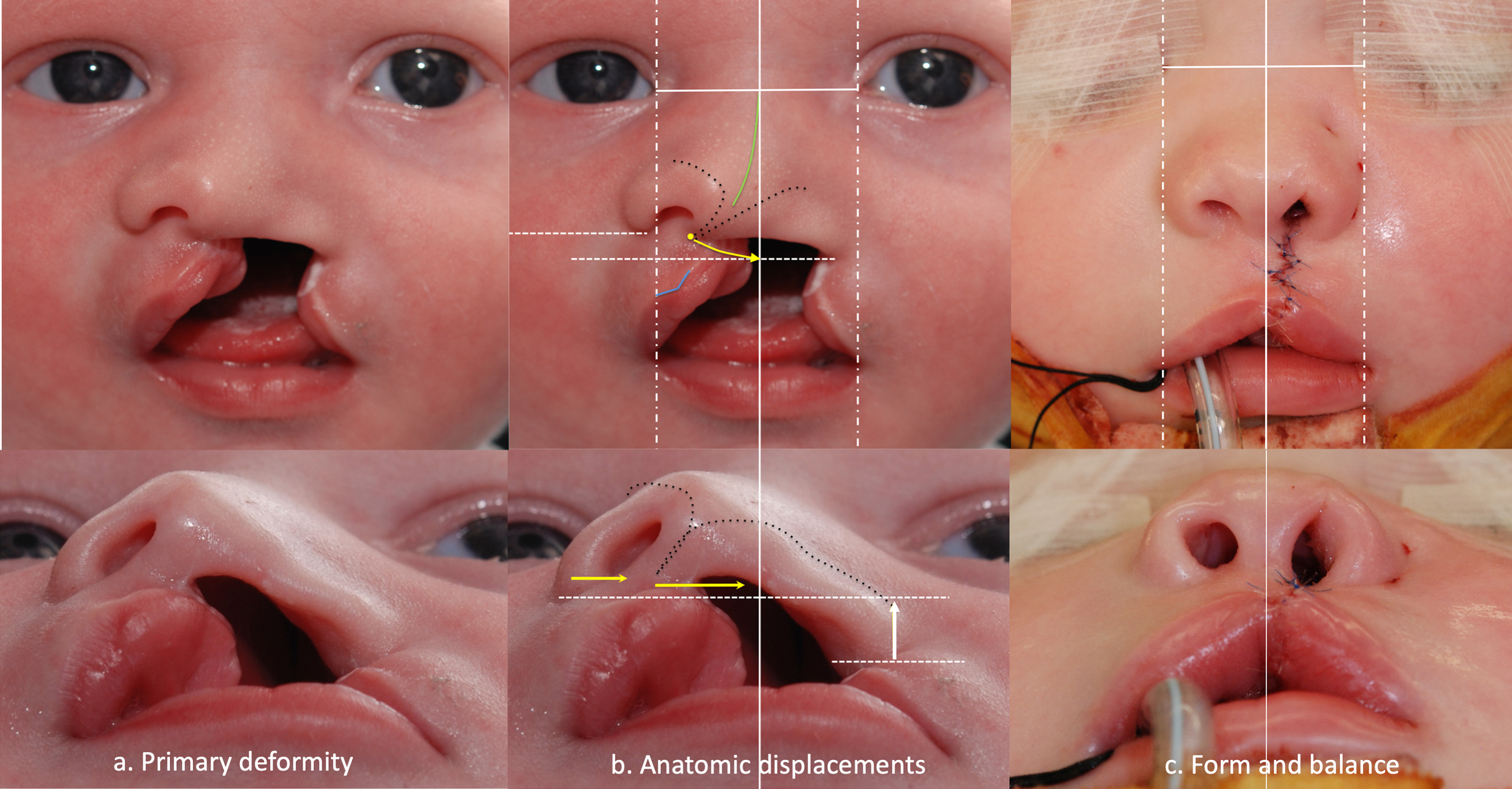
Under the surface, the relationship of maxillary segments defines 3-dimensional nasolabial configurations ( Fig. 7 ). Uncoupling of the greater and lesser segments results in an outward, forward, and upward swing of the premaxilla that drives the prolabium, anterior nasal spine, caudal septum, and columellar base away from midline and onto the noncleft side of the face. The nasal dorsum (including dorsal septum and bony pyramid) follow, deviating to the noncleft side. Meanwhile, lateral to the cleft, the lesser segment has been “left behind,” resulting in posterior retrusion of the lateral lip and cleft alar base (that is normal in its medial-to-lateral position). The orthogonal vectors of displacement result not only in an obliquely oriented widening of the lip but also in a twisting collapse of the alar dome. The degree of displacement and consequent nasal collapse occurs along a continuum related to the outward swing of the premaxilla (that is governed by the degree and extent of uncoupling by the cleft) and explains the clinical spectrum of presentation.
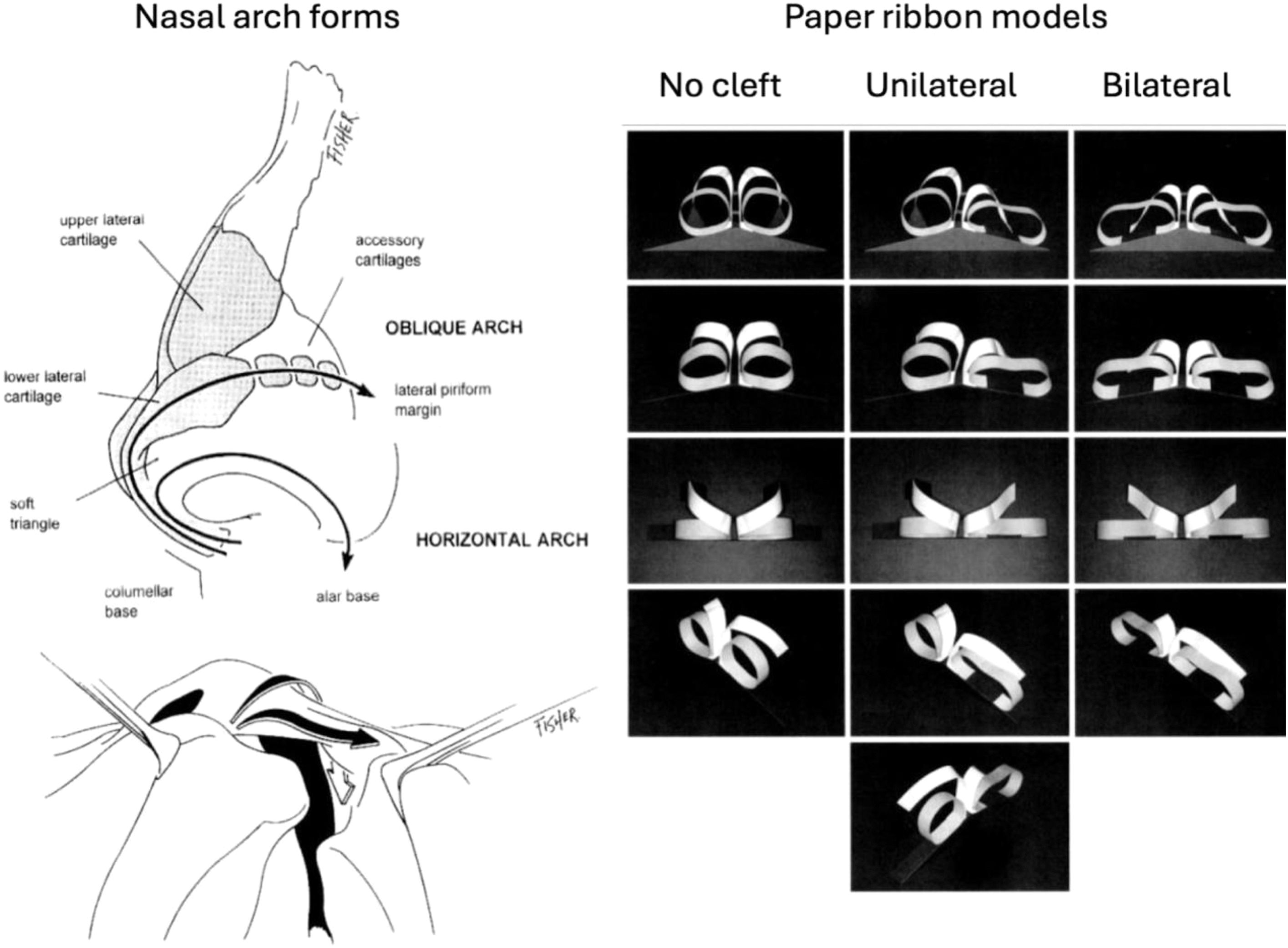
In the conceptual model proposed by Fisher, nasal form is defined by horizontal and oblique arches that follow the nostril rim and the lower lateral cartilage/accessory chain of cartilages, respectively ( Fig. 8 ). If those arches are represented by paper ribbons, when their ends are moved, the resulting shapes mimic those of the nasal deformity. Specifically, on the cleft side (where the base elements are widened), the medial genu of the lower lateral cartilage (LLC) becomes obtuse and the lateral crus of LLC contributes to a vestibular web.
Goals of treatment seek to reverse these aberrations. In addition to leveling Cupid’s bow and aligning elements of respective subunits (including cutaneous roll and vermilion), the prolabium needs to be centralized and the lateral lip advanced anteriorly ( Fig. 7 ). To untwist the nose, the columellar base needs to be centralized and alar base positions need to be balanced by moving the noncleft alar base medial and the cleft alar base anterior.
An appreciation of the subtle features of the deformity helps when balancing nasolabial elements to achieve harmony. The noncleft side has historically been treated as the “normal ideal” or “unaffected side”; however, the asymmetric uncoupling produces opposing changes to the noncleft side. As the premaxilla “drives” the nose lateral and “pushes” the noncleft alar base with it, the noncleft nasal sill gets “squished” ( Fig. 9 ). That constriction “pinches” the lateral alar crural ring causing the noncleft tip defining point to elevate and appear “boxy.” These noncleft side alterations occur in opposition to the cleft side where our attention focuses on the widened nasal sill and slumped tip/hemidome. In addition, as the cleft philtral height shortens, the noncleft philtral height bows and elongates. Although these features are less apparent, they can be seen when examining patients across the spectrum of presentation (see Fig. 9 ) and when carefully tracking changes through a repair ( Fig. 10 ). Through surgery, the noncleft nasal sill widens, the noncleft nasal tip defining point softens, the noncleft philtral height shortens, and the shape of the upper cutaneous lip subunit changes shape. Recognizing the dynamic nature of the noncleft side is important when trying to achieve balance.