CHAPTER 14 Dermatologic Implications of Secondary Lymphedema of the Lower Leg
KEY POINTS
Peau d’orange skin texture, a common presentation of lymphedema, results from swelling of the upper dermis limited by tethering of adnexal structures to the skin.
Most dermatologic manifestations of lymphedema occur in the lower extremity.
Venous insufficiency should be estimated in all patients with lymphedema.
Lymphatic filariasis is the most common cause of lower extremity lymphedema. It is transmitted by mosquito and is endemic in 78 developing nations.
Podoconiosis (or mossy foot), which results from damage to the tissues and lymph nodes of individuals who walk barefoot in irritant soil, is commonly observed in Ethiopia.
Recurrent secondary infection from bacteria and fungi worsen lymphedema.
Excess collagen and dilated thick-walled lymphatics and loss of elastin are the key histologic changes associated with worsening lymphedema.
Most of the changes seen with lymphedema occur in the lower extremity rather than in the upper extremity. For that reason, this chapter concentrates on changes of the lower leg. Primary lymphedema is caused by congenital hypoplasia of the lymphatics, failures of connection between the initial and connecting lymphatics, or impaired connections with the blood vascular system. Lymph is intercellular fluid formed by blood capillaries plus macromolecules and cells generated in the skin but not taken up by the venous system. The classic theory is that 90% of this fluid is absorbed by the venules, but this is no longer considered the case. The new perspective on fluid exchange postulates that there is dwindling filtration along the arterial and venous blood capillaries. Thus the lymphatic system is the only effective means of removing capillary filtrate from most tissues. 1 The brain is the most studied exception.
If the balance between filtration and resorption is disturbed, fluid accumulates in the intercellular space and edema develops. When this becomes chronic, the tissues react with the development of fibrosis and hyperplasia—features of lymphedema—and in its severest form elephantiasis. Many causes account for the failure of normal function, including cardiac failure, renal failure, gravitational overload of the venous system and immobility, inflammation, cancer and its treatment by surgery or radiotherapy 2 and lymphatic filariasis 3 (see Chapter 15).
Normal and Pathologic Tissue Fluids
There is, of course, always some fluid in the interstitium provided by its blood supply and controlled by Starling’s law that describes the balance between intravascular and tissue hydrostatic and oncotic forces. It is currently believed that lymphedema results from a failure of lymphatic function. It rarely is a total failure; mostly it is a partial failure aggravated by overload from a failing venous system or inflammation causing transudation from the blood capillary bed.
The richest capillary bed of the skin is found immediately deep to the epidermis, and the network of initial lymphatics lies immediately deep to the blood supply at the junction of the upper and middle dermis. When sectioned horizontally, the rete ridges of the epidermis provide a closely knit network. The capillary bed lies deep to this by less than 0.1 mm and has slightly wider mesh and hairpin-shaped capillary loops projecting into the papillae. Below that is the initial lymphatic network with a much wider mesh (up to 1.0 mm) lying at the junction of the upper and middermis normally without projections into the papillae. This layering was well illustrated by Kubik and Manestar 4 and can be reproduced and downloaded from Ikomi and Schmid-Schönbein. 5
Ultrasonographic studies of the skin show very clearly the relative water content versus cellular and fibrous components of the skin. They reveal the relative density of the epidermis, the collagen fibers of the dermis, and the water-filled interstitium. Most of the water content is found in the upper dermis, where the capillary bed is the richest. Ultrasonographic findings also show an accumulation of water in the upper dermis after prolonged venous overload from the gravitational effects of dependency of the leg, and there is a reduction of water in the upper dermis after 2 hours of elevation. 6 Ultrasound examination can show localized indentation of the upper dermis by the fingernail or with a matchstick to a depth of 0.3 mm to indent and disperse the upper dermal interstitial fluid. Light massage with circular movements has the same effect, whereas deeper kneading massage shifts deep dermal water often like a deep bruise, bringing it to the upper dermal lymphatics.
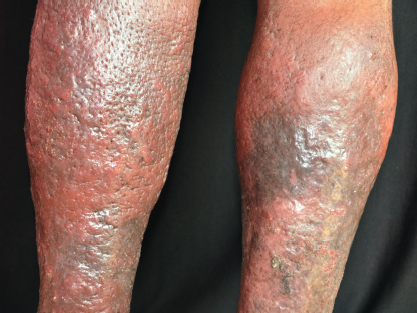
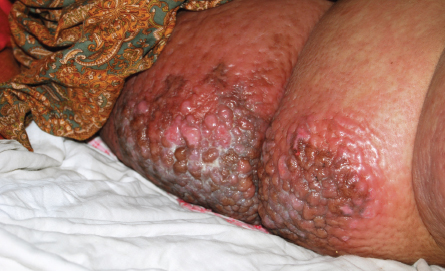
A great increase in water content, such as when the lymphatic system fails and cannot cope with venous overload, results in the expansion of the upper dermis, but adnexal components, such as the hair follicle, prevent such expansion in their immediate vicinity. It gives the appearance of orange peel, known as peau d’orange (Fig. 14-1). When fluid accumulation increases, such as in cellulitis caused by streptococcal infections of the regions of lymphedema, the hair follicles are unable to prevent further expansion of the dermis. As a result, lymphedema becomes painful, warm, and swollen, and the superficial skin becomes red. As the edema increases because of active infection, the peau d’orange appearance can be seen at the expanding edges of cellulitis while more central tissues are destroyed (Fig. 14-2).
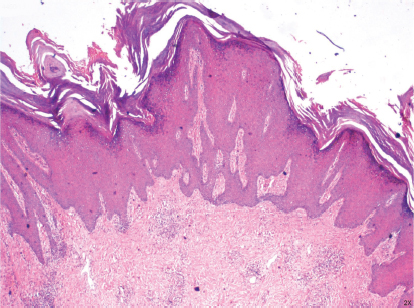
The epidermis and upper dermis are subject to morphologic findings ranging from a flat epidermis—such as in atrophy—to extreme outward projection of the papilla and inward projection of the epidermis, giving the picture of acanthosis or hyperplasia (Fig. 14-3). The capillaries in the dermal papillae elongate and coil. Mostly the initial lymphatics maintain their position at the junction of the upper dermis with the middermis.
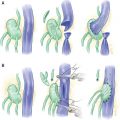
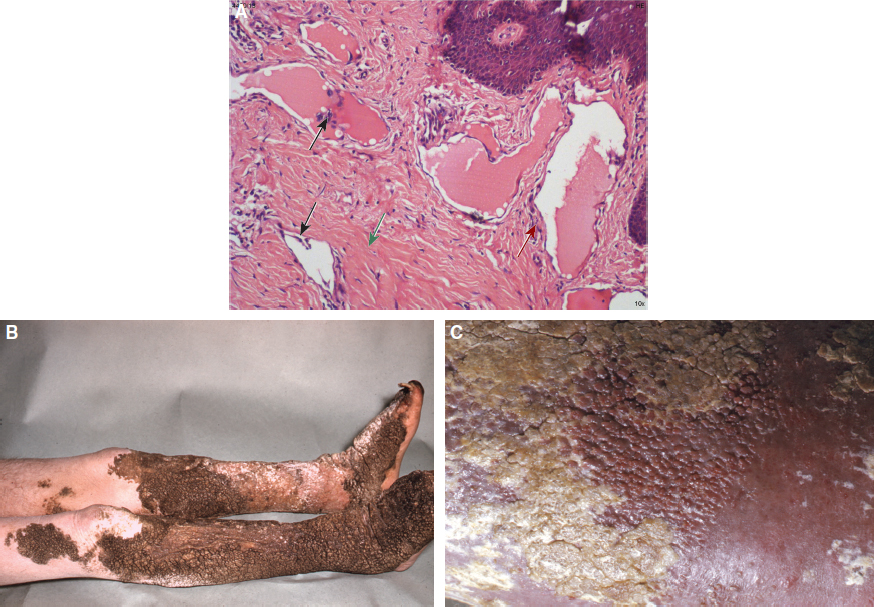
One of the features of lymphatic failure resulting from blockage of the collecting ducts into which they drain is that the initial lymphatics, which have only a single overlapping layer of endothelium in healthy individuals, develop smooth muscle, and the intralymphatic pressure rises as contractions become stronger (Fig. 14-4, A). One effect of this raised intralymphatic capillary pressure is to encourage the lymphatics undergoing lymphangiogenesis to penetrate higher in the upper dermis and into the widened papilla. As this becomes a dominant feature, the papilla extends closer to the surface, and the dilated lymphatic may reach the surface (Fig. 14-4, B). The entire papillae may resemble small intestinal villi (Fig. 14-4, C). Capillaries and lymphatics extend to the peak of each villus or present as vesicular fluid-filled lymphatics (see Fig. 14-6). Histologically there may be a smooth muscle–lined deep cyst into which the lymphatics drain and receive their lymph under high pressure. 7
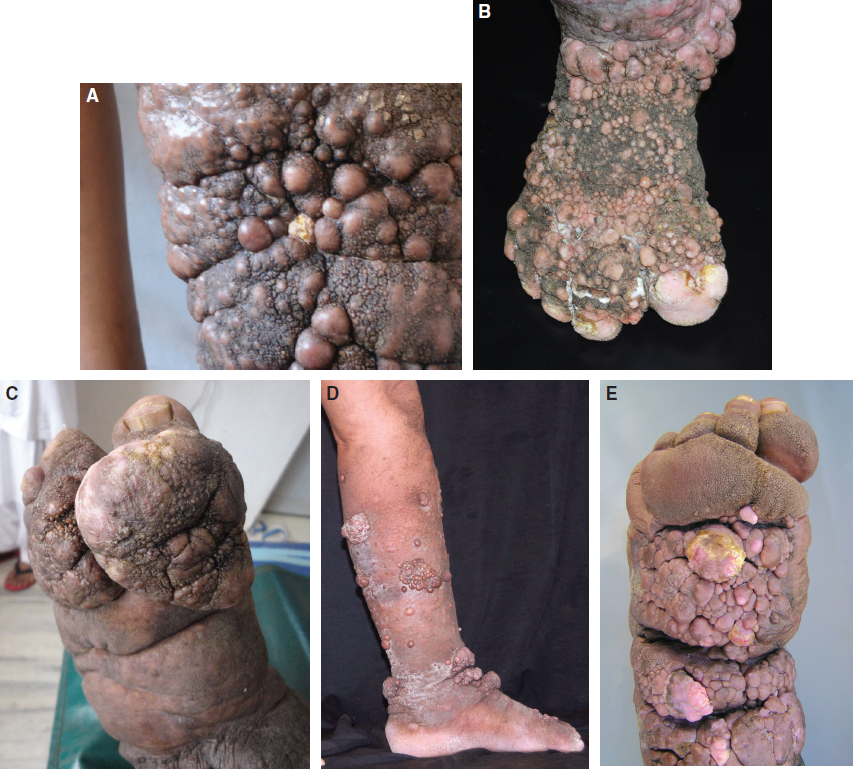
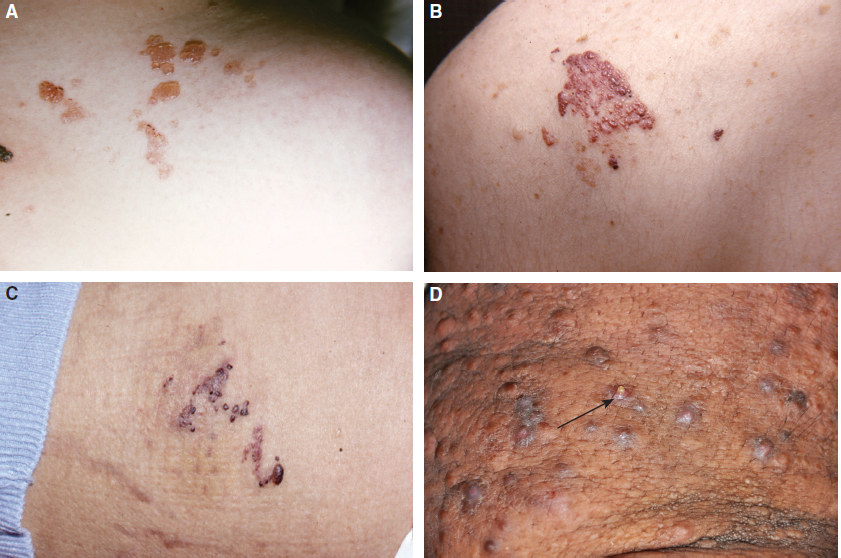
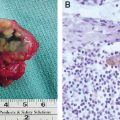
The variations in the dimensions of the polyplike protrusions can be observed in Fig. 14-5. The cobblestone-like nodules are often referred to as elephantiasis nostras verrucosa. 8 Originally the Latin term for “ours,” nostras, referred to belonging to “our region,” indicating its typically tropical prevalence.
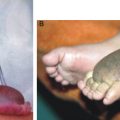
The socalled mossy foot is now also used to describe podoconiosis, which is caused by damage to the tissues and lymph nodes by an alkaline colloid of silica from the soil penetrating the skin in individuals who walk barefoot; the condition is commonly observed in Ethiopia. 9 Mossy foot, which is also described in Aboriginal Australians, usually begins around the toes. Gradually there is accompanying hypertrophy, and deep crevasses become entry points for bacteria and soil irritants. Lymph leaks and wets the surface of the skin, causing maceration, and secondary infection by bacteria and fungi occurs. The production of excess collagen gives rise to increasingly larger protuberances in which the lymphatics are sometimes hugely dilated. The condition is reported in all cases of lymphedema and occurs as a result of chronicity and repeated secondary infection of the area.
Lymphangioma Circumscriptum
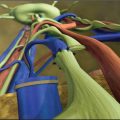
Dilated lymphatics often penetrate the papilla and epidermis to reach the surface of the skin. They develop contractile smooth muscle and loss of valves. Whimster 7 found that these contractile lymphatics often drain into large high-pressure cystic dilations of the collecting lymphatics. The color of the superficial vesicular lymphatics depends on the number of red cells, or they can be milky white from chyle (Fig. 14-6). The term chylous reflux describes a backflow of chyle from its normal route from the bowel through the cisterna chyli and thoracic duct to reach the bloodstream in the great veins of the thorax. The clinical presentations include small blisters containing chyle-chylous vesicles, which may appear on the skin in the lower parts of the body and discharge milky fluid, thus forming one type of chylous fistula. Chylometrorrhagia causes vaginal discharge of chyle. Chyle may collect in the serous cavities of the body—producing chylothorax, chylous ascites, and chylocele. 10
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree