Introduction
Breast or chest surgery, specifically either augmentation mammaplasty or mastectomy/chest reconstruction, are commonly requested procedures in the transgender and gender diverse population. The overarching goal of such surgeries is to alleviate symptoms of gender dysphoria and to allow individuals to live as their true selves. Individual goals vary between patients. In some individuals, breast or chest surgery is the only desired procedure, while in others, such surgery is one of many steps in their transition. From a technical perspective, the goals of surgery include a successful cosmetic and functional result with minimal complications.
In caring for the transgender individual, the surgeon functions as part of the multidisciplinary health-care team that may include mental health professionals, primary care providers, endocrinologists, and midlevel practitioners. It is the responsibility of the operating surgeon to understand the diagnosis that has led to the recommendation for surgery, medical comorbidities that may impact the surgical outcome, the effects of hormonal therapy (when applicable) on the patient’s health, and the patient’s ultimate satisfaction with the surgical result. Furthermore, the surgeon should assist with the coordination of the patient’s postoperative care in order to assure continuity.
Surgeons performing breast and chest surgery should also be familiar with the World Professional Association for Transgender Health’s (WPATH) Standards of Care (SOC). As previously mentioned, these guidelines offer a flexible framework to aid with providing care to transgender and gender diverse individuals. While procedures such as augmentation mammaplasty and chest surgery are not as invasive as genital surgery, care should nonetheless be taken to assure that individuals pursuing such surgery are appropriate candidates.
The SOC recommend that individuals who request breast or chest surgery have one referral letter from a mental health provider. In addition, input from a patient’s primary care doctor, or in some cases, endocrinologist, is useful in confirming that an individual is medically fit for surgery. The surgeon should, when needed, communicate directly with members of the health-care team, especially if there are any questions regarding a patient’s appropriateness for surgery. The SOC recommend the following criterion for individuals who desire breast or chest surgery :
- 1.
Persistent, well-documented gender dysphoria;
- 2.
Capacity to make a fully informed decision and to consent for treatment;
- 3.
Age of majority in a given country (if younger, additional recommendations apply);
- 4.
If significant medical or mental health concerns are present, they must be reasonably well-controlled.
Hormone therapy is not required for mastectomy/chest reconstruction surgery. Although hormone therapy is not specifically required for augmentation mammaplasty, it is recommended that individuals requesting such surgery undergo at least 12 months of feminizing hormone therapy prior to surgery in order to maximize breast growth to improve the aesthetic results of surgery.
If an individual is an appropriate candidate for surgery, a surgical consultation should be obtained. During the consultation, the surgeon should discuss the available surgical techniques, the advantages and disadvantages of each technique, the limitations of the procedure, and the risks and possible complications of various techniques. Furthermore, the surgeon should review the postoperative course and discuss the individual’s expectations from surgery. Patients who have unrealistic expectations risk disappointment with their final results.
If an individual decides to proceed with surgery, written documentation of informed consent should be included in the patient’s chart.
Augmentation Mammaplasty, Techniques, and Considerations
Breast development and hormone therapy
Development of the breasts during the prenatal stage of life is independent of sex hormones and is, therefore, the same in males and females. During embryonic development, breast buds composed of networks of tubules develop from the ectoderm. In females, these tubules will eventually become the matured milk ducts. Until puberty, the tubule networks of the breast buds remain quiet. At puberty, male and female breast development diverges. In females, high levels of estrogen and progestins, in conjunction with growth hormone and insulin-like growth factor-1, result in growth and maturation of the tubules into the ductal system of the breasts. Estrogens are generally believed to induce breast proliferation whereas progestins result in differentiation. Progestins are not thought to have a significant role in breast volume. In contrast, in puberty of males, androgens (testosterone and dihydrotestosterone) increase about 10-fold higher compared to females, and estrogen is approximately 10-fold lower compared to females. The high levels of androgens strongly suppress the action of estrogen in the breast at puberty, resulting in lack of breast development in men.
The suppression of androgens and supplementation with estrogens can lead to breast growth in transwomen. Androgen blockade can be achieved with antiandrogens. Spironolactone is most commonly used in the United States, whereas cyproterone acetate is widely used in Europe. A major difference between the agents is that cyproterone also has progestogenic properties. As previously mentioned, it is not approved for use in the United States due to concerns of hepatotoxicity. Some centers use gonadotropin-releasing hormone analogs to suppress androgen production, but cost limits the use of these agents. Alternatively, orchiectomy is an effective means to decrease androgen levels.
Breast size typically begins to increase 2 to 3 months after the initiation of hormone therapy. Initially, tender breast buds begin to form and breast growth progresses over 2 years. For this reason, the SOC recommend hormone therapy for at least 1 year prior to breast augmentation. Response to therapy varies among individuals, but breast and nipple development in transwomen is rarely as complete as it is in cisgender women. Few studies have addressed the optimal hormone regimen to maximize breast growth in transwomen. While studies have demonstrated the efficacy of various hormone therapies, reported data are observational and subjective. The majority of available literature does not suggest that estrogen type or dose affects the final breast size in transwomen. In addition, current data do not provide evidence that progestins enhance breast growth. Some, but not all authors suggest that younger age, tissue sensitivity, and body weight may impact breast size. Furthermore, shoulder width may play a role in perceived breast size and adequacy of growth. Overall, data do suggest that final breast size with hormone therapy is unsatisfactory in many transwomen; 60% to 70% seek surgical breast augmentation.
Patients should be counseled on the degree of breast growth they may expect from hormone therapy and the appropriate options should they desire larger breasts. Some transwomen have unfortunately resorted to “pumping,” an illegal and dangerous practice of injecting liquid silicone into breast tissue to enhance breast size. Serious complications of pumping range from local inflammatory reactions to pulmonary embolism and death. Still, because it is a cheap alternative compared to approved treatments, this potential deadly practice continues.
Augmentation mammaplasty
Many transwomen who report inadequate breast growth with hormone therapy continue to wear external prostheses or padded bras. As such, augmentation mammaplasty may be requested. Breast augmentation can be performed at the same time as vaginoplasty; this can help decrease surgery time and cost in individuals who desire both procedures. In a retrospective survey of 107 transwomen, Kanhai et al. reported that 80% of participants had mammaplasty and vaginoplasty simultaneously. The percentage of patients undergoing both procedures at the same time is likely far lower and variable between clinical practices.
Anatomic differences between the male and female chest are relevant to implant selection, incision choice, and pocket location. The cis male chest is not only wider than the cis female chest, but the pectoralis major muscle is usually more developed. Furthermore, the cis male areola is smaller than the cis female areola, the distance between the nipple and inframammary crease is less, and there is less ptosis in the breasts of transmen, even after hormonal therapy ( Figs. 9.1 A, B and 9.2 A, B ).
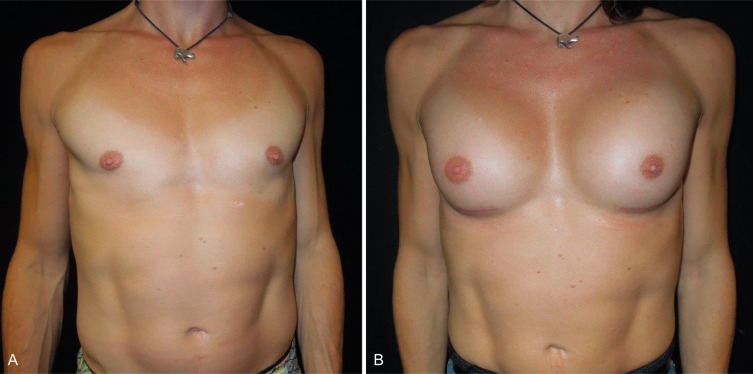
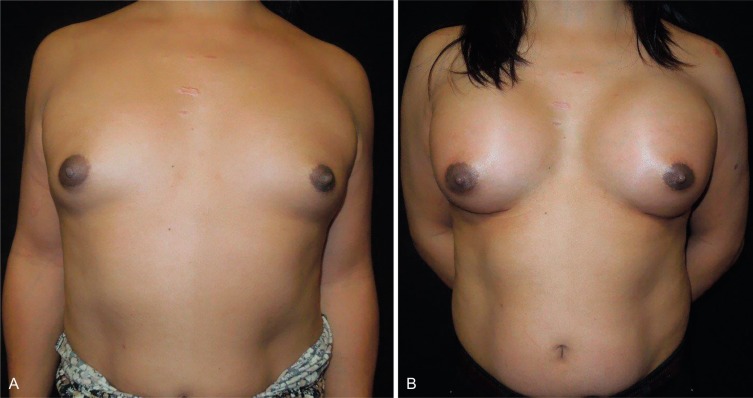
While the principles of augmentation mammaplasty in transwomen are similar to that of cis women, the broader chest, larger pectoralis muscle, and shorter distance between the nipple and inframammary crease warrant additional consideration. These anatomic characteristics may require lowering the inframammary crease and releasing the lower sternal attachments of the pectoralis major muscle ( Fig. 9.3 ). When releasing the sternal attachments of the pectoralis muscle, the overlying pectoralis fascia is left intact. These maneuvers may assist with implant positioning relative to the position of the nipple-areola complex, and help to prevent lateral implant displacement. Due to the wider chest wall diameter in transmen, a wide interbreast width is common, even with the selection of larger implants.
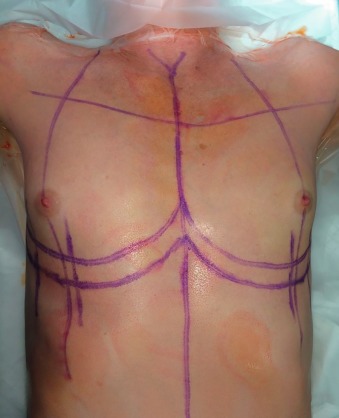
The implants may be placed in either a subglandular or subpectoral pocket. This decision depends upon the degree of breast growth in response to hormonal therapy. Subglandular implants may be more palpable and may have higher rates of capsular contracture due to less soft tissue coverage overlying the implant. However, subpectoral implants may be more prone to displacement due to the activity of the overlying pectoralis major muscle. Overall, the subpectoral position remains the most common pocket location.
In terms of incisions, transaxillary, periareolar, or inframammary crease approaches may be used. The choice of incision is tailored to the requests and the anatomy of the individual. Due to the smaller size of the male areola and the use of larger implants, an inframammary crease approach is most commonly chosen. Trans axillary incisions are sometimes used, whereas periareolar incisions are infrequently utilized. With the increased use of form-stable implants, larger incisions are often required, which also favor an inframammary crease approach.
While both saline and silicone implants are available, recently, the authors have favored form-stable implants placed in a subpectoral pocket through an inframammary crease incision. In the authors’ opinion, this approach allows the surgeon to most effectively lower the inframammary crease, centralize the implant underneath the nipple-areola complex, and release the pectoralis major muscle.
Many transwomen prefer larger implants. Kanhai et al. reported that the average size of implants in transwomen nearly doubled in their practice from 165 mL in 1979 to 287 mL in 1996. In a long-term follow-up study of 107 patients, the authors reported that 25% of patients were unhappy with their mammaplasty. The most common reason for dissatisfaction was that that the breasts were too small. Further augmentation was reported in 19% of these patients.
In order to decrease the risk of venous thromboembolism (VTE), hormones are discontinued prior to surgery, and either fractionated or unfractionated heparin is administered subcutaneously upon induction of anesthesia. In our practice, estrogens are discontinued 2 weeks prior to surgery. Following surgery, a compression bra is worn for 3 weeks. The individual is also instructed to limit upper body exercise for the first several weeks following surgery to decrease the risk of implant displacement. Gentle breast massage is instituted approximately 7 to 10 days following surgery.
Third-party payer coverage
While there has been significant progress in third-party coverage for gender confirming procedures, many insurance providers continue to consider breast augmentation a “cosmetic” procedure and, therefore, do not provide benefits. However, the SOC point out that in some individuals, a “cosmetic” procedure can have a radical and permanent effect on their quality of life. In fact, research has suggested that gains in breast satisfaction, psychosocial well-being, and sexual well-being after breast augmentation in transgender individuals are statistically significant and clinically meaningful. Because insurance benefits vary, it is worthwhile to review benefits on a case-by-case basis to determine if augmentation mammaplasty is covered.
Mastectomy/Chest reconstruction, Techniques, and Considerations
Hormone therapy
Many transgender men desire masculinization with testosterone therapy. However, testosterone therapy is not a prerequisite for mastectomy/chest reconstruction surgery. Several formulations of testosterone are available and it is most commonly administered intramuscularly or topically. Dosage should be titrated to reach plasma concentrations of an adult man. Testosterone binds to androgen receptors throughout the body and can suppress ovarian production of estrogen and progesterone. Because testosterone is converted peripherally to estradiol by the aromatase enzyme, estradiol will often remain measurable in transmen.
Aside from growth of chest hair, testosterone therapy does not cause significant change in breast appearance. On a microscopic level, some changes have been observed. Evaluation of surgically removed breast tissue from 100 transmen who had received testosterone therapy for at least 6 months showed decreased glandular tissue and increased fibrous connective tissue in 93% of the pathologic samples. In addition, there was mild lobular atrophy and severe lobular atrophy in 86% and 7% of the tissue samples, respectively. Two fibroadenomas, 34 fibrocystic lesions, and no carcinomas were reported in this series.
Breast binding
Transgender individuals often use breast binding as a means to hide breast tissue. Breast binding involves using tight material to hold the breasts flat against the torso to allow them to be more easily hidden beneath clothing. Little is known about the long-term health effects, if any, of breast binding. However, breast binding over several years can decrease skin elasticity and quality, and, as a result, can affect the surgical technique and aesthetic results from mastectomy and chest reconstruction.
Mastectomy/chest reconstruction
Chest-wall contouring is an important surgical step for many transmen. For some transgender and gender diverse individuals, chest surgery is the only desired surgery to alleviate gender dysphoria while in others, chest surgery is one of many steps in transitioning. The goals of chest surgery include the aesthetic contouring of the chest by removing breast tissue and excess skin, reducing and repositioning the nipple-areola complex when necessary, releasing the inframammary crease, performing liposuction of the chest, and, when possible, minimizing chest scars and preserving nipple sensitivity.
Before chest surgery is performed, preoperative breast imaging (i.e., mammogram or ultrasound) may be considered depending upon patient age, personal and family history, and physical examination. The American Congress of Obstetricians and Gynecologists recommends annual mammograms beginning at age 40. Earlier and additional testing may be warranted in high-risk individuals.
Chest surgery in transmen may present an aesthetic challenge due to breast volume, breast ptosis, nipple-areola size and position, degree of skin excess, and potential loss of skin elasticity. Breast binding may necessitate significant amounts of skin removal. Several surgical methods are utilized, and the choice of technique depends upon the skin quality and elasticity, the degree of breast ptosis, and the position of the nipple-areola complex. In addition, preserving subcutaneous fat on the mastectomy skin flaps, preserving the pectoralis and serratus fascia, releasing the inframammary crease and sternal attachments, and contouring the lateral chest wall are also important components of chest surgery and chest wall contouring.
Small, nonptotic breasts can often be treated with periareolar incisions (“limited incision”). In these cases, the nipple may be reduced by a wedge resection of the lower pole, but the areola is not repositioned. A small amount of tissue is left beneath the nipple-areola to preserve viability ( Fig. 9.4 ). Circumareolar (“pursestring”) or vertical incisions with free nipple-areola grafts can be used for larger breasts with mild ptosis requiring smaller amounts of skin removal ( Fig. 9.5 ). Finally, traditional transverse inframammary crease incisions (“double incision”) with free nipple-areola grafts may better serve individuals with larger breast volumes and increased breast ptosis requiring large amounts of skin removal ( Fig. 9.6 A and B ). Nipple reduction is commonly employed, and often in conjunction with free nipple-areola grafts. In addition, liposuction is frequently used for discontiguous undermining of the inframammary crease and lateral chest wall. Generally, free nipple-areola grafts, as opposed to maintenance of the nipple-areola complex on a dermoglandular pedicle, are the preferred techniques for nipple transposition to prevent residual breast fullness.