Lower lid blepharoplasty surgery can be a challenging procedure for both the neophyte and the accomplished surgeon. It requires mastering complex periorbital anatomy and choosing the correct approach from a wide variety of patient presentations. This article spans the meticulous clinical evaluation, diagnostic approaches, and surgical techniques required to address challenging clinical scenarios of the lower eyelid, lid–cheek junction, and midface. By following these principles, surgeons can achieve excellent esthetic and functional results, even in the most challenging cases.
Key points
- •
Complex periorbital anatomy and diverse patient presentation make lower lid blepharoplasty particularly challenging.
- •
Thorough physical examination and special tests help provide an accurate diagnosis for surgical treatment.
- •
It is important to identify patient factors that increase risk and complexity of treatment.
- •
Perform the least invasive surgical option to address patient problems.
Introduction
Blepharoplasty is one of the most common elective surgical procedures in esthetic facial surgery. Complex periorbital anatomy, diverse presentations of periorbital aging, and significant functional and esthetic operative risks make lower blepharoplasty a particularly challenging procedure. Surgical approaches to lower blepharoplasty are quite varied and depend on both the patient-specific anatomy and the complexity or degree of facial aging. The surgical procedure chosen should be the simplest technical procedure that adequately addresses the underlying problem. Appropriate surgery may be as limited as isolated transconjunctival fat removal, for example, in patients with isolated lower lid fat, no excess skin, and good lid position and tone. Appropriate surgery may also be more complex, requiring a combination of fat repositioning, skin excision, lateral canthal suspension, and correction of tear trough, palpebral malar grooves, and malar mounds to fully address presenting pathology. A thorough and thoughtful physical examination should identify patients who will require a more complex surgical approach and those at higher risk for complications. Current trends seem to favor the transconjunctival approach for fat repositioning and correction of problems at the lid cheek junction, but a transcutaneous approach is often warranted when significant skin or orbicularis problems are present or when significant midface descent needs to be addressed. In addition, lower lid tightening is considered by many as a prerequisite to successful lower lid surgery in most cases.
Lower eyelid assessment
A thorough physical examination of the lower eyelid should include assessment of all 3 layers of the lower lid and the tarsoligamentous sling. , Proper examination will ensure correct diagnosis, identify patients at increased risk for complications, and facilitate appropriate surgical decision-making. Tepper and colleagues identified key preoperative findings that increase risk for lid malposition after lower blepharoplasty. These findings include negative vector, lid snap-back and distraction suggestive of horizontal lid laxity, lower lid scleral show, negative or neutral canthal tilt, and a distance from the lateral orbital rim to the lateral canthus of greater than 1 cm. Each will be discussed in detail later.
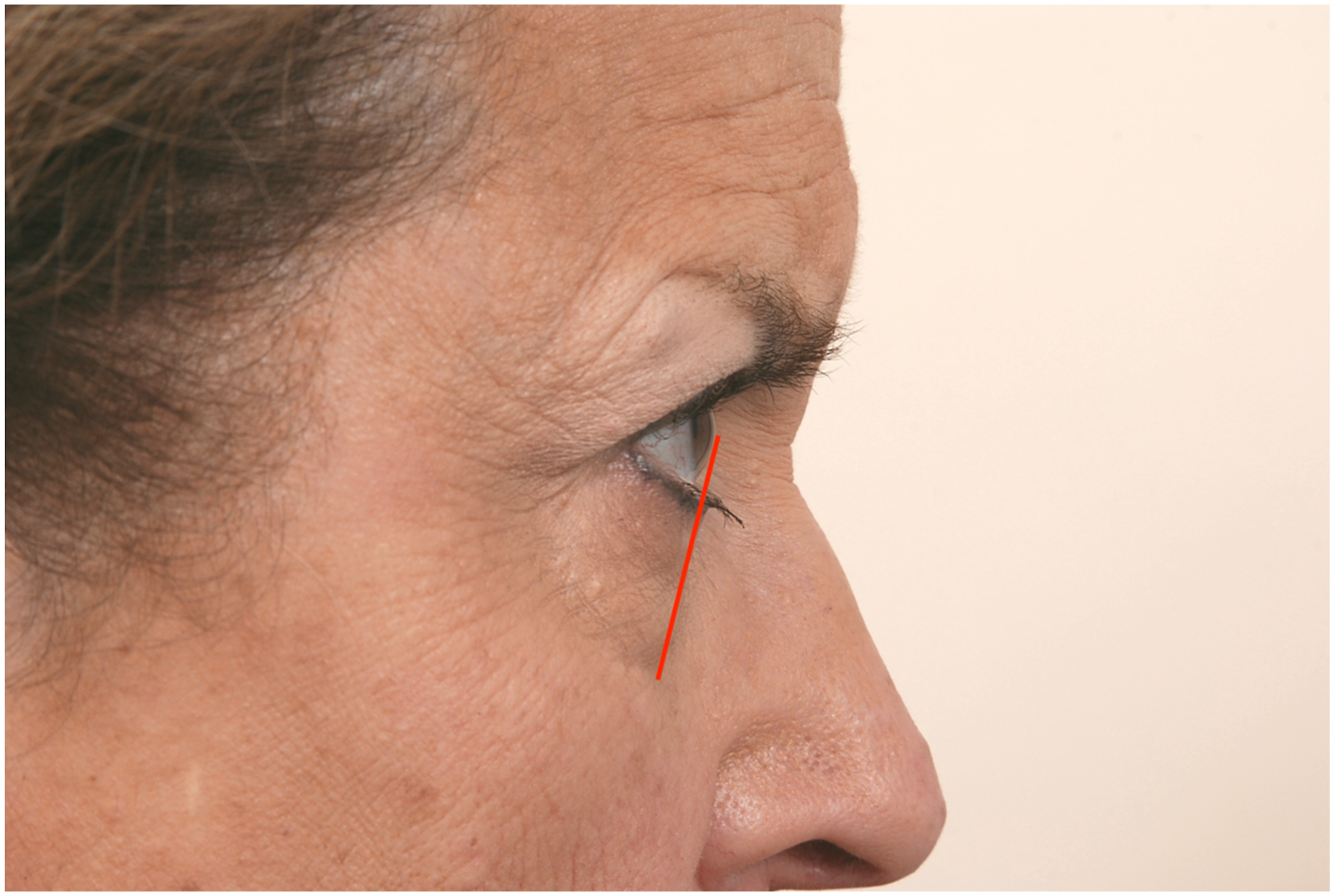
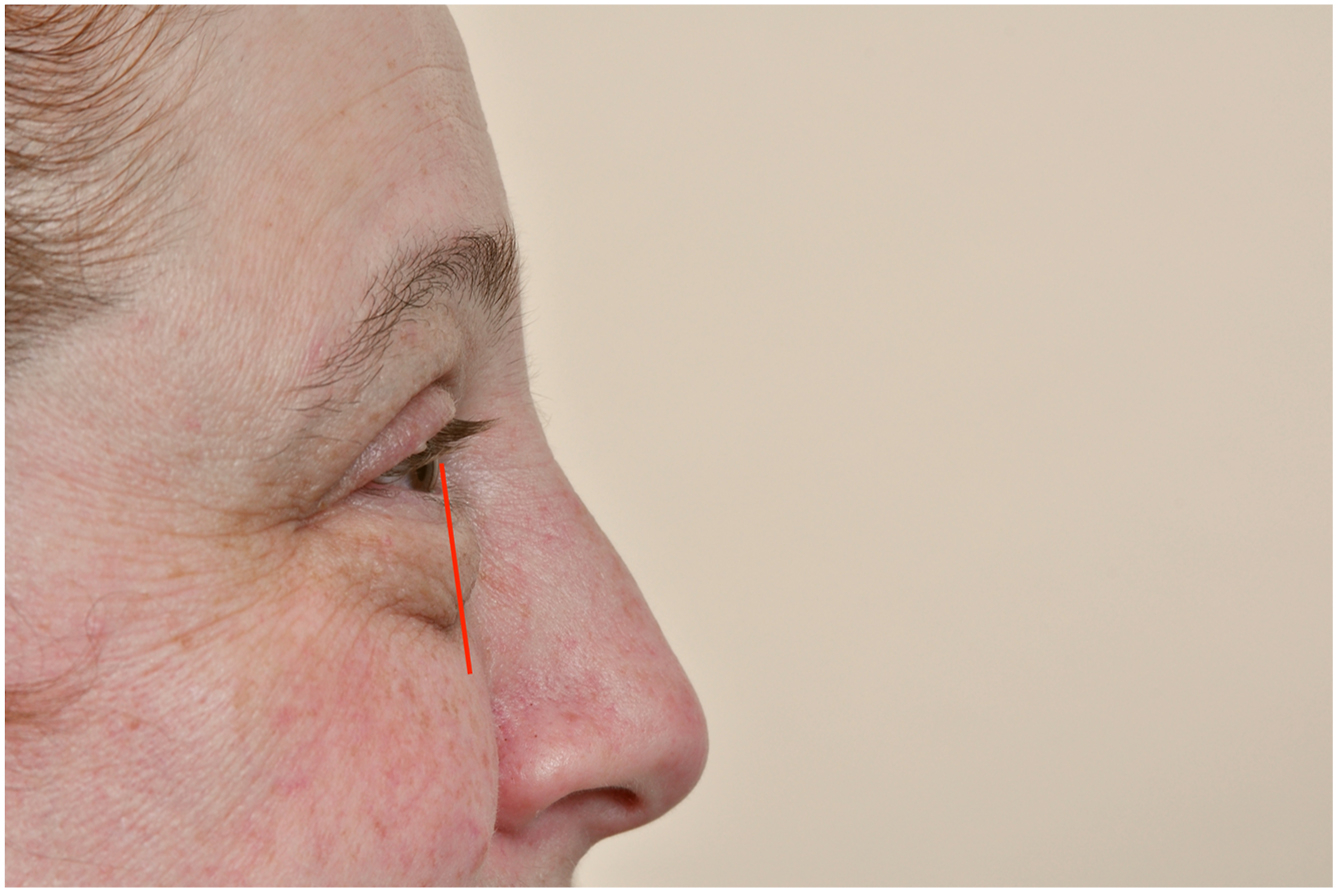
Vector analysis, performed on lateral view, is the comparison between the anterior projection of the globe with the anterior projection infraorbital rim. A negative vector describes globe projection more than that of the infraorbital rim ( Fig. 1 ). A positive vector describes globe projection less than that of the infraorbital rim ( Fig. 2 ). A neutral vector describes globe projection at approximately the same level as the infraorbital rim. Importantly, negative and neutral vector findings are correlated with an increased risk for soft tissue descent in the postoperative period and potential risk for lower lid malposition. Positive vectors reflect more supportive malar soft tissues and are protective against postoperative lid malposition.
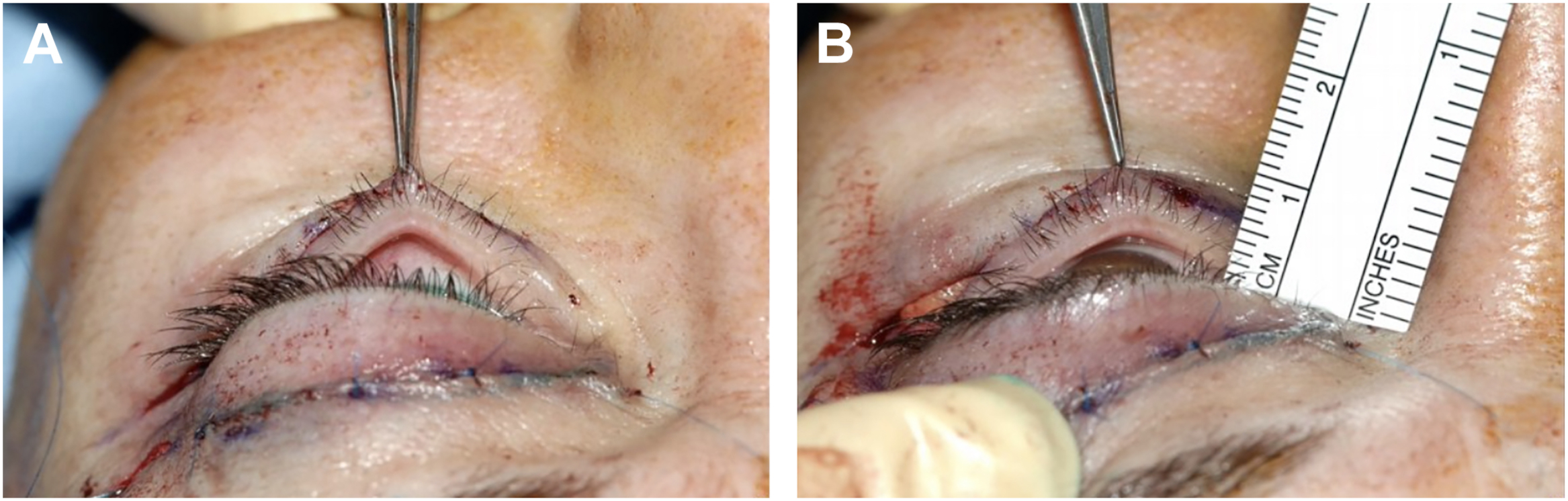
Lid margin laxity should be evaluated using snap-back and distraction tests as previously described. Patients with 6 mm or less of lid distraction can oftentimes be adequately treated with an isolated lateral canthopexy. Patients with greater than 6 mm of distraction will typically necessitate a canthal tightening procedure ( Fig. 3 ).
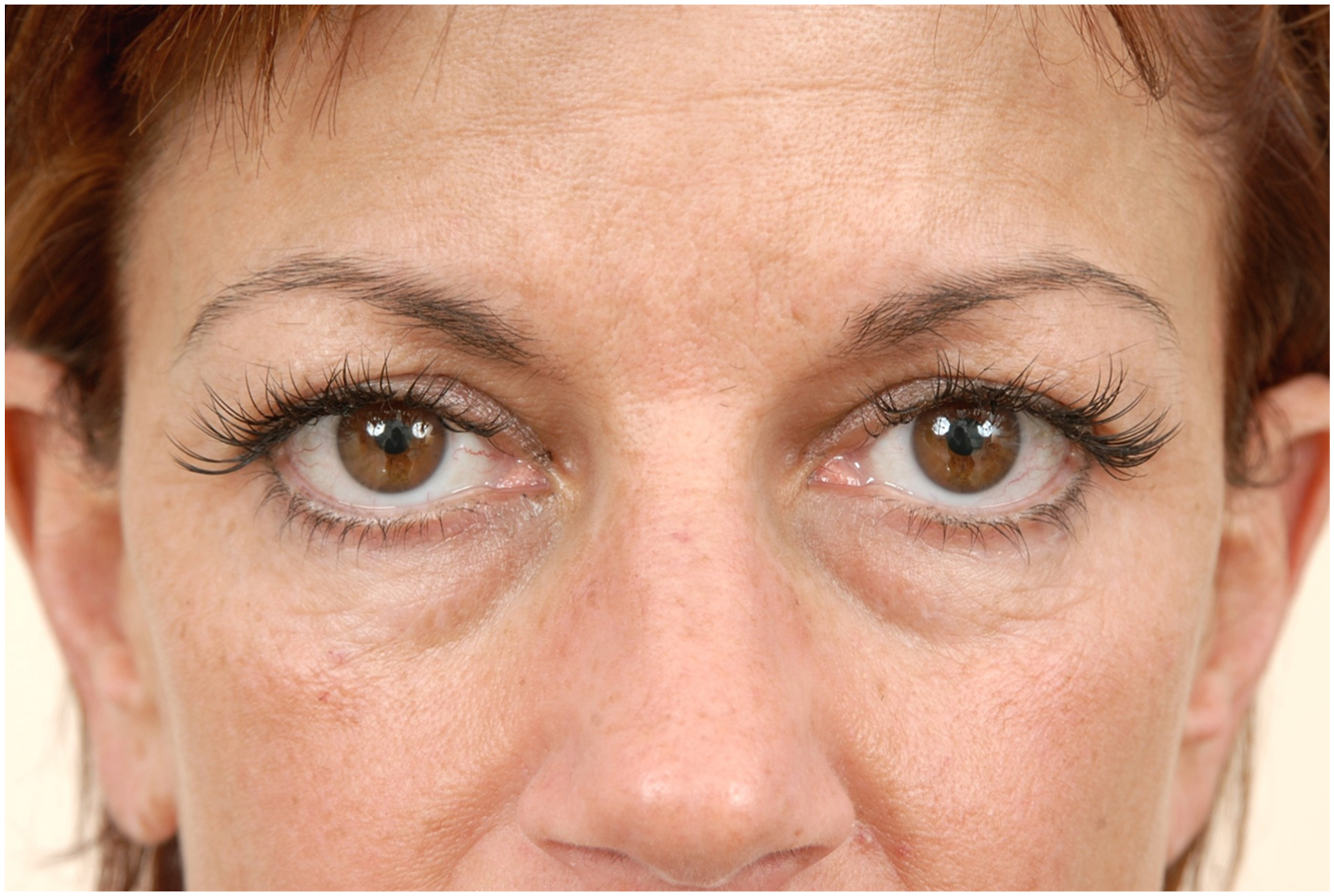
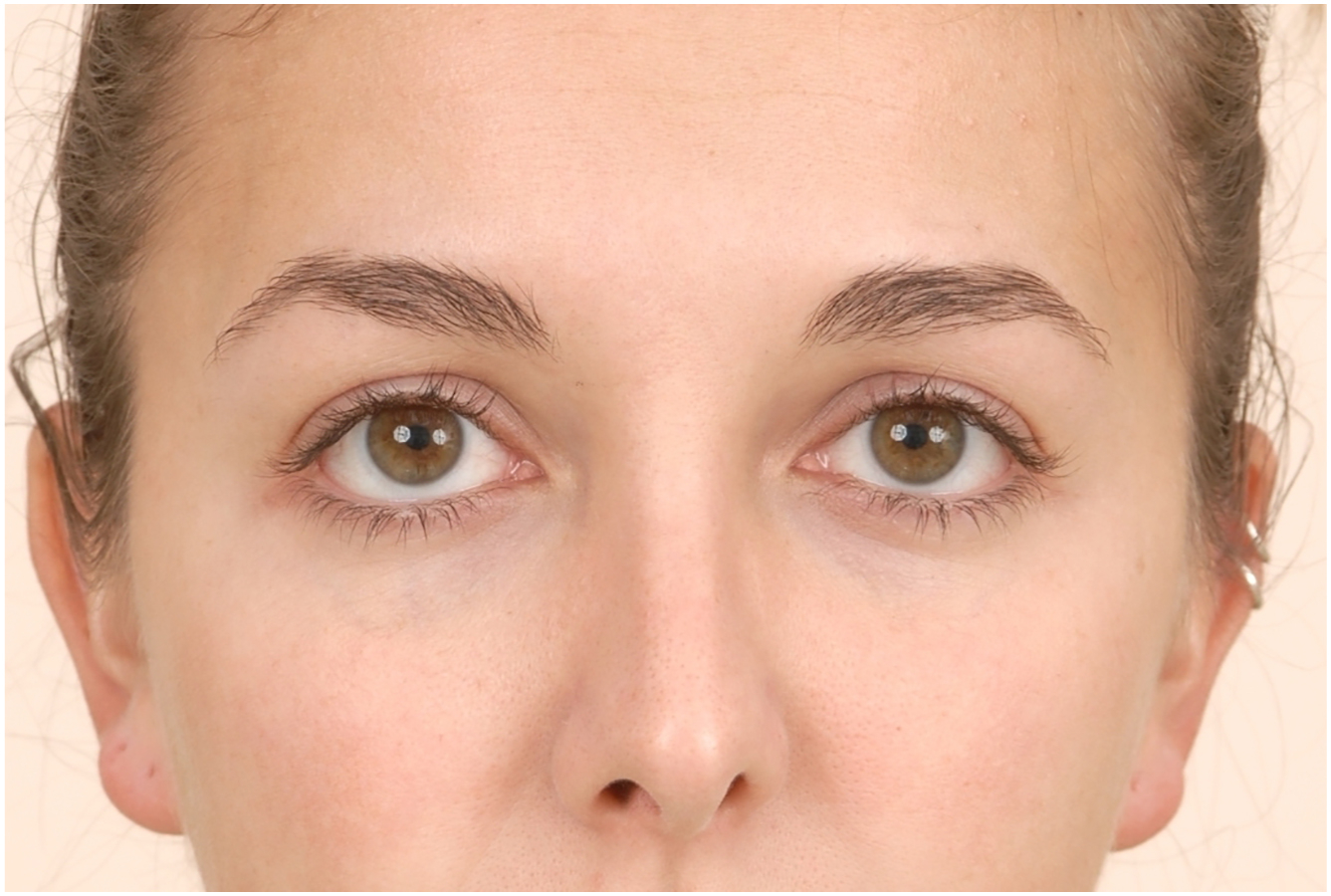
Scleral show is an objective finding describing visible sclera above the lower lid and below the inferior corneal scleral limbus. An esthetic lower lid should rest at the lower limbus without sclera show. Decreased lower lid tone is often associated with scleral show. The Margin to Reflex Distance 2 (MRD2) measures distance from the pupillary light reflex to the lower lid margin and thus similarly describes lower lid position relative to the lower scleral limbus. An esthetic, normal lower lid typically measures an MRD2 of approximately 5 mm ( Fig. 4 ). An MRD2 greater than 5 mm can also be an indicator of decreased lower lid tone. , ,
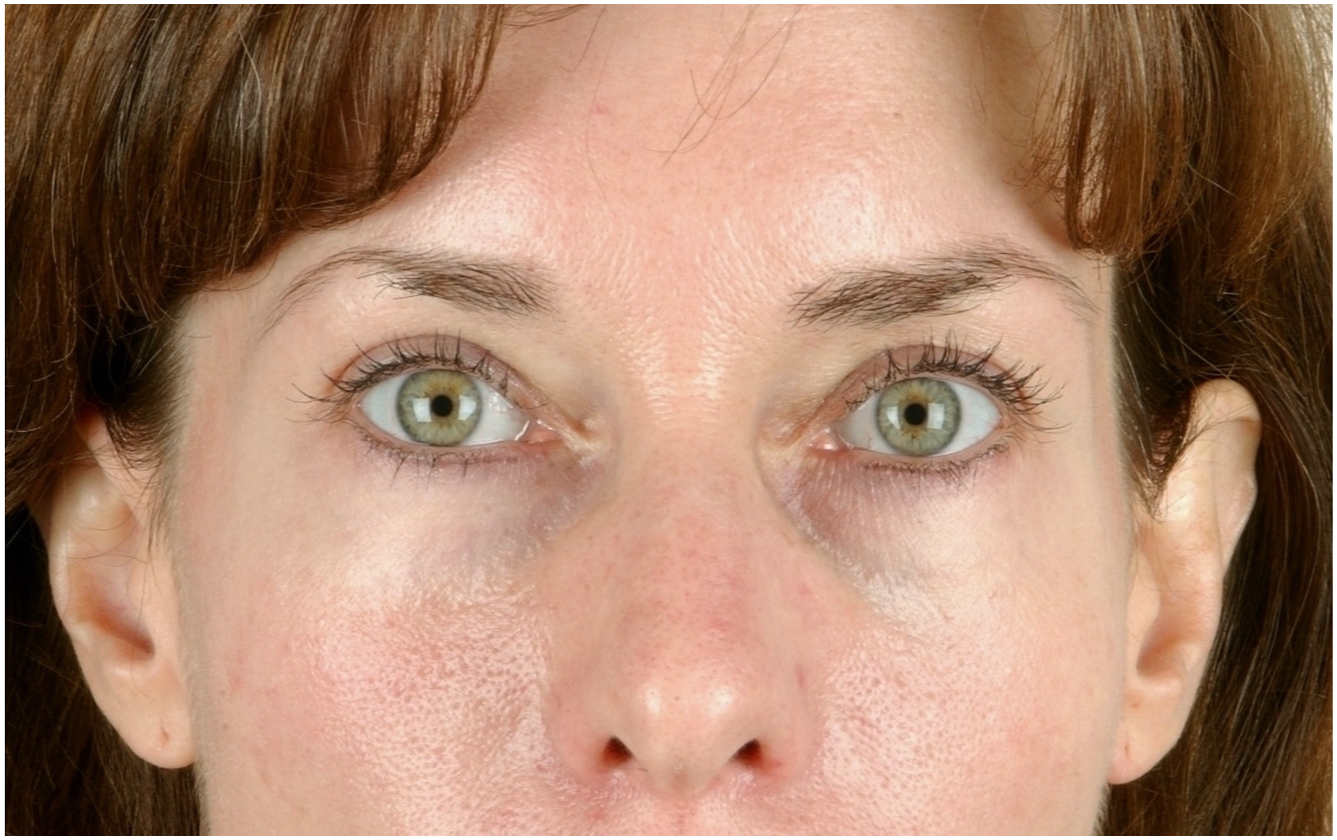
Canthal tilt describes the position of the medial canthus relative to that of the lateral canthus. Positive canthal tilt describes a lateral canthus that is positioned higher, or more cranial, than the medial canthus ( Fig. 5 ). Positive canthal tilt is considered favorable for lid support and prevention of postoperative lid malposition. Conversely, negative describes a lateral canthus that is positioned lower, or more caudal, than the medial canthus ( Fig. 6 ). Negative and neutral canthal tilts suggest suboptimal lid support.
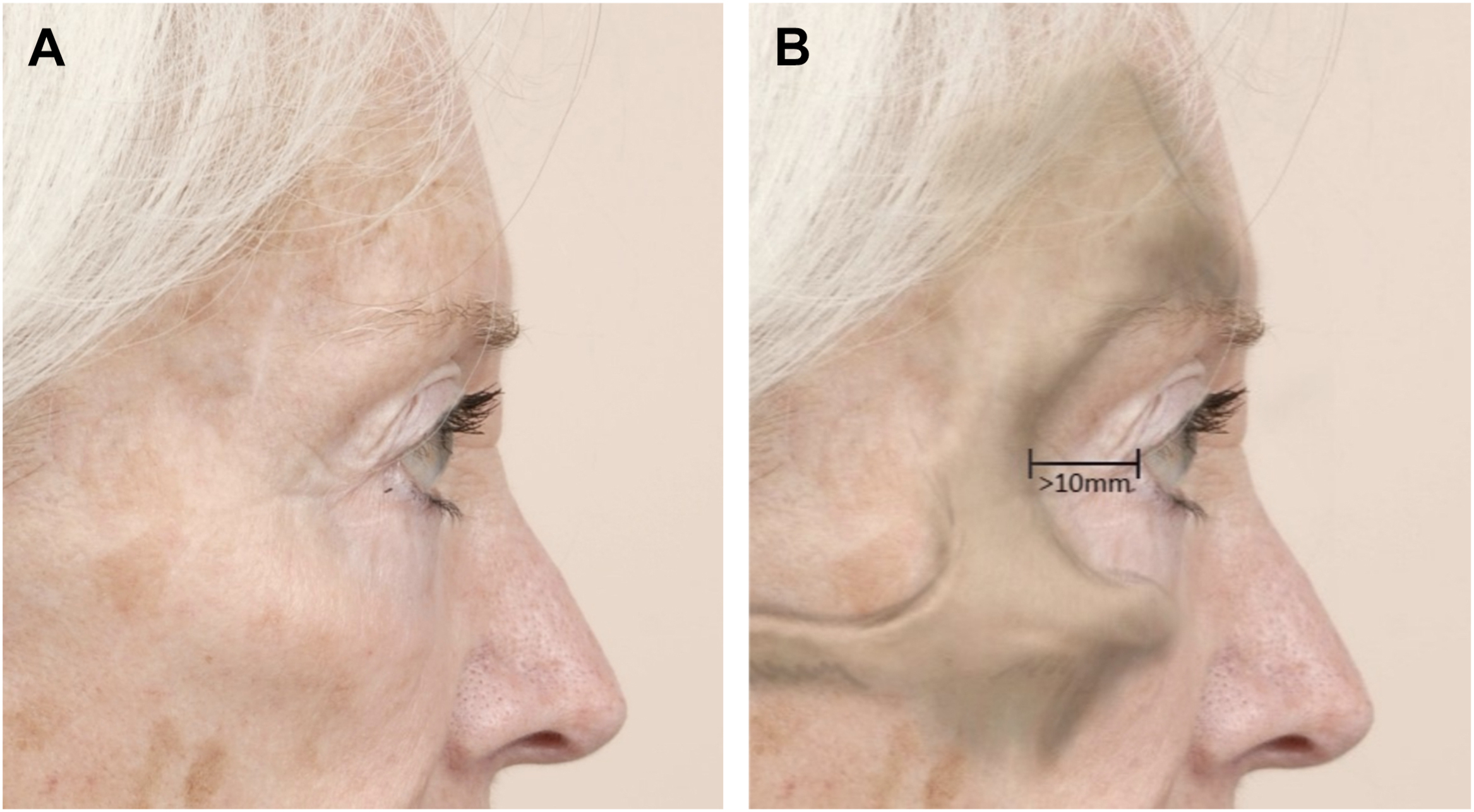
The lateral canthus to orbital rim distance should also be noted. Distances greater than 1 cm are associated with a higher risk for lid malposition and would benefit from therapeutic or prophylactic canthal tightening ( Fig. 7 ).
The 4 finger technique described by Patipa can be used to assess the extent of excessive lid laxity and the most appropriate surgical intervention to address it. This simple, yet effective, test as described by Patipa highlights the intimate relationship between the midface and the lower lid. This can be performed by using a series of steps outlined in the following:
- 1.
Place a single finger at the lateral canthus, then apply gentle traction both superiorly and laterally. If this successfully reestablishes the desired lower eyelid position, a lateral canthal tightening procedure is indicated. If malposition of the middle portion of the lower eyelid remains, proceed to step 2.
- 2.
Place a second finger at the central lower eyelid margin. If this successfully reestablishes the desired lower eyelid position, a spacer graft is also indicated to provide additional lower lid support and vertical lid elevation. If the malar fat pad remains descended with associated malar eminence flattening, proceed to step 3.
- 3.
Place a third finger over the malar eminence, then apply upward force. If this additional digit adequately repositions the cheek fat pad, pre-periosteal malar fat pad elevation is indicated in addition to the lateral canthal tightening and spacer graft. If the midface remains descended, proceed to step 4.
- 4.
Place a fourth finger over the cheek, then apply upward force. If this maneuver reestablishes the position of the lower lid and midface, subperiosteal midface elevation is indicated in addition to the lateral canthal tightening and spacer graft instead of the pre-periosteal malar fat pad elevation.
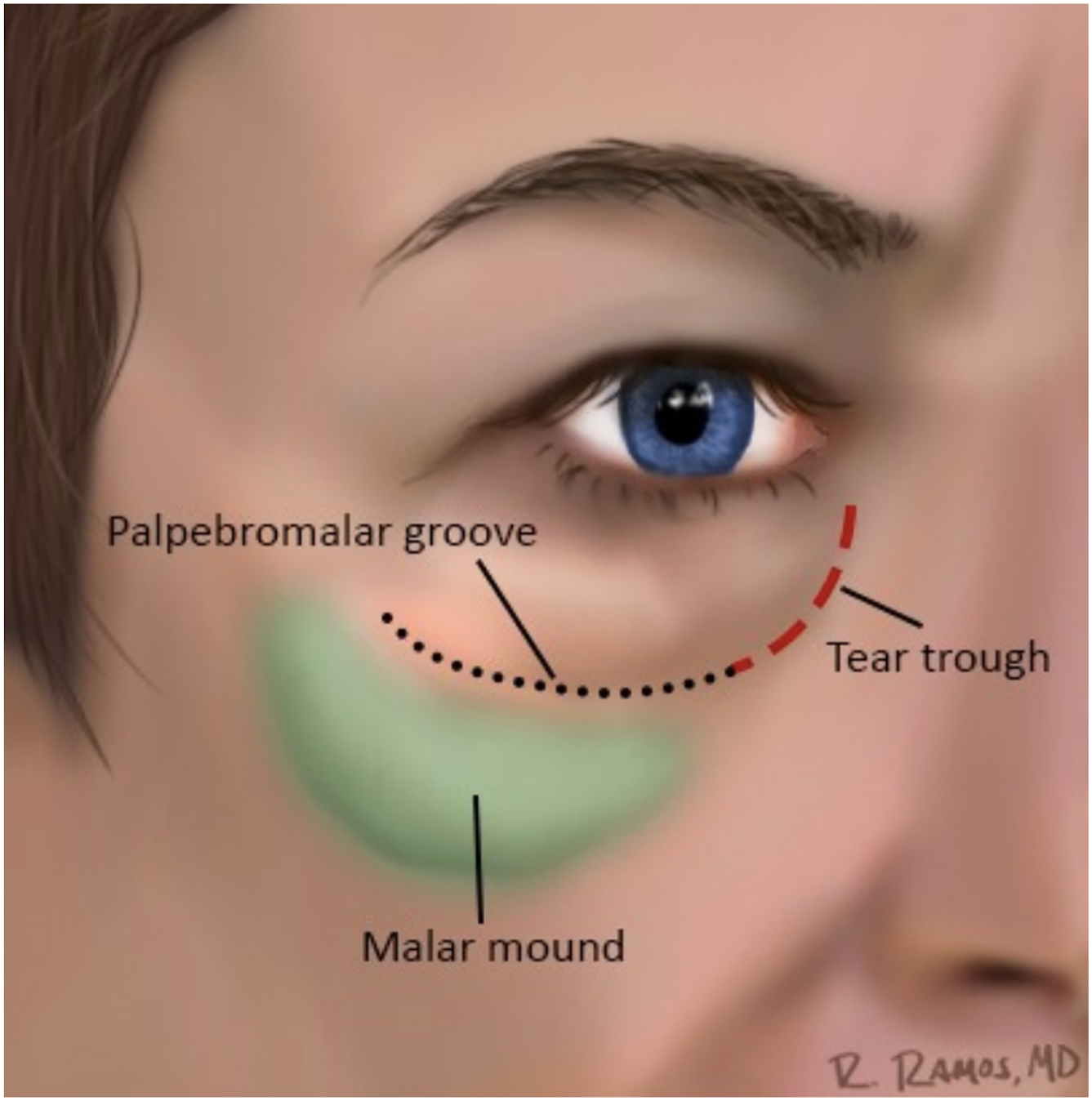
The lid–cheek junction also plays a crucial role in analysis of periorbital aging. A variety of terms have been used to describe similar findings in the lower lid area leading to confusion for the reader, as well as difficulty comparing the findings and surgical results in the literature. We suggest consistent anatomic descriptors of these lid–cheek junction aging problems as described in the anatomy study of this text. , It is important to accurately document the presence and severity of the lower lid–cheek junction deformities, including tear trough deformities, palpebromalar grooves, malar mounds, malar edema, and festoons ( Figs. 8 and 9 ). Further evaluation can be performed by utilizing the squinch test, pinch test, and the 4 finger test described earlier. ,