The lower lid cheek junction is a complex region. Patients are concerned about contour deformities of the lower eyelid and the cheek, but the causes of these issues are found in the underlying anatomy. Age-related bony changes result in a recessed infraorbital rim and a recessed maxilla. Loss of cheek soft tissue contributes to the formation of a tear trough deformity. Configuration of the tear trough comes in 3 classes, each of which requires a different surgical treatment. Combined procedures on the lower lid and the cheek often result in the most significant improvement.
Key points
- •
Patients present with concerns about visible contour deformities of the lower eyelid cheek junction.
- •
Surface deformities are are caused by the underlying anatomy which changes with with age.
- •
Surgical blending of the Lower Lid Cheek junction can be accomplished with lower eyelid surgery, with surgery of the anterior cheek, or a combination of the two.
- •
The tear trough deformity can be classifed into 3 categories, each of which requires a different surgical treatment.
- •
Lower eyelid surgery often requires additional measures to support lower lid position.
Video content accompanies this article at http://www.plasticsurgery.theclinics.com .
Introduction
Age-related changes at the junction of the lower eyelid and the cheek present a constellation of complex challenges for the aesthetic surgeon. In 1993, Flowers wrote: “Too much is done to the lower eyelid in plastic surgery…results, if honestly recorded are consistently deficient. Often, they are terrible”. This frank assessment of lower lid surgery was made at a time when our understanding of the anatomy of the lower lid cheek junction was limited. While we have learned a great deal in the ensuing 30 years, these comments still have an element of truth today.
It is the visible contour deformities of surface anatomy that concern our patients. The surgeon’s task is to ascertain the underlying anatomy behind the surface changes and determine the advisability of a surgical correction. In the attractive, youthful lower lid cheek junction there is a smooth transition from lid to cheek without any bulges or depressions. Surgical procedures to rejuvenate the aging lower lid cheek junction include skeletal augmentation and the manipulation of orbital and cheek fat by removal, addition, or by fat repositioning. In all cases, care must be taken to preserve the normal function and position of the lower eyelid, a critical, but delicate structure. Measures to maintain lower lid position and function are a necessary part of surgery in this anatomic area.
Surface contour of the lid cheek junction
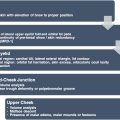
For the purposes of this article, the lid-cheek junction is defined as the slight groove or surface depression between the lower lid and the cheek. Often, but not always, this coincides with the junction of thin lower eyelid skin with the thicker skin of the cheek. In young patients this depression frequently overlies the infraorbital rim, the but in older patients it can be found slightly lower.
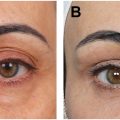
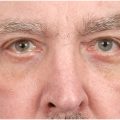
In the attractive lower lid complex, there is a smooth transition from lower lid to the cheek with a minimal depression defining the lid cheek junction. There is no bulging in the lower lid itself and there is minimal laxity of lower eyelid skin. The lower lid height (measured from the lower lid cheek junction to the eyelid margin) is relatively short in vertical height. ( Fig. 1 ).
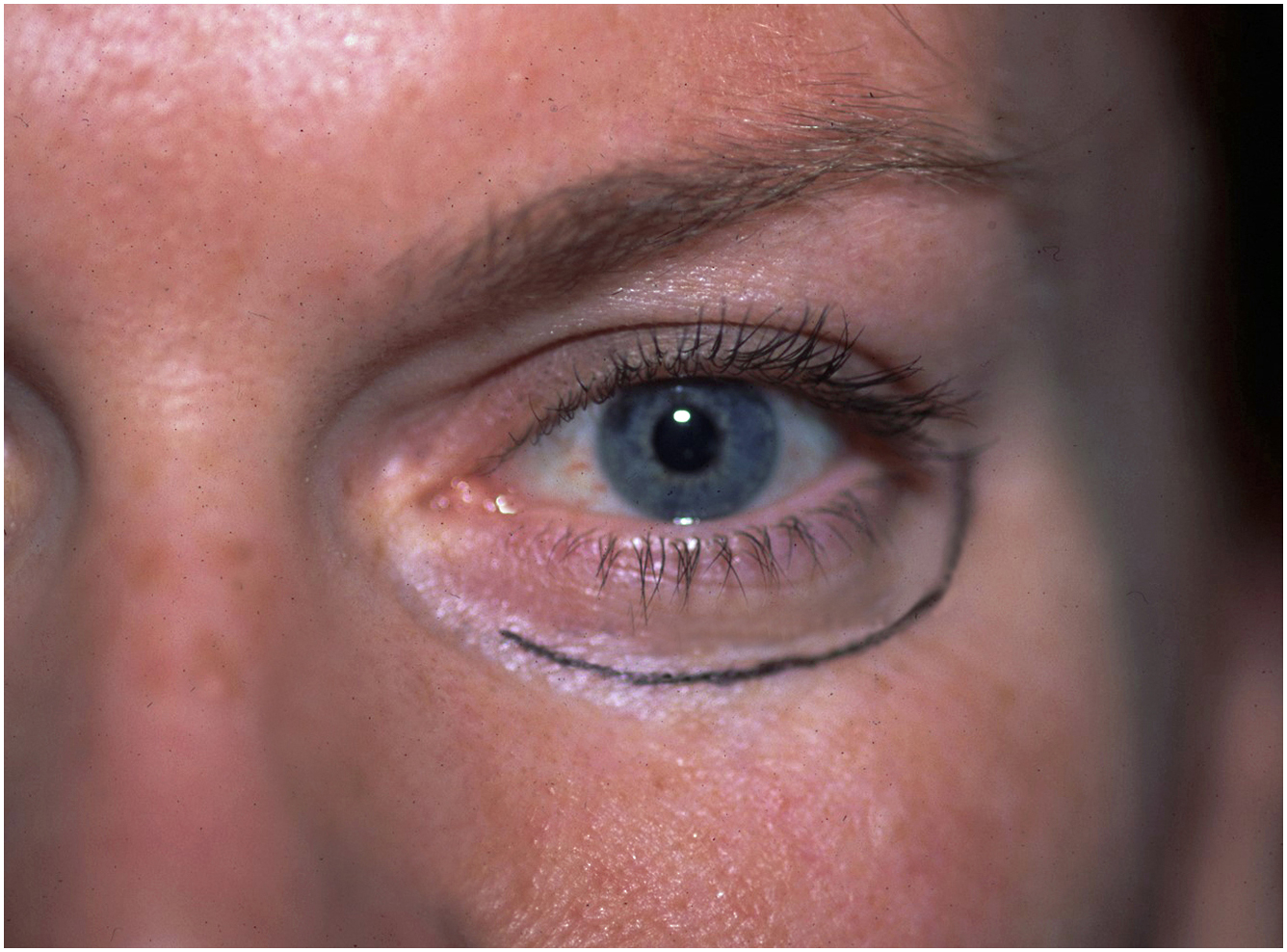
Patients presenting for treatment of this area are concerned about the loss of youthful looking surface anatomy. Their typical concerns are the visible bulging of lower eyelids, the groove below this bulging (perceived as a “dark circle”) and laxity of overlying skin, especially in animation ( Fig. 2 ).
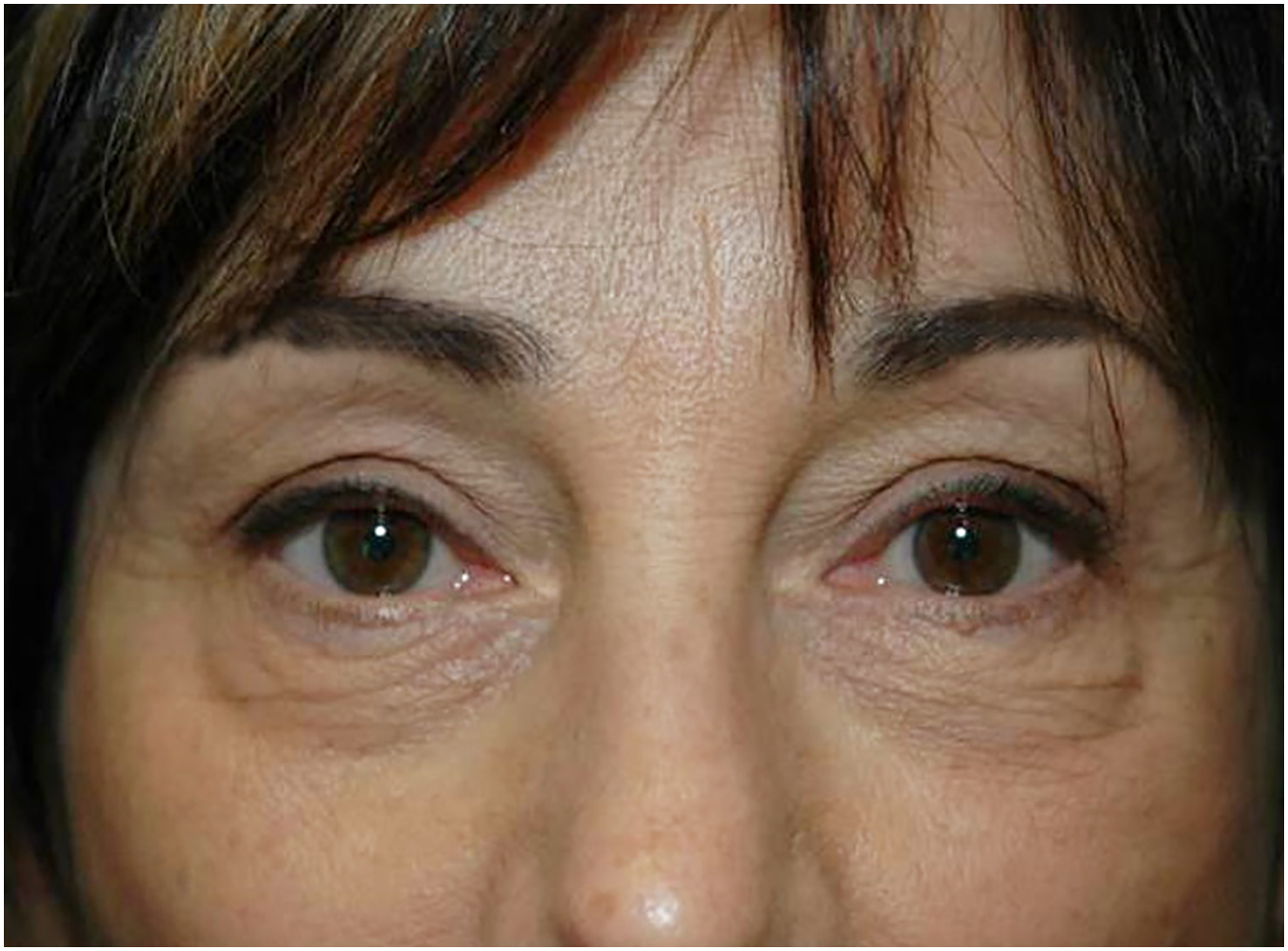
In addition to the appearance of the lower eyelid itself, the surface contour of the mid-face is one of the keys to facial attractiveness. In young adults, when round and full, the anterior cheek contour imparts an appearance of attractiveness and health. If the cheeks are depressed and deflated, the appearance can be unhealthy and unattractive, regardless of age.
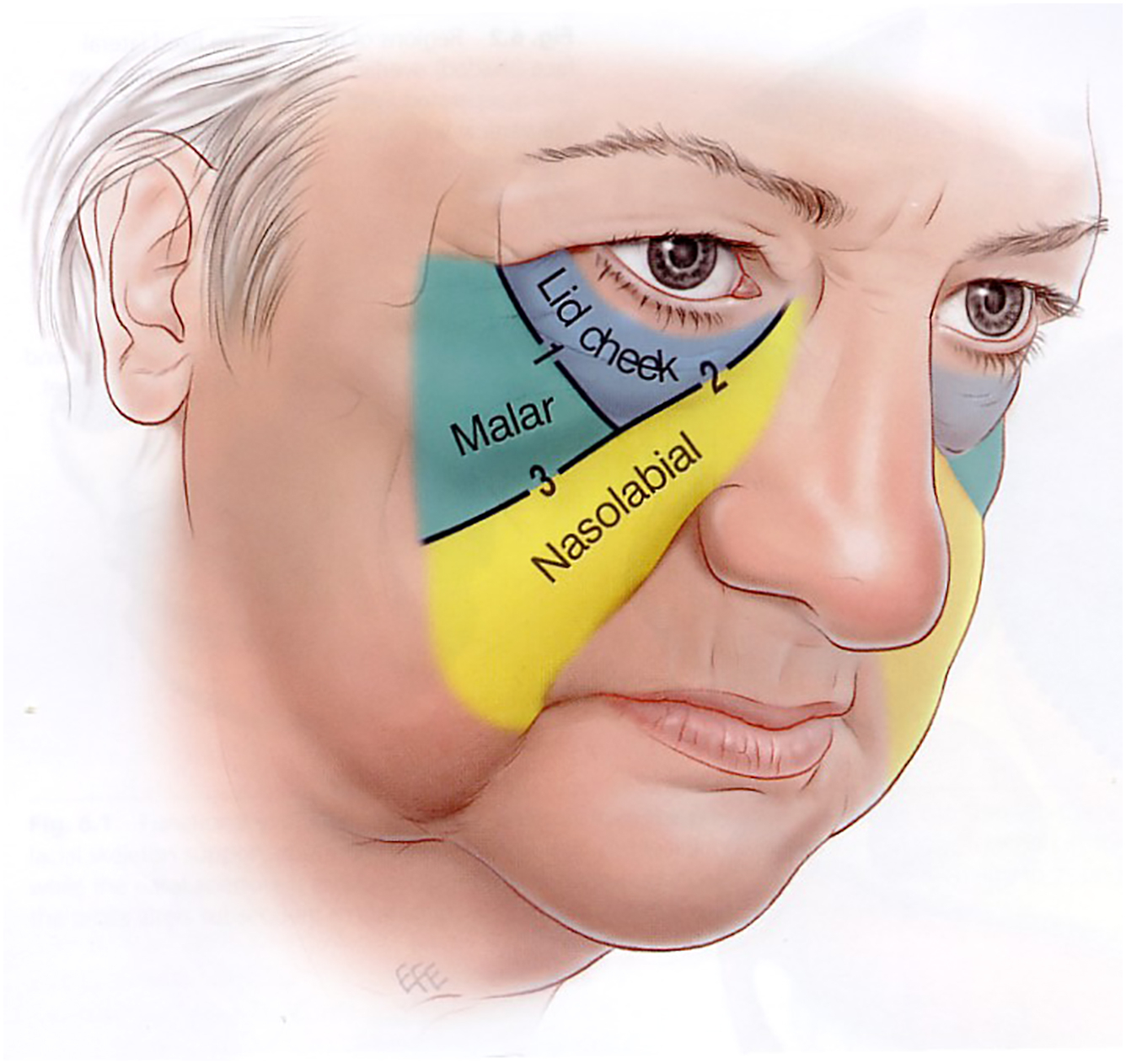
With age, we have learned that the fullness, projection, and shape of the anterior cheek undergo visible changes. In 2020, Lambros showed that the aging lid cheek junction deepens, but does not descend appreciably. Extending from the lid cheek junction a “mid face groove” develops, angling obliquely across the cheek coursing inferolateral. Mendelson has demonstrated that this groove is defined by the obliquely running zygomatic cutaneous ligaments ( Fig. 3 ). Considerable anatomic work has been done, demonstrating that visible changes on the surface are explained by changes in the underlying anatomy.
Anatomic changes
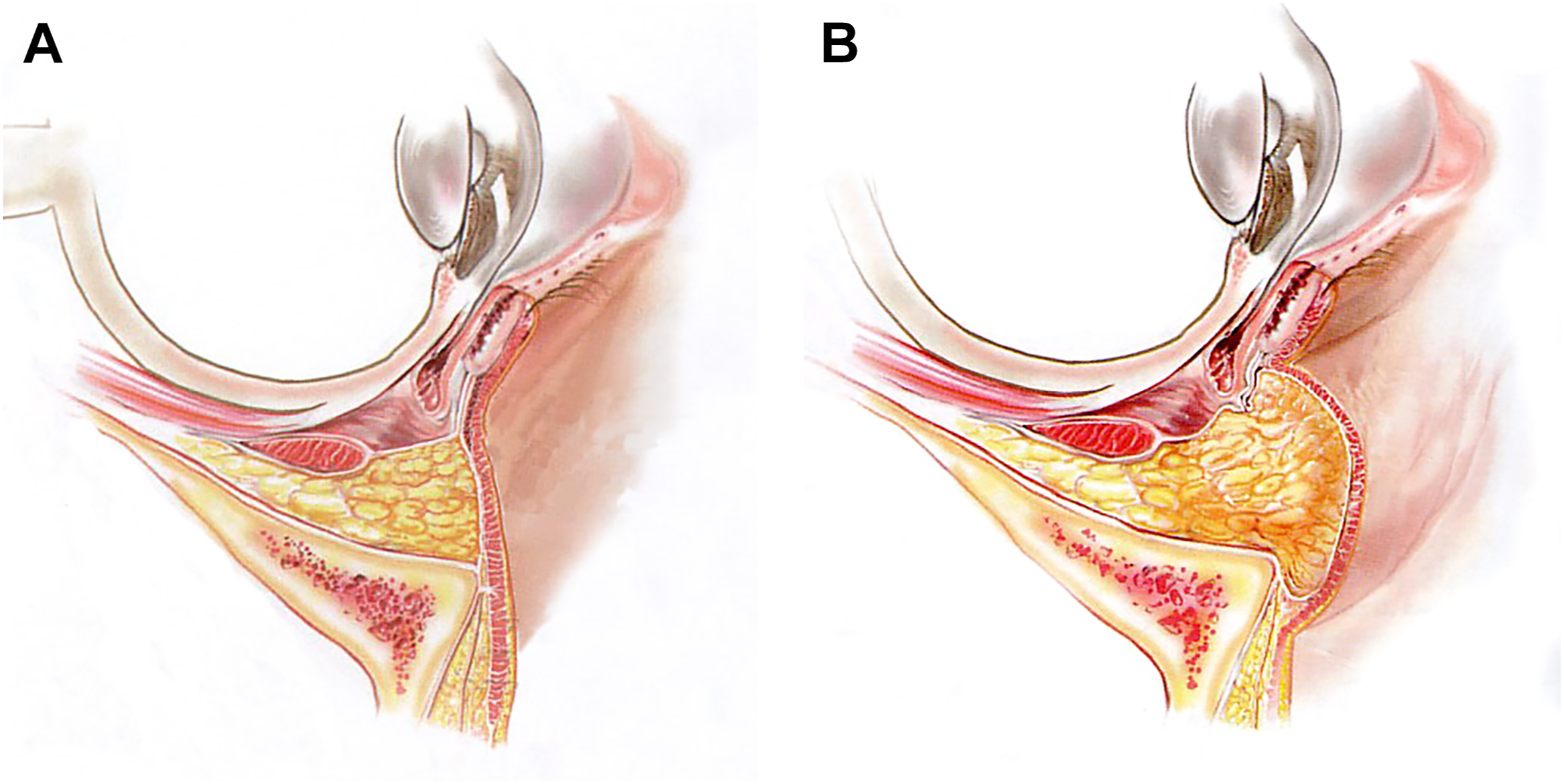
Historically, the aesthetic issues at the lower lid cheek junction were perceived as a purely lower lid problem. Deformities identified were excess skin in the lower eyelids and bulging orbital fat. Traditional logic has been that as Lockwood’s suspensory ligament relaxes, the globe drops slightly and as the orbital septum stretches, orbital fat bulges forward ( Fig. 4 ). Early surgeons attempted various techniques to directly excise excess skin on the lower eyelids. By the 1950’s, surgeons had developed reliable methods to remove bulging orbital fat either through a subciliary incision or through a transconjunctival approach.
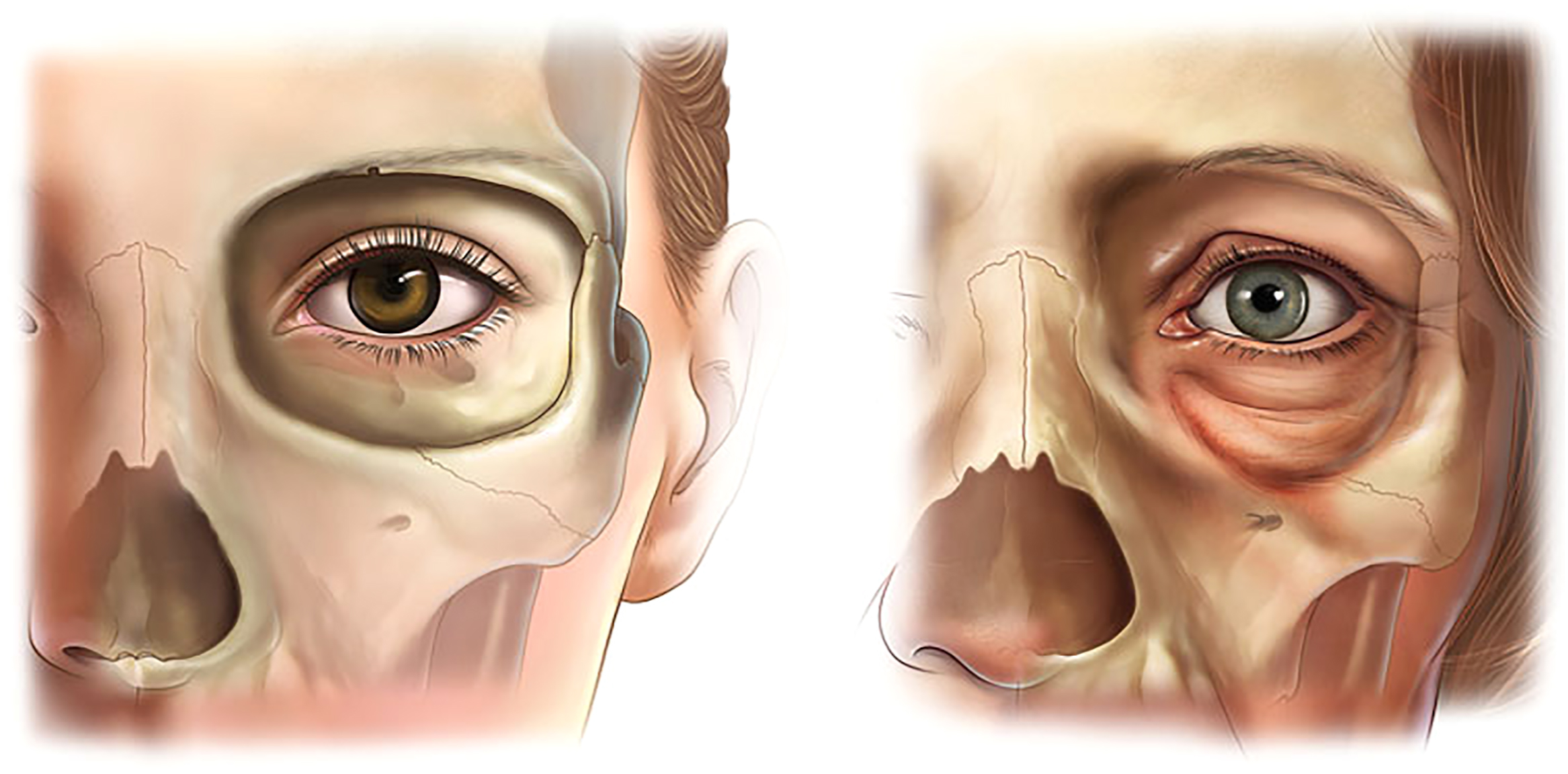
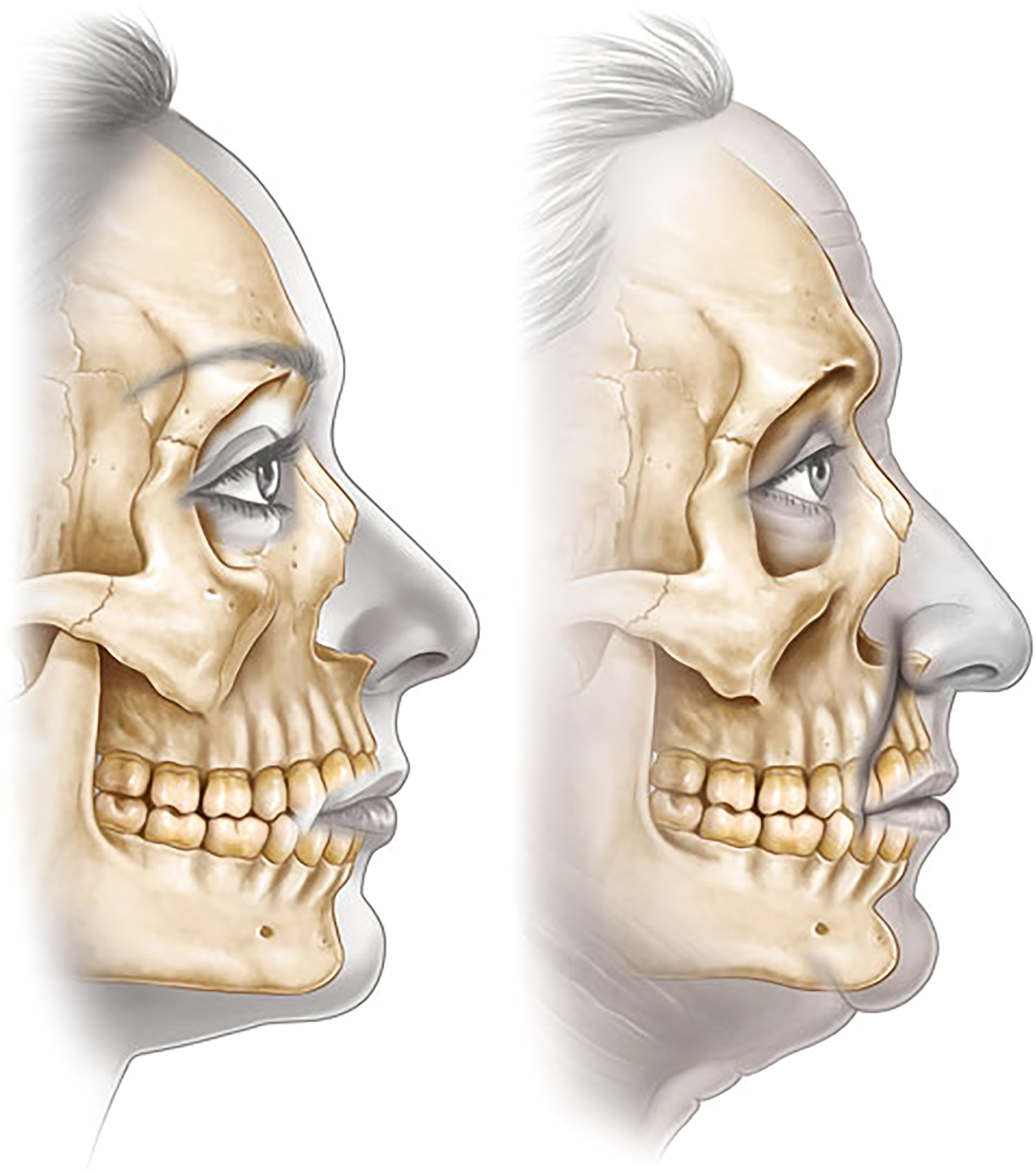
Looking more carefully at the anatomy of this area, the skeletal underpinnings of the lid cheek junction consist of the maxilla medially and the zygoma laterally. Shaw and Kahn showed that these bones attenuate with age causing the orbital aperture to become more oval as the lateral orbital rim recesses. Pessa showed that the anterior maxilla retrudes with age. , These findings have been confirmed by others. , ( Fig. 5−7 ) Flowers showed that hypoplasia of the infra orbital rim and the anterior face of the maxilla was a significant factor in the development of what he called the “tear trough deformity”.
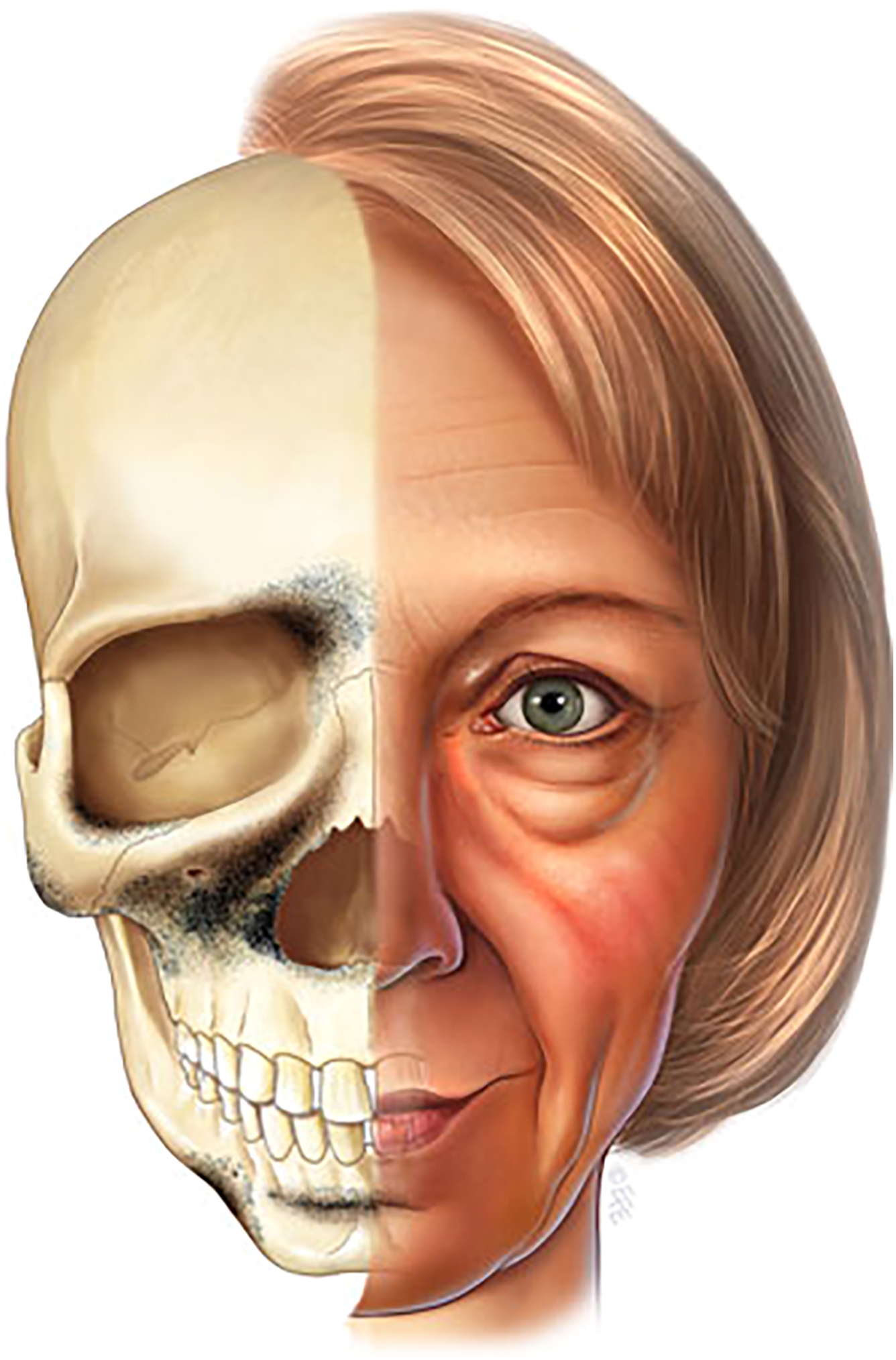
Looking at the overlying soft tissue, Jelks studied the relationship of the anterior cheek to globe prominence, showing that inadequate cheek projection was associated with lower lid malposition complications after standard lower lid blepharoplasty. This was later defined as a “negative vector” relationship. While this could be a congenital issue, Pessa showed that the prominence of the anterior cheek soft tissue, the infraorbital rim, and the maxillary face all recess posteriorly as part of the aging process.
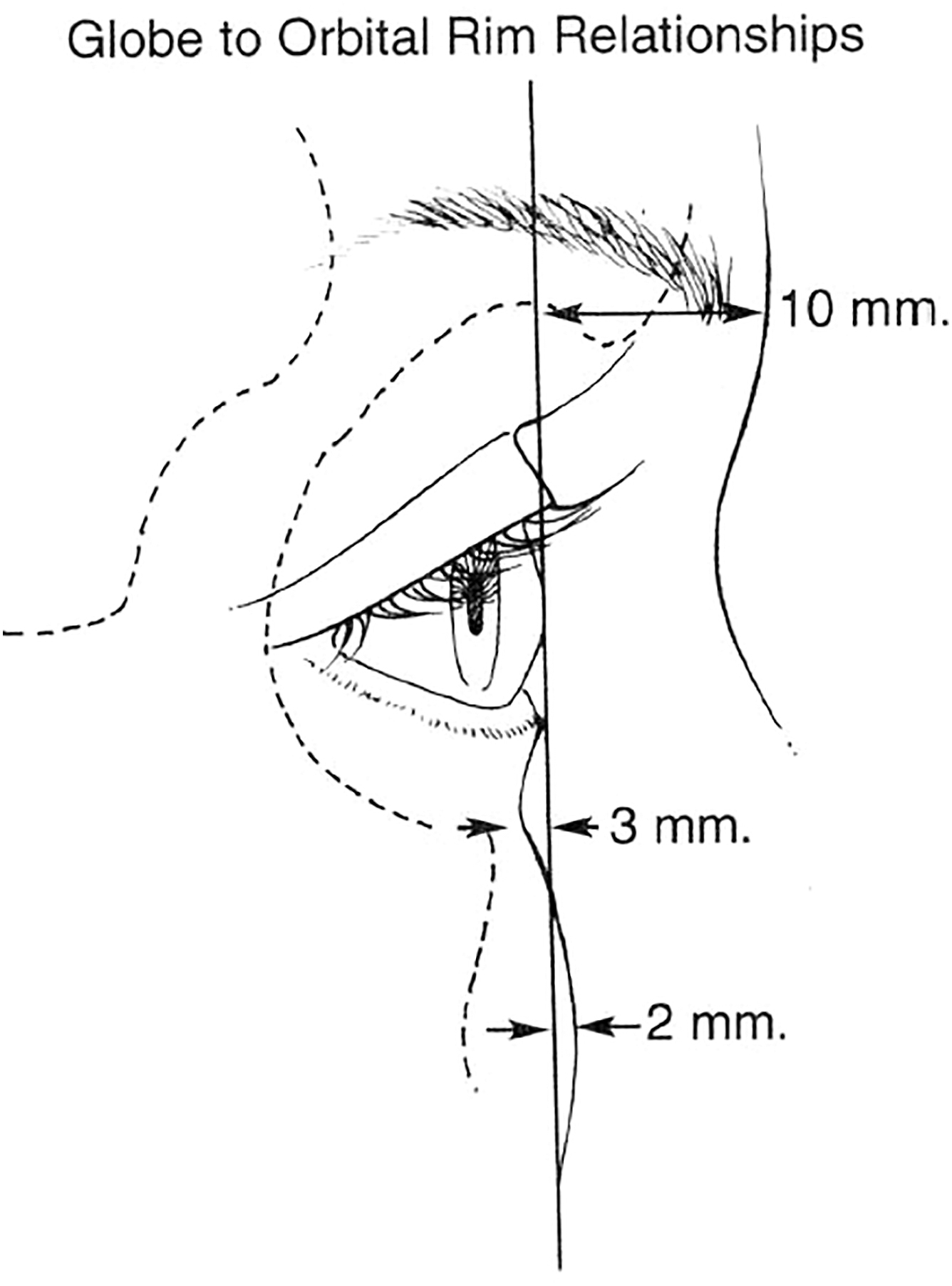
Yaremchuk summarized the relationship between globe projection and the infraorbital rim in young healthy adults. ( Fig. 8 ). This was consistent with anthropometric measurements done by Farkas. When the maxilla is flat and the cheek is less prominent, the subject appears to be older.
While the age-related loss of bony projection has been relatively easier to study, changes in the overlying soft tissue have been more difficult to elucidate. In 2021, Boehm showed that anterior cheek fat volume significantly decreases with advancing age. This occurred in both the superficial and the deep cheek fat compartments but was more pronounced in the deep. In 2023, Minelli and colleagues described how the superficial cheek fat becomes ptotic with age, thinning out along the infraorbital rim, and becoming a tear dropped shaped mass with increased volume bunching up inferiorly. ( Fig. 9 )
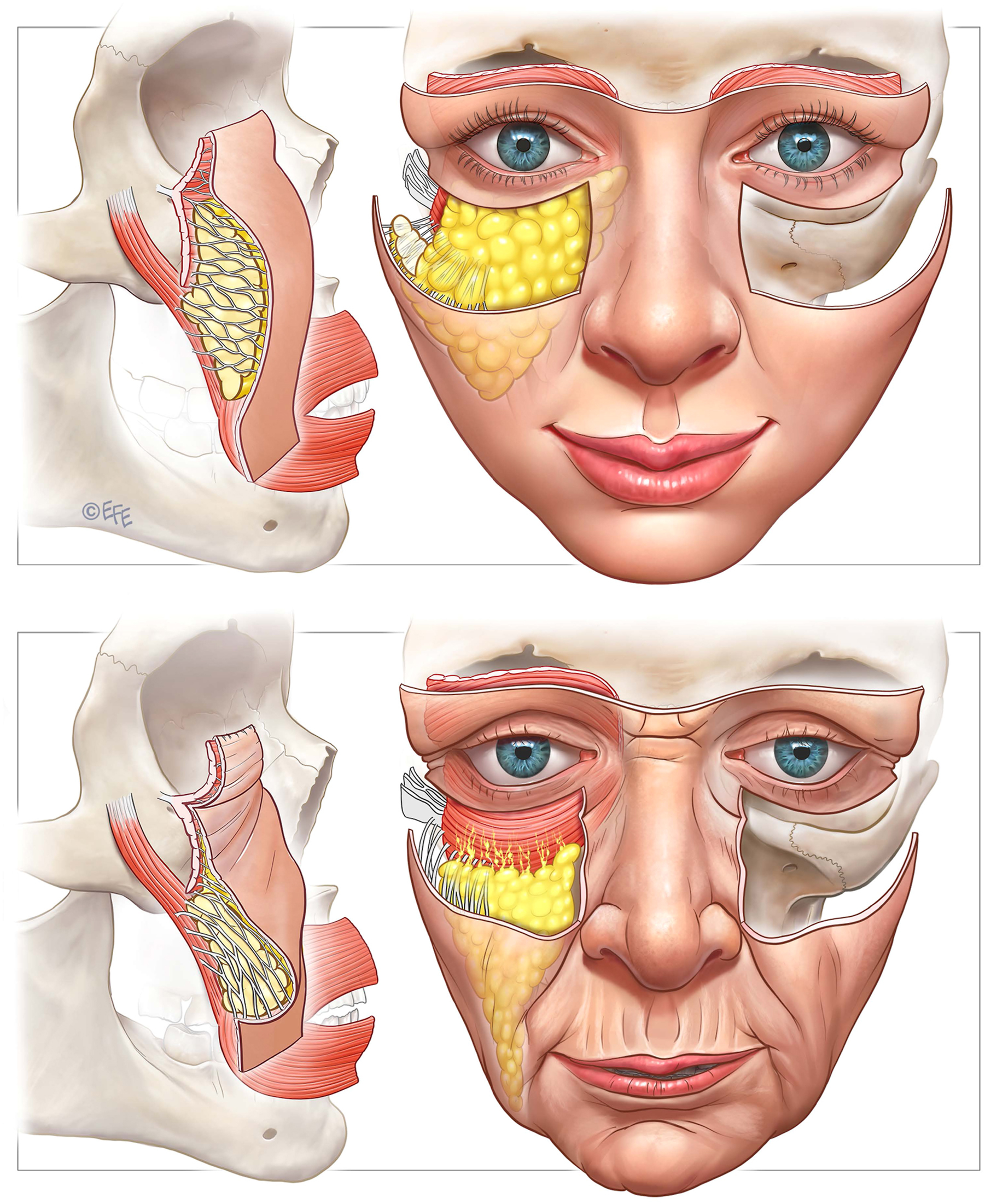
Other characteristics of anatomic change are superficial in nature. In 1978, Furnas described “Festoons” as consisting of bunched up orbicularis oculi muscle and excess overlying skin. , ( Fig. 10 and 11 ) He differentiated this condition from malar mounds, which consist of superficial fat overlying the malar prominence, bounded by the orbicularis retaining ligament above, and the zygomatic cutaneous ligaments below. ( Fig. 12 )
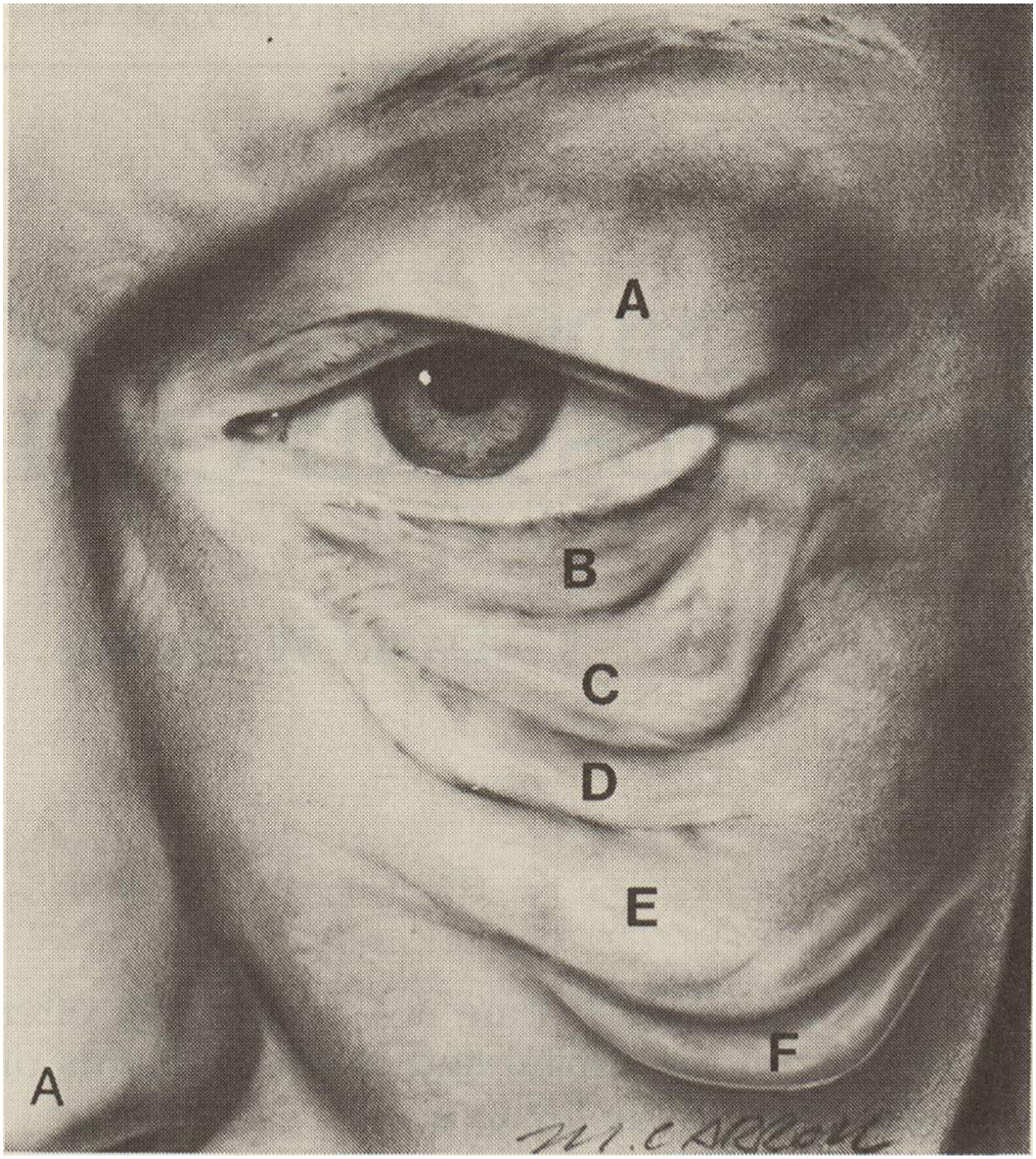
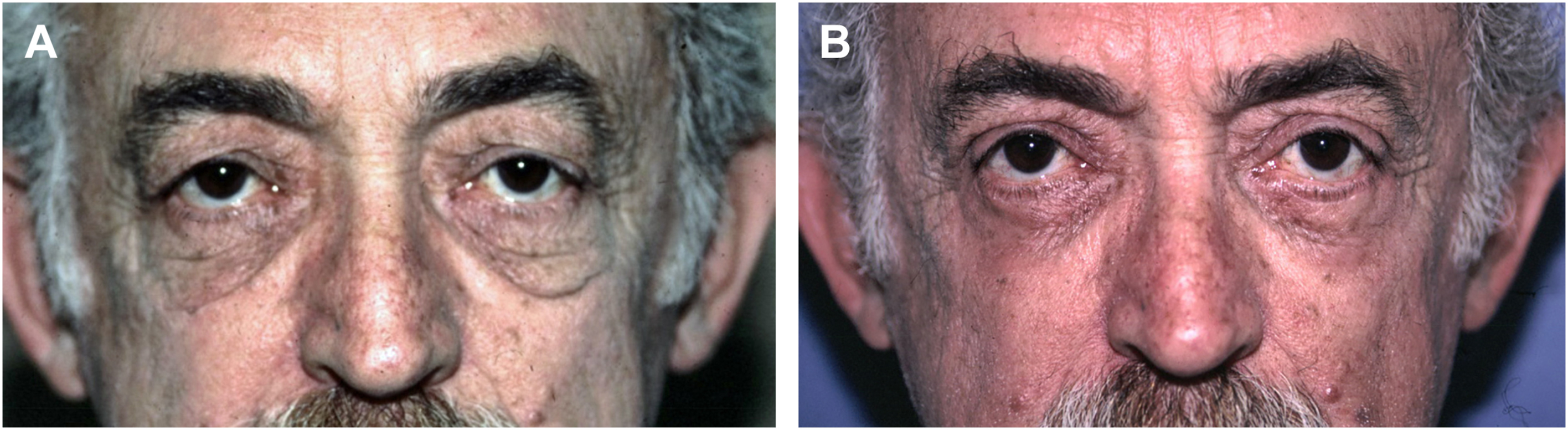
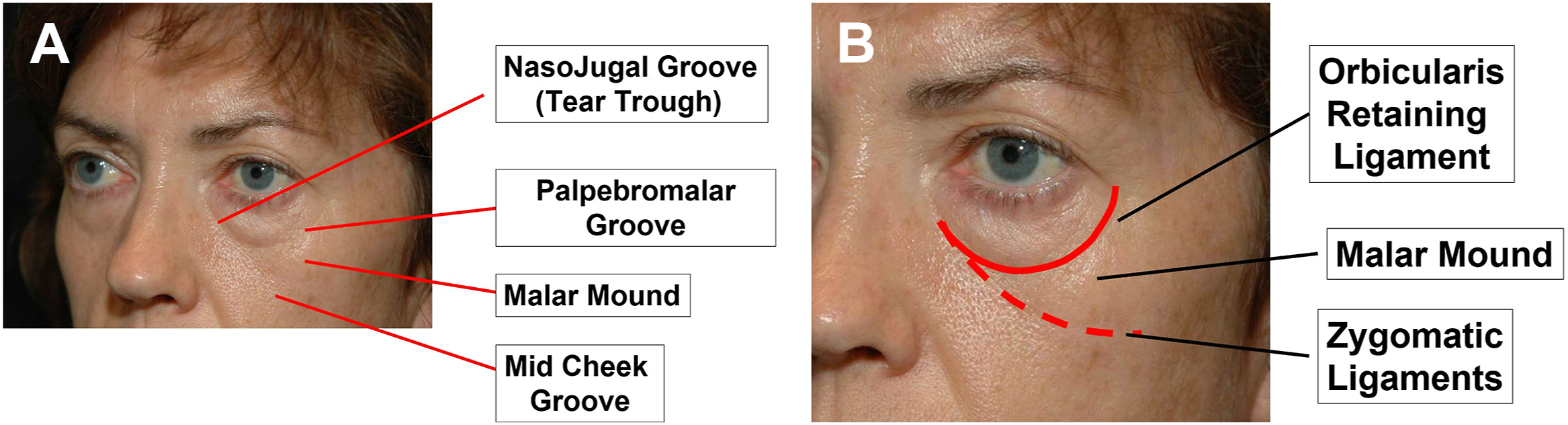
The tear trough
The Tear Trough deformity deserves special mention. When present, this anatomic entity is an accentuated version of the normal depression defining the lid cheek junction. It runs as a crescentic shaped groove just inferior to infraorbital rim, beginning medially. The groove can continue along the infraorbital rim, laterally becoming the palpebral malar groove. The term “tear trough” was coined by Flowers in 1970 and published in 1993. , In 1978, Loeb, a Brazilian, identified the same groove, calling it the naso-jugal groove; in 1981 he published his landmark paper in English demonstrating his proposed treatment. ,
Since its description, further anatomic research has delineated the various factors, which contribute to the presence of a tear trough. These are summarized in Table 1 . The primary factor present in most (but not all) patients is bulging orbital fat pushing against a weakening orbital septum. With lighting from above, this bulge casts a shadow below. Second is a soft tissue deficiency causing a groove or depression just below the superior edge of the infraorbital rim. Third is tethering of the soft tissue to bone, caused by the orbicularis retaining ligament and the tear trough ligament within the orbicularis oculi over the medial third of the infraorbital rim. Last there is skin color, which is in some patients can be much darker within the groove.
| Surface Anatomy | Underlying Anatomy |
|---|---|
| Lower Lid Bulge | Protruding Orbital Fat |
| Orbital Rim Groove | Infraorbital Rim Retrusion |
| Loss of subcutaneous fat | |
| Soft Tissue Tethering | Orbicularis Retaining Ligament |
| Skin Color | Increased Skin Pigment |
Pre-operative Assessment
Surgical strategies have been devised to deal with the various anatomic issues that contributte to the apearance of a tear trough deformity. In that regard, every case is different, and surgeons should idnetify the underlying anatomic problems in the lower lid (bulging fat, excess skin), along the infraorbital rim (bone loss, soft tissue deficiency) or in the anterior cheek (bone retrusion, soft tissue loss, and soft tissue ptosis).
The surgeon must keep in mind that the lower eyelids are critically important anatomic structures, functioning to protect the globe, supply the lipid component of the tear film through the Meibomian glands, and house the inferior punctum, which drains fluid from the surface of the globe. Unfortunately, lower lid malposition is a well-recognized post-operative problem after lower lid surgery. Therefore, a number of criteria must be addressed on physical examination before proceeding with lower lid surgery. Jelks has summarized 7 variables that should be addressed: 1. palpebral aperture, 2. Jelks vector analysis, 3. midface descent, 4. canthal tilt, 5. lateral canthus-to-lateral orbit soft tissue distance, 6. presence of mid lamellar cicatrix, and 7. tarsoligamentous integrity. In assessing these parameters, I find 3 practical measurements and tests to be particularly helpful: 1. the globe’s projection from the lateral orbital rim, 2. a snap back test, and 3. a distraction test. Normal values for these are less than 18 mm for globe projection, less than 3 sec for lid snap-back, and less than 5 mm for lid distraction. In my hands, if a patient “fails” to meet any of these normal values and lower lid blepharoplasty is planned, canthopexy support will be necessary.
Physical examination of the lower lid should ascertain the presence and amount of bulging fat and in which compartments this finding is present. The amount of loose skin is assessed by having the patient squint gently, tightening the oribicularis oculi and then using non-toothed forceps to grasp the skin. The lower lid orbicularis should be observed for muscle thickness, something that can be thinned during surgery.
The orbital rim can be palpated to determine its prominence and to estimate the amount of soft tissue superficial to bone, within the nasojugal groove. Projection of the anterior cheek mass in relation to orbital projection should be assessed to determine the presence or absence of a Jelks negative vector relationship.
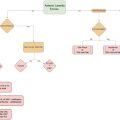
Tear Trough Assessment and Treatment
In determining the surgical management of the tear trough 2 key factors will determine the surgical approach: the presence (or absence) of bulging orbital fat and the presence (or absence) of a depression just below the edge of the infraorbital rim. Previously, the tear trough has been classified a number of different ways. In this article, a surgically-oriented classification is introduced that is very helpful to determine the correct surgical approach ( Table 2 ). Class 1 patients with bulging orbital fat but no tear trough can be treated with transconjunctival fat removal. Class 2 patients with a groove put a paucity of bulging orbital fat can be treated with synthetic filler injection, or fat grafting. Class 3 patients with bulging orbital fat adjacent to a tear trough groove are effectively treated with transposition or orbital fat into the tear trough.