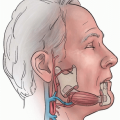
Bilobed Nasal Skin Flaps
A. MATARASSO
B. STRAUCH
INDICATIONS
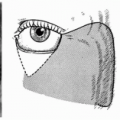
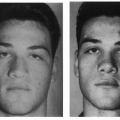
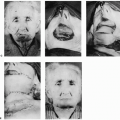
This flap is most commonly used for patients following removal of basal-cell cancers. Bilobed nasal flaps are appropriate for partial-thickness losses of less than 1.5 cm of the lateral aspect of the nose, ala, and tip area. It is feasible in situations where sufficient laxity exists in surrounding nasal tissue, to allow the excess to be transposed for wound coverage, while permitting primary closure of the final donor site. The concept of transferring tissue laxity from the upper to the lower nose or “robbing Peter to pay Paul,” allows losses of tissue to be replaced in kind (6). A bilobed flap may also be used in conjunction with other flaps to reconstruct more complex contour defects in the nasal area (7). For example, it may be used to cover a full-thickness nasal-tip defect, where lining and support are provided by a composite graft to the underside of the bilobed nasal flap.
ANATOMY
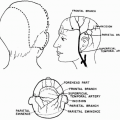
This flap is essentially a rotation flap divided into two transposition flaps. The bilobed flap has a random-pattern blood supply. However, there is evidence that, when the flap is designed near the level of the inner canthus, a portion has a direct axial blood supply (angular and supraorbital arteries) (8). The flap is composed of full-thickness nasal skin and subcutaneous tissue. A readily apparent cleavage plane is established between the flap and the underlying muscular elements.
FLAP DESIGN AND DIMENSIONS
Approaches to the bilobed flap have changed over time from consideration of two flaps alike in size and form to the utilization of a smaller secondary flap, more triangular in shape, facilitating closure of the donor deformity (9). Esser (10), the first to describe the use of bilobed rotation flaps for the repair of nasal tip defects, believed that 90° was the optimal angle between the two flaps; however, it could vary between 95° and 180° (11). The greater the angle, the larger is the resultant dog-ear that must be adjusted. This should be considered when planning the flap, because trimming the excess tissue can compromise the vascular pedicle.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree