Over half of orthopedic surgeons will change jobs prior to their fifth year in practice. Commonly cited reasons behind the change include compensation, work–life balance, poor job fit, and dissatisfaction with management. Many of these factors are difficult to vet as a job applicant and are often only realized during the course of real-life practice. Possessing the tools and knowledge for effective self-reflection is crucial. It enables a clear understanding of why the current job may not be working and provides insights on how to transition to a different career path.
Key points
- •
Over half of orthopedic surgeons will change jobs prior to their fifth year in practice.
- •
Most commonly cited reasons for changing jobs include financial reasons and expectations of the practice not being met.
- •
Selecting a first job can be challenging as orthopedic trainees receive little to no formal training on job evaluation and selection during their training.
- •
Challenges of first jobs include new responsibilities as leader of a clinical and operating room team, increased documentation burden, increased involvement in administrative and business aspects of medicine, and difficulty with work–life balance leading to burn out.
- •
When considering changing jobs, one must consider the personal and professional factors that would allow for more satisfaction in their career.
Changing jobs: a common part of early practice
Laratta and colleagues conducted a survey of members of the American Academy of Orthopedic Surgeons to investigate the rate at which recently trained orthopedic surgeons change their initial job and to identify factors influencing the job selection process. Out of the 351 respondents, which accounted for 21% of those who received the survey, 51% left their first job before completing their fifth year in practice. The primary reasons for leaving were often either financial issues (34%) or discrepancies between the advertised and actual nature of the practice (31%). Authors found that regardless whether orthopedic surgeons switched jobs, the most crucial factors influencing the selection of their initial posttraining job were practice location and practice type. Among those who did switched jobs, these 2 factors remained the most important influences in job selection. The majority of respondents found they had inadequate training in selecting their first job (53%) and most found they felt unprepared in the business side of medicine to make an informed decision (88%). This article will delve deeper into these factors further and aims to assist orthopedic surgeons in determining whether transitioning to another job is the right decision for them.
Challenges of the first job
Once entering practice, there are many new aspects to working that make the first job challenging. The earliest challenge begins with actual job selection; orthopedic residents receive little to no formal training on job evaluation and selection during their training. For many, this task is the first fully autonomous career decision they will make as a practicing surgeon, after a more rigid job selection structure through residency and fellowship match. As their personal and career goals rapidly evolve through training and in their personal lives, these changes can lead to a less distinct understanding of personal motivations and a long-term career trajectory. Young surgeons may also feel pressure to choose a job that does not meet all of their needs in order to navigate a competitive job market. This is of particular concern in sports medicine, which has the highest ratio of graduating fellows per advertised job (6.3) of any orthopedic specialty. The desire to find a job in a highly competitive job market can fundamentally undermine a young surgeon’s ability to negotiate a job that meets the core priorities of that surgeon. There may even be a lack of understanding of how a compromise on core values may affect long-term job satisfaction.
Financially, many trainees will also accrue significant financial debt, with the average medical student graduating with approximately US$250,000 in debt. The burden of debt can significantly impact decision-making during the initial job selection process. In some cases, incentives for debt relief may lead new surgeons to choose less desirable locations or practices that do not align with their long-term goals. Additionally, physicians tend to undervalue themselves during salary negotiations for their first job contract. This valuation can lead to feelings of dissatisfaction with the end result and may be an important motivator for changing jobs if salary is later deemed as unsatisfactory.
Transitioning from training to practice brings forth various challenges in both clinical and business aspects of medicine. These challenges encompass assuming new roles as the primary decision-maker in clinical and operating room settings, facing an increased documentation burden, navigating through bureaucracy and administrative obstacles associated with the practice, financial considerations, and contending with a lack of experience with the business side of medicine.
The duties related to documentation and billing, along with the assumption of new administrative roles, introduce fresh challenges to the daily workload of an early-career surgeon. The increased demand for documentation through chart dictation and billing processes can extend working hours significantly. Studies have shown that most orthopedic residents lack knowledge in basic billing and coding skills and that formalized training in this area can significantly improve surgeons’ medical billing competency. , New administrative roles that involve practice management can also be daunting and time consuming. In the previous survey by Laratta and colleagues, 88% of respondents felt unprepared for the business side of medicine entering practice.
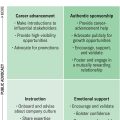
Studies demonstrate that mentorship and sponsorship play a crucial role in the development of early-career surgeons. Mentors offer valuable guidance not only in clinical situations but also in navigating the complexities of practice management. The absence of mentorship with a practice can intensify the stress experienced during this pivotal stage of a young surgeon’s career. , Additionally, having career sponsors who actively support advancement and leadership development is essential for fostering job satisfaction. Sponsors work to promote career growth and advocate for the young surgeon, ensuring access to relevant career opportunities. Both mentors and sponsors serve as critical role models for young surgeons, contributing to job satisfaction and career progression. The lack of effective mentorship and sponsorship has been shown to negatively impact career advancement, especially in academics and particularly noteworthy among women and underrepresented minority surgeons.
Interpersonal relationships at work and the overall workplace culture are crucial factors to consider when assessing job satisfaction. The collegiality within one’s work environment and the support network among colleagues hold significant importance. This aspect of the work environment, especially for female surgeons, strongly influences overall job satisfaction. An anonymous survey was distributed to approximately 1100 members of the Ruth Jackson Orthopedic Society and 1600 members of Women in Orthopedics Facebook group, with an estimated response rate of 50% for both, and protocols in place to mitigate duplicate response. Out of the 373 respondents, 72% reported experiencing workplace conflict self-attributed to their gender. Additionally, 8% either left their previous job or were forced to leave due to workplace conflict, resulting in feelings of depression, anxiety, and burnout.
Finally, navigating increased burdens on work–life balance poses a well-recognized challenge. Many early-career surgeons are concurrently managing personal pursuits, such as finding a partner or starting a family, and can encounter difficulties in balancing the heightened responsibilities at both work and home. A survey conducted in 2015 revealed that, for 67% of orthopedic surgeons, work-related stress significantly impacted their personal lives. Moreover, 70% of orthopedists reported that extended work hours negatively affect their family lives with few having formal support at their institutions. Studies have found that physicians who spend less than 20% of their time on meaningful work have much higher rates of burnout.
A lack of available personal and professional support at a job can increase dissatisfaction and burnout emphasizing the importance of considering practice location to assure a strong network for support.
A recurring theme throughout is that many challenges faced by early-career surgeons not only contribute to job dissatisfaction but also parallel risk factors for physician burnout. The reported rate of burnout among practicing orthopedic surgeons ranges from 32% to 46%, and it is even higher among early-career orthopedists, with rates among orthopedic residents reaching as high as 56%. Burnout is characterized by 3 components: emotional exhaustion, depersonalization (including dehumanization and indifference), and loss of personal accomplishment. Gollac and colleagues defined 6 psychosocial risk factors for burnout, which include (1) intensity and complexity of the work; (2) significant emotional requirements of work and from patients; (3) loss of autonomy at work; (4) deterioration of social interactions at work; (5) conflict in values (between the physician and their institution); and (6) job and work insecurity (including socioeconomic insecurity and a drive for change at the work institution). It is crucial for a surgeon contemplating a job change to discern whether their current job dissatisfaction stems from burnout. More importantly, if related to burnout, understanding whether the factors contributing to the physician’s burnout are specific to their current job (potentially alleviated with a career change) or independent of their current job (thus at risk of persisting in a new position) is essential.
Considerations for leaving your current job
It is essential to identify the aspects of professional and personal life that contribute to happiness and satisfaction. While a job may be clinically rewarding job, its location might be too far from social support systems, therefore, posing challenges to the job’s sustainability. Conversely, an ideal location may not facilitate a desirable clinical setting or manageable call burden. Additionally, it is important to assess whether challanges which exist at the current job are insurmountable.
Orthopedic surgeons must weigh multiple variables when contemplating a job switch, including the practice model/setting, clinical practice/patient population, practice volume, interpersonal dynamics of a group, call schedules, location, compensation, dedicated operating room time and/or support, and the availability of clinical support and resources ( Table 1 ). Before making the decision to transition to a new position, surgeons should clarify why they want to leave their current job, articulate what they seek in a new job and consider if adjustments to their current job could enhance job satisfaction. Beyond direct job satisfaction, financial and personal factors should also be taken into account.