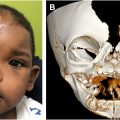
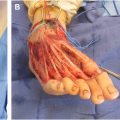
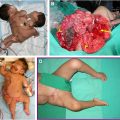
Robin sequence is a congenital condition characterized by micrognathia, glossoptosis, and airway obstruction with or without cleft palate. The condition is best managed by a multidisciplinary team proficient in treating the complex pediatric airway, including pediatricians, speech and feeding specialists, and surgeons. Conservative treatment includes prone positioning, nasopharyngeal airways, supplemental oxygen, and feeding support to maintain a patent airway and promote infant growth. For infants requiring further intervention, the tongue may be repositioned anteriorly through surgical tongue-lip adhesion or nonsurgical techniques including the orthodontic airway plate. Mandibular distraction osteogenesis is used in severe cases with the goal to avoid tracheostomy.
Key points
- •
Robin sequence (RS) is the clinical triad of mandibular hypoplasia, glossoptosis, and airway obstruction. It is commonly associated with cleft palate.
- •
The mainstay of treatment is conservative management to support an infant’s airway, breathing, feeding, and growth during the neonatal period.
- •
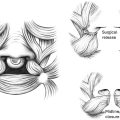
Surgical intervention is sometimes indicated to relieve severe airway obstruction, commonly by tongue-lip adhesion or mandibular distraction osteogenesis.
- •
RS may have syndromic and non-syndromic etiologies, and there is significant heterogeneity of clinical severity and outcomes of treatment.
Background
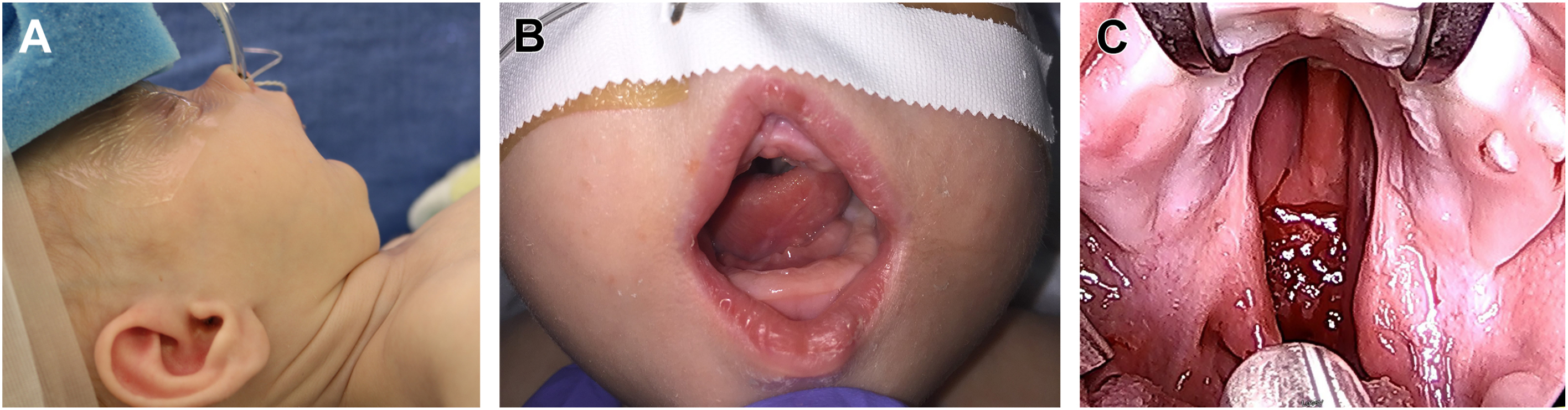
Robin sequence (RS) is the clinical triad of mandibular hypoplasia, glossoptosis, and airway obstruction, named after the French stomatologist who described these findings in a seminal paper in 1923. The prevalence of RS globally is estimated at 9.5 births per 100,000. Cleft palate is commonly associated with RS, identified in approximately 85% of patients, and typically seen as a wide, U-shaped cleft of the secondary palate ( Fig. 1 ).
Embryology
During the sixth to eighth week of gestation, neural crest cells migrate into the mandibular arch and Meckel’s cartilage subsequently serves as the scaffold for mandible and tongue development. , In RS, the morphology of the mandible is notably different from normative controls. The ramus and body of the mandible are both shorter in length, with a more acute gonial angle and more obtuse symphyseal angle , .
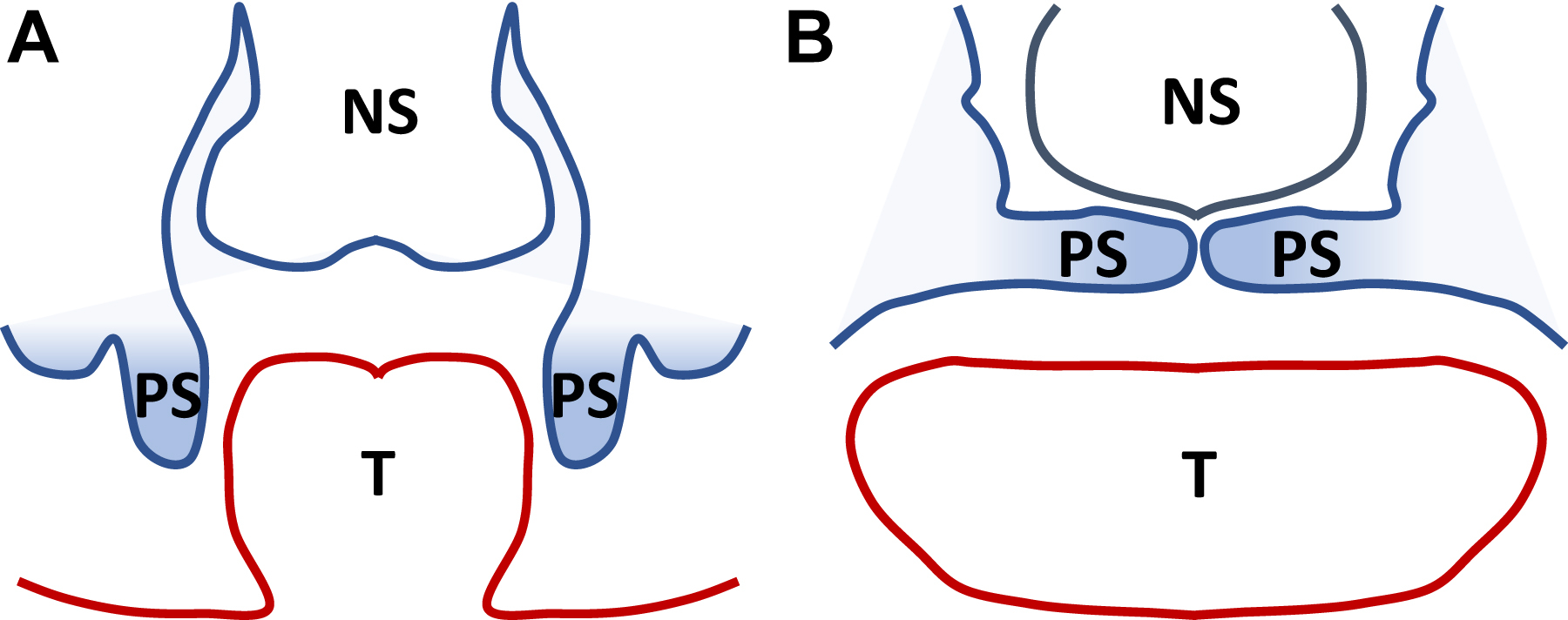
The maxilla develops simultaneously with the maxillary arch forming the lateral palatine processes. The lateral palatine shelves are initially vertically positioned alongside the tongue and move to a horizontal position where they then fuse with each other and the median palatine process anteriorly ( Fig. 2 ). , A retrognathic mandible is hypothesized to contribute to the tongue being positioned between these lateral palatine shelves, impeding normal fusion of the palate and contributing to the wide U-shaped cleft deformity commonly seen in RS (see Fig. 1 C).
Associations
In 62% of children, RS occurs in the absence of other congenital anomalies, which is described as isolated RS. In other children, RS is associated with other congenital anomalies, and may be one feature of a genetic syndrome ( Table 1 ). , Therefore, there is significant heterogeneity in phenotype of RS. The degree or cause of mandibular hypoplasia as well as the severity of glossoptosis and airway obstruction may vary significantly. Additionally, RS may be associated with other airway anomalies, which can complicate the clinical picture and treatment plan.
| Syndromes Associated with RS | Gene (If Known) | Associated Features |
|---|---|---|
| Stickler | COL2A1, COL11A1, COL11A2 | Myopia, retinal detachment, hearing loss |
| Marshall | COLL11A1 | Congenital cataracts, hypoplastic nasal bones, sensorineural hearing loss |
| Treacher Collins | TCOF1 | Downslanting palpebral fissures, lower eyelid colobomas, zygomatic hypoplasia |
| Nager | SF3B4 | Downslanting palpebral fissures, conductive hearing loss |
| Auriculocondylar syndrome | GNAI3, PLCB4 | “Question mark” ear, temporomandibular joint, and condyle anomalies |
| Craniofacial microsomia/hemifacial microsomia/oculo-auriculo-vertebral spectrum/Goldenhar | SF3B2, FOXI3 | Microtia/atresia, unilateral or bilateral mandible hypoplasia, facial nerve paralysis, rib/skeletal anomalies, cardiac/renal anomalies, epibulbar dermoid, coloboma of the eyelid |
| Campomelic dysplasia | SOX9 | Short stature, campomelia, hearing loss |
| Kabuki | KMT2D | Arched eyebrows, prominent ears, developmental delay |
| Carey-Fineman-Ziter | Hypotonia, moebius, growth delay, scoliosis | |
| Fetal alcohol | Teratogenic | Microcephaly, growth delay |
| 22q11.2 deletion | TBX1 | Conotruncal heart defects, prominent nose, renal/endocrine anomalies, neuropsychiatric problems |
| Trisomy 18 | Microcephaly, growth and cognitive impairment, low set ears, cardiac defects | |
| Trisomy 21 | Characteristic facies, developmental delay | |
| 2q33 microdeletion | SATB2 | Growth restriction, dental anomalies, downslanting palpebral fissures |
| 17q24 deletions and translocations | SOX9 | Isolated RS |
Evaluation
A multidisciplinary approach to the evaluation and management of patients with RS is important to success. Team members typically include neonatology, genetics, pulmonology and sleep medicine, otolaryngology, plastic surgery, gastroenterology, developmental pediatrics/genetics, speech and language pathology, nursing, and social work.
Prenatal Evaluation
Prenatally, RS can occasionally be identified based on ultrasonographic findings suggestive of micrognathia, glossoptosis, cleft palate, and/or polyhydramnios. The inferior facial angle is one measurement that may help characterize retrognathia, defined by the line orthogonal to the forehead at the nasofrontal suture and the line from mentum to anterior border of the lip ( Fig. 3 ). When less than 50 o , this may prompt additional evaluation for glossoptosis or cleft palate on ultrasound or fetal MRI. ,
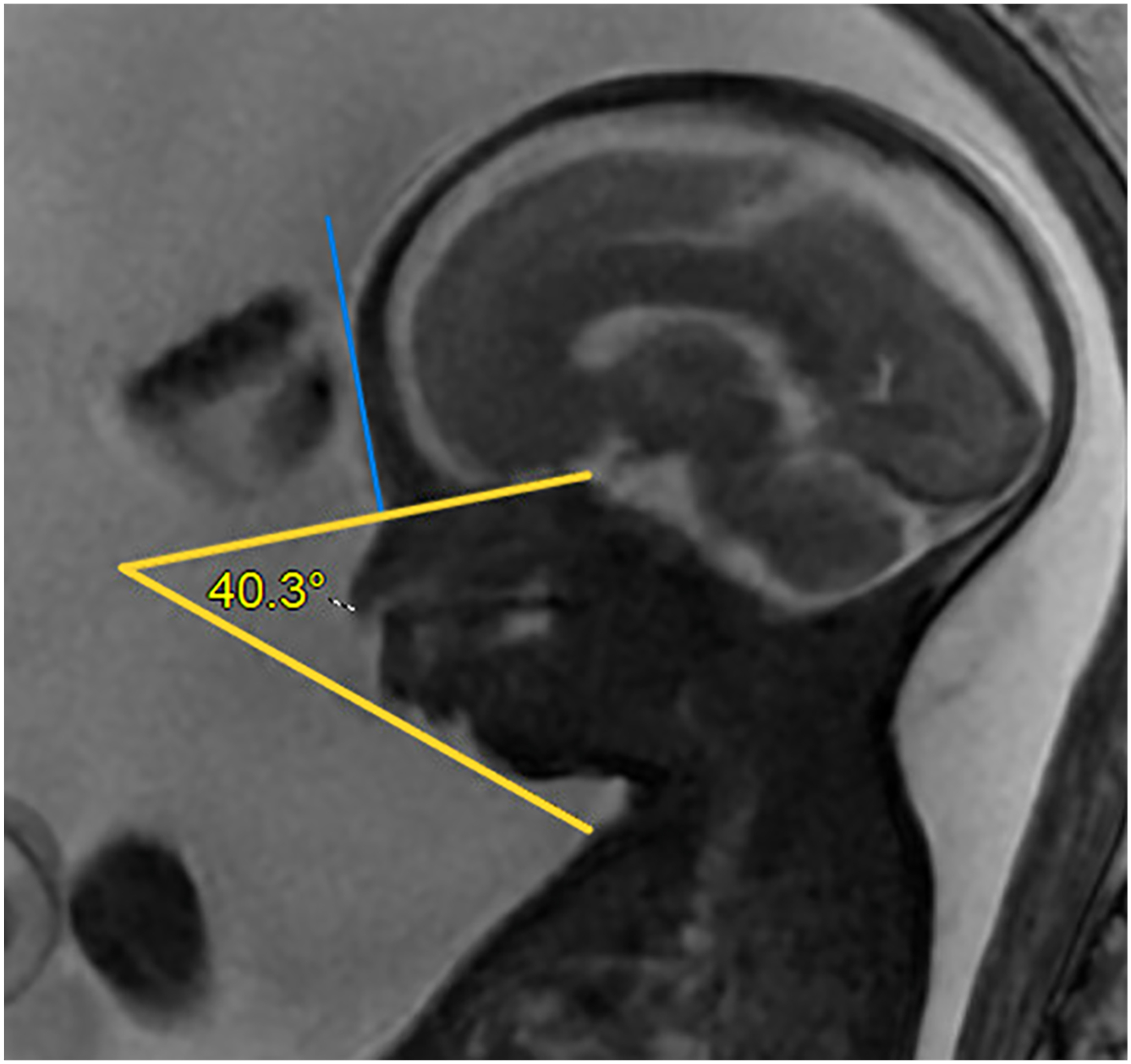
Clinical Examination
Evaluation of the infant with RS begins with assessing and treating airway obstruction. This includes physical examination for evaluation of an increased work of breathing, stertor (low-pitched snoring emanating above the level of the larynx/upper airway), stridor (high-pitched, noisy breathing emanating from the level of the larynx or below/lower airway), and the use of accessory muscles of respiration. Clinical evaluation includes the evaluation of oxygen saturation, heart rate, and apneic events. Airway obstruction in the supine versus side lying and/or prone position may be helpful to understand if the obstruction is positional. Side lying or prone positioning can relieve obstruction related to glossoptosis. Airway support may include repositioning, nasal cannula, nasopharyngeal airway, noninvasive positive pressure ventilation (NIPPV, including continuous positive airway pressure [CPAP] or bilevel positive airway pressure [BiPAP]), or use of a laryngeal mask airway or endotracheal intubation if obstruction does not respond to more conservative measures.
Micrognathia can be assessed by evaluating the distance between the alveolar process of the maxilla and mandible, or the maxillomandibular overjet. The jaw index is another measurement of micrognathia, characterized by a combination of maxillomandibular overjet as well as the ratio of the distance from tragus to tragus through subnasale and pogonion. , Glossoptosis is noted when the tongue tip is posteriorly positioned often with the presence of audible stertor. An improvement of the airway with jaw thrust may help clarify whether tongue-based obstruction is present. Intraoral evaluation for cleft palate is necessary. RS may be associated with no cleft, submucous cleft palate, or any degree of clefting of the soft and/or hard palate.
Airway Evaluation
Evaluation of the airway by a pediatric otolaryngologist typically includes flexible laryngoscopy to evaluate the severity of glossoptosis and evaluation for associated airway malformations including laryngomalacia. This may be done at bedside under an awake state or drug-induced sleep endoscopy may be performed. In the operating theater, a more thorough evaluation of the airway may be performed by rigid microlaryngo-tracheo-bronchoscopy to evaluate for other associated airway lesions.
Sleep Evaluation
Oximetry, capnography, and formal polysomnogram (PSG) are useful to quantify the severity of obstruction. Overnight PSG requires specialized equipment and staff in a sleep laboratory for data capture and analysis. The thresholds for diagnosis of obstructive sleep apnea (OSA) in neonates remain controversial, as normal values in neonates may vary with prematurity and be higher than in children over a year of age. , However, saturations are consistently below 90%, and Obstructive Apnea Hypopnea Index (OAHI) of > 5 is considered consistent with moderate sleep apnea. OAHI > 10 is characterized as severe sleep apnea and values above this often indicate additional management intervention. In addition to the OAHI, the degree and frequency of desaturations help clinicians stratify mild cases from more severe ones.
Feeding Evaluation
Feeding in RS can be complex, with a variety of challenges in the newborn. Feeding requires rhythmic coordination of suction, swallowing, and breathing, which may be impacted by jaw position, jaw size, tongue position, airway obstruction, and cleft palate. Evaluation by a feeding specialist familiar with cleft and RS is essential. Patients with cleft palate cannot generate appropriate negative pressure with breast or bottle feeding, and therefore, the use of an appropriate cleft feeding system is necessary. Optimization of infant position during feeding, nipple flow rate, and monitoring for clinical signs of aspiration is important. When dysphagia or aspiration is suspected, video fluoroscopic swallow study or functional endoscopic evaluation of swallowing can be used to evaluate unexplained swallowing difficulties or evaluate for aspiration in real time. Gastroesophageal reflux can lead to increased upper airway edema and further exacerbate feeding challenges or contribute to laryngomalacia in these patients. In many cases, treatment of reflux may be helpful in managing feeding-related complications. ,
Poor growth or failure to thrive may be indicative of chronic airway obstruction. This is related to increased energy expenditure due to increased work of breathing or difficulty with feeding relative to caloric input. Feeding times may be prolonged (>30 min) due to poor efficiency. Children with multiple congenital anomalies suspected to have syndromic or neuromotor disorders may additionally struggle with feeding due to tone and coordination. Prompt identification of the feeding challenges in infants with RS is necessary to allow the child to safely grow. Supplementation of oral feeding with nasogastric or gastric tube feeds is occasionally needed for short-term management of feeding difficulties in these patients. A team of feeding specialists including speech and language pathologists, nursing, neonatology, and gastroenterology is needed to optimize the care of these patients.
Genetic Evaluation
Evaluation of the infant with RS by a clinical geneticist is recommended for all patients to evaluate for additional anomalies which may impact feeding, growth, airway obstruction, and management. RS can be associated with numerous syndromes and chromosomal anomalies which may impact the etiology of micrognathia and airway obstruction and correlate with other congenital anomalies which may impact the child’s management and prognosis (see Table 1 ). , Evaluation of family history of similar diagnoses, other abnormal craniofacial examination findings, eye or vision concerns, developmental delays, cleft, or speech concerns may indicate a syndromic phenotype. Ophthalmologic evaluation is indicated if there is concern for Stickler syndrome between 6 and 12 months of age. Neurologic evaluation including brain MRI is indicated if there is abnormal tone, microcephaly, or other abnormal craniofacial features. Congenital heart defects, particularly ventricular septal defects (VSD), are common associations and echocardiogram should be considered if a murmur is present or if 22q11.2 deletion is suspected. Other commonly associated anomalies include renal abnormalities, hypospadias, ear and hearing concerns, and limb defects, including syndactyly, hypoplasia, and arthrogryposis.
Imaging
CT scan may be a useful adjunct for evaluation of additional airway lesions, to characterize the mandibular morphology or evaluate other craniofacial anomalies. This is most commonly used prior to planning surgical intervention.
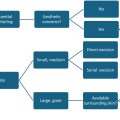
Management
Management of RS varies due to the heterogeneity of patient presentation and a paucity of long-term comparative outcomes data. Some patients present with an emergent need for surgical intervention during the neonatal period to alleviate airway obstruction, while others may be managed conservatively. The advantages and disadvantages of the diverse nonsurgical and surgical treatment modalities must be considered for each individual patient ( Box 1 ). This review will focus on management in the neonatal period, however, some children with RS may benefit from elective orthognathic surgery at skeletal maturity for occlusal and esthetic indications.
| Evaluation | Management |
|---|---|
|
|
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree