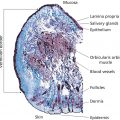
Anna Hare1 and Phoebe Rich2 1 Oregon Dermatology and Research Center, Portland, OR, USA 2 Oregon Health & Science University, Portland, OR, USA Understanding nail unit anatomy and pathophysiology is essential to maximizing the benefits of nail cosmetics without inducing pathology via cosmetic materials and procedures. The nail unit is composed of the nail matrix, proximal and lateral nail folds, the hyponychium, and the nail bed (Figure 28.1). Table 28.1 lists common nail signs and definitions relevant to nail cosmetics. The nail matrix is composed of germinative epithelium from which the nail plate is derived (Figure 28.2). The majority of the matrix lies under the proximal nail fold. The distal portion of the nail matrix creates the white lunula, visible through the proximal nail plate on some digits. It is hypothesized that the white color of the lunula can be attributed to both incomplete nail plate keratinization and loose connective tissue in the underlying dermis. The proximal nail matrix generates the dorsal (superficial) nail plate, while the distal nail matrix generates the ventral (inferior) nail plate. This concept is crucial to understanding nail pathology. Preserving and protecting the matrix during nail cosmetic processes is essential for proper nail plate formation. Significant damage to the nail matrix can result in permanent nail plate dystrophy. The nail plate is derived from the nail matrix and composed of closely packed, keratinized epithelial cells called onychocytes. Cells in the matrix become progressively flattened and broadened and lose their nuclei as they mature into the nail plate. The nail plate is curved in both the longitudinal and transverse planes, allowing adhesion to the nail bed, and the plate ensheathed by the proximal and lateral nail folds. Longitudinal ridging may be present on both the dorsal and ventral surface of the nail plate. Mildly increased longitudinal ridging on the dorsal nail plate is considered a normal part of aging. Ridging on the ventral surface of the nail plate is caused by the structure of the underlying nail bed and vertically oriented blood vessels. The composition and properties of the nail plate are further discussed below. The nail folds surround and protect the nail unit by sealing out environmental irritants and microorganisms through the tight attachment of the cuticle to the nail plate. This barrier formed by the cuticle, or eponychium, is essential to preventing the invasion of irritants, moisture, bacteria, and yeasts under the nail fold. Disruption of this barrier as often occurs in cosmetic nail procedures when the cuticle is cut or pushed back, can result in infection or inflammation of the nail fold, termed paronychia (Figure 28.3). Chronic paronychia may disrupt the underlying nail matrix and subsequently lead to nail plate dystrophy. Figure 28.1 Nail unit with lines indicating important structures. The hyponychium is the cutaneous margin underlying the free edge of the nail plate. It is contiguous with the volar aspect of the fingertip. The nail bed ends at the hyponychium. The hyponychium functions like the cuticle, acting as an adherent seal to protect the nail unit. Overmanipulating of the hyponychium during nail grooming (i.e. excessive cleaning under the nail) can result in onycholysis, or separation of the nail plate from the nail bed. This space created between the nail plate and bed retains moisture, creating an ideal environment for potential pathogens, such as yeast, bacteria, or fungi. The nail bed is thin, 2–5 cell layer thick epithelium that underlies the nail plate. It extends from the lunula to the hyponychium. The nail bed is composed of longitudinal, parallel rete ridges with a rich vascular supply. This vascularity is responsible for the pink coloration of the bed as well as longitudinal ridges on the ventral surface of the nail plate. In chronic onycholysis, when the nail plate is separated from the nail bed for an extended duration, the nail bed epithelium may become keratinized, form a granular layer, and lead to permanent onycholysis (Figure 28.4). The distal phalanx lies immediately beneath the nail unit. The extensor tendon runs over the distal interphalangeal joint and attaches to the distal phalanx 12 mm proximal to the proximal nail fold. Given that there is little space between the nail unit and distal phalanx, minor injury to the nail unit may extend to the periosteum and lead to infection. Normal nail growth has been cited to vary from less than 1.8 mm to more than 4.5 mm per month. The average fingernail growth is 0.1 mm per day, or 3 mm per month. This information is useful when determining the duration of nail pathology. For example, if splinter hemorrhages are located 6 mm from the proximal nail fold, it can be estimated that they occurred from injury approximately 2 months prior. Based on this growth rate, fingernails grow out completely in about 6 months. Toenails grow at one‐third to half of the rate of fingernails and take 12–18 months to grow out completely. Several factors affect the rate of nail growth. Age affects nail growth rate, with nail growth peaking at 10–14 years and declining after 20 years. Nail growth is proportional to finger length, with the fastest growth occurring in the third fingernail and slowest growth in the fifth fingernail, and faster nail growth has been noted in the dominant hand. Nails grow slower at night and during the winter. Other factors causing slower nail plate growth include lactation, immobilization, paralysis, poor nutrition, yellow nail syndrome, antimitotic drugs, and acute infection. Pregnancy, psoriasis, and nail‐biting are other factors linked to faster nail growth. Table 28.2 summarizes factors influencing nail growth. Table 28.1 Common nail signs associated with or helped by nail cosmetics. Figure 28.2 Diagram of the nail unit. Figure 28.3 Paronychia. The nail plate is composed mainly of keratin, which is embedded in a matrix of nonkeratin proteins. There is a wide variation in the reported percentage of inorganic elements found in the nail plate. Several elements, including sulfur, calcium, iron, aluminum, copper, silver, gold, titanium, phosphorus, zinc, and sodium, are constituents of the nail plate. Of these elements, sulfur, contained in the cysteine bonds that cross‐link nail plate keratin, has the greatest contribution to nail structure and comprises approximately 5% of the nail plate. Some studies attribute brittle nails to decreased cysteine levels. Cytokeratin 16 and 17 are present in normal nails but diminished in brittle nails [1]. There is a popular misconception that calcium content is responsible for nail hardness. However, calcium comprises less than 1% of the nail plate by weight [2], and no current evidence supports an association between calcium deficit and brittle nails or shows increased nail strength with calcium supplementation. In fact, in kwashiorkor, a condition of nutritional deficiency caused by insufficient protein intake, nails are thin and soft, and with increased nail plate calcium. The water content of the normal nail plate is reported to range between 10% and 30%. The most commonly accepted value is 18% water content in normal nails and 16% in brittle nails, though some studies also note no difference [3]. Lipids, including squalene and cholesterol, are also constituents of the nail plate and comprise 5% of the nail plate by weight. These lipids are thought to diffuse from the nail bed to the nail plate. The water‐binding capacity of brittle nails is less than that of normal nails which may be due to an abnormality in lipid content, keratin, or keratin‐associated proteins or lipid content [1, 4].
CHAPTER 28
Nail Physiology and Grooming
Introduction: nail physiology
Nail unit anatomy
Nail matrix
Nail folds
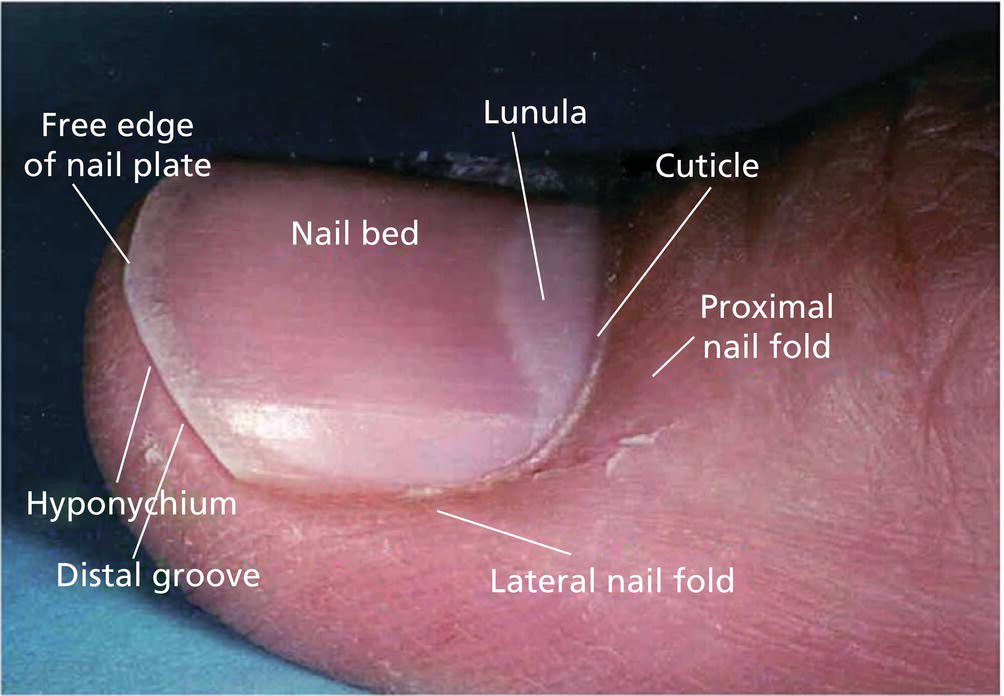
Hyponychium
Nail bed
Other structures
Nail growth
Nail sign
Definition
Association
Onycholysis
Separation of the nail plate from the nail bed
Vigorous cleaning of hyponychium exacerbates. Polish hides
Onychorrhexis
Increased longitudinal ridging
Associated with aging, distal notching. Polish may help
Onychoschizia
Lamellar splitting of the free end of the nail plate
Paronychia
Inflammation of the nail fold
Exacerbated by manipulation of cuticles and nail folds
Dyschromia yellow
Staining of the surface of the nail plate yellow from the dye in nail polish
Caused by repetitive or long‐standing polish use
Green/black discoloration
Pseudomonas is a bacterium that generates a green–black pigment that discolors the nail plate
Often associated with onycholysis and paronychia
Keratin granulation
White spots on the surface of the nail plate
Related to nail enamel especially in toenails when polish stays on nails for an extended time. Similar appearance to white superficial onychomycosis 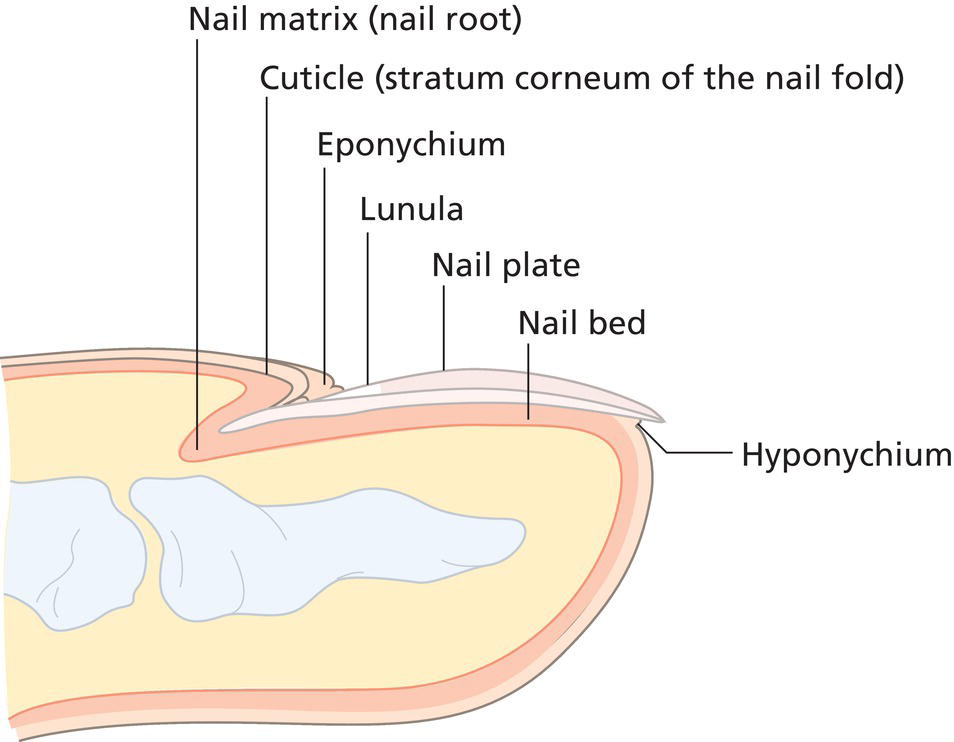
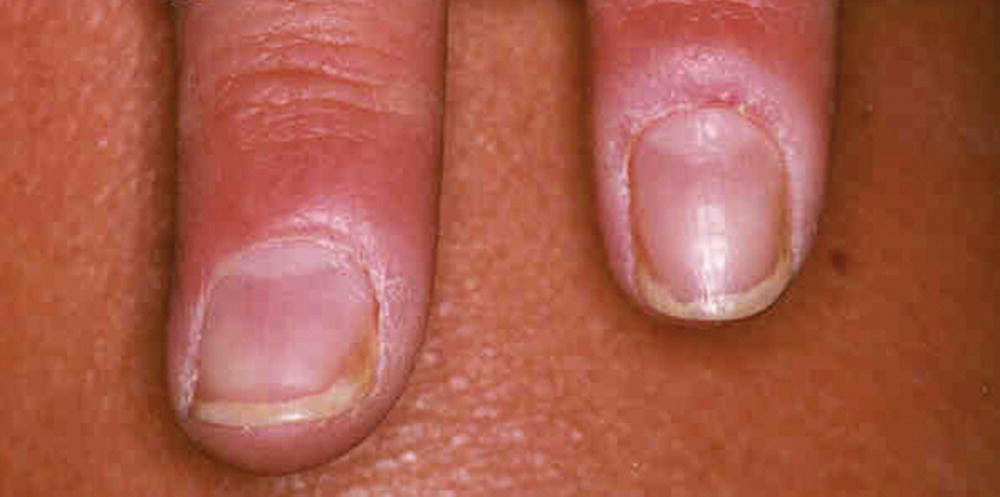
Physical properties of nails
Nail composition
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree