(1)
Yotsuya Medical Cube, Chiyoda-ku, Tokyo, Japan
Basic Principles
The palm of the hand is responsible for the important action of enclosing objects.
Therefore it is necessary to cover this area using tissue that is soft with sufficient thickness. It is not necessary to pro-actively pursue a sensory reconstruction, but if a similar tissue is used for reconstruction, it is possible to obtain a protective sensation.
Small skin defects can be covered using localized flaps. When creating localized flaps on the palm, the skin flap must be designed to be moved in a horizontal direction.
For large defect areas, although medial plantar flaps were previously preferred, this can lead to the formation of a sore on the donor area in the long term, and the use of a medial pedis flap creates less problems. For larger areas, the use of a pedicled or free thinned abdominal flap is practical.
Selectable Flaps and Surgical Procedures
V-Y advancement flapPedicled abdominal flapFree medial plantar flapFree medial pedis flapFree abdominal perforator flapUlnar parametacarpal flapReverse flow radial forearm flapHand relaxation incisionThe difficulty level of each surgical procedure is shown subsequent to the procedure title (e.g., Level of Difficulty: 2). The levels range from 1 to 5, with level 1 indicating a preliminary level and level 5 indicating a very advanced level.
5.1 V-Y Advancement Flap (Level of Difficulty: 1)
Information
Vascular pedicle Perforators of cutaneous branch from palmar digital artery.
Size Size based on the width of the skin defect area that can be transferred horizontally.
Advantage Same quality skin and scar is not obvious.
Caution In principle, V-Y plasty of the palm is created in a horizontal direction.

5.1.1 Operation Procedures
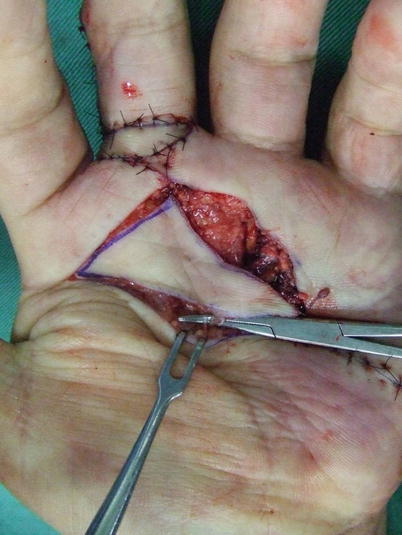
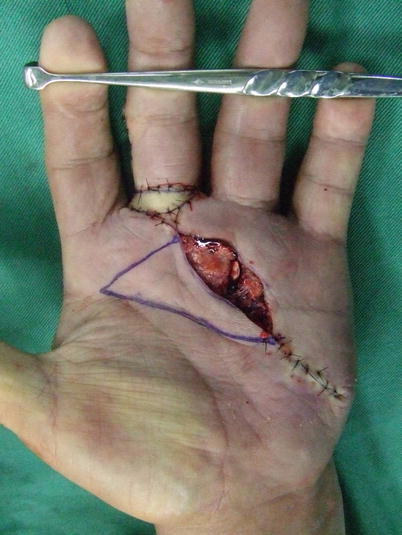
Fig. 5.1
Procedure 1: The skin flap is designed in a horizontal direction
Note
By designing a bigger skin flap there is more chance of multiple cutaneous branches being included in the flap, and it is possible to get more stretch out of the flap itself.
After first making an incision in the margin of the flap, an incision is then made in the palmar fascia.
Note
In this case example, a digitolateral flap is inserted in the base of the middle finger.
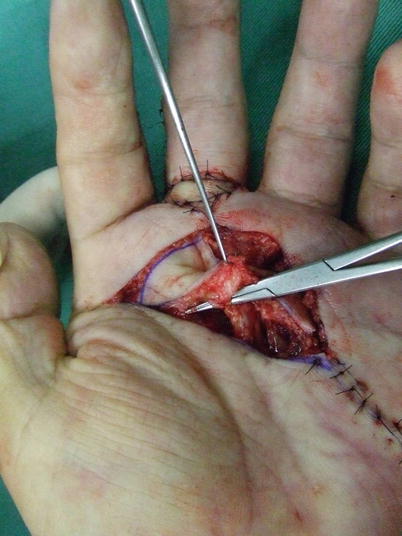

Fig. 5.2
Procedure 2: An attempt is made to move the flap, and if there is insufficient transfer distance, an additional incision is made in the stretched palmar fascia
Note
This method enables for easy transfer of the skin flap.
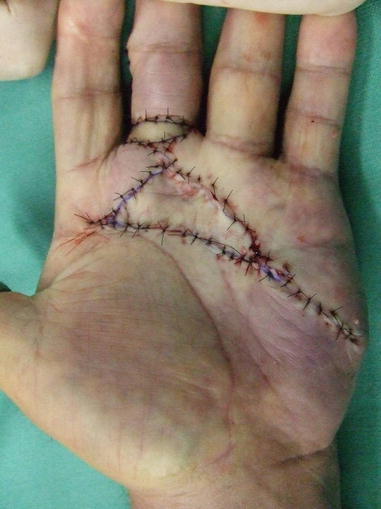
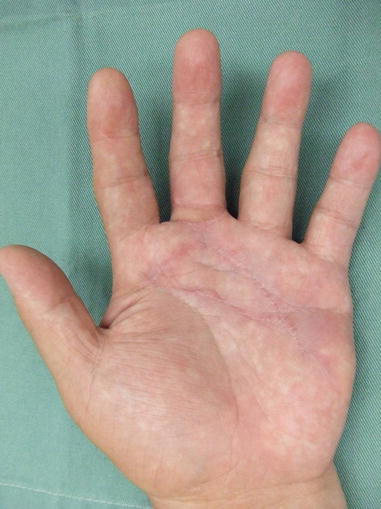

Fig. 5.3
Procedure 3: The wound is sutured closed from the distal part of the flap

Fig. 5.4
Procedure 4: Fluffy gauze is placed over the skin flap and a dressing applied with light pressure. There is no restriction of movement of fingers
Tips
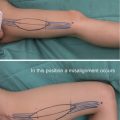
Flexion contracture tends to occur in triangular skin flaps of the palm that are transferred longitudinally.
Although there is no problem with regard to circulation based on the direction triangular skin flaps are created in the palm, flexion contracture of the fingers tends to occur when flaps are transferred longitudinally. A V-Y skin flap should only be created longitudinally when there is a long skin defect in a horizontal direction running parallel with the palmar crease. It is also difficult to see the scar when the flap is transferred horizontally.

5.2 Free Medial Plantar Flap (Level of Difficulty: 4)
Information
Vascular pedicle Superficial branch of medial plantar blood vessels.
Size Aligning with the section of the instep arch, a width of 5 cm and a length of 10 cm is available. If the medial pedis flap section is also included, the width can be increased by 3 cm.
Advantage Similar skin texture to the palm.
Disadvantage If the donor site is on a weight bearing area, tends to create a chronic sore. An arch support (worn in the shoes) is required to be worn over a long period.
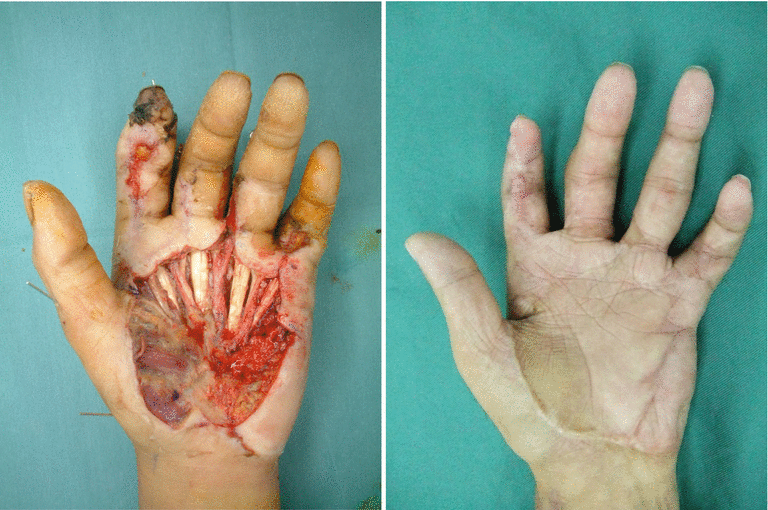

5.2.1 Operation Procedures
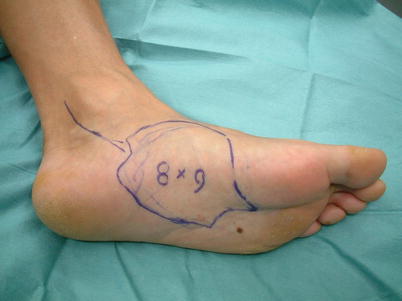
Fig. 5.5
Procedure 1: The flap is designed in line with the instep arch, but when larger flaps are required, the design is combined with the medial pedis flap including above the scaphoid tubercle
Note
If only harvesting the medial pedis flap, the flap is elevated with the deep branch of the lateral plantar blood vessels, but when combining the medial plantar flap and the medial pedis flap, then there is no issue with circulation if only using the superficial branch of medial plantar artery.
Refer to Section of
“Reconstruction of Calcaneal Region & Lateral Plantar Region/Medial plantar flap” in Chap. 18
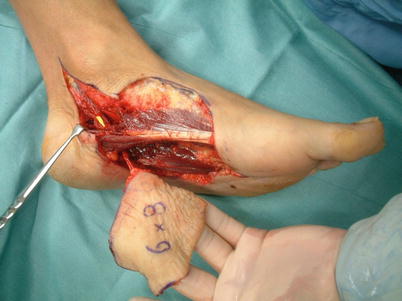
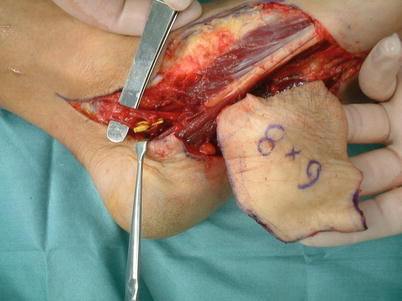

Fig. 5.6
Procedure 2: First, an incision is made in the posterior medial malleolus of the tibia, and confirmation is made of the posterior tibial blood vessels, which are then separated from the nerves. The incision is extended distally, with dissection continued down to the branching of the medial/lateral plantar arteries. The blood vessels are dissected from the reverse side while being careful to avoid cutting the abductor hallucis muscle. An incision is then made in the distal margin of the flap and dissection is made avoiding the toe nerves beneath the plantar fascia. It becomes enabling confirmation of the cutaneous branch of the blood vessels that enter the flap

Fig. 5.7
Procedure 3: The blood vessels beneath the abductor hallucis muscle are dissected and the deep branch of the medial plantar artery is ligated and cut
Note
The abductor hallucis muscle is not cut because doing so can cause hallux valgus post surgery.
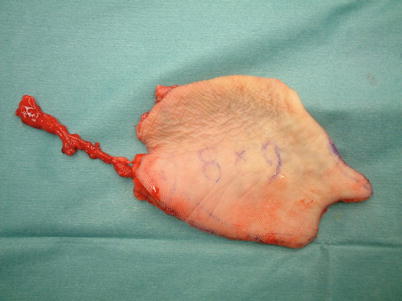
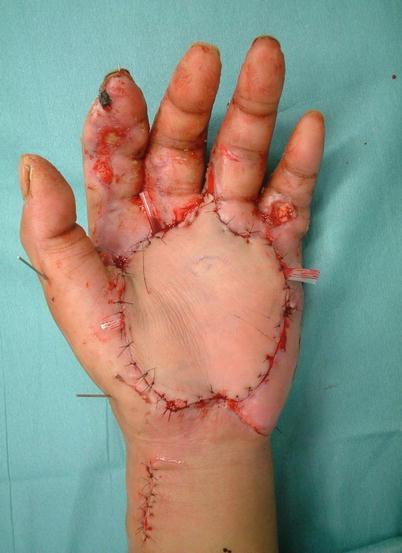

Fig. 5.8
Procedure 4: The posterior tibial blood vessels are severed with the required length, and the flap harvested with the vascular pedicle passed beneath the abductor hallucis muscle

Fig. 5.9
Procedure 5: The flap is sutured in place and anastomosis conducted with the posterior tibial blood vessels to the radial blood vessels
Note
If possible, end-to-side anastomosis is performed for the arteries.
A drain tube is inserted in the margin of the flap.
Tips
A split-thickness skin graft is performed on the donor site, and a compression dressing applied.
The patient is instructed to walk with an arch support in their shoes for several months following surgery.
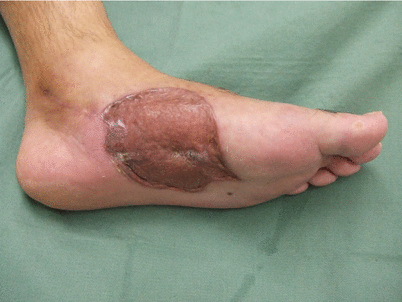

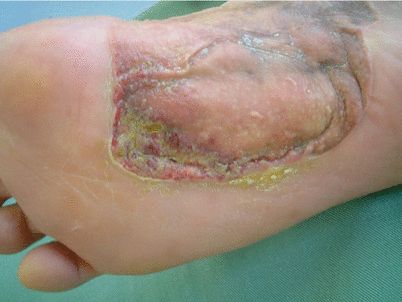
Tips
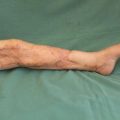
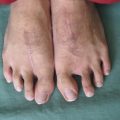
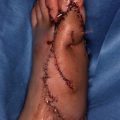
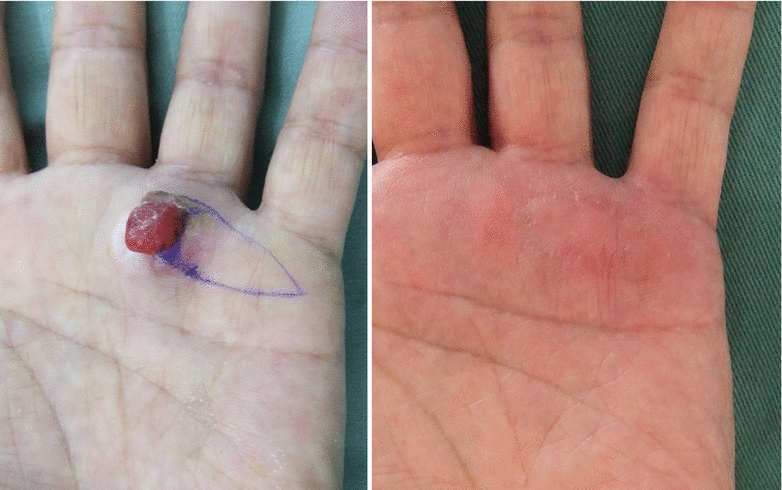
The biggest problem of medial plantar flaps is in the donor site.
Even if the flap is created so as to avoid the weight bearing area, if the patient stops wearing the arch support, then they tend to develop a sore. It is necessary to get the patient to understand that arch supports for the shoes should be worn at all times. Also, for patients employed in jobs that require them to walk on gravel roads or similar, it is best to avoid selecting this flap.
Photo is of sore that still re-occurs 5 years after surgery.

5.3 Free Medial Pedis Flap (Level of Difficulty: 4)
Information
Vascular pedicle Medial branch of deep branch of medial plantar artery.
Size Width of around 3 cm and length of around 7 cm centered around the scaphoid tubercle.
Advantage Comparatively thin, flexible and suitable for small skin defects of the palm.
Possible to retain the lateral plantar blood vessels and use only the medial plantar arteries. Patient not required to wear an arch support.
Disadvantage Cannot be a sensory flap. Not suited to covering a large area on the palm.
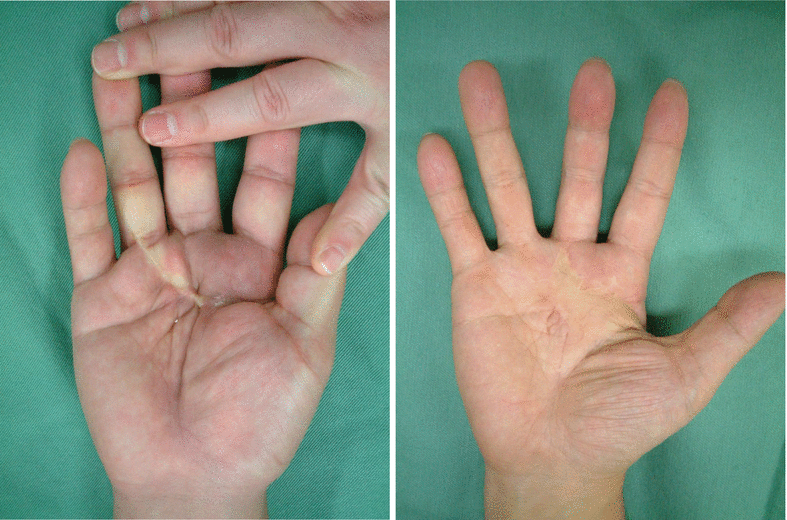

5.3.1 Operation Procedures
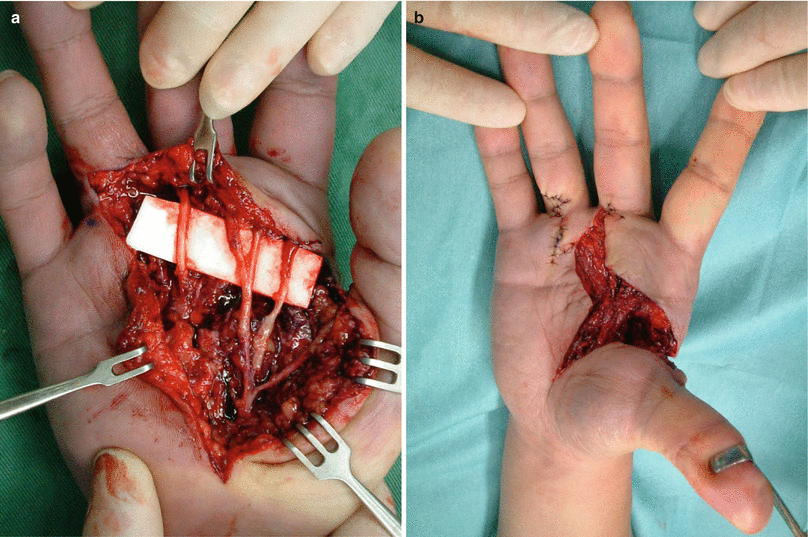
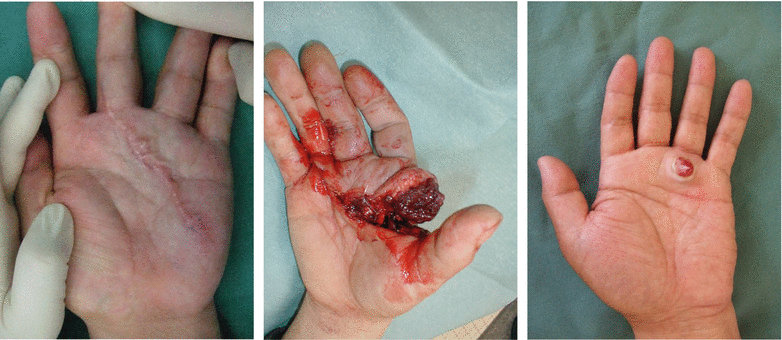
Fig. 5.10




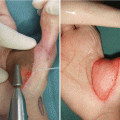
(a, b) Procedure 1: Scar on palm is resected and a free nerve transplant harvested from the forearm was performed. Skin defect present from palm to first web space area
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree