(1)
Department of Dermatology, University of Pennsylvania, Penn Presbyterian Medical Center Medical Arts Building, Philadelphia, PA, USA
17.1.1 Neurotoxins
17.1.2 Fillers
17.1.3 Peels
17.1.4 Lasers
17.1.5 Phototherapy
17.1.6 Photodynamic Therapy
17.1.7 Sclerotherapy
17.1.8 Dermabrasion
17.1.10 Liposuction
17.2 Surgery
17.2.1 Anatomy
17.2.2 Antiseptics
17.2.3 Sterilization
17.2.4 Pre-surgery Medication
17.2.5 Wound Healing
17.2.6 Wound Dressings
17.2.7 Mohs Surgery
17.2.8 Indications for Mohs Surgery
17.2.9 Reconstruction
17.2.10 Healing by Secondary Intention
17.2.11 Flaps
17.2.12 Grafts
17.2.13 Sutures
17.2.14 Safety/Needlesticks
17.2.15 Other Surgical Rules
17.2.16 Margins
17.2.17 Cryosurgery/Cryotherapy
17.2.18 Electrosurgery
Abstract
This section reviews the most high yield facts regarding procedures in dermatology, including cosmetics and surgery.
Keywords
CosmeticsSkin SurgeryLasersNeurotoxinsProcedural Dermatology17.1 Procedures and Cosmetics
17.1.1 Neurotoxins
Botox (onabotulinumtoxin A):
Mechanism: binds SNAP-25 (BTX-1) or other SNARE complex protein (such as synaptobrevin (VAMP) by BTX-2). The SNARE complex is responsible for allowing neurotransmitter (acetylcholine) vesicle fusion at neuromuscular junction (postsynaptic cholinergic)
Duration: takes 24–72 h to start effect, full effect by 2 weeks, lasts 3–5 months
Use: for wrinkles (approved for moderate/severe glabellar lines and lateral canthal lines, all other wrinkles off-label), primary axillary hyperhidrosis; originally for strabismus, blepharospasm, cervical dystonia, recently approved for migraine headaches
Muscles of the brow:
Depressors (4): procerus, orbicularis oculi, depressor supercilli, corrugator supercilli
Elevator: frontalis
Associated effects: ptosis (if affect levator palpebrae superioris, so inject at least 1 cm above superior orbital rim, avoid lateral aspect above brow), lip drop (if affect zygomaticus major/minor – be careful when injecting lateral/inferior orbicularis oculi)
Other neurotoxins:
Dysport (abobotulinumtoxin A) = ~2.5–3:1 conversion ratio with Botox
Xeomin (incobotulinumtoxin A) = 1:1 conversion ratio with Botox
17.1.2 Fillers
Semi-permanent fillers:
Bovine collagen (Zyderm)
Hyaluronic acid (Restylane, Juvéderm)
Derived from bacterial fermentation of Streptococci
Poly-L-lactic acid (Sculptra) (longer-lasting)
Works by stimulating collagen production (collagen neosynthesis)
Calcium hydroxyapatite microspheres (Radiesse) (longer-lasting)
Permanent fillers:
Polymethylmethacrylate beads suspended in bovine collagen (Artefill, rebranded as Bellafill)
Risks: nodules/granulomatous reactions
Danger areas:
Glabella
Risk of glabellar necrosis
Risk of embolization to ophthalmic artery and blindness due to retrograde movement of material (more likely if injecting in tear trough)
Nasolabial folds
Risk of vascular occlusion of angular artery
17.1.3 Peels
Alpha hydroxy acids = trichloroacetic acid (TCA), glycolic acid; can penetrate into dermis depending on concentration and anatomic location
Glycolic acid peels must be washed off with water or neutralized with sodium bicarbonate; TCA frosts and does not neutralize, and rinsing is only for patient comfort
Beta hydroxy acids = salicylic acid (the only one); can enter sebaceous unit, only penetrates stratum corneum; good for acne
Jessner solution = salicylic acid, lactic acid, resorcinol in ethanol
Phenol = a deeper peel, but given risk of arrhythmias from systemic absorption, need constant EKG monitoring (almost nobody uses phenol because of this risk); also has risk of acute kidney injury
17.1.4 Lasers
Basic principles
LASER = Light Amplification by Stimulated Emission of Radiation
Lasers are monochromatic, high intensity, coherent (in phase), and collimated (in parallel)
Three main chromophores: water, hemoglobin, and melanin
These chromophores all absorb best at different wavelengths. The principle is to choose a laser wavelength which will be absorbed by your target chromophore and not be absorbed by the chromophores you wish to leave unaffected (principle of selective photothermolysis).
The higher the laser wavelength, the deeper it penetrates into the skin (however, once above 1300 nm, water absorption in stratum corneum limits penetration)
If you are targeting a specific color pigment as a chromophore, the best laser should have a different color from the target. The color of an object reflects the wavelengths of light it does not absorb, and thus how it appears that color to our eyes. The ideal laser color may be the opposite end of the color wheel.
Thermal relaxation time = time required for chromophore to cool to 50 % of heated temperature; dependent on square of diameter of chromophore
Pulse duration = must equal or be less than thermal relaxation time; if too long, heat will diffuse and damage normal tissue
In order to eliminate pigment, one should use a q-switched laser, which uses a very short pulse duration (nanoseconds as opposed to milliseconds) and effectively targets the melanosome
In hair removal, melanin is the target chromophore; thus it follows that the ideal patient for hair removal is a light skinned person with dark hair. In dark-skinned patients, it could be hard to remove hair without causing hypopigmentation of the skin as well. That said, a deep penetrating laser (higher wavelength) should target dermal > epidermal pigment. E.g. could use a Nd:Yag laser in type IV skin for hair removal. Also, a long pulsed laser is recommended, as a longer pulse duration is needed for heat to go from the hair follicle to the stem cells in the bulge
In laser skin resurfacing, high wavelength lasers are used for their higher coefficient of absorption for water
Fractional laser resurfacing = produces microcolumns of damage with normal surrounding skin, allows for faster healing
To increase depth of laser penetration, in general: increase wavelength, spot size (less photo scatter), and pulse duration
Terms:
Fluence = energy per unit area for a single pulse = J/cm2 (fluence = irradiance x time)
Irradiance = power per unit area for a single pulse (power density) = W/cm2
Energy is proportional to frequency; frequency and wavelength are inversely proportional
Know the UV spectrum:
Below 400 nm = ultraviolet light
400–700 nm = visible light
Above 700 nm = infrared light
Know the absorption spectra of hemoglobin, melanin, and water (Fig. 17.1):
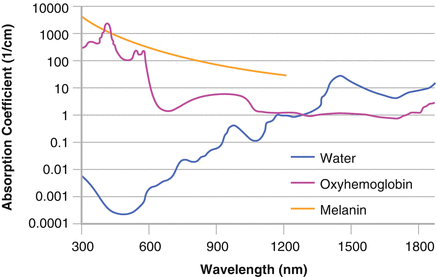
Figure 17.1
Laser absorption spectra for hemoglobin, melanin, and water
Hemoglobin (oxyhemoglobin): absorbs best at 500–600 nm (peaks at 540 (alpha peak) and 580 (beta peak))
Melanin: absorbs at 300–1000 nm, though generally target 600–800 nm when specifically targeting pigment to avoid hemoglobin absorption
Water: absorbs best above 1000 nm
Toxicities/complications:
Ocular toxicity:
Cornea absorbs like water (damage with Er:YAG and CO2)
Retina (rod and cones) absorbs like melanin (damage with lasers in melanin spectra)
Tattoo removal complication:
Can see paradoxical darkening of tattoos containing beige, red, white or light brown color; thought to be from reduction of ferric oxide to ferrous oxide, leading to immediate gray-black color.
Purpura:
Short pulse durations effectively target in PDL, but may lead to purpura, which can be reduced with greater pulse durations.
Know the commonly used lasers:
Excimer: 193 nm, 308 nm, 355 nm (in UV range, can cause cataracts)
Argon: 488 nm, 514 nm (green) – risk of scarring
KTP: 532 nm (green)
Pulsed dye laser (PDL): 585–600 nm (yellow) = good for vascular lesions
Ruby: 694 nm (red)
Alexandrite: 755 nm
Diode: 800 nm, 810 nm
Nd:YAG: 1064 nm, 1320 nm (frequency-doubled Nd:YAG = 532 nm)
Er:YAG: 2940 nm
CO2: 10,600 nm
Intense Pulsed Light (IPL): 500–1200 nm (not a laser; can use filters to narrow wavelength range)
Note:
UVB = 280–320 nm, UVA-2 = 320–340 nm, UVA-1 = 340–400 nm,
Soret band = 400–410 nm (blue); Oxygen (ozone) absorbs UVC 100–200 nm
Shortest UV wavelength = infrared
Longest UV wavelength = radiowaves
17.1.5 Phototherapy
UVB phototherapy (NBUVB = 311 nm)
Light therapy without any photosensitizers
Mechanism = reduces DNA synthesis, induces expression of tumor suppressor p53, various cytokine release; this would explain how it works in psoriasis; in CTCL, may work by impairing Langerhans cell function
Indications = psoriasis, CTCL, vitiligo; also atopic dermatitis, GVHD, PLEVA/PLC, pruritus
MED (minimal erythema dose) = lowest dose that causes minimally perceptible erythema; this peaks at 24 h, so doses may be increased with each treatment
Efficacy = UVB inferior to PUVA, but NBUVB may be nearly as effective
UVA-1 phototherapy (UVA-1 = 340–400 nm)
Indications = sclerotic diseases (morphea, eosinophilic fasciitis, chronic GVHD, lichen sclerosus) thought to have greater penetration, less carcinogenic risk than PUVA
Mechanism = Unclear, but may upregulate matrix metalloproteinases (collagenase) and decrease production of collagen
PUVA/Psoralen (UVA = 320–400 nm)
Background: Psoralens = naturally occurring linear furocoumarins found in a number of plants. In PUVA (Psoralen + UVA), typically use 8- methoxypsoralen (8-MOP), which is orally ingested or applied topically; 5-MOP is less efficacious, but has fewer side effects
Mechanism: In the absence of UV, psoralen intercalates with DNA. With absorption of UVA photons, this leads to cross-links with the pyrimidine bases and the production of reactive oxygen species. It is thought that this interaction with DNA inhibits replication and causes cell cycle arrest. Some effects even in absence of DNA crosslinks.
Specifically, mechanism in three steps:
1.
In absence of UV radiation, psoralen intercalates into DNA strand.
2.
Absorption of UVA photons results in formation of 3,4 or 4’,5’ cyclobutane monoadduct with pyrimidine bases of native DNA.
3.
The 4’,5’ monoadducts can absorb a second photon, which leads to an interstrand crosslink with the 5,6 double bond of the pyrimidine base of the opposite side.
Side effects = nausea/vomiting (from 8-MOP), erythema (peaks 72–96 h after exposure), pigmentation, pruritus, cataracts (eye protection mandatory), long-term risk of photocarcinogenesis (though perhaps not as much as once feared)
17.1.6 Photodynamic Therapy
Photosensitizer + photoactivating light + target cell + tissue oxygen
PDT works by producing cytotoxic oxygen radicals (primarily singlet oxygen, 102) from photoactivation. These lead to the therapeutic response. Singlet oxygen is one of the most potent oxidant species and may cause oxidative damage that leads to cell death.
Light source: must have wavelength >400 nm (to limit UV light penetration, avoiding photocarcinogenesis), but <800 nm.
Absorption spectrum of protoporphyrin IX has blue (417 nm) and red (630 nm) peaks
Indications: actinic keratoses, superficial BCCs; also acne, photoaging, MF, CTCL
Topical ALA + red light approved for tx of BCC, AKs, SCC; topical ALA + blue light approved for tx of AKs.
Photosensitizers:
5-ALA (5-aminolevulinic acid) and methyl-esterified ALA (mALA)
Mechanism:
In a way, causing a transient iatrogenic erythropoietic protoporphyria
5-ALA (pro-drug) → protoporphyrin-IX (wait an hour after application to apply light; conversion can be checked with Wood’s lamp). On exposure to light, singlet oxygen species may be produced. The 5-ALA is preferentially absorbed by cells with high turnover; stops at protoporphyrin-IX since lack next enzyme in cascade.
17.1.7 Sclerotherapy
Indications: telangiectasias and reticular veins
Agents:
Detergents (sodium tetradecyl sulfate = Sotradecol)
Disrupt vein membrane
Osmotic agents (hypertonic solution)
Damage cells by shifting water balance
Chemical irritants (glycerin)
Damage cell wall by direct destruction
Greatest risk of arterial clot = injection into popliteal fossa
17.1.8 Dermabrasion
Microdermabrasion and mechanical dermabrasion are techniques for resurfacing skin defects; most commonly used for treatment of acne scarring
Recommendations are to wait 6–8 weeks post-surgery, 6–12 months post-isotretinoin (may be more than necessary)
Risk of scarring greatest over bony prominences (e.g. mandible)
17.1.9 Hair Transplantation (Follicular Unit Transplantation)
Techniques of restorative surgery to relocate hair follicular units
Should not be done on patients who are too young or have too diffuse hair loss
Requires aesthetic sense for hairline design, anticipation of future hair loss
Donor strip may be harvested using triple-bladed scalpel, typically done from posterior scalp
17.1.10 Liposuction
A technique for removal of fat; not a treatment for obesity
Uses tumescent anesthesia with lidocaine; allows large volumes of fat to be removed with minimal blood loss
Contraindications include bleeding disorders
17.2 Surgery
17.2.1 Anatomy
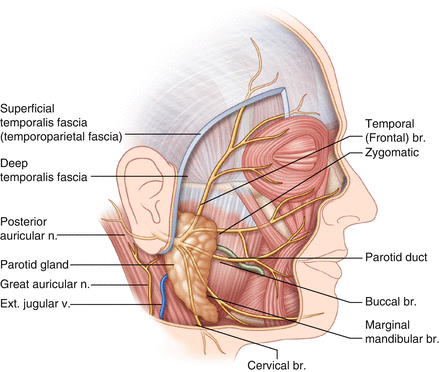
Anatomy of the face: nerves, arteries, veins
Get Clinical Tree app for offline access
Motor innervation of muscles of facial expression = facial nerve (Fig. 17.2)