Chapter 25. Principles of Approaches in Secondary Rhinoplasty
Ronald P. Gruber, MD; Meryl Singer, MD; Kenton Fong, MD
INDICATIONS
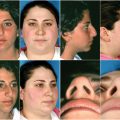
The indication for performing a secondary rhinoplasty depends upon whether the needs of the patient are reasonable and can be met by the surgeon. Photographic imaging analysis is extremely helpful in making this determination as it allows the surgeon to give the patient some idea of what can be done and allows the patient to give feedback as to what the patient does or does not like about the imaged result. It is often prudent not to attempt major revisions for at least one year after the most recent nasal surgery, although earlier surgery may be performed with the understanding that the desired final result may be more difficult to obtain. Evaluation of the nasal skin quality is one of the most important initial considerations. Very-thick-skin patients are less amendable to the open rhinoplasty approach because the transcolumellar incision aggravates postoperative edema and causes subsequent fibrosis that mars the final sculpted result. One common subset of secondary rhinoplasty patients that is useful for illustrative purposes is the overresected short-nose patient. These cases often require dorsal augmentation, septal extension grafts, tip grafts, spreader grafts, columellar strut, intercartilaginous grafts, rim grafts, and suture techniques, all of which illustrate secondary rhinoplasty techniques in general.
PREOPERATIVE PREPARATION
Most patients require at least 2 consultations prior to surgery. The most important aspect of the informed consent is warning the patient that a touch-up or revision might be necessary. This occurs in at least 20% of cases. On the morning of surgery, it is important that the surgeon has thought out a clear game plan prior to beginning the operation. It can be extremely helpful to perform mock surgery with the photo imager before going to the operating room.
ANESTHESIA
Most rhinoplasties can be performed under conscious sedation. Intramuscular Vistaril (hydroxyzine HCl) 100 mg (for its antiemetic effect) and an analgesic, for example, Demerol (meperidine HCl) or Nubain (nalbuphine HCl), are given in the preoperative holding area. Intraoperatively, the patient receives intravenous Versed (midazolam HCl) as needed to achieve adequate sedation as well as a onetime dose of intravenous ketamine 30 to 50 mg prior to local anesthetic injection. The dose of ketamine allows for 5 minutes of complete dissociation during the normally unpleasant injection process. Local anesthesia consists of a mixture of Xylocaine and Marcaine (bupivacaine HCl) with fresh 1:200,000 epinephrine concentration. If general anesthesia is used, the concentration of epinephrine may be increased to 1:100,000. To facilitate elevation of the nasal skin flap and minimize the risk of skin perforation, the nose is typically hyperinfiltrated with 20 to 30 mL of local anesthetic in the subcutaneous space, septal mucosa, and turbinates. Using this technique, no topical anesthetics are necessary and osteotomies may be performed.
POSITION AND MARKINGS
The patient is positioned in the supine position and the face is prepped with Castile soap or dilute Betadine (povidone-iodine). Working with loop magnification makes it difficult to appreciate the gestalt of the sculpted result. Therefore, it is ideal to have a video camera and monitor in the operating room that give the surgeon a true lateral view of the patient. Otherwise, it is helpful for the surgeon to occasionally walk to the other side of the patient to get a fresh perspective. For open rhinoplasties, an inverted V incision at the narrowest point in the columella is used unless the patient has a different scar from the primary surgery.
DETAILS OF PROCEDURES
Most secondary rhinoplasties need adequate exposure in order to perform detailed and accurate sculpting of the underlying framework; consequently, most major secondary rhinoplasties require an open approach. As mentioned above, to facilitate elevation of the flap with minimal risk of skin perforation the nose is hyperinfiltrated with 20 to 30 mL of local anesthetic into the subcutaneous space, septal mucosa, and turbinates.
Soft-tissue Release to Lengthen the Nose
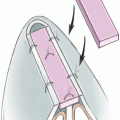
The anterior septal angle is exposed first because it is easiest to locate when there is significant scar tissue. From there the mucoperichondrium is elevated off the caudal septum and the upper lateral cartilages are released from the dorsal septum (Figs. 25-1 to 25-3). A double hook is placed on the tip cartilages to retract the lower lateral cartilages (LLCs) from the upper lateral cartilages (ULCs). Using a pair of scissors, a gap is created between the ULCs and LLCs (Fig. 25-4).
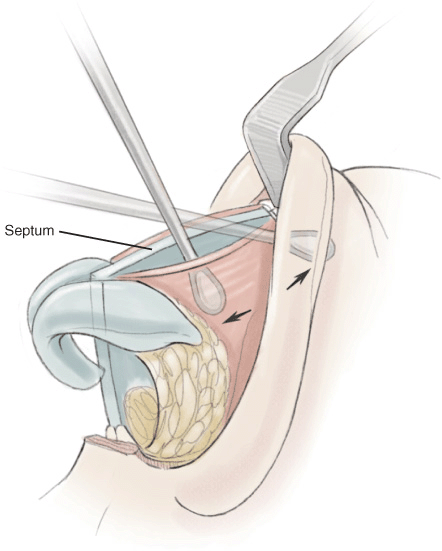
Figure 25-1 Schematic of releasing upper lateral cartilage and septal mucoperichondrium.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree