Parastomal hernia risk factors
Obesity/waist size
Concomitant incisional hernia
Increased intraabdominal pressure
Chronic obstructive pulmonary disease
Postoperative sepsis
Age
Cigarette smoking
Malnutrition
Emergency surgery
Colostomy
Steroids
In recent years it has been suggested that prophylaxis against hernia at the time of the original surgery with mesh reinforcement of the stoma either in an onlay [11] or sublay [12] position may reduce the risk of development of a parastomal hernia. In this respect, waist circumference has been shown to be an independent risk factor for the development of parastomal hernia, although as yet in this select group there is little conclusive evidence that the rate of hernia is affected by definitive use of prophylactic mesh, its technique of deployment, or the operative approach utilized [9]. Early results in nonobese patients thus far have been moderately promising, with a major decrease in the incidence of parastomal hernia, especially when the mesh is placed in the posterior sublay position, namely, posterior to the rectus muscle but above the posterior rectus sheath. Long-term follow-up is required to assess both the efficacy of prophylactic mesh and to address the ultimate risk of mesh erosion as well as other potential mesh-related problems when its deployment is routine. In this regard, clinical trials of biologic meshes in the prophylactic setting are ongoing. If prophylactic mesh is indeed shown to be a safe and effective approach in adequately powered trials with long-term follow-up, the main issues to be determined will be the most appropriate type of material to be used and its optimal location of placement.
Surgical Approach
Surgery is required in patients who develop obstruction or unacceptable pain or who present with pouching problems that cannot be adequately managed with enterostomal therapy. Perhaps the first question to be asked is whether the patient can have their ostomy closed. Notably, if the patient has undergone a Hartmann’s procedure in the past, stoma take-down may actually be the best way to deal with the coincident hernia. Any repair of the parastomal hernia will necessitate preservation or creation of an abdominal wall defect to permit exit of the bowel, and elimination of the ostomy altogether would provide the best chance for a durable closure of the abdominal wall.
Unfortunately, in many patients, closure of the stoma is not an option and formal parastomal hernia repair is required. In this group of patients, collated results have been remarkably poor over the years. Commonly utilized approaches have included local tissue repair, stoma relocation, and repair with prosthetic materials. Repairs of local tissue defects have been associated with a 46–100 % recurrence rate. Stoma relocation also has had a relatively poor track record but remains useful if the existing stoma location is no longer useable or satisfactory. In addition to recurrent hernia at the new site, there is a considerable incidence of herniation at the old stoma site or the midline wound if formal laparotomy is performed, as is commonly required with stoma relocation. Rubin and colleagues [13] have reported a 76 % recurrence rate for local tissue repair and a 36 % recurrence rate for stoma relocation.
It seems evident that repair with prosthetic material is the best available option. However, it remains uncertain what type of mesh should be used and what is the optimal position for placement. The mesh may be placed in an underlay position (intraperitoneal), above the peritoneum but beneath the fascia (extraperitoneal), or as a fascial onlay. If the mesh is placed intraperitoneally, the bowel may be placed through the mesh (i.e., the keyhole technique) or lateral to the mesh as described by Sugarbaker [14, 15]. Generally speaking, it seems to be preferable to place the mesh in an underlay position, where intra-abdominal pressure tends to keep the mesh in place when positioned beneath the abdominal wall, whereas the mesh is “outside” the pressure gradient in the onlay position. Recurrence rates for intraperitoneal placement have been superior to a mesh placed in the onlay position [16].
Lateralization of the stoma has had superior results when compared with the keyhole technique because the slit in the mesh tends to widen over time [17]. In this respect, Hansson and colleagues [18] have reported a 37 % hernia recurrence rate at a median of 36 months utilizing a keyhole in an expanded polytetraflouroethylene patch. Using the same mesh material without a slit, Mancini et al. [19] reported a 4 % recurrence rate at 19 months. The Sugarbaker, or lateralization technique, secures the bowel to the lateral abdominal wall without a slit or keyhole, covering it with mesh to supposedly create a “flap valve.” Theoretical concerns about obstruction with this technique do not seem to be a major issue in actual clinical experience; however, concerns about mesh erosion [20, 21] in all locations have spurred an interest in the utilization of biologic mesh [22], with the preferred capacity for biologic mesh to resist infection making its use particularly appealing in infected cases. The ideal mesh combining adequate strength, minimal tissue reactivity, tissue in-growth, reasonable cost, and ease of use remains to be defined.
The Authors’ Approach
Our practice is to avoid operating on a parastomal hernia unless absolutely necessary. When surgery is indicated and stoma closure is not a good option, we typically consider laparoscopic placement of synthetic mesh in the sublay position to be the preferred option. Patients who are reasonably healthy, who do not have an exceptionally hostile abdomen, and who can tolerate pneumoperitoneum are selected for laparoscopic mesh repair via an intraperitoneal exposure. Many of these patients have a concomitant incisional hernia that is repaired at the same time.
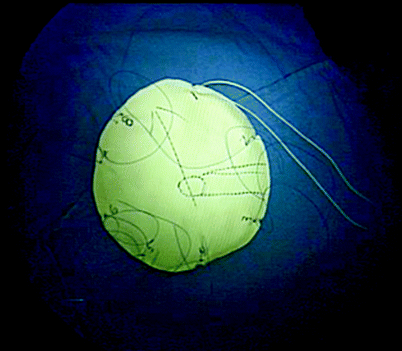
A blanket or roll is used to elevate the ipsilateral hip to secure access to the flank for lateral mesh coverage. The stoma may be closed with a purse string suture to prevent enteric contents from contaminating the surgical field. The stoma is then covered with gauze to absorb mucus and the entire abdomen is covered by an Ioban dressing that isolates the stoma and prevents mesh contamination when the mesh comes in contact with the abdominal wall (Fig. 44.1).
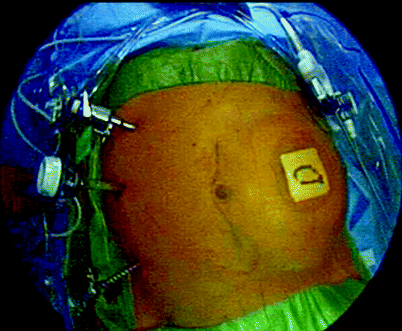

Fig. 44.1
Surgical set-up showing location of ports opposite the colostomy site
Access to the peritoneal cavity should be obtained on the side opposite the stoma. A Veress needle technique to insufflate the abdomen is most helpful for obese patients. We prefer an optical trocar for first access if the Hasson open technique is not used. Three ports are placed on that side to facilitate the dissection. An angled laparoscope (we use a 5-mm, 30° scope) will optimize the view of the abdominal wall lateral to the stoma limb as well as any bowel loops. Adhesions are taken down from the abdominal wall, which is inspected for a concomitant incisional hernia. If present, a single mesh is used to cover both defects.
Great care is taken to avoid bowel injury during adhesiolysis. Often, most of the bowel in the defect reduces with internal traction and external counter-pressure on the hernia. Thermal energy sources during adhesiolysis are avoided to prevent capacitance coupling of the laparoscopic instruments and injury to other bowel loops or the stoma limb itself. It sometimes can be difficult to discern the stoma limb from the surrounding bowel. The stoma limb, as well as the mesentery with its associated blood supply, must be preserved or the stoma could be at risk for devascularization (Fig. 44.2).
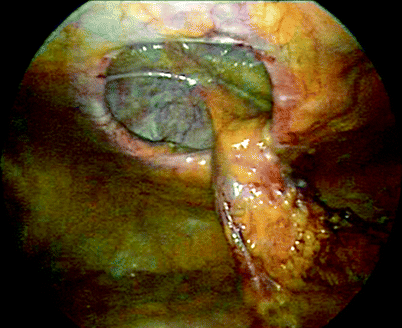

Fig. 44.2
Parastomal hernia with fascial defect and stoma limb
Occasionally, an assistant’s finger can be used to digitalize the stoma for identification of the bowel leading to the ostomy and to aid in developing a plane between the bowel loops and the stoma limb itself. After all adhesions are taken down from the abdominal wall, the fascial defect is marked on the skin. Measuring at least 5 cm past the defect, an expanded polytetraflouroethylene mesh is chosen and cut to size. A ruler placed intracorporeally helps to precisely measure the size of the mesh required for parastomal hernia repair (Fig. 44.3). Because stomas are typically off the midline on the abdominal wall, the stab incisions corresponding to the appropriate anchoring suture will need to be placed even further laterally to avoid excessive mesh laxity. A spinal needle passed through the lateral abdominal wall can help pinpoint the expected position of the lateral edge of the mesh, and the stab incisions in the skin for suture placement can be positioned accurately. Permanent anchoring sutures are placed at the periphery of the mesh at approximately 6-cm intervals (Fig. 44.4). The stoma site is marked on the mesh as well as the path of the limb, which will run anterior to the mesh. This will aid in placement of the lateral anchoring sutures and will help avoid placing tacks in or near the stoma limb itself.
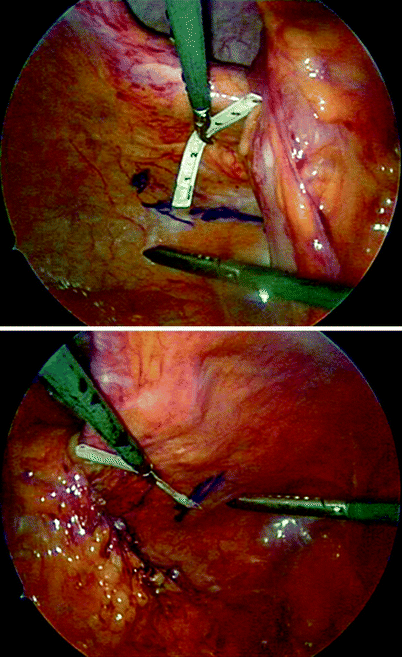

Fig. 44.3
Using a ruler helps to precisely size the mesh