Chapter 45. Hair Transplantation
Alfonso Barrera, MD, FACS
In the past 25 years, great advances have occurred in techniques of hair transplantation for the treatment of male pattern baldness, allowing for natural and aesthetic results. The most significant change has been the ability to transplant a large number of significantly smaller grafts (follicular unit grafts) in an artistic way that mimics nature.
This technique gradually evolved from the traditional hair plugs to the use of follicular unit grafts, which have become the gold standard today. The original hair plug or punch graft technique was described by Orentrech in 1959 for the treatment of male pattern baldness, and was the standard of care for many years. These 4-mm plugs contained 10 to 20 hairs and resulted on an artificial “corn row” appearance. We learned a lot from the use of hair plugs, specifically the “donor dominance concept,” that is the fact that the longevity of hair growth is dependent on the genetic programming of the hair follicles (hair roots) of the donor area. The success of hair transplantation today rests on this concept: Transplanted hair will continue to grow on the transplanted site as long as it was going to do so on the donor area. Male pattern baldness occurs primarily on the top of the head and not on the occipital or temporal areas. The hair follicles on the top of the head are genetically sensitive to dehydrotestosterone (DHT), whereas the hair follicles on the occipital and temporal areas are not. This feature is maintained as they are transplanted to the bald area.
As the use of smaller and more numerous grafts were introduced, much better results were obtained. The first report of the use of single hair grafts on the scalp was that of Nordstrom in 1980. He described the benefit of such grafts camouflaging the scarring and unnatural appearance of hair plugs, finally allowing for natural-looking results. It was very time consuming working at the front hairline and it did not seem feasible at the time that the entire area of baldness could be treated with such small grafts. Uebel, in 1991, reported his technique using micrografts (1 to 2 hair grafts) and minigrafts (3 to 4 hair grafts) in large numbers (1000 to 1200 grafts) per session to graft large areas of hair loss such as the entire top of the head in cases of male pattern baldness (MPB).
In 1993, I became interested in hair transplantation based on the work of Nordstrom and Uebel, and this has become the most common procedure in my practice today. The key for a natural result has been doing a large number of very small grafts and using finer instrumentation to avoid detectable scarring both on the transplanted area, and on the donor site.
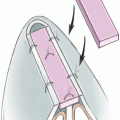
In 1984, Headington reported an interesting anatomical finding on hair follicle anatomy. He studied horizontal sections of scalp and found that hair follicles come in anatomic units of 1, 2, 3, or 4 hairs; they have their own blood supply, sebaceous glands, sweat glands, piloerectile muscle, and innervation and are surrounded by a sheath of collagen. This configuration is what we know as follicular units. They appear to be true physiologic units. As long as you do not use grafts larger than these the results are very natural looking. Of course, it is also important to transplant them artistically in terms of orientation and direction of hair growth.
There is a variable nomenclature regarding grafts, the most logical and common today is “follicular unit grafts,” as mentioned above.
I have been working on improving the technique by further increasing the number of grafts transplanted in a single session, I frequently do well over 2000 and have done as many as 2900 in a single session for MPB patients, which works out to be approximately 6000 hairs in a single session.
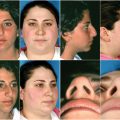
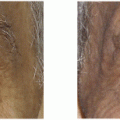
I have found additional applications restoring natural looking hair in reconstructive cases such as iatrogenic alopecia (ie, as a result of facelift procedures), but also alopecia caused by burns, accidents, tumor resections, congenital deformities, etc.
PATIENT SELECTION
To date, we have no method to create new hair. All current techniques for hair restoration involve redistributing the patient’s existing hair. Therefore, to be a candidate, the patient must have a favorable ratio between the donor-site surface area and density relative to the size of the area to be transplanted. Patients who have a higher donor density and a larger potential donor site area (occipital and temporal areas) and a smaller the surface area to be grafted have optimal ratios.
Unfortunately, MPB is a progressive condition. The rate of hair loss may slow down after the age of 40 years, but it never stops completely.
Therefore, the preoperative plan must ensure results that look natural both short- and long-term. Good communication with patients is essential to establishing realistic expectations.
Be conservative; design a mature hairline by leaving a reasonable degree of frontotemporal recession even in the young patient, as this will help the patient to look natural long term. Explain to the patient that it is not uncommon to have more than one session of grafts. I prefer to wait at least a year before a second session; density may be increased at that time by adding grafts between the ones done before.
Several centers worldwide are working on tissue engineering in an attempt to clone hair follicles or culture and multiply hair follicles in the laboratory setting. When successful, we will be able to treat patients with limited donor hair (the follicular-challenged patient), will only need to harvest a sample of hair follicles, and will eliminate the minimal donor-site morbidity and discomfort almost completely.
PREOPERATIVE PREPARATION
As in all other elective plastic surgical procedures the patient must be in good health and have no significant health problems. The patient needs to avoid aspirin, Plavix (clopidogrel), Coumadin (warfarin), and all types of anticoagulants for at least a week preoperatively. It is very important to have a normal clotting time.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree