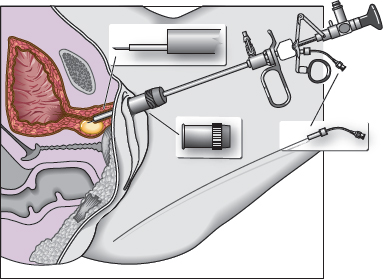
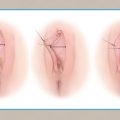
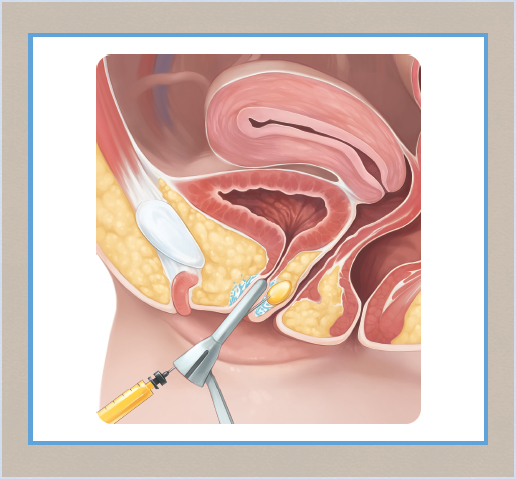
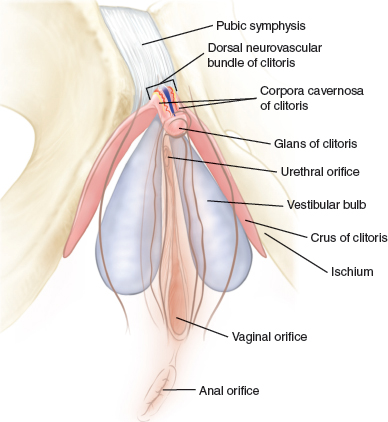
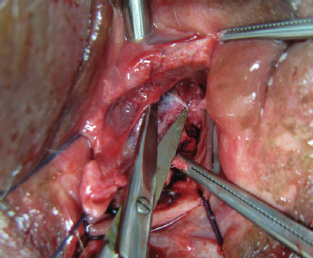
CHAPTER 14 • The G-spot is located below or inferior to the female urethra, approximately midway between the pubic bone and the cervix, and is responsible for vaginally activated orgasms. • The precise anatomy of the G-spot is not completely understood. • Vaginal laxity can be treated with vaginoplasty, which involves lifting the vaginal mucosa to tighten the sling muscles, removing excess vaginal lining, and reattaching the muscles. • Vulvovaginal atrophy can be treated with vaginal estrogens, systemic estrogens, radiofrequency (RF), and laser therapies. • Laser vaginal rejuvenation is a minimally invasive, temporary treatment that can be performed alone or after vaginoplasty. • RF vaginal restoration promotes collagen formation and remodeling and is a temporary treatment; similar to laser rejuvenation, it may prove to be an effective treatment after vaginoplasty. Seldom in modern medicine, and particularly in sexology and sexual medicine, has there been so much reactivity as that related to the female orgasm in general and to the G-spot in particular. According to mythology, Tiresias, the son of a shepherd and a nymph, was punished by the goddess Hera for hitting a pair of copulating snakes and, in punishment, was turned into a woman. Later, Tiresias became embroiled in an argument between Zeus and Hera over who has more pleasure during sex: the man, as claimed by Hera, or the woman, as claimed by Zeus. As a woman who had once been a man, Tiresias was deemed to know the answer and replied, “of 10 parts, a man only enjoys one.” Hera instantly struck Tiresias blind for his (or her) impiety and for revealing the secret of the female orgasm. This myth shows how, for whatever reason, the truth about female sexuality has largely been hidden, even since ancient times.1 In the twentieth century, modern Western culture had moved toward the belief that women were incapable of an intense orgasm, except by clitoral manipulation. This concept was reinforced by the work of Masters and Johnson,2 whose research claimed that a woman’s clitoris was the only source of female pleasure, even though many women had found that this was far from the truth. This misguided notion persisted until 1950, when an article by the German gynecologist Ernst Gräfenberg3 drew attention to his findings of a highly erotic area in the female urethra approximately midway between the pubic bone and the cervix. Drs. John Perry and Beverly Whipple4 named this area of the urethra the Gräfenberg spot or the G-spot. Whipple—co-author of The G-Spot and Other Discoveries About Human Sexuality5—claimed that the G-spot was overlooked by so many physicians during the first half of the nineteenth century for two reasons. First, the G-spot lies on the anterior wall of the vagina, which is an area that is not palpated during a normal vaginal examination. When physicians palpate this area in their patients, the patients have a sexual response. Second, doctors are trained not to sexually stimulate their patients. Whipple claimed that all gynecologists who palpated this area according to her and Dr. Perry’s instructions found the erotic area. All members of this early group of physicians later reported back to Whipple’s research group that they had subsequently found the erotic area of the urethra (G-spot) in every woman examined. Women can have two kinds of orgasm. However, they are not strictly “clitoral” versus “vaginal,” as some authors have reported. Rather, they are “clitorally activated” versus “vaginally activated.” In their study on vaginally activated orgasms versus clitorally activated orgasms, Jannini et al6 showed that orgasms resulting from direct clitoral stimulation have been reported to be sharp, bursting, short-lasting, superficial, and more localized, confined only to the pubic area.7,8 By contrast, vaginally activated orgasms have been described as more diffuse, whole-body, radiating, psychologically more satisfying, and longer lasting.6–8 It has been further shown that women who have both types of orgasm have even deeper, more powerful, blended orgasms resulting from contractions in both areas at once. The most common orgasm (sometimes called a clitorally activated orgasm) also involves the vagina, because clitoral stimulation produces contractions of the pubococcygeal muscle supporting the pelvic floor, which is where vaginal contractions are felt. Orgasms that result from G-spot stimulation involve the vagina as well but cause contractions around the uterus, which is several inches above the pelvic floor, and may also involve the muscles of the lower part of the anterior abdominal wall. The anatomic structures that might provoke a vaginally activated orgasm, rather than a clitorally activated orgasm, have not been completely and unequivocally described. This is probably the result of major uncertainty regarding human gross anatomy (Fig. 14-1). After the publication of the book The G-Spot and Other Discoveries About Human Sexuality5 in 1982, many scientists began the search for a specific, discrete organ or site within the anterior vaginal wall with a high nerve density that could explain the increased sensitivity of this region reported by many women.9,10 Recently, Gravina et al11 demonstrated a direct correlation between the thickness of the urethrovaginal space, or G-spot, and vaginal orgasms. Zaviacic et al12 affirmed that the urethrovaginal space is occupied by the female prostate. On the other hand, Crooks and Baur13 reported that the G-spot consists of a system of glands (Skene glands) and ducts that surround the urethra. The female prostate has been considered as an afunctional, vestigial gland. Zaviacic and Albin14 demonstrated that the prostate can be considered as another organ in both males and females, having a different size, weight, and function, yet the same qualitative parameters in both genders. Battaglia et al15 studied a group of women by ultrasound and color Doppler examination. The urethrovaginal space and the clitoral body were scanned with high-resolution ultrasound using the color Doppler mode. Fig. 14-1 Gross anatomy of the vaginal introital area of the vulva. Gravina et al11 examined the urethrovaginal space along a line drawn between the border of the smooth muscle, the mucosal-submucosal layer of the urethral wall, and the border of the vaginal wall and its lumen. The three-dimensional reconstruction of the urethrovaginal space had a glandlike aspect with small feeding vessels. Komisaruk et al16 confirmed the presence of several different organs in this highly complex body region. They stated that this area may include the anterior vaginal wall, the urethra itself, the Skene glands (including the periurethral glands, also known as the female prostate gland), perhaps the other glands in this region (vestibular glands and Bartholin glands), the surrounding muscle and connective tissue, and possibly the crura of the clitoris. Gravina et al11 demonstrated that women who reported vaginally activated orgasms had a larger distance between the urethra and the vaginal mucosa than women who reported having no vaginally activated orgasm, thereby suggesting a bigger and possibly more active cliterourethrovaginal complex (G-spot). This finding was confirmed by other researchers, who found that vaginally activated orgasms were associated not only with a thicker, but also with a longer urethrovaginal septum.17 In addition to the potentially important role of engorgement of the vascular erectile components of the cliterourethrovaginal complex during sexual arousal,17 these tissues were located superficially below the mucosal layer of the vagina in a cadaveric autopsy study.18 Based on this anatomic finding, subvaginal filling (as in G-spot augmentation), performed transvaginally is potentially incorrect. These findings suggest that the filler should be placed closer to the urethra than to the vaginal wall. The clitoris is innervated mainly by the pudendal nerve (see Fig. 1-11), the vagina primarily by the pelvic nerves, and the cervix by the hypogastric, pelvic, and vagus nerves.8 If several neural pathways are activated during cliterourethrovaginal complex stimulation (the pelvic, hypogastric, and vagus nerves), whereas only the pudendal nerve is directly stimulated during clitoral stimulation, this could at least partially explain perceptual differences between clitorally activated orgasms and vaginally activated orgasms. In a recent study by anatomic dissection of fresh frozen cadavers, Ostrzenski19 identified the G-spot as an elongated structure lying on the superodorsal perineal membrane at an oblique angle of 35 degrees dorsal (that is, vaginalward) to the urethra, with the perinealward pole lying 3 mm from the urethra, the cervivalward pole 15 mm from the urethra, and the whole structure parallel to the urethra (Fig. 14-2). Fig. 14-2 The G-spot is seen as bluish, grapelike compositions between the superodorsal perineal membrane and the inferior pubocervical fascia and grossly resembling that cavernous tissue, which creates a 35-degree angle with the lateral urethra. The ropelike structure emerges from the tail that disappears into the adjacent tissue. The lower pole measures 3 mm and the upper pole 15 mm from the urethra. The G-spot’s housing looked grossly like the fibroconnective tissues. All women have a G-spot. Not all women have G-spot (cliterourethrovaginal complex) orgasms. The reason may be that the clitoris is superficial and easily stimulated, whereas the G-spot is hidden and more difficult to stimulate. Both women and men initially tend to concentrate on stimulation of the clitoris, especially during autostimulation; however, some women discover their G-spot during their immediate postpubertal years and learn to stimulate it. These women are more likely to have G-spot orgasms than those focused only on the clitoris. Therefore, when taking a patient’s history, determining what kind of orgasm the patient has is essential. Patients who do not have vaginally activated (G-spot) orgasms need to be taught how to achieve these, because simply augmenting the G-spot will not guarantee that a patient will have G-spot orgasms (see Self-Discovery of the G-Spot). A physical examination, apart from a standard general examination, requires a vaginal examination that includes locating the patient’s G-spot. With the fingers gently inserted into the vagina about 5 to 6 cm past the introitus and beneath the pubic bone, pressure on the anterior vaginal wall roughly midway between the pubic bone and the cervix will initially cause a desire to micturate. After releasing and reapplying pressure, the patient will eventually report that this produces erotic and pleasing feelings. The examiner should stop at this point, record the depth of the G-spot in relation to a fixed anatomic landmark such as the urethral orifice, and continue to inform the patient verbally. The recorded depth of the G-spot will be useful later during G-spot augmentation. Nonvaginally activated patients must be taught how to stimulate their G-spot. They should have G-spot–induced orgasms before undergoing G-spot augmentation. This will help to ensure quality results. To do this, the patient helps me to find her G-spot (in the presence of my nurse). Once located, the exact site is recorded. The patient sits upright and is shown how and where to identify her own G-spot using her fingers. This can be difficult for some patients. In these cases, I take a G-spot vibrator and locate the spot for her. She then reinserts the vibrator herself and locates the site of the erotically centered spot on her anterior vaginal wall. If she has brought her own vibrator with her, we use it, and we mark the front edge of the vibrator to assist her with finding the correct depth when attempting this at home. Most patients learn the technique easily, although some require more than one session. I advise them to sit in front of a mirror at home with the thighs fully abducted and slightly flexed at the hips to expose the vaginal introitus. They should proceed as shown in my examination room. I think having a nurse chaperone (not a friend or family member) is critical. I wear gloves to clinically and psychologically emphasize as much as possible the nonpersonal nature of this highly intimate examination. About 35% of women are unable to convert to even mild G-spot orgasms. I refer these patients to a sex therapist, which is helpful in many cases (approximately 15%). Some are lost to follow-up, and some continue to have therapy. As part of the physical examination, once the physician has located the G-spot, the patient should be shown where it is by having her insert her fingers along the anterior vaginal wall until she feels the same sensation that the examiner was able to cause during the examination. The patient should be told to acquire a so-called G-spot vibrator, which is specially shaped to stimulate the anterior vaginal wall so that she can improve her G-spot sensations in the privacy of her own home. The patient’s partner should also be taught to locate the position of the G-spot and to perform the “come hither” finger technique, which he can use to stimulate his partner’s G-spot. Platelet-rich plasma and other methods of G-spot augmentation should be given only to women who have had G-spot orgasms, however inadequate. These techniques will only enhance the duration and intensity of G-Spot orgasms in these women. These methods, in my experience, will not induce G-spot orgasms in women who have not had G-spot orgasms. Platelet-rich plasma is a new addition to this area (see Chapter 15). Experience with its use is limited, and there are no peer-reviewed articles about its use. I have made no conclusions about this product based on my own limited experience using it for improving G-spot performance. In the small number of cases that I have performed, none has reported improved G-spot orgasms, and none has converted from not having G-spot orgasms to having them. Augmentation of the G-spot works on the basis that bulking the G-spot forward toward the vaginal lumen on the vaginal wall will bring it into greater contact with the vaginal contents and increase the likelihood of the patient having longer and more intense G-spot orgasms. Current techniques for transvaginally instilling material such as collagen or other nonpermanent fillers or various permanent fillers into the anterior wall of the vagina do not—on the basis of current anatomic knowledge8,11,13,15—make a great deal of sense to me. The G-Shot®, as demonstrated by its inventor, David Matlock, is given either just into the subvaginal mucosa (that is, between the G-spot and the vaginal mucosa) or into the G-spot in the urethrovaginal septum (that is, directly into the G-spot itself). Because the bulk of the G-spot tissues lies closer to the vaginal wall than to the urethral wall in the urethrovaginal septum, it makes more sense to place the bulking material just under the musculature of the urethra at about its midpoint (Figs. 14-3 and 14-4) to push the G-spot structures caudally (toward the vaginal lumen) and bring these structures closer to intravaginal contents such as a penis or a finger to facilitate stimulation. I achieve this by injecting 1.5 to 2.5 ml of Macroplastique® (Cogentix Medical) transurethrally using a Storz Viscous Fluid Injection Set (see Fig. 14-3). Macroplastique is placed just under the muscularis of the urethra, above the previously determined G-spot to cause the G-spot to bulge vaginalward. Alternatively, the Macroplastique Implantation Device can be used, which involves a blind procedure and requires that the G-spot be palpated transvaginally to make sure that the tip of the device is in the urethra at the correct position (see Fig. 14-4). The needle is inserted and injection is completed. Macroplastique is medical-grade silicone that is thermogravimetric analysis (TGA)–approved for periurethral and periureteric injection for various urologic indications. It is permanent and does not migrate or lose any appreciable volume. Macroplastique lasts forever, and if it is inadvertently placed incorrectly, it is fairly easy to remove. By contrast, hyaluronic acid is temporary, lasting only 12 to 18 months; if it is combined with Botox, it may last 2 to 2½ years. It can be diminished by injecting hyaluronidase to dispel it, but 100% removal takes time. Allergy to hyaluronic acid occurs occasionally, whereas allergy to silicone has never been reported, to my knowledge.
Future Avenues and Advances
Colin C.M. Moore
Key Points
The G-Spot
History
Orgasm Types
Anatomy of the G-Spot
Treatment
Patient History and Physical Examination
Self-Discovery of the G-Spot
Women Who Do Not Have G-Spot Orgasms
Women Who Have G-Spot Orgasms
Platelet-Rich Plasma
Transvaginal Versus Transurethral Augmentation of the G-Spot
Plastic Surgery Key
Fastest Plastic Surgery & Dermatology Insight Engine