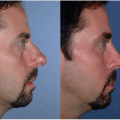
Chapter 30. Chin Augmentation
Ryan Michael Garcia, MD; Bahman Guyuron, MD, FACS
INDICATIONS
Genioplasty is performed to correct horizontal and vertical discrepancies in the lower third of the face. The chin serves a pivotal role in balancing the overall aesthetic appeal and has a direct effect on the perception of other facial features. In particular, the inverse relationship of the chin and nose must be respected, as enhancement of the chin has the greatest effect on the appearance of the nose. A classification of chin deformities has been devised to help guide the surgical approach and various treatment options available.
The goals and limitations of each genioplasty procedure must be appreciated and the surgical plan individualized to the patient. Generally, osseous surgical options include simple burr reduction ostectomy, osteotomy with repositioning of the caudal segment (vertical and horizontal), osteotomy and grafting, or osteotomy and segmental sectioning. Other less technically demanding augmentation options include autologous grafting or the use of alloplastic implants. The benefits of shorter operative and recovery times associated with alloplastic implantation must be weighed against their limitations. For example, alloplastic implantation cannot significantly alter an undesirable cervicomental angle, and these procedures have guarded success in the correction of vertical and asymmetric chin deformities.
Genioplasty is contraindicated in a number of clinical situations. Genioplasty alone should not be performed in patients with severe facial disharmony where orthognathic surgery may be of better benefit. Furthermore, patients with advanced medical comorbidities, such as uncontrolled diabetes or uncorrectable coagulopathies, making surgical interventions and anesthesia unsafe, should not undergo elective genioplasty. Surgeons should caution the use of alloplastic implants in patients with immunocompromised conditions because of the increased risks of periprosthetic infections. On the other hand, patients in their sixth decade of life or older with minimal chin deformities may be better suited for an alloplastic implant as osseous corrections may be too extensive.
PREOPERATIVE PREPARATION
Careful preoperative soft-tissue cephalometric analysis using life-size photographs is critical to a successful aesthetic outcome. Vertical assessment of the chin is performed with frontal and profile view analysis. The ideal vertical face is divided into 3 equal sections (upper, middle, and lower face) by arbitrary lines drawn through the hairline, lower glabella, subnasale, and menton. The lower third of the face and lips are further analyzed by subdividing the lower face with a line through the stomion. The distance from the stomion to the menton should be twice the distance from the stomion to the subnasion. The female chin should have a single light reflection, whereas the wider and more rectangular male chin has a double light reflection.
Horizontal assessment of the chin is performed with profile analysis and aids the surgeon in balancing the inverse relationship of the nose and chin. Analysis starts with a tangent line drawn through the most projected portion of the upper lip, lower lip, and pogonion (anterior projection of the chin pad), thus creating Riedel’s plane. Generally, if the chin lies posterior to the Riedel plane, then microgenia exists, whereas a chin that lies anterior represents a macrogenic chin. Next, a line drawn from the subnasion to the pogonion should make an 11 ± 4-degree angle to a line drawn from the glabella to the subnasion. The lips in profile are also analyzed in relation to any perceived chin deformity. Ideally, the upper lip is at the same level as the lower lip or slightly anterior to it. Upper lip deficiency is most often skeletal in nature and related to either relative (secondary to a deficient maxilla) or absolute mandibular prognathia.
Identifying chin asymmetry and then distinguishing the underlying cause are performed in both the vertical and horizontal plane. Vertical symmetry is confirmed when the chin lies within a line that is drawn through the midglabella, the tip of the nose, and the philtral dimple. Horizontal symmetry is confirmed by parallel lines drawn through the oral commissures and medial canthi. Non-parallel lines through the oral commissures can represent asymmetry secondary to distortion of the maxilla or mandible and orthognathic surgery may be necessary for proper correction. On the other hand, an asymmetric chin with a parallel intercommissural line is likely intrinsic to the chin and osseous genioplasty alone can be planned.
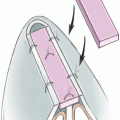
Vertical, horizontal, and combined chin deformities have been previously classified (Groups I to VII) based on the extent of bone or soft-tissue abnormality. Macrogenic chins (vertical, horizontal, or combined) are classified as Group I deformities and can be managed in a number of ways, depending on the extent of deformity. This includes simple burr ostectomy (Fig. 30-1); horizontal segment block or wedge resection (vertical); an osteotomy and caudal segment setback correction (horizontal); or a combined procedure, depending on the extent and plane of deformity present. Microgenic chins (vertical, horizontal, or combined) are classified as Group II deformities and can be managed by horizontal osteotomy and caudal segment repositioning (vertical), augmentation genioplasty, or horizontal osteotomy and caudal segment advancement (horizontal) (Figs. 30-2 and 30-3). Combined chin deformities (Group III) are defined as having an osseous excess in one plane and deficiency in the other plane. Horizontal excess and vertical deficiency can be corrected by an osteotomy with vertical advancement and posterior positioning of the caudal segment, whereas vertical excess and horizontal deficiency necessitates removal of an anterior cortical wedge along with cephalic and anterior repositioning of the caudal segment (Figs. 30-4 and 30-5). Asymmetric chin deformities (Group IV) are not well suited for alloplastic genioplasty secondary to the limited ability of a symmetric implant to correct an asymmetric deformity. Patients with an asymmetric chin but normal lower facial height are best treated by wedge osteotomy, osseous removal of the excessive side, and equal osseous grafting of the deficient side. Asymmetric chins with an excessive facial height require a closing wedge osteotomy with greater removal on the side of excess, whereas asymmetric chins with a deficient facial height require a single osteotomy with caudal repositioning and grafting of the deficient side. Pseudomacrogenic chins (Group V) are defined as having an excess of soft tissue demonstrated on radiographic studies and are best treated with resection through a submental incision. Pseudomicrogenic chins (Group VI) result from vertical maxillary excess along with a clockwise rotational deformity of the mandible. These deformities require orthognathic correction. Finally, witch’s chin deformities (Group VII) are characterized by soft-tissue ptosis and are corrected by an elliptical excision of soft tissue in the submental area.
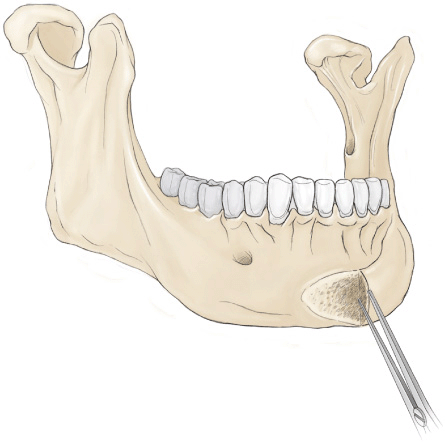
Figure 30-1 Macrogenic chin deformity can be managed with ostectomy using a large oval-tipped burr. The burr reduction is first completed on one half of the chin and measured precisely with a caliper prior to completing the opposite side. (Reproduced, with permission, from Guyuron B. Genioplasty. In: Plastic Surgery: Indications and Practice, Vol 2. St. Louis, MO: Elsevier; 2008:1536.)
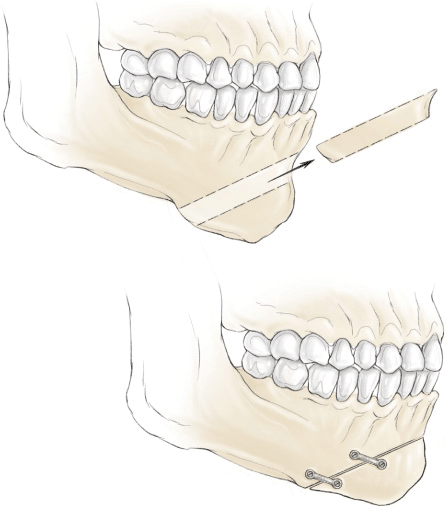
Figure 30-2
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree