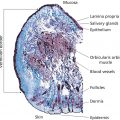
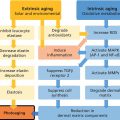
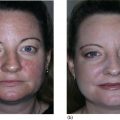
Christopher B. Harmon and Daniel P. Skinner Surgical Dermatology Group, Birmingham, AL, USA Dermabrasion is a skin resurfacing technique that surgically abrades or planes the epidermis through the use of a rapidly rotating wire brush or diamond fraise [1]. The wire brush or diamond fraise is used as the abrading tip to create an open wound that will heal by second intention. An irregular or scarred cutaneous surface may be surgically abraded in order to achieve a more regular plane, or a more gradual transition between different planes, thereby improving skin contour and appearance. In its simplest form, dermabrasion was practiced by ancient Egyptians in circa 1500 BC, who employed the abrasive characteristics of pumice and alabaster to treat skin blemishes [2]. Kurtin presented the first series of patients who underwent dermabrasion to Mount Sinai Hospital in 1953. Kurtin described the use of high‐speed rotary abraders, intraoperative freezing, and a variety of abrasive end pieces [3]. Later publications further refined Kurtin’s technique, including the use of the diamond fraise and the wire brush [4–7]. Since the introduction of modern dermabrasion by Kurtin, growing interest in the technique has culminated in its application to a variety of lesions including most commonly, facial scars secondary to acne, trauma, and surgery. The growing number of applications of dermabrasion has been accompanied by evolution of the technique from the use of common sandpaper in the mid‐twentieth century to electrically powered devices with wire brush tips or diamond fraises of varying sizes, shapes, and textures that can achieve speeds of over 33,000 revolutions per minute [8]. Fundamentally, the skin can be subdivided into three layers – epidermis, dermis, and subcutaneous tissue. The dermis is further subdivided into the more superficial papillary dermis, containing both a finely woven meshwork of collagen interdigitating with the epidermal rete as well as the superficial vascular plexus, and the deeper reticular dermis, composed of thick bundles of predominantly Type I collagen [9]. Resurfacing, by definition, involves iatrogenic removal of one or multiple layers of the skin to create a cutaneous wound. Dermabrasion mechanically removes the epidermis and papillary dermis, creating a partial‐thickness wound to heal by second intention. The well‐characterized, yet complex, wound healing response is triggered, involving transforming growth factor beta 1 (TGF‐β1)‐driven myofibroblastic deposition of new Type I and Type III collagen and subsequent remodeling in the dermis [10]. Additionally, TGF‐1β and epidermal growth factor (EGF) as well as other growth factors and matrix metalloproteinases (MMPs) stimulate re‐epithelialization from both underlying skin appendages and adjacent epithelialized skin [10]. Defined ultrastructural and molecular alterations accompany the clinically visible changes apparent in the dermabraded area. These include increased collagen bundle density and size with a tendency toward unidirectional orientation of collagen fibers parallel to the epidermal surface, as well as altered levels of α6‐ and β4‐integrin expression in the stratum spinosum [11]. When properly performed, the irregularly contoured or actinically damaged epidermal and papillary dermal layers are removed, and second intention wound healing occurs. The clinical result is a smoother, more evenly contoured surface, with fewer irregularities in the form of acne scars, rhytides, keratoses, or step‐off transitions. The most common indications for dermabrasion are desired improvement of acne scars, traumatic and surgical scars, rhinophyma, deep rhytides, and partial‐thickness Mohs defects (Figure 53.1) [12]. However, it has also been described for improvement of actinic keratoses, seborrheic keratoses, angiofibromas, syringomas, solar elastosis, epidermal nevi, tattoo removal, and, more recently, vitiligo [13–15]. With regard to acne scarring, even in the era of laser devices, fractionated delivery approaches, and non‐invasive “tissue‐tightening” procedures, dermabrasion remains an important tool in the combination approach to the improvement of cystic acne scarring. While the shallow and wide, undulating, or “rolling” type acne scars are better treated with subcision, dermal grafts, fillers, or fractionated laser devices, the slightly deeper and narrower “box‐car” type acne scars that demonstrate step‐off vertical borders respond best to mechanical dermabrasion. Additionally, the deepest and narrowest “ice‐pick” type acne scars respond best to dermabrasion subsequent to punch excisions, punch grafts, or trichloroacetic acid (TCA) cross destruction. Dermabrasion allows a skilled practitioner to selectively plane off “hilltops” surrounding atrophic scars which are so prominent in moderate to severe acne scarring. Chemical peels and laser treatments in contrast produce an injury of equivalent depth in both areas. Fractional CO2 resurfacing does have the advantage of creating skin contraction through the deep penetration, causing microthermal zones, which in some cases can produce improvement in acne scarring equivalent to dermabrasion [16, 17]. Figure 53.1 Dermabrasion after partial‐thickness Mohs layer on the nose. (a) Male patient with a partial‐thickness defect after 1 stage of Mohs micrographic surgery for the removal of basal cell carcinoma. (b) Immediately after spot dermabrasion to blend the surgical defect with the surrounding skin. (c) 2 weeks after Mohs and dermabrasion. For traumatic and surgical scars, the thickness, contour, and overall appearance are routinely improved with postoperative dermabrasion (Figure 53.2). Also known as “scarabrasion,” this procedure is best performed 6–8 weeks after the initial surgery or wounding event [18]. When performed during this 6–8 week window, the late proliferative and early remodeling phases of wound healing are interrupted and partially “reset,” resulting in an improved final cosmetic result. While several modalities, including wire loop electrosurgery and CO2 laser resurfacing, have been described for the treatment of rhinophyma, dermabrasion remains unmatched in the operator’s ability to re‐establish the complex contour of the many cosmetic subunits of the nose. Furthermore, although fractionated laser resurfacing has largely replaced dermabrasion for full face treatment of facial rhytides, dermabrasion can be as efficacious or more efficacious at removal of both fine and moderate facial rhytides. However, with patient preferences moving in the direction of less invasive procedures with shorter downtime, full face dermabrasion for rhytides is unlikely to return to widespread use in the foreseeable future. Figure 53.2 Dermabrasion of scar on the nose after Mohs surgery and reconstruction. (a) Female patient with a scar on the right nasal sidewall and lateral tip 6 weeks after Mohs surgery and flap reconstruction. (b) Immediately after dermabrasion to multiple cosmetic subunits of the nose. Feathering the border of the dermabraded area helps to minimize the color differences between the treated and untreated areas. (c) 2 weeks after dermabrasion with significant improvement in the appearance and texture of the scar. Finally, dermabrasion proves to be an incredibly useful technique in the armamentarium of the Mohs surgeon. Thin carcinomas in cosmetically sensitive or high‐risk areas can often be completely removed with a shallow Mohs layer to the level of the superficial reticular dermis. After clearance, these partial‐thickness defects, particularly on the nose and scalp, may lend themselves to healing by second intention rather than primary closure, yet with slightly increased risk of an evident contour discrepancy or sharp pigmentary transition. Dermabrasion of the edges surrounding the partial‐thickness Mohs defect greatly improves the final contour by replacing the steeply beveled wound edge with a more gradual slope. Additionally, dermabrading the remainder of an involved cosmetic subunit of the nose results in a less obvious scar by placing the pigmentary demarcation lines at the less perceptible subunit boundaries. As compared to fully ablative resurfacing with the CO2 and Er:YAG lasers, dermabrasion demonstrates similar or greater efficacy for the treatment of scars, rhytides, and precancerous lesions, with less postoperative erythema and more rapid re‐epithelialization. While newer, fractionated delivery protocols result in even less erythema and quicker re‐epithelialization than dermabrasion, their efficacies for the improvement of scars, rhytides, and precancerous lesions do not currently match that seen with mechanical dermabrasion. However, a recent study comparing fractionated CO2 laser and mechanical dermabrasion for post‐Mohs scars did show the same efficacy for both treatment modalities, with less bleeding erythema and edema in the group treated with CO2 laser [19]. Dermabrasion has also been shown to be more efficacious than 5‐fluorouracil for the treatment of actinic keratosis [20]. The major disadvantage of dermabrasion as compared to the above modalities is that it is much more operator dependent. Unlike laser and light devices, the depth of penetration is not pre‐programmed. Successful treatment relies not only on the physician’s knowledge of the modality and application settings, but also on his or her skilled execution. In the novice’s hands, dermabrasion exhibits a narrower window or buffer between effective treatment depth and inappropriate scarring depth. However, this is quickly overcome with experience. The most important components of the preoperative consultation are determining the patient’s specific motivation for resurfacing and establishing realistic expectations regarding the treatment outcome. The ultimate goal of any resurfacing treatment should be an improvement of the given defect rather than a complete eradication. Dermabrasion consistently achieves 30–50% improvement in the appearance of deep acne scars and rhytides (Figure 53.3
CHAPTER 53
Dermabrasion
Definition and history
Mechanism of action
Indications
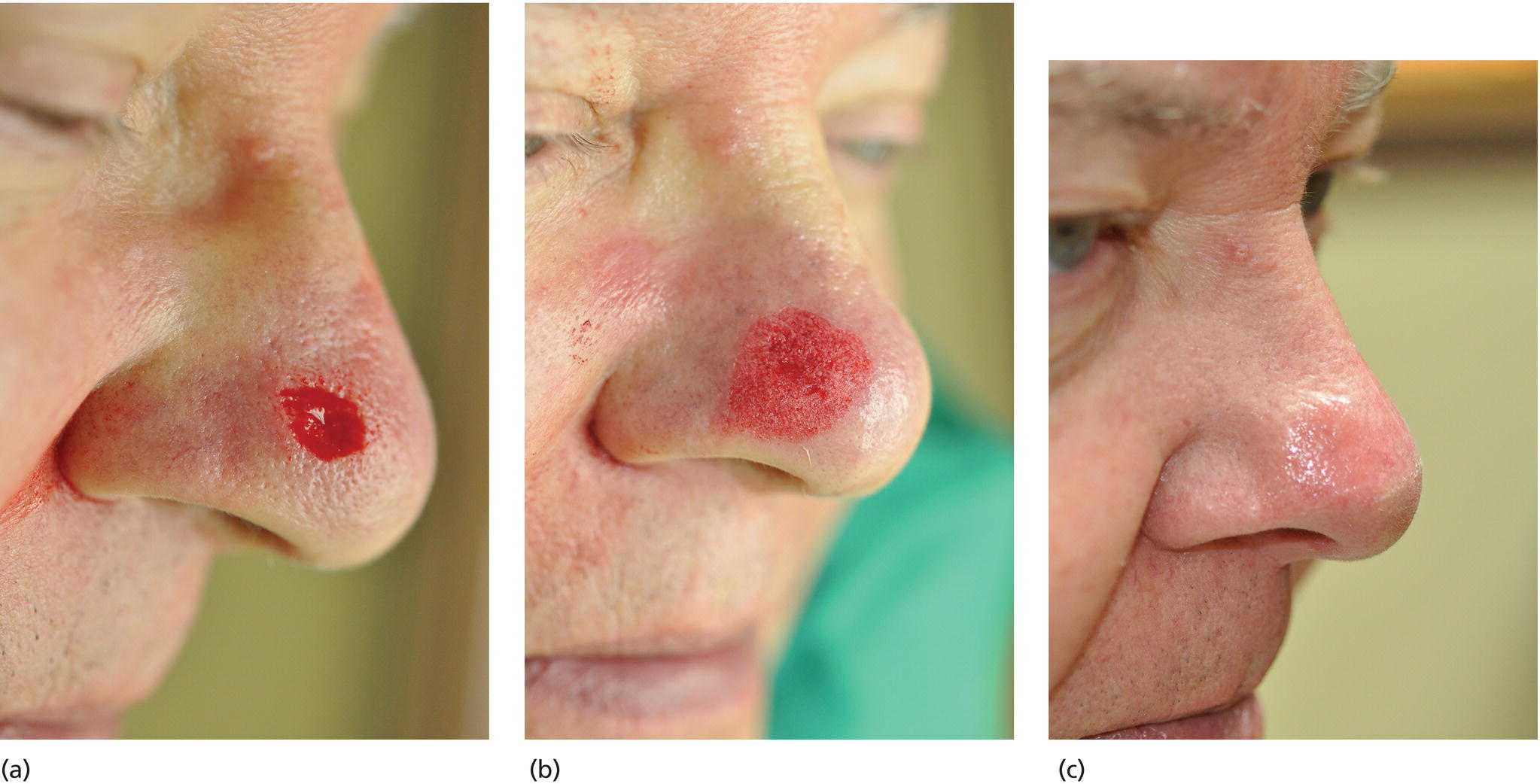
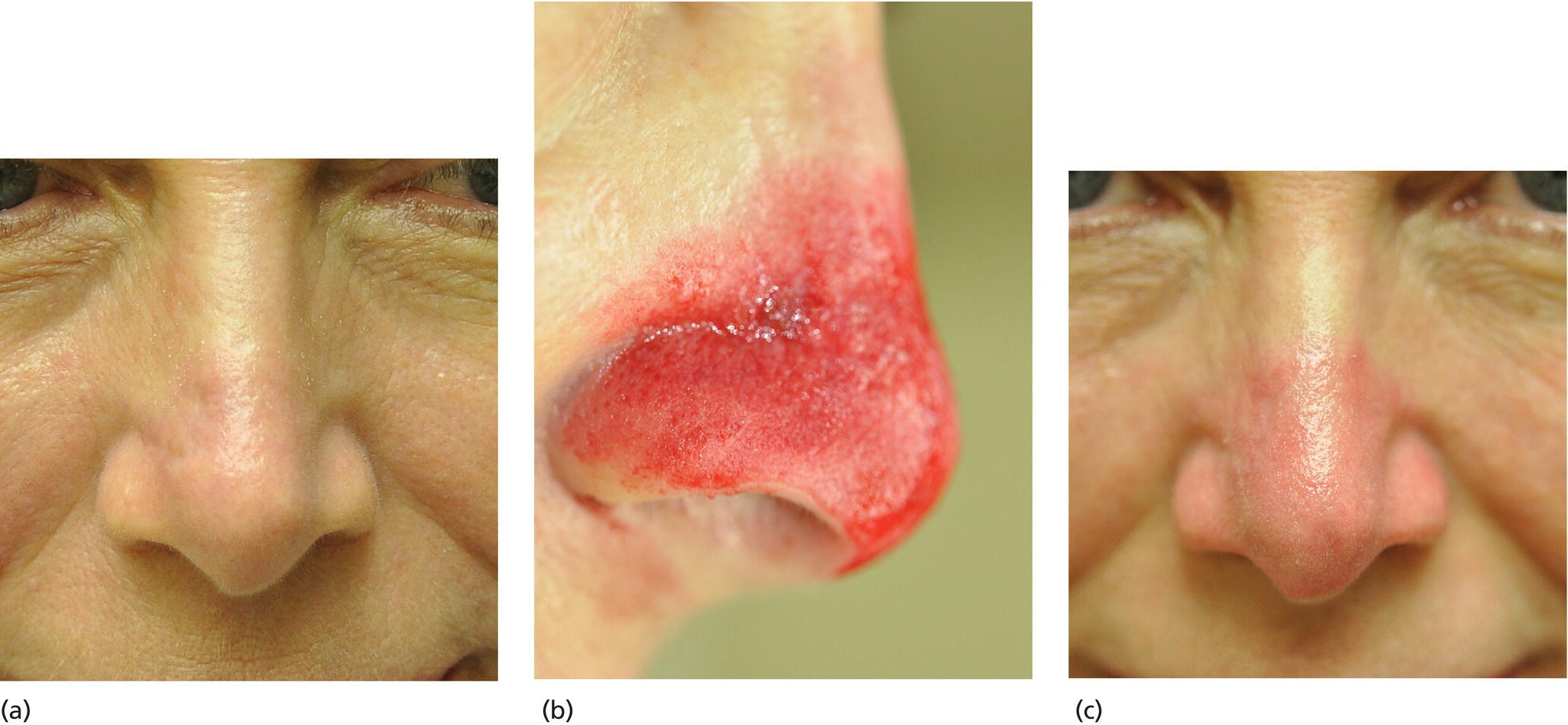
Advantages and disadvantages
Patient selection and preoperative consultation
![]()
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree